Abstract
Objectives
To describe the current unmet major depression and substance use disorder (SUD) treatment needs among reproductive age women
Methods
Data from the 2007 to 2014 National Survey on Drug Use and Health (NSDUH) were analyzed to determine proportions of women ages 18 to 44 years with unmet treatment need for depression and SUD. Logistic regression determined factors associated with receiving past year SUD and major depression treatment among those in need.
Results
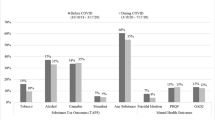
Only 9.2% of women with past year SUD treatment need received treatment (95% CI 8.3–10.1%) compared to 60.7% for those in need of depression treatment (95% CI 59.5–62.0%). Over time, treatment receipt for depression increased significantly (OR 1.4, 95% CI 1.15–1.67) but not for substance use disorders (OR 1.4, 95% CI 0.69–1.45). Neither pregnant nor parenting women were more likely to receive treatment for SUD or depression. Young and racial/ethnically minority women were less likely to receive needed behavioral health treatment for either condition.
Conclusions
Depression and SUD treatment need are common among women. However, treatment receipt differs between these behavioral health conditions.

Similar content being viewed by others
References
ACOG. (2015). The American College of Obstetricians and Gynecologists Committee Opinion no. 630. Screening for perinatal depression. Obstetrics & Gynecology,125(5), 1268–1271. https://doi.org/10.1097/01.AOG.0000465192.34779.dc.
Ahmed, A., Bowen, A., Feng, C. X., & Muhajarine, N. (2019). Trajectories of maternal depressive and anxiety symptoms from pregnancy to five years postpartum and their prenatal predictors. BMC Pregnancy Childbirth,19(1), 26. https://doi.org/10.1186/s12884-019-2177-y.
Barry, C. L., McGinty, E. E., Pescosolido, B. A., & Goldman, H. H. (2014). Stigma, discrimination, treatment effectiveness, and policy: Public views about drug addiction and mental illness. Psychiatric Services (Washington, D. C.),65(10), 1269–1272. https://doi.org/10.1176/appi.ps.201400140.
CDC-Foundation. (2018). Building U.S. capacity to review and prevent maternal deaths. Retrieved September 4, 2018 from https://reviewtoaction.org/2018_Report_from_MMRCs.
Coleman-Cowger, V. H., Oga, E. A., Peters, E. N., Trocin, K. E., Koszowski, B., & Mark, K. (2019). Accuracy of three screening tools for prenatal substance use. Obstetrics & Gynecology,133(5), 952–961. https://doi.org/10.1097/aog.0000000000003230.
Cox, E. Q., Sowa, N. A., Meltzer-Brody, S. E., & Gaynes, B. N. (2016). The Perinatal depression treatment cascade: Baby steps toward improving outcomes. Journal of Clinical Psychiatry,77(9), 1189–1200. https://doi.org/10.4088/JCP.15r10174.
Creedon, T. B., & Cook, B. L. (2016). Access to mental health care increased but not for substance use while disparities remain. Health Affairs (Millwood),35(6), 1017–1021. https://doi.org/10.1377/hlthaff.2016.0098.
Crisp, A., Gelder, M., Goddard, E., & Meltzer, H. (2005). Stigmatization of people with mental illnesses: A follow-up study within the changing minds campaign of the Royal College of Psychiatrists. World Psychiatry,4(2), 106–113.
Curry, S. J., Krist, A. H., Owens, D. K., Barry, M. J., Caughey, A. B., Davidson, K. W.,… Wong, J. B. (2019). Interventions to prevent perinatal depression: US preventive services task force recommendation Statement. Jama, 321(6), 580–587. https://doi.org/10.1001/jama.2019.0007https://doi.org/10.1001/jama.2019.0007
Gavin, N. I., Gaynes, B. N., Lohr, K. N., Meltzer-Brody, S., Gartlehner, G., & Swinson, T. (2005). Perinatal depression: A systematic review of prevalence and incidence. Obstetrics and Gynecology,106(5 Pt 1), 1071–1083. https://doi.org/10.1097/01.AOG.0000183597.31630.db.
Gemmill, A., Kiang, M. V., & Alexander, M. J. (2019). Trends in pregnancy-associated mortality involving opioids in the United States, 2007–2016. American Journal of Obstetrics and Gynecology,220(1), 115–116. https://doi.org/10.1016/j.ajog.2018.09.028.
Haight, S. C., Ko, J. Y., Tong, V. T., Bohm, M. K., & Callaghan, W. M. (2018). Opioid use disorder documented at delivery hospitalization—United States, 1999–2014. Morbidity and Mortality Weekly Report,67(31), 845–849. https://doi.org/10.15585/mmwr.mm6731a1.
Howell, E. A., Brown, H., Brumley, J., Bryant, A. S., Caughey, A. B., Cornell, A. M., … Grobman, W. A. (2018). Reduction of peripartum racial and ethnic disparities: A conceptual framework and maternal safety consensus bundle. Journal of Midwifery Womens Health, 63(3), 366–376. https://doi.org/10.1111/jmwh.12756.
Huhn, A. S., Berry, M. S., & Dunn, K. E. (2019). Review: Sex-based differences in treatment outcomes for persons with opioid use disorder. Am J Addict,28(4), 246–261. https://doi.org/10.1111/ajad.12921.
Kotelchuck, M., Cheng, E. R., Belanoff, C., Cabral, H. J., Babakhanlou-Chase, H., Derrington, T. M., … Bernstein, J. (2017). The prevalence and impact of substance use disorder and treatment on maternal obstetric experiences and birth outcomes among singleton deliveries in Massachusetts. Matern Child Health J, 21(4), 893–902. https://doi.org/10.1007/s10995-016-2190-y.
Krans, E. E., Kim, J. Y., James, A. E., 3rd, Kelley, D., & Jarlenski, M. P. (2019). Medication-assisted treatment use among pregnant women with opioid use disorder. Obstetrics and Gynecology,133(5), 943–951. https://doi.org/10.1097/aog.0000000000003231.
Le, T. L., Kenaszchuk, C., Milligan, K., & Urbanoski, K. (2019). Levels and predictors of participation in integrated treatment programs for pregnant and parenting women with problematic substance use. BMC Public Health,19(1), 154. https://doi.org/10.1186/s12889-019-6455-4.
Lean, R. E., Pritchard, V. E., & Woodward, L. J. (2013). Child protection and out-of-home placement experiences of preschool children born to mothers enrolled in methadone maintenance treatment during pregnancy. Children and Youth Services Review,35(11), 1878–1885. https://doi.org/10.1016/j.childyouth.2013.09.003.
Lewkowitz, A. K., Rosenbloom, J. I., Keller, M., Lopez, J. D., Macones, G. A., Olsen, M. A., et al. (2019). Association between severe maternal morbidity and psychiatric illness within 1 year of hospital discharge after delivery. Obstetrics and Gynecology,134(4), 695–707. https://doi.org/10.1097/aog.0000000000003434.
Marsh, J. C., Park, K., Lin, Y. A., & Bersamira, C. (2018). Gender differences in trends for heroin use and nonmedical prescription opioid use, 2007–2014. Journal of Substance Abuse Treatment,87, 79–85. https://doi.org/10.1016/j.jsat.2018.01.001.
Mazure, C. M., & Fiellin, D. A. (2018). Women and opioids: Something different is happening here. Lancet,392(10141), 9–11. https://doi.org/10.1016/s0140-6736(18)31203-0.
Nielsen, T., Bernson, D., Terplan, M., Wakeman, S. E., Yule, A. M., Mehta, P. K.,… Schiff, D. M. (2019). Maternal and infant characteristics associated with maternal opioid overdose in the year following delivery. Addiction. https://doi.org/10.1111/add.14825.
SAMHSA. (2009). 2009 National survey on drug use and health public use data file codebook. Retrieved from Rockville, MD.
SAMHSA. (2017). Behavioral Health Barometer: United States, volume 4: Indicators as measured through the 2015 National Survey on drug use and health and national survey of substance abuse treatment services. Retrieved from Rockville, MD.
Scholl, L., Seth, P., Kariisa, M., Wilson, N., & G, B. (2019). Drug and opioid-involved overdose deaths—United States, 2013–2017.
Siu, A. L., Bibbins-Domingo, K., Grossman, D. C., Baumann, L. C., Davidson, K. W., Ebell, M.,… Pignone, M. P. (2016). Screening for depression in adults: US preventive services task force recommendation statement. JAMA, 315(4), 380–387. https://doi.org/10.1001/jama.2015.18392.
Smid, M. C., Stone, N. M., Baksh, L., Debbink, M. P., Einerson, B. D., Varner, M. W.,… Clark, E. A. S. (2019). Pregnancy-associated death in Utah: Contribution of drug-induced deaths. Obstetrics & Gynecology, 133(6), 1131–1140. https://doi.org/10.1097/aog.0000000000003279.
Terplan, M., Kennedy-Hendricks, A., & Chisolm, M. S. (2015). Prenatal substance use: Exploring assumptions of maternal unfitness. Subst Abuse,9(Suppl 2), 1–4. https://doi.org/10.4137/sart.S23328.
Terplan, M., McNamara, E. J., & Chisolm, M. S. (2012). Pregnant and non-pregnant women with substance use disorders: The gap between treatment need and receipt. Journal of Addictive Diseases,31(4), 342–349. https://doi.org/10.1080/10550887.2012.735566.
Watts, J. R., O'Sullivan, D., & Chatters, S. J. (2018). Strengthening the working alliance for clients with substance use disorders and child maltreatment histories. Journal of Mental Health Counseling,40(1), 58–74. https://doi.org/10.17744/mehc.40.1.05.
Weissman, M. M., & Olfson, M. (1995). Depression in women: Implications for health care research. Science,269(5225), 799–801.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Martin, C.E., Scialli, A. & Terplan, M. Addiction and Depression: Unmet Treatment Needs Among Reproductive Age Women. Matern Child Health J 24, 660–667 (2020). https://doi.org/10.1007/s10995-020-02904-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-020-02904-8