Abstract
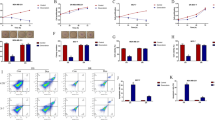
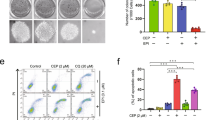
Triple negative breast cancer (TNBC) is a kind of refractory cancer with poor response to conventional chemotherapy. Recently, the combination of baicalein and doxorubicin was reported to exert a synergistic antitumor effect on breast cancer. However, the underlying mechanism how baicalein sensitizes breast cancer cells to doxorubicin remains to be elucidated. Here, it was found that 20 μM baicalein increased the autophagy markers including the ratio of LC3B II/I, GFP-LC3 punctate aggregates and down-regulation of p62 expression, and up-regulated mitophagy marker PINK1 and Parkin in TNBC MDA-MB-231 cells as well. In contrast, doxorubicin decreased the levels of autophagy markers, and significantly up-regulated CDK1 in MDA-MB-231 cells. Pretreatment with baicalein markedly inhibited the doxorubicin-induced decrease in autophagy markers and up-regulation of CDK1, which was reversed by the autophagy inhibitor 3-Methyladenine. Moreover, baicalein alleviated the doxorubicin-induced expression and phosphorylation (at Ser616) of mitochondrial fission protein Drp1. Intriguingly, the autophagy inhibitor 3-Methyladenine also significantly weakened the effect of baicalein on doxorubicin-induced viability decrease and apoptosis in MDA-MB-231 cells. Taken together, our data indicate that baicalein improves the chemosensitivity of TNBC cells to doxorubicin through promoting the autophagy-mediated down-regulation of CDK1, also suggest a novel strategy for prevention of TNBC in the future.









Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 COUNTRIES. CA Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Yin L, Duan JJ, Bian XW, Yu SC (2020) Triple-negative breast cancer molecular subtyping and treatment progress. Breast Cancer Res 22:61. https://doi.org/10.1186/s13058-020-01296-5
Park JH, Ahn JH, Kim SB (2018) How shall we treat early triple-negative breast cancer (TNBC): from the current standard to upcoming immuno-molecular strategies. ESMO Open 3:e000357. https://doi.org/10.1136/esmoopen-2018-000357
Momparler RL, Karon M, Siegel SE, Avila F (1976) Effect of adriamycin on DNA, RNA, and protein synthesis in cell-free systems and intact cells. Cancer Res 36:2891–2895
Darwito D, Dharmana E, Riwanto I, Budijitno S, Suwardjo S, Purnomo J, Widodo I, Ghozali A, Aryandono T, Anwar SL (2019) Effects of omega-3 supplementation on Ki-67 and VEGF expression levels and clinical outcomes of locally advanced breast cancer patients treated with neoadjuvant CAF chemotherapy: a randomized controlled trial report. Asian Pac J Cancer Prev 20:911–916. https://doi.org/10.31557/apjcp.2019.20.3.911
Al-Malky HS, Al Harthi SE, Osman AM (2020) Major obstacles to doxorubicin therapy: cardiotoxicity and drug resistance. J Oncol Pharm Pract 26:434–444. https://doi.org/10.1177/1078155219877931
Lao J, Madani J, Puértolas T, Alvarez M, Hernández A, Pazo-Cid R, Artal A, Antón Torres A (2013) Liposomal doxorubicin in the treatment of breast cancer patients: a review. J Drug Deliv 2013:456409. https://doi.org/10.1155/2013/456409
Liu H, Wang H, Xiang D, Guo W (2017) Pharmaceutical measures to prevent doxorubicin-induced cardiotoxicity. Mini Rev Med Chem 17:44–50. https://doi.org/10.2174/1389557516666160621083659
Abushouk AI, Ismail A, Salem AMA, Afifi AM, Abdel-Daim MM (2017) Cardioprotective mechanisms of phytochemicals against doxorubicin-induced cardiotoxicity. Biomed Pharmacother 90:935–946. https://doi.org/10.1016/j.biopha.2017.04.033
Sahu BD, Kumar JM, Kuncha M, Borkar RM, Srinivas R, Sistla R (2016) Baicalein alleviates doxorubicin-induced cardiotoxicity via suppression of myocardial oxidative stress and apoptosis in mice. Life Sci 144:8–18. https://doi.org/10.1016/j.lfs.2015.11.018
Otto T, Sicinski P (2017) Cell cycle proteins as promising targets in cancer therapy. Nat Rev Cancer 17:93–115. https://doi.org/10.1038/nrc.2016.138
Ding L, Cao J, Lin W, Chen H, Xiong X, Ao H, Yu M, Lin J, Cui Q (2020) The roles of cyclin-dependent kinases in cell-cycle progression and therapeutic strategies in human breast cancer. Int J Mol Sci. https://doi.org/10.3390/ijms21061960
Lu Y, Yang G, Xiao Y, Zhang T, Su F, Chang R, Ling X, Bai Y (2020) Upregulated cyclins may be novel genes for triple-negative breast cancer based on bioinformatic analysis. Breast Cancer 27:903–911. https://doi.org/10.1007/s12282-020-01086-z
Liu Y, Zhu YH, Mao CQ, Dou S, Shen S, Tan ZB, Wang J (2014) Triple negative breast cancer therapy with CDK1 siRNA delivered by cationic lipid assisted PEG-PLA nanoparticles. J Control Release 192:114–121. https://doi.org/10.1016/j.jconrel.2014.07.001
Xia Q, Cai Y, Peng R, Wu G, Shi Y, Jiang W (2014) The CDK1 inhibitor RO3306 improves the response of BRCA-proficient breast cancer cells to PARP inhibition. Int J Oncol 44:735–744. https://doi.org/10.3892/ijo.2013.2240
Herrero-Ruiz J, Mora-Santos M, Giráldez S, Sáez C, Japón MA, Tortolero M, Romero F (2014) βTrCP controls the lysosome-mediated degradation of CDK1, whose accumulation correlates with tumor malignancy. Oncotarget 5:7563–7574. https://doi.org/10.18632/oncotarget.2274
Galindo-Moreno M, Giráldez S, Sáez C, Japón M, Tortolero M, Romero F (2017) Both p62/SQSTM1-HDAC6-dependent autophagy and the aggresome pathway mediate CDK1 degradation in human breast cancer. Sci Rep 7:10078. https://doi.org/10.1038/s41598-017-10506-8
Han XJ, Yang ZJ, Jiang LP, Wei YF, Liao MF, Qian Y, Li Y, Huang X, Wang JB, Xin HB, Wan YY (2015) Mitochondrial dynamics regulates hypoxia-induced migration and antineoplastic activity of cisplatin in breast cancer cells. Int J Oncol 46:691–700. https://doi.org/10.3892/ijo.2014.2781
Smith AG, Macleod KF (2019) Autophagy, cancer stem cells and drug resistance. J Pathol 247:708–718. https://doi.org/10.1002/path.5222
Yan C, Li TS (2018) Dual role of mitophagy in cancer drug resistance. Anticancer Res 38:617–621. https://doi.org/10.21873/anticanres.12266
Taguchi N, Ishihara N, Jofuku A, Oka T, Mihara K (2007) Mitotic phosphorylation of dynamin-related GTPase Drp1 participates in mitochondrial fission. J Biol Chem 282:11521–11529. https://doi.org/10.1074/jbc.M607279200
Liang X, Wang S, Wang L, Ceylan AF, Ren J, Zhang Y (2020) Mitophagy inhibitor liensinine suppresses doxorubicin-induced cardiotoxicity through inhibition of Drp1-mediated maladaptive mitochondrial fission. Pharmacol Res 157:104846. https://doi.org/10.1016/j.phrs.2020.104846
Gharanei M, Hussain A, Janneh O, Maddock H (2013) Attenuation of doxorubicin-induced cardiotoxicity by mdivi-1: a mitochondrial division/mitophagy inhibitor. PLoS ONE 8:e77713. https://doi.org/10.1371/journal.pone.0077713
Xue C, Wang C, Sun Y, Meng Q, Liu Z, Huo X, Sun P, Sun H, Ma X, Ma X, Peng J, Liu K (2017) Targeting P-glycoprotein function, p53 and energy metabolism: combination of metformin and 2-deoxyglucose reverses the multidrug resistance of MCF-7/Dox cells to doxorubicin. Oncotarget 8:8622–8632. https://doi.org/10.18632/oncotarget.14373
Wang LH, Yang JY, Yang SN, Li Y, Ping GF, Hou Y, Cui W, Wang ZZ, Xiao W, Wu CF (2014) Suppression of NF-κB signaling and P-glycoprotein function by gambogic acid synergistically potentiates adriamycin -induced apoptosis in lung cancer. Curr Cancer Drug Targets 14:91–103. https://doi.org/10.2174/1568009613666131113100634
Chen C, Lu L, Yan S, Yi H, Yao H, Wu D, He G, Tao X, Deng X (2018) Autophagy and doxorubicin resistance in cancer. Anticancer Drugs 29:1–9. https://doi.org/10.1097/cad.0000000000000572
Kong JN, He Q, Wang G, Dasgupta S, Dinkins MB, Zhu G, Kim A, Spassieva S, Bieberich E (2015) Guggulsterone and bexarotene induce secretion of exosome-associated breast cancer resistance protein and reduce doxorubicin resistance in MDA-MB-231 cells. Int J Cancer 137:1610–1620. https://doi.org/10.1002/ijc.29542
Thi-Kim Nguyen Y, Moon JY, Ryu JY, Eum S, Bach TT, Cho SK (2019) Methanol extract of aerial parts of Pavetta indica L enhances the cytotoxic effect of doxorubicin and induces radiation sensitization in MDA-MB-231 triple-negative breast cancer cells. Molecules. https://doi.org/10.3390/molecules24122273
Takashima S, Saito H, Takahashi N, Imai K, Kudo S, Atari M, Saito Y, Motoyama S, Minamiya Y (2014) Strong expression of cyclin B2 mRNA correlates with a poor prognosis in patients with non-small cell lung cancer. Tumour Biol 35:4257–4265. https://doi.org/10.1007/s13277-013-1556-7
Kim SJ, Nakayama S, Shimazu K, Tamaki Y, Akazawa K, Tsukamoto F, Torikoshi Y, Matsushima T, Shibayama M, Ishihara H, Noguchi S (2012) Recurrence risk score based on the specific activity of CDK1 and CDK2 predicts response to neoadjuvant paclitaxel followed by 5-fluorouracil, epirubicin and cyclophosphamide in breast cancers. Ann Oncol 23:891–897. https://doi.org/10.1093/annonc/mdr340
Liu H, Dong Y, Gao Y, Du Z, Wang Y, Cheng P, Chen A, Huang H (2016) The fascinating effects of baicalein on cancer: a review. Int J Mol Sci. https://doi.org/10.3390/ijms17101681
Wu JY, Tsai KW, Li YZ, Chang YS, Lai YC, Laio YH, Wu JD, Liu YW (2013) Anti-bladder-tumor effect of baicalein from scutellaria baicalensis georgi and its application in vivo. Evid Based Complement Alternat Med 2013:579751. https://doi.org/10.1155/2013/579751
Guo Z, Hu X, Xing Z, Xing R, Lv R, Cheng X, Su J, Zhou Z, Xu Z, Nilsson S, Liu Z (2015) Baicalein inhibits prostate cancer cell growth and metastasis via the caveolin-1/AKT/mTOR pathway. Mol Cell Biochem 406:111–119. https://doi.org/10.1007/s11010-015-2429-8
Chandrashekar N, Selvamani A, Subramanian R, Pandi A, Thiruvengadam D (2012) Baicalein inhibits pulmonary carcinogenesis-associated inflammation and interferes with COX-2, MMP-2 and MMP-9 expressions in-vivo. Toxicol Appl Pharmacol 261:10–21. https://doi.org/10.1016/j.taap.2012.02.004
Hsu SL, Hsieh YC, Hsieh WC, Chou CJ (2001) Baicalein induces a dual growth arrest by modulating multiple cell cycle regulatory molecules. Eur J Pharmacol 425:165–171. https://doi.org/10.1016/s0014-2999(01)01144-x
Zhang S, Bao Y, Ju X, Li K, Shang H, Ha L, Qian Y, Zou L, Sun X, Li J, Wang Q, Fan Q (2015) BA-j as a novel CDK1 inhibitor selectively induces apoptosis in cancer cells by regulating ROS. Sci Rep 5:13626. https://doi.org/10.1038/srep13626
Yan W, Ma X, Zhao X, Zhang S (2018) Baicalein induces apoptosis and autophagy of breast cancer cells via inhibiting PI3K/AKT pathway in vivo and vitro. Drug Des Devel Ther 12:3961–3972. https://doi.org/10.2147/dddt.S181939
Chen M, Peng L, Gong P, Zheng X, Sun T, Zhang X, Huo J (2021) Baicalein mediates mitochondrial autophagy via miR-30b and the NIX/BNIP3 signaling pathway in Parkinson’s disease. Biochem Res Int 2021:2319412. https://doi.org/10.1155/2021/2319412
Catanzaro MP, Weiner A, Kaminaris A, Li C, Cai F, Zhao F, Kobayashi S, Kobayashi T, Huang Y, Sesaki H, Liang Q (2019) Doxorubicin-induced cardiomyocyte death is mediated by unchecked mitochondrial fission and mitophagy. Faseb j 33:11096–11108. https://doi.org/10.1096/fj.201802663R
Funding
This work was supported by National Natural Science Foundation of China (81472371), Jiangxi Province Major discipline and academic leaders training Program Project (20172BCB22028), the Research Fund for Jiangxi Geriatric Clinical Medical Research Center (2020BCG74003), Key Research and Development Program of Jiangxi Province (20192BBG70049), Science and Technology Plan Projects of Administration of Traditional Chinese Medicine of Jiangxi Province (2022B063) and the Innovation Fund Designated for Graduate Students of Jiangxi Province (YC2019-S014).
Author information
Authors and Affiliations
Contributions
All authors contributed to this study. The experiments were conceived and designed by XJH and FFT. The cellular and molecular biological experiments were conducted by FH, YYX, XHQ, SSL and KZ. The flow cytometry was performed by SSL, CZ and JLH. Data collection and analysis were performed by YZ, LPJ and YYW. The first draft of the manuscript was written by XJH and FFT, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Consent to participate
Not applicable.
Consent for publication
We would like to declare on behalf of my co-authors that the work was original research that has not been published previously, and not under consideration for publication elsewhere, in whole or in part. The manuscript is approved by all authors for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hua, F., Xiao, YY., Qu, XH. et al. Baicalein sensitizes triple negative breast cancer MDA-MB-231 cells to doxorubicin via autophagy-mediated down-regulation of CDK1. Mol Cell Biochem 478, 1519–1531 (2023). https://doi.org/10.1007/s11010-022-04597-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-022-04597-9