Abstract
Purpose
To evaluate whether ZIP-code level neighborhood socioeconomic status (SES) is associated with adverse pregnancy outcomes.
Methods
A retrospective study of 2009–2014 Oregon Health and Science University (OHSU) births with maternal ZIP codes in one of 89 Portland metropolitan area ZIP codes. Deliveries with ZIP codes outside of the Portland metro area were excluded. Deliveries were stratified by SES based on ZIP code median household income: low (below 10th percentile), medium (11th–89th percentile), and high (above 90th percentile). Univariate analysis and multivariable logistic regression with medium SES as the reference group evaluated perinatal outcomes and strength of association between SES and adverse events.
Results
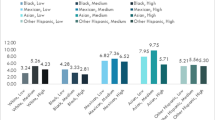
This study included 8118 deliveries with 1654 (20%) classified as low SES, 5856 (72%) medium SES, and 608 (8%) high SES. The low SES group was more likely to be younger, have a higher maternal BMI, have increased tobacco use, identify as Hispanic or Black, and less likely to have private insurance. Low SES was associated with a significantly increased risk of preeclampsia (RR 1.23 95% CI 1.01–1.49), but this was no longer significant after adjusting for confounders (aRR 1.23 95% CI .971–1.55). High SES was negatively associated with gestational diabetes mellitus (GDM), even after adjusting for confounders (aRR 0.710, 95% CI 0.507–0.995).
Conclusion
In the Portland metropolitan area, high SES was associated with a lower risk of GDM. Low SES was associated with a higher risk of preeclampsia before accounting for covariates. ZIP code-based risk assessment may be a useful indicator in detecting healthcare disparities.
Significance
Low socioeconomic status (SES) is associated with adverse pregnancy outcomes. However, literature exploring neighborhood SES and pregnancy outcomes, particularly using Neighborhood Socioeconomic Status and Perinatal Outcomes ZIP code as a SES surrogate, is limited. Our study suggests that even within a single metropolitan area living in a ZIP-code in the lowest 10th percentile SES is associated with preeclampsia. However, this association is no longer significant after adjusting for confounders such as BMI and tobacco use, suggesting these lifestyle factors may be playing a role in preeclampsia in low SES populations. Understanding this relationship may help guide counseling for this vulnerable population.
Similar content being viewed by others
Data Availability (data transparency)
Data was abstracted from patient EHR and is managed in a departmental RedCap database.
Code Availability (software application or custom code)
The code used for statistical analysis in STATA was written by Dr. Amy Valent.
References
Adhikari, K., Patten, S. B., Williamson, T., Patel, A. B., Premji, S., Tough, S., Letourneau, N., Giesbrecht, G., & Metcalfe, A. (2019). Does neighborhood socioeconomic status predict the risk of preterm birth? A community-based canadian cohort study. BMJ open, 9(2), e025341–e025341. https://doi.org/10.1136/bmjopen-2018-025341.
Airaksinen, J., Hakulinen, C., Pulkki-Råback, L., Lehtimäki, T., Raitakari, O. T., Keltikangas-Järvinen, L., & Jokela, M. (2016). Neighbourhood effects in health behaviours: A test of social causation with repeat-measurement longitudinal data. European journal of public health, 26(3), 417–421. https://doi.org/10.1093/eurpub/ckv210.
Anna, V., Van Der Ploeg, H. P., Cheung, N. W., Huxley, R. R., & Bauman, A. E. (2008). Sociodemographic correlates of the increasing Trend in Prevalence of Gestational Diabetes Mellitus in a large Population of Women between 1995 and 2005. Diabetes Care, 31(12), 2288–2293. https://doi.org/10.2337/dc08-1038.
Barker, D. J. P. (2006). Adult consequences of fetal growth restriction. Clinical obstetrics and gynecology, 49(2), 270–283. https://doi.org/10.1097/00003081-200606000-00009.
Bongaarts, J. (2016). United Nations Statistics Division The World’s Women 2015: Trends and Statistics New York: United Nations, 2015. 260 p. In (Vol. 42, pp. 154–154): Wiley Subscription Services, Inc.
Boubred, F., Pauly, V., Romain, F., Fond, G., Boyer, L., & Farrar, D. (2020). The role of neighbourhood socioeconomic status in large for gestational age. PloS One, 15(6), e0233416–e0233416. https://doi.org/10.1371/journal.pone.0233416.
Christensen, M. A., & Haeffner, M. (2021). Feminization of poverty: Causes and implications (pp. 368–377). Cham: Cham: Springer International Publishing.
Clayborne, Z. M., Giesbrecht, G. F., Bell, R. C., & Tomfohr-Madsen, L. M. (2017). Relations between neighbourhood socioeconomic status and birth outcomes are mediated by maternal weight. Social Science & Medicine, 175, 143–151. https://doi.org/10.1016/j.socscimed.2016.12.041.
Cullinan, J., Gillespie, P., Owens, L., Avalos, G., & Dunne, F. P. (2012). Is there a socioeconomic gradient in the prevalence of gestational diabetes mellitus? Irish medical journal, 105(5 Suppl), 21.
Greiner, K. J., Speranza, R. J., Rincon, M., & Burwick, R. M. (2018). 640: Impact of insurance status on outcomes in women with hypertensive disorders in pregnancy. American journal of obstetrics and gynecology, 218(1), S381–S382. https://doi.org/10.1016/j.ajog.2017.11.169.
Hilmers, A., Hilmers, D. C., & Dave, J. (2012). Neighborhood Disparities in Access to Healthy Foods and their Effects on Environmental Justice. American journal of public health (1971), 102(9), 1644–1654. https://doi.org/10.2105/AJPH.2012.300865.
Jimenez, M. P., Wellenius, G. A., Subramanian, S. V., Buka, S., Eaton, C., Gilman, S. E., & Loucks, E. B. (2019). Longitudinal associations of neighborhood socioeconomic status with cardiovascular risk factors: A 46-year follow-up study. Social science & medicine (1982), 241, 112574–112574. https://doi.org/10.1016/j.socscimed.2019.112574
Jolly, M., Mikolaitis, R. A., Shakoor, N., Fogg, L. F., & Block, J. A. (2010). Education, Zip Code-based annualized Household Income, and Health Outcomes in patients with systemic Lupus Erythematosus. The Journal of Rheumatology, 37(6), 1150. https://doi.org/10.3899/jrheum.090862.
Kim, M. K., Lee, S. M., Bae, S. H., Kim, H. J., Lim, N. G., Yoon, S. J., Lee, J. Y., & Jo, M. W. (2018). Socioeconomic status can affect pregnancy outcomes and complications, even with a universal healthcare system. International journal for equity in health, 17(1), 2–2. https://doi.org/10.1186/s12939-017-0715-7.
Larrañaga, I., Santa-Marina, L., Begiristain, H., Machón, M., Vrijheid, M., Casas, M., Tardón, A., Fernández-Somoano, A., Llop, S., Rodriguez-Bernal, C. L., & Fernandez, M. F. (2013). Socio-Economic Inequalities in Health, Habits and Self-Care during pregnancy in Spain. Maternal and child health journal, 17(7), 1315–1324. https://doi.org/10.1007/s10995-012-1134-4.
Lisonkova, S. M. D. P., & Joseph, K. S. M. D. P. (2013). Incidence of preeclampsia: Risk factors and outcomes associated with early- versus late-onset disease. American journal of obstetrics and gynecology, 209(6), 544. .e541-544.e512.
Morland, K., Wing, S., Roux, D., A., & Poole, C. (2002). Neighborhood characteristics associated with the location of food stores and food service places. American journal of preventive medicine, 22(1), 23–29. https://doi.org/10.1016/S0749-3797(01)00403-2.
Nahum Sacks, K., Friger, M., Shoham-Vardi, I., Spiegel, E., Sergienko, R., Landau, D., & Sheiner, E. (2018). Prenatal exposure to preeclampsia as an independent risk factor for long-term cardiovascular morbidity of the offspring. Pregnancy hypertension, 13, 181–186. https://doi.org/10.1016/j.preghy.2018.06.013.
Phillips, G. S., Wise, L. A., Rich-Edwards, J. W., Stampfer, M. J., & Rosenberg, L. (2013). Neighborhood Socioeconomic Status in Relation to Preterm Birth in a U.S. Cohort of Black Women. Journal of urban health, 90(2), 197–211. https://doi.org/10.1007/s11524-012-9739-x.
Räisänen, S., Gissler, M., Sankilampi, U., Saari, J., Kramer, M. R., & Heinonen, S. (2013). Contribution of socioeconomic status to the risk of small for gestational age infants–a population-based study of 1,390,165 singleton live births in Finland. International journal for equity in health, 12(1), 28–28. https://doi.org/10.1186/1475-9276-12-28.
Robert, S. A. (1999). Socioeconomic position and health: The Independent Contribution of Community Socioeconomic Context. Annual review of sociology, 25(1), 489–516. https://doi.org/10.1146/annurev.soc.25.1.489.
Silva, L., Coolman, M., Steegers, E., Jaddoe, V., Moll, H., Hofman, A., Mackenbach, J., & Raat, H. (2008). Low socioeconomic status is a risk factor for preeclampsia: The Generation R Study. Journal of hypertension, 26(6), 1200–1208. https://doi.org/10.1097/HJH.0b013e3282fcc36e.
US Census Bureau (2019). Poverty status in the past 12 months.
Vinikoor-Imler, L. C., Messer, L. C., Evenson, K. R., & Laraia, B. A. (2011). Neighborhood conditions are associated with maternal health behaviors and pregnancy outcomes. Social science & medicine (1982), 73(9), 1302–1311. https://doi.org/10.1016/j.socscimed.2011.08.012.
Yu, Y., Verfuerden, M., Hardelid, P., Zylbersztejn, A., Liew, Z., Olsen, J., Gilbert, R., Li, J., & Fu, B. (2017). Maternal socioeconomic status and infant mortality with low birth weight as a mediator: An inter-country comparison between Scotland and Denmark using administrative data. International journal of population data science, 1(1), https://doi.org/10.23889/ijpds.v1i1.368.
Acknowledgements
The authors would like to thank Brandon Sawyer for assistance with acquisition of Portland, OR Census data.
Funding
No Funding was received for this project.
Author information
Authors and Affiliations
Contributions
Study design and data collection were performed by Deepraj Pawar, Minhazur Sarker and Amy Valent. The first draft of the manuscript was written by Deepraj Pawar and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to disclose.
Ethics Approval (include appropriate approvals or waivers)
Our study was approved by the Oregon Health and Science University institutional review board (IRB 1545).
Consent to Participate (include appropriate consent statements)
Our IRB deems minimal risk based on the deidentified nature of the database.
Consent for Publication
Our IRB deems minimal risk based on the deidentified nature of the database.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was accepted as an abstract and presented as a poster at American College of Obstetricians and Gynecologists Virtual Conference on October 30–31, 2020 Acknowledgements: The authors would like to thank Brandon Sawyer for assistance with acquisition of Portland, OR Census data.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pawar, D.K., Sarker, M., Caughey, A.B. et al. Influence of Neighborhood Socioeconomic Status on Adverse Outcomes in Pregnancy. Matern Child Health J 27, 1401–1406 (2023). https://doi.org/10.1007/s10995-023-03701-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-023-03701-9