Abstract
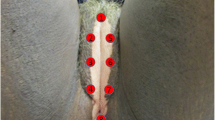
Vulvar lichen sclerosus (VLS) is a chronic non-neoplastic skin lesion characterized by vulvar itching, pain, atrophy, whitening of the skin and mucous membranes, and gradual atrophy and disappearance of the labia minora, which can eventually lead to vulvar scarring, causing functional impairment and seriously affecting the patient’s physical and mental health. VLS can occur at any age, however, its pathogenesis and etiology are not fully understood. Considerable progress has been made in related research on genetic susceptibility factors, autoimmune disorders, collagen metabolism abnormalities, and their triggering factors in disease formation and progression. This article reviews the etiology of vulvar lichen sclerosus.

Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Fruchter R, Melnick L, Pomeranz MK (2017) Lichenoid vulvar disease: a review. Int J Womens Dermatol 3:58–64
Eva LJ (2012) Screening and follow up of vulval skin disorders. Best Pract Res Clin Obstet Gynaecol 26:175–188
Singh N, Ghatage P (2020) Etiology, clinical features, and diagnosis of Vulvar Lichen Sclerosus: a scoping review. Obstet Gynecol Int 2020:7480754
Nelson DM, Peterson AC (2011) Lichen Sclerosus: epidemiological distribution in an equal access health care system. J Urol 185:522–525
Bleeker MC, Visser PJ, Overbeek LI et al (2016) Lichen Sclerosus: incidence and risk of Vulvar squamous cell carcinoma. Cancer Epidemiol Biomarkers Prev 25:1224–1230
Yang M, Wen W, Chang J (2018) Vulvar lichen sclerosus: a single-center retrospective study in China. J Dermatol 45:1101–1104
Micheletti L, Preti M, Radici G et al (2016) Vulvar Lichen Sclerosus and Neoplastic Transformation: a retrospective study of 976 cases. J Low Genit Tract Dis 20:180–183
Lee A, Fischer G (2018) Diagnosis and treatment of Vulvar Lichen Sclerosus: an update for dermatologists. Am J Clin Dermatol 19:695–706
Steinkasserer L, Hachenberg J, Hillemanns P et al (2023) Characterization of patients with vulvar lichen sclerosus and association to vulvar carcinoma: a retrospective single center analysis. Arch Gynecol Obstet 307:1921–1928
Tran DA, Tan X, Macri CJ et al (2019) Lichen Sclerosus: an autoimmunopathogenic and genomic enigma with emerging genetic and immune targets. Int J Biol Sci 15:1429–1439
Heymann WR (2020) Juvenile lichen sclerosus: a loss of innocence. J Am Acad Dermatol 82:301–302
Corazza M, Schettini N, Zedde P et al (2021) Vulvar lichen sclerosus from pathophysiology to therapeutic approaches: evidence and prospects. Biomedicines 9(8):950
Oyama N, Hasegawa M, Sclerosus L (2022) A current landscape of autoimmune and genetic interplay. Diagnostics (Basel) 12(12):3070
Lis-Święty A, Mierzwińska K, Wodok-Wieczorek K et al (2014) Co-existence of lichen sclerosus and localized scleroderma in female monozygotic twins. J Pediatr Adolesc Gynecol 27:e133–136
Liu GL, Cao FL, Zhao MY et al (2015) Associations between HLA-A\B\DRB1 polymorphisms and risks of vulvar lichen sclerosus or squamous cell hyperplasia of the vulva. Genet Mol Res 14:15962–15971
Gao XH, Barnardo MC, Winsey S et al (2005) The association between HLA DR, DQ antigens, and vulval lichen sclerosus in the UK: HLA DRB112 and its associated DRB112/DQB10301/04/09/010 haplotype confers susceptibility to vulval lichen sclerosus, and HLA DRB10301/04 and its associated DRB10301/04/DQB10201/02/03 haplotype protects from vulval lichen sclerosus. J Invest Dermatol 125:895–899
Powell J, Wojnarowska F, Winsey S et al (2000) Lichen Sclerosus premenarche: autoimmunity and immunogenetics. Br J Dermatol 142:481–484
Holt PJ, Darke C (1983) HLA antigens and bf allotypes in lichen Sclerosus et atrophicus. Tissue Antigens 22:89–91
Haefner HK, Welch KC, Rolston AM et al (2019) Genomic profiling of Vulvar Lichen Sclerosus patients shows possible pathogenetic disease mechanisms. J Low Genit Tract Dis 23:214–219
Torres A, Zaborek-Łyczba M (2022) The Importance of Immunological Disorders in the Pathogenesis of Lichen Sclerosus in Pediatric Patients: A Systematic Review. Int J Mol Sci 23(22):14212
Terlou A, Santegoets LA, Van Der Meijden WI et al (2012) An autoimmune phenotype in vulvar lichen sclerosus and lichen planus: a Th1 response and high levels of microRNA-155. J Invest Dermatol 132:658–666
Wang L, Yi JL, Chen HY et al (2021) Level of Foxp3, DNMTs, methylation of Foxp3 promoter region, and CD4 + CD25 + CD127low regulatory T cells in vulvar lichen sclerosus. Kaohsiung J Med Sci 37:520–527
Tchórzewski H, Rotsztejn H, Banasik M et al (2005) The involvement of immunoregulatory T cells in the pathogenesis of lichen sclerosus. Med Sci Monit 11:Cr39–43
Wang L, Lv Q, Guo J et al (2022) Transcriptome Profiling and Network Analysis Provide Insights into the pathogenesis of Vulvar Lichen Sclerosus. Front Genet 13:905450
Gross T, Wagner A, Ugurel S et al (2001) Identification of TIA-1 + and granzyme B + cytotoxic T cells in lichen Sclerosus et atrophicus. Dermatology 202:198–202
Wenzel J, Wiechert A, Merkel C et al (2007) IP10/CXCL10 - CXCR3 interaction: a potential self-recruiting mechanism for cytotoxic lymphocytes in lichen Sclerosus et atrophicus. Acta Derm Venereol 87:112–117
Sander CS, Ali I, Dean D et al (2004) Oxidative stress is implicated in the pathogenesis of lichen sclerosus. Br J Dermatol 151:627–635
Tan X, Ren S, Yang C et al (2021) Differentially regulated miRNAs and their related molecular pathways in lichen sclerosus. Cells 10(9):2291
Bao Y, Li Z, Liu W et al (2021) Study of Langerhans cells and T lymphocytes in vulvar lichen sclerosus lesions. Australas J Dermatol 62:e217–e222
Bieber AK, Steuer AB, Melnick LE et al (2021) Autoimmune and dermatologic conditions associated with lichen sclerosus. J Am Acad Dermatol 85:228–229
Grassi S, Tadiotto Cicogna G, Magri F et al (2021) Frontal fibrosing alopecia and genital Lichen sclerosus: single-center experience. J Cosmet Dermatol 20:615–620
Kreuter A, Kryvosheyeva Y, Terras S et al (2013) Association of autoimmune diseases with lichen sclerosus in 532 male and female patients. Acta Derm Venereol 93:238–241
Godoy CA, Teodoro WR, Velosa AP et al (2015) Unusual remodeling of the hyalinization band in vulval lichen sclerosus by type V collagen and ECM 1 protein. Clin (Sao Paulo) 70:356–362
Chan I, Oyama N, Neill SM et al (2004) Characterization of IgG autoantibodies to extracellular matrix protein 1 in lichen sclerosus. Clin Exp Dermatol 29:499–504
Sercu S, Zhang M, Oyama N et al (2008) Interaction of extracellular matrix protein 1 with extracellular matrix components: ECM1 is a basement membrane protein of the skin. J Invest Dermatol 128:1397–1408
Ren L, Zhao Y, Huo X et al (2018) MiR-155-5p promotes fibroblast cell proliferation and inhibits FOXO signaling pathway in vulvar lichen sclerosis by targeting FOXO3 and CDKN1B. Gene 653:43–50
Ishige T, Nishimura M, Satoh M et al (2016) Combined Secretomics and Transcriptomics revealed Cancer-Derived GDF15 is involved in diffuse-type gastric Cancer progression and fibroblast activation. Sci Rep 6:21681
Corazza M, Oton-Gonzalez L, Scuderi V et al (2020) Tissue cytokine/chemokine profile in vulvar lichen sclerosus: an observational study on keratinocyte and fibroblast cultures. J Dermatol Sci 100:223–226
De Oliveira GA, De Almeida MP, Soares FA et al (2012) Metalloproteinases 2 and 9 and their tissue inhibitors 1 and 2 are increased in vulvar lichen sclerosus. Eur J Obstet Gynecol Reprod Biol 161:96–101
Krapf JM, Mitchell L, Holton MA et al (2020) Vulvar Lichen Sclerosus: current perspectives. Int J Womens Health 12:11–20
Corrêa AC, Azevedo L, Almeida G et al (2007) Decorin and chondroitin sulfate distribution in vulvar lichen sclerosus: correlation with distinct histopathologic stages. J Reprod Med 52:38–42
Zhao Y, Zhao S, Li H et al (2018) Expression of galectin-7 in vulvar lichen sclerosus and its effect on dermal fibroblasts. Oncol Lett 16:2559–2564
De Luca DA, Papara C, Vorobyev A et al (2023) Lichen Sclerosus: the 2023 update. Front Med (Lausanne) 10:1106318
Zannoni GF, Faraglia B, Tarquini E et al (2006) Expression of the CDK inhibitor p27kip1 and oxidative DNA damage in non-neoplastic and neoplastic vulvar epithelial lesions. Mod Pathol 19:504–513
Paulis G, Berardesca E (2019) Lichen Sclerosus: the role of oxidative stress in the pathogenesis of the disease and its possible transformation into carcinoma. Res Rep Urol 11:223–232
Eisendle K, Grabner T, Kutzner H et al (2008) Possible role of Borrelia burgdorferi sensu lato infection in lichen sclerosus. Arch Dermatol 144:591–598
Edmonds E, Mavin S, Francis N et al (2009) Borrelia burgdorferi is not associated with genital lichen sclerosus in men. Br J Dermatol 160:459–460
Hald AK, Blaakaer J (2018) The possible role of human papillomavirus infection in the development of lichen sclerosus. Int J Dermatol 57:139–146
Kvistad S, Myhr KM (2014) Antibodies to Epstein-Barr virus and MRI disease activity in multiple sclerosis. Mult Scler 20:1833–1840
Aidé S, Lattario FR, Almeida G et al (2010) Epstein-Barr virus and human papillomavirus infection in vulvar lichen sclerosus. J Low Genit Tract Dis 14:319–322
Cong Q, Guo X, Zhang S et al (2021) HCV poly U/UC sequence-induced inflammation leads to metabolic disorders in vulvar lichen sclerosis. Life Sci Alliance. https://doi.org/10.26508/lsa.202000906
Haidopoulos D, Bakolas G, Michala L (2016) Turner syndrome: don’t forget the vulva. Endocrinol Diabetes Metab Case Rep 2016:160016
Potter JE, Moore KA (2013) Lichen Sclerosus in a breast cancer survivor on an aromatase inhibitor: a case report. J Gen Intern Med 28:592–595
Günthert AR, Faber M, Knappe G et al (2008) Early onset vulvar Lichen Sclerosus in premenopausal women and oral contraceptives. Eur J Obstet Gynecol Reprod Biol 137:56–60
Günthert AR, Limacher A, Beltraminelli H et al (2022) Efficacy of topical progesterone versus topical clobetasol propionate in patients with vulvar lichen sclerosus - A double-blind randomized phase II pilot study. Eur J Obstet Gynecol Reprod Biol 272:88–95
Higgins CA, Cruickshank ME (2012) A population-based case-control study of aetiological factors associated with vulval lichen sclerosus. J Obstet Gynaecol 32:271–275
Virgili A, Borghi A, Cazzaniga S et al (2017) New insights into potential risk factors and associations in genital lichen sclerosus: data from a multicentre Italian study on 729 consecutive cases. J Eur Acad Dermatol Venereol 31:699–704
Chattopadhyay S, Arnold JD, Malayil L et al (2021) Potential role of the skin and gut microbiota in premenarchal vulvar lichen sclerosus: a pilot case-control study. PLoS ONE 16:e0245243
Kirtschig G (2016) Lichen Sclerosus-Presentation, diagnosis and management. Dtsch Arztebl Int 113:337–343
Ismail D, Owen CM (2019) Paediatric vulval lichen sclerosus: a retrospective study. Clin Exp Dermatol 44:753–758
Kirby L, Gran S, Orekoya F et al (2021) Is urinary incontinence associated with vulval lichen sclerosus in women? A cross-sectional study. Br J Dermatol 185:1063–1065
Orszulak D, Dulska A (2021) Pediatric Vulvar Lichen Sclerosus-A Review of the Literature. Int J Environ Res Public Health 18(13):7153
Acknowledgements
We gratefully acknowledge the Clinical Trial Center of Zhongnan Hospital of Wuhan University for supporting this study.
Funding
This study was supported by grants from the Clinical Research and Development Project, Science and Technology Innovation Cultivation Fund, Zhongnan Hospital of Wuhan University (lcyf202203).
Author information
Authors and Affiliations
Contributions
Xingkui Xie conceived the work that led to the acquisition of literatures and drafted the manuscript, Kejia Wu designed the outline of the review, revised the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xie, X., Wu, K. Advances in the pathogenesis of vulvar lichen sclerosus. Mol Biol Rep 51, 396 (2024). https://doi.org/10.1007/s11033-024-09318-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11033-024-09318-7