Abstract
Background
Cardiomyocyte injury is a typical feature in cardiovascular diseases. Changes in cardiomyocytes strongly affect the progression of cardiovascular diseases. This work aimed to investigate the biological function and potential mechanism of action of miR-150-5p in cardiomyocytes.
Methods and results
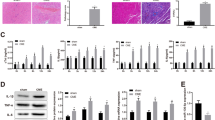
A myocardial ischemia (MI) injury rat model was constructed to detect miR-150-5p and tetratricopeptide repeat domain 5 (TTC5) expression during heart ischemia injury. Primary cardiomyocytes were isolated for in vitro study. CCK-8 assays were used to detect cardiomyocyte viability. Western blots were used to detect TTC5 and P53 expression. qPCR was utilized to measure RNA expression of miR-150-5p and TTC5. The TUNEL assay was used to determine cell apoptosis. ELISA was used to determine cytokine (TNF-α, IL-1β, IL-6, and IL-8) levels in heart tissues and cell culture supernatants. A dual-luciferase reporter assay was carried out to verify the binding ability between miR-150-5p and TTC5. Oxygen–glucose deprivation (OGD) treatment significantly inhibited cell viability. Ultrasound-targeted microbubble destruction (UTMD)-mediated uptake of miR-150-5p inverted these results. Additionally, UTMD-mediated uptake of miR-150-5p retarded the effects of OGD treatment on cell apoptosis. Besides, UTMD-mediated uptake of miR-150-5p counteracted the effects of OGD treatment on the inflammatory response by regulating cytokine (TNF-α, IL-1β, IL-6, and IL-8) levels. For the mechanism of the protective effect on the heart, we predicted and confirmed that miR-150-5p bound to TTC5 and inhibited TTC5 expression.
Conclusions
UTMD-mediated uptake of miR-150-5p attenuated OGD-induced primary cardiomyocyte injury by inhibiting TTC5 expression. This discovery contributes toward further understanding the progression of primary cardiomyocyte injury.







Similar content being viewed by others
Data availability
The data used to support the findings of this study are available from the corresponding author upon request.
Code availability
Not applicable.
References
Frangogiannis NG (2015) Pathophysiology of myocardial infarction. Compr Physiol 5(4):1841–1875. https://doi.org/10.1002/cphy.c150006
Koleini N, Kardami E (2017) Autophagy and mitophagy in the context of doxorubicin-induced cardiotoxicity. Oncotarget 8(28):46663–46680. https://doi.org/10.18632/oncotarget.16944
Kyselovic J, Leddy JJ (2017) Cardiac fibrosis: the beneficial effects of exercise in cardiac fibrosis. Adv Exp Med Biol 999:257–268. https://doi.org/10.1007/978-981-10-4307-9_14
Yuan X, Braun T (2017) Multimodal regulation of cardiac myocyte proliferation. Circ Res 121(3):293–309. https://doi.org/10.1161/circresaha.117.308428
Ye B, Chen X, Dai S, Han J, Liang X, Lin S, Cai X, Huang Z, Huang W (2019) Emodin alleviates myocardial ischemia/reperfusion injury by inhibiting gasdermin D-mediated pyroptosis in cardiomyocytes. Drug Des Dev Ther 13:975–990. https://doi.org/10.2147/dddt.S195412
Cai Y, Yu X, Hu S, Yu J (2009) A brief review on the mechanisms of miRNA regulation. Genomics Proteomics Bioinformatics 7(4):147–154. https://doi.org/10.1016/s1672-0229(08)60044-3
Lu TX, Rothenberg ME (2018) MicroRNA. J Allergy Clin Immunol 141(4):1202–1207. https://doi.org/10.1016/j.jaci.2017.08.034
Sanjay S, Girish C (2017) Role of miRNA and its potential as a novel diagnostic biomarker in drug-induced liver injury. Eur J Clin Pharmacol 73(4):399–407. https://doi.org/10.1007/s00228-016-2183-1
Tutar Y (2014) miRNA and cancer; computational and experimental approaches. Curr Pharm Biotechnol 15(5):429. https://doi.org/10.2174/138920101505140828161335
Verjans R, Peters T, Beaumont FJ, van Leeuwen R, van Herwaarden T, Verhesen W, Munts C, Bijnen M, Henkens M, Diez J, de Windt LJ, van Nieuwenhoven FA, van Bilsen M, Goumans MJ, Heymans S, Gonzalez A, Schroen B (2018) MicroRNA-221/222 family counteracts myocardial fibrosis in pressure overload-induced heart failure. Hypertension 71(2):280–288. https://doi.org/10.1161/hypertensionaha.117.10094
Lock MC, Tellam RL, Botting KJ, Wang KCW, Selvanayagam JB, Brooks DA, Seed M, Morrison JL (2018) The role of miRNA regulation in fetal cardiomyocytes, cardiac maturation and the risk of heart disease in adults. J Physiol 596(23):5625–5640. https://doi.org/10.1113/jp276072
Bernardo BC, Ooi JY, Lin RC, McMullen JR (2015) miRNA therapeutics: a new class of drugs with potential therapeutic applications in the heart. Fut Med Chem 7(13):1771–1792. https://doi.org/10.4155/fmc.15.107
Liu X, Deng Y, Xu Y, Jin W, Li H (2018) MicroRNA-223 protects neonatal rat cardiomyocytes and H9c2 cells from hypoxia-induced apoptosis and excessive autophagy via the Akt/mTOR pathway by targeting PARP-1. J Mol Cell Cardiol 118:133–146. https://doi.org/10.1016/j.yjmcc.2018.03.018
Deng S, Zhao Q, Zhen L, Zhang C, Liu C, Wang G, Zhang L, Bao L, Lu Y, Meng L, Lu J, Yu P, Lin X, Zhang Y, Chen YH, Fan H, Cho WC, Liu Z, Yu Z (2017) Neonatal heart-enriched miR-708 promotes proliferation and stress resistance of cardiomyocytes in rodents. Theranostics 7(7):1953–1965. https://doi.org/10.7150/thno.16478
Sakr M, Takino T, Sabit H, Nakada M, Li Z, Sato H (2016) miR-150-5p and miR-133a suppress glioma cell proliferation and migration through targeting membrane-type-1 matrix metalloproteinase. Gene 587(2):155–162. https://doi.org/10.1016/j.gene.2016.04.058
Dai FQ, Li CR, Fan XQ, Tan L, Wang RT, Jin H (2019) miR-150-5p inhibits non-small-cell lung cancer metastasis and recurrence by targeting HMGA2 and beta-catenin signaling. Mol Ther Nucleic Acids 16:675–685. https://doi.org/10.1016/j.omtn.2019.04.017
Li T, Xie J, Shen C, Cheng D, Shi Y, Wu Z, Zhan Q, Deng X, Chen H, Shen B, Peng C, Li H, Zhu Z (2014) miR-150-5p inhibits hepatoma cell migration and invasion by targeting MMP14. PLoS ONE 9(12):e115577. https://doi.org/10.1371/journal.pone.0115577
Shen J, Xing W, Gong F, Wang W, Yan Y, Zhang Y, Xie C, Fu S (2019) MiR-150-5p retards the progression of myocardial fibrosis by targeting EGR1. Cell Cycle 18(12):1335–1348. https://doi.org/10.1080/15384101.2019.1617614
Scrutinio D, Conserva F, Passantino A, Iacoviello M, Lagioia R, Gesualdo L (2017) Circulating microRNA-150-5p as a novel biomarker for advanced heart failure: a genome-wide prospective study. J Heart Lung Transplant 36(6):616–624. https://doi.org/10.1016/j.healun.2017.02.008
Amabile PG, Waugh JM, Lewis TN, Elkins CJ, Janas W, Dake MD (2001) High-efficiency endovascular gene delivery via therapeutic ultrasound. J Am Coll Cardiol 37(7):1975–1980. https://doi.org/10.1016/s0735-1097(01)01253-0
Bonci D, Cittadini A, Latronico MV, Borello U, Aycock JK, Drusco A, Innocenzi A, Follenzi A, Lavitrano M, Monti MG, Ross J Jr, Naldini L, Peschle C, Cossu G, Condorelli G (2003) “Advanced” generation lentiviruses as efficient vectors for cardiomyocyte gene transduction in vitro and in vivo. Gene Ther 10(8):630–636. https://doi.org/10.1038/sj.gt.3301936
Qin D, Li H, Xie H (2018) Ultrasoundtargeted microbubble destructionmediated miR205 enhances cisplatin cytotoxicity in prostate cancer cells. Mol Med Rep 18(3):3242–3250. https://doi.org/10.3892/mmr.2018.9316
Chen S, Ding JH, Bekeredjian R, Yang BZ, Shohet RV, Johnston SA, Hohmeier HE, Newgard CB, Grayburn PA (2006) Efficient gene delivery to pancreatic islets with ultrasonic microbubble destruction technology. Proc Natl Acad Sci USA 103(22):8469–8474. https://doi.org/10.1073/pnas.0602921103
Sutton JT, Raymond JL, Verleye MC, Pyne-Geithman GJ, Holland CK (2014) Pulsed ultrasound enhances the delivery of nitric oxide from bubble liposomes to ex vivo porcine carotid tissue. Int J Nanomed 9:4671–4683. https://doi.org/10.2147/ijn.S63850
Wu S, Li L, Wang G, Shen W, Xu Y, Liu Z, Zhuo Z, Xia H, Gao Y, Tan K (2014) Ultrasound-targeted stromal cell-derived factor-1-loaded microbubble destruction promotes mesenchymal stem cell homing to kidneys in diabetic nephropathy rats. Int J Nanomed 9:5639–5651. https://doi.org/10.2147/ijn.S73950
Chen ZY, Liang K, Qiu RX, Luo LP (2011) Ultrasound- and liposome microbubble-mediated targeted gene transfer to cardiomyocytes in vivo accompanied by polyethylenimine. J Ultrasound Med 30(9):1247–1258. https://doi.org/10.7863/jum.2011.30.9.1247
Li P, Gao Y, Liu Z, Tan K, Zuo Z, Xia H, Yang D, Zhang Y, Lu D (2013) DNA transfection of bone marrow stromal cells using microbubble-mediated ultrasound and polyethylenimine: an in vitro study. Cell Biochem Biophys 66(3):775–786. https://doi.org/10.1007/s12013-013-9523-x
Zhang L, Sun Z, Ren P, Lee RJ, Xiang G, Lv Q, Han W, Wang J, Ge S, Xie M (2015) Ultrasound-targeted microbubble destruction (UTMD) assisted delivery of shRNA against PHD2 into H9C2 cells. PLoS ONE 10(8):e0134629. https://doi.org/10.1371/journal.pone.0134629
Sander V, CeG Su, Jopling C, Morera C, Izpisua Belmonte JC (2013) Isolation and in vitro culture of primary cardiomyocytes from adult zebrafish hearts. Nat Protoc 8(4):800–809. https://doi.org/10.1038/nprot.2013.041
Rupaimoole R, Slack FJ (2017) MicroRNA therapeutics: towards a new era for the management of cancer and other diseases. Nat Rev Drug Discov 16(3):203–222. https://doi.org/10.1038/nrd.2016.246
Lee YS, Dutta A (2009) MicroRNAs in cancer. Annu Rev Pathol 4:199–227. https://doi.org/10.1146/annurev.pathol.4.110807.092222
Hathaway QA, Durr AJ, Shepherd DL, Pinti MV, Brandebura AN, Nichols CE, Kunovac A, Goldsmith WT, Friend SA, Abukabda AB, Fink GK, Nurkiewicz TR, Hollander JM (2019) miRNA-378a as a key regulator of cardiovascular health following engineered nanomaterial inhalation exposure. Nanotoxicology 13(5):644–663. https://doi.org/10.1080/17435390.2019.1570372
Hu Y, Jin G, Li B, Chen Y, Zhong L, Chen G, Chen X, Zhong J, Liao W, Liao Y, Wang Y, Bin J (2019) Suppression of miRNA let-7i-5p promotes cardiomyocyte proliferation and repairs heart function post injury by targetting CCND2 and E2F2. Clin Sci (Lond) 133(3):425–441. https://doi.org/10.1042/cs20181002
Yu L, Xiao Y, Zhou X, Wang J, Chen S, Peng T, Zhu X (2019) TRIP13 interference inhibits the proliferation and metastasis of thyroid cancer cells through regulating TTC5/p53 pathway and epithelial-mesenchymal transition related genes expression. Biomed Pharmacother 120:109508. https://doi.org/10.1016/j.biopha.2019.109508
Lin Z, Gasic I, Chandrasekaran V, Peters N, Shao S, Mitchison TJ, Hegde RS (2020) TTC5 mediates autoregulation of tubulin via mRNA degradation. Science 367(6473):100–104. https://doi.org/10.1126/science.aaz4352
Rasheed A, Gumus E, Zaki M, Johnson K, Manzoor H, LaForce G, Ross D, McEvoy-Venneri J, Stanley V, Lee S, Virani A, Ben-Omran T, Gleeson JG, Naz S, Schaffer A (2021) Bi-allelic TTC5 variants cause delayed developmental milestones and intellectual disability. J Med Genet 58(4):237–246. https://doi.org/10.1136/jmedgenet-2020-106849
Lynch JT, Somerville TD, Spencer GJ, Huang X, Somervaille TC (2013) TTC5 is required to prevent apoptosis of acute myeloid leukemia stem cells. Cell Death Dis 4(4):e573. https://doi.org/10.1038/cddis.2013.107
Liu X, Klionsky DJ (2019) Regulation of JMY’s actin nucleation activity by TTC5/STRAP and LC3 during autophagy. Autophagy 15(3):373–374. https://doi.org/10.1080/15548627.2018.1564417
Chen H, Hwang JH (2013) Ultrasound-targeted microbubble destruction for chemotherapeutic drug delivery to solid tumors. J Ther Ultrasound 1:10. https://doi.org/10.1186/2050-5736-1-10
Chen ZY, Lin Y, Yang F, Jiang L, Ge S (2013) Gene therapy for cardiovascular disease mediated by ultrasound and microbubbles. Cardiovasc Ultrasound 11:11. https://doi.org/10.1186/1476-7120-11-11
Wan C, Li F, Li H (2015) Gene therapy for ocular diseases meditated by ultrasound and microbubbles (Review). Mol Med Rep 12(4):4803–4814. https://doi.org/10.3892/mmr.2015.4054
Ma J, Du LF, Chen M, Wang HH, Xing LX, Jing LF, Li YH (2013) Drug-loaded nano-microcapsules delivery system mediated by ultrasound-targeted microbubble destruction: a promising therapy method. Biomed Rep 1(4):506–510. https://doi.org/10.3892/br.2013.110
Funding
This research was financially supported by the Natural Science Foundation of Hunan Province (Grant No. 2019JJ80080), Scientific Research Projects of Hunan Provincial Health Commission (Grant Nos. B2019062, 20200198), the Scientific Research Project of Hunan Provincial Education Department (Grant No. 20B357) and Key Project of Education Department of Hunan Province (Grant No. 21A0032).
Author information
Authors and Affiliations
Contributions
XZ and YH conceived and designed the study. YC, XL, and HC performed the experiments. ZZ and HP collected the data. JP, YL, and HW interpreted the results. YH contributed to the preparation, review, and revision of the manuscript. All authors agreed to be accountable for the content of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
Not applicable.
Patient consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (TIF 7793 KB)
Figure S1. UTMD treatment had no effect on cell viability or cell apoptosis. Cell viability in the control, control + UTMD, OGD, and OGD + UTMD group cells by the CCK-8 assay. (B) Cell apoptosis determined by the TUNEL assay. n = 3. Compared with control/control + UTMD, *p < 0.05.
Supplementary file2 (JPG 426 KB)
Figure S2. Validation results of transfection efficiency. qPCR assay results of miR-150-5p expression level after transfection with miR-NC or miR-150-5p mimic. n = 3. Compared with miR-NC, *p < 0.05. (B) TTC5 protein expression levels after transfection with pcDNA3.1-TTC5 (TTC5 group) or pcDNA3.1 (TTC5 vector group) determined by western blotting. n = 3. Compared with TTC5 vector, *p < 0.05.
Rights and permissions
About this article
Cite this article
Zhong, X., Chen, Y., Long, X. et al. Ultrasound-targeted microbubble destruction (UTMD)-mediated miR-150-5p attenuates oxygen and glucose deprivation-induced cardiomyocyte injury by inhibiting TTC5 expression. Mol Biol Rep 49, 6041–6052 (2022). https://doi.org/10.1007/s11033-022-07392-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-07392-3