Abstract
Background
Acetaminophen overdose causes renal injury via oxidative stress and apoptosis induction. Carvacrol has several pharmacological properties such as antioxidant, anti-inflammation and anti-apoptotic effect. The aim of this study was to determine the protective effect of carvacrol on acetaminophen-induced renal damage in rats.
Methods and results
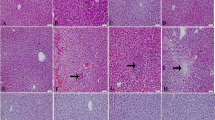
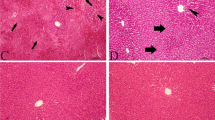
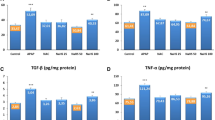
Forty male Wistar rats were randomly divided to five groups (n = 8) including control, carvacrol 10 mg/kg, acetaminophen, acetaminophen + carvacrol 5 mg/kg, and acetaminophen + carvacrol 10 mg/kg. Animals received a single dose of acetaminophen (500 mg/kg), then were treated with carvacrol for 1 week (daily). Afterwards, renal blood flow (RBF), mean arterial pressure, renal perfusion pressure, renal vascular resistance (RVR), blood urea nitrogen (BUN), and serum creatinine were measured. Also, malondialdehyde (MDA) concentration, glutathione peroxidase (GPx) and superoxide dismutase (SOD) activity levels were measured in the kidney tissue. Hematoxylin and eosin method was used for histological assessment. The Western blotting analysis was used to determine the Bax, Bcl-2 and cleaved caspase-3 proteins expression level in the kidney tissue. Carvacrol (10 mg/kg) significantly increased the RBF, GPx and SOD activities and also reduced the RVR, serum creatinine, BUN, and MDA in the acetaminophen + carvacrol 10 mg/kg group versus acetaminophen group (P < 0.05). Also, carvacrol significantly decreased the cleaved caspase-3, Bax proteins expression level, and kidney tissue damage score in the acetaminophen + carvacrol 10 mg/kg group versus acetaminophen group (P < 0.05).
Conclusions
This study showed that carvacrol can attenuate the acetaminophen induced acute kidney damage via suppressing oxidative stress and apoptosis biochemical factors.



Similar content being viewed by others
References
Roy S, Pradhan S, Das K, Mandal A, Mandal S, Patra A, Samanta A, Sinha B, Nandi DK (2015) Acetaminophen induced kidney failure in rats: a dose response study. J Biol Sci 15(4):187. https://doi.org/10.3923/jbs.2015.187.193
Lorz C, Justo P, Sanz A, Subirá D, Egido J, Ortiz A (2004) Paracetamol-induced renal tubular injury: a role for ER stress. J Am Soc Nephrol 15(2):380–389
Aycan İÖ, Tokgöz O, Tüfek A, Alabalık U, Evliyaoğlu O, Turgut H, Çelik F, Güzel A (2015) The use of thymoquinone in nephrotoxicity related to acetaminophen. Int J Surg 13:33–37. https://doi.org/10.1016/j.ijsu.2014.11.020
Mazer M, Perrone J (2008) Acetaminophen-induced nephrotoxicity: pathophysiology, clinical manifestations, and management. J Med Toxicol 4(1):2–6. https://doi.org/10.1007/BF03160941
El-Shafey MM, Abd-Allah GM, Mohamadin AM, Harisa GI, Mariee AD (2015) Quercetin protects against acetaminophen-induced hepatorenal toxicity by reducing reactive oxygen and nitrogen species. Pathophysiology 22(1):49–55. https://doi.org/10.1016/j.pathophys
Kaeidi A, Sahamsizadeh A, Allahtavakoli M, Fatemi I, Rahmani M, Hakimizadeh E, Hassanshahi J (2020) The effect of oleuropein on unilateral ureteral obstruction induced-kidney injury in rats: the role of oxidative stress, inflammation and apoptosis. Mol Biol Rep 47(2):1371–1379. https://doi.org/10.1007/s11033-019-05237-0
Kaeidi A, Taghipour Z, Allahtavakoli M, Fatemi I, Hakimizadeh E, Hassanshahi J (2020) Ameliorating effect of troxerutin in unilateral ureteral obstruction induced renal oxidative stress, inflammation, and apoptosis in male rats. Naunyn Schmiedeberg’s Arch Pharmacol 393(5):879–888. https://doi.org/10.1007/s00210-019-01801-4
Hassanshahi J, Mirzahosseini-Pourranjbar A, Hajializadeh Z, Kaeidi A (2020) Anticancer and cytotoxic effects of troxerutin on HeLa cell line: an in-vitro model of cervical cancer. Mol Biol Rep 47(8):6135–6142. https://doi.org/10.1007/s11033-020-05694-y
Butler MS (2008) Natural products to drugs: natural product-derived compounds in clinical trials. Nat Prod Rep 25(3):475–516. https://doi.org/10.1039/b514294f
Feher M, Schmidt JM (2003) Property distributions: differences between drugs, natural products, and molecules from combinatorial chemistry. J Chem Inf Comput Sci 43(1):218–227. https://doi.org/10.1021/ci0200467
Al-Attar AM, Elnaggar MH, Almalki EA (2017) Protective effect of some plant oils on diazinon induced hepatorenal toxicity in male rats. Saudi J Biol Sci 24(6):1162–1171. https://doi.org/10.1016/j.sjbs.2016.10.013
Cai Y, Luo Q, Sun M, Corke H (2004) Antioxidant activity and phenolic compounds of 112 traditional Chinese medicinal plants associated with anticancer. Life Sci 74(17):2157–2184. https://doi.org/10.1016/j.lfs.2003.09.047
Fukumoto L, Mazza G (2000) Assessing antioxidant and prooxidant activities of phenolic compounds. J Agric Food Chem 48(8):3597–3604. https://doi.org/10.1021/jf000220w
Suntres ZE, Coccimiglio J, Alipour M (2015) The bioactivity and toxicological actions of carvacrol. Crit Rev Food Sci Nutr 55(3):304–318. https://doi.org/10.1080/10408398.2011.653458
Kohen R, Nyska A (2002) Invited review: oxidation of biological systems: oxidative stress phenomena, antioxidants, redox reactions, and methods for their quantification. Toxicol Pathol 30(6):620–650. https://doi.org/10.1080/01926230290166724
Mandal A, Patra A, Mandal S, Roy S, Mahapatra SD, Mahapatra TD, Paul T, Das K, Mondal KC, Nandi DK (2015) Therapeutic potential of different commercially available synbiotic on acetaminophen-induced uremic rats. Clin Exp Nephrol 19(2):168–177. https://doi.org/10.1007/s10157-014-0971-4
Melo FHC, Moura BA, de Sousa DP, de Vasconcelos SMM, Macedo DS, de Fonteles MMF, de Viana GSB, de Sousa FCF (2011) Antidepressant-like effect of carvacrol (5-isopropyl-2-methylphenol) in mice: involvement of dopaminergic system. Fundam Clin Pharmacol 25(3):362–367. https://doi.org/10.1111/j.1472-8206.2010.00850.x
Uyanoglu M, Canbek M, Ceyhan E, Senturk H, Bayramoglu G, Gunduz O, Ozen A, Turgak O (2011) Preventing organ injury with carvacrol after renal ischemia/reperfusion. J Med Plants Res 5(1):72–80
Amin F, Memarzia A, Rad HK, Kazerani HR, Boskabady MH (2021) Carvacrol and PPARγ agonist, pioglitazone, affects inhaled paraquat-induced lung injury in rats. Sci Rep 11(1):1–15. https://doi.org/10.1038/s41598-021-87546-8
Gunes S, Ayhanci A, Sahinturk V, Altay DU, Uyar R (2017) Carvacrol attenuates cyclophosphamide-induced oxidative stress in rat kidney. Can J Physiol Pharmacol 95(7):844–849. https://doi.org/10.1139/cjpp-2016-0450
Hassanshahi J, Nematbakhsh M (2018) The role of Mas receptor on renal hemodynamic responses to angiotensin 1–7 in both irreversible and reversible unilateral ureteral obstruction rats. Adv Biomed Res. https://doi.org/10.4103/abr.abr_176_17
Samimiat A, Khosravi MS, Hassanshahi J, Nematbakhsh M (2018) The effect of AT2 and Mas receptors antagonists on renal hemodynamic and excretory disorders induced by ischemia/reperfusion in male and female rats. Physiol Pharmacol 22(2):133–140
Hantz H, Adesuyi A, Adebayo O (2001) Differential effects of U46619 on renal regional hemodynamics in the rat: involvement of endothelin. J Pharmacol Exp Ther 299(1):372–376
Hassanshahi J, Maleki M, Nematbakhsh M (2018) Renal blood flow and vascular resistance responses to angiotensin II in irreversible and reversible unilateral ureteral obstruction rats; the role of angiotensin II type 1 and 2 receptors. J Nephropathol 7(2):57–64
Richard MJ, Portal B, Meo J, Coudray C, Hadjian A, Favier A (1992) Malondialdehyde kit evaluated for determining plasma and lipoprotein fractions that react with thiobarbituric acid. Clin Chem 38(5):704–709
Ōyanagui Y (1984) Reevaluation of assay methods and establishment of kit for superoxide dismutase activity. Anal Biochem 142(2):290–296. https://doi.org/10.1016/0003-2697(84)90467-6
Flohé L, Günzler WA (1984) [12] Assays of glutathione peroxidase. Methods Enzymol 105:114–120
Wang B, Liu D, Zhu Q-h, Li M, Chen H, Guo Y, Fan L-p, Yue L-s, Li L-y, Zhao M (2016) Rutin ameliorates kidney interstitial fibrosis in rats with obstructive nephropathy. Int Immunopharmacol 35:77–84. https://doi.org/10.1016/j.intimp.2016.03.029
Sancak EB, Tan YZ, Turkon H, Silan C (2017) Attenuation of partial unilateral ureteral obstruction–induced renal damage with hyperbaric oxygen therapy in a rat model. Int Braz J Urol 43(5):946–956. https://doi.org/10.1590/S1677-5538.IBJU.2016.0565
Pakravan N, Bateman DN, Goddard J (2007) Effect of acute paracetamol overdose on changes in serum and urine electrolytes. Br J Clin Pharmacol 64(6):824–832. https://doi.org/10.1111/j.1365-2125.2007.02952.x
Trumper L, Girardi G, Elías MM (1992) Acetaminophen nephrotoxicity in male Wistar rats. Arch Toxicol 66(2):107–111. https://doi.org/10.1111/j.1472-8206.2009.00768.x
Chiam E, Bellomo R, Churilov L, Weinberg L (2018) The hemodynamic effects of intravenous paracetamol (acetaminophen) vs normal saline in cardiac surgery patients: a single center placebo controlled randomized study. PLoS ONE 13(4):e0195931
Wang B, Yang X, Yu H, Man X (2020) The comparison of ibuprofen versus acetaminophen for blood pressure in preeclampsia: a meta-analysis of randomized controlled studies. J Matern Fetal Neonatal Med. https://doi.org/10.1080/14767058.2020.1720641
Peixoto-Neves D, Silva-Alves K, Gomes M, Lima F, Lahlou S, Magalhães P, Ceccatto V, Coelho-de-Souza A, Leal-Cardoso J (2010) Vasorelaxant effects of the monoterpenic phenol isomers, carvacrol and thymol, on rat isolated aorta. Fundam Clin Pharmacol 24(3):341–350. https://doi.org/10.1111/j.1472-8206.2009.00768.x
Gheitasi I, Azizi A, Omidifar N, Doustimotlagh AH (2020) Renoprotective effects of Origanum majorana methanolic L and carvacrol on ischemia/reperfusion-induced kidney injury in male rats. Evid Based Complement Altern Med. https://doi.org/10.1155/2020/9785932
Yoon E, Babar A, Choudhary M, Kutner M, Pyrsopoulos N (2016) Acetaminophen-induced hepatotoxicity: a comprehensive update. J Clin Transl Hepatol 4(2):131. https://doi.org/10.14218/JCTH.2015.00052
Bozkurt M, Em S, Oktayoglu P, Turkcu G, Yuksel H, Sarıyıldız MA, Caglayan M, Batmaz İ, Nas K, Bozkurt Y (2014) Carvacrol prevents methotrexate-induced renal oxidative injury and renal damage in rats. Clin Invest Med. https://doi.org/10.25011/cim.v37i1.20865
Suganthi RU, Manpal S (2013) Biological and pharmacological of actions carvacrol and its effects on poultry: an updated review. World J Pharm Pharm Sci 2(2013):3581–3595
Potočnjak I, Domitrović R (2016) Carvacrol attenuates acute kidney injury induced by cisplatin through suppression of ERK and PI3K/Akt activation. Food Chem Toxicol 98:251–261. https://doi.org/10.1016/j.fct.2016.11.004
El-Sayed EM, Abd-Allah AR, Mansour AM, EL-Arabey AM (2015) Thymol and carvacrol prevent cisplatin-induced nephrotoxicity by abrogation of oxidative stress, inflammation, and apoptosis in rats. J Biochem Mol Toxicol 29(4):165–172. https://doi.org/10.1002/jbt.21681
Acknowledgements
This study was supported by Rafsanjan University of Medical Sciences (Grant # 97301).
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: JH. Performed the experiments: AK, JH, MR, and AN. Analyzed the data: JH and MR. Contributed reagents/materials/analysis tools: EH, and JH. Wrote the paper: AN, JH and AK.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Consent to participate
All authors voluntarily agreed to participate in this study.
Consent to publish
All authors voluntarily agreed to publish the results of this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Najafizadeh, A., Kaeidi, A., Rahmani, M. et al. The protective effect of carvacrol on acetaminophen-induced renal damage in male rats. Mol Biol Rep 49, 1763–1771 (2022). https://doi.org/10.1007/s11033-021-06985-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-021-06985-8