Abstract
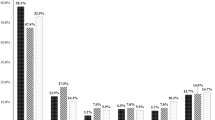
Objectives Substance use during pregnancy is a significant public health issue. Prenatal substance use increased in the past decade while prenatal cigarette smoking has remained stable. Co-use of tobacco and other drugs is a concern because of potential additive risks. This study aims to describe the prevalence rates of substance use among pregnant women and examine the association between smoking status (nonsmoker, recent quitter and current smoker) and other drug use. Methods In this cross-sectional study, pregnant women (n = 500) were recruited from two obstetric practices to complete three substance use screeners and have their urine tested for 12 different drug classes, including cannabis, opioids and cocaine. Participants were divided into three groups based on survey responses: nonsmokers, recent quitters (smoked in the month prior to pregnancy but not past month) and current smokers (past-month). Results Approximately 29% of participants reported smoking in the month before pregnancy. During pregnancy, 17, 12 and 71% were current smokers, recent quitters and nonsmokers respectively. Overall prevalence of illicit or prescription drug use in pregnancy was 27%. Cannabis was the most common drug used in pregnancy with prevalence of 22%, followed by opioids (4%), cocaine (1%), tricyclic antidepressants (TCAs) (1%), amphetamines (1%), and benzodiazepines (1%). On multivariable logistic regression, smoking in pregnancy was associated with a positive urine drug screen; with adjusted odds ratio (aOR) 4.7 (95% CI 2.6–8.3) for current smokers and 1.6 (95% CI 0.8–3.3) for recent quitters. Factors negatively associated with positive drug screen were second and third trimester pregnancies, 0.5 (0.3–0.9) and 0.3 (0.2–0.6) respectively; and employment, 0.5 (0.3–0.8). Conclusions for Practice Co-use of tobacco and illicit drugs, particularly cannabis, is relatively high during pregnancy. Additional research is needed to understand the health implications of co-use versus use of tobacco only. Given the strong association between smoking and other drug use, clinicians should routinely assess for illicit drug use in women who smoke during pregnancy.
Similar content being viewed by others
References
ACOG. (2015). Alcohol abuse and other substance use disorders: Ethical issues in obstetric and gynecologic practice. The American College of Obstetricians and Gynecologists (ACOG). Committee Opinion, Number 633. Retrieved June, 2015, from https://www.acog.org/-/media/Committee-Opinions/Committee-on-Ethics/co633.pdf?dmc=1.
Brown, Q. L., Sarvet, A. L., Shmulewitz, D., Martins, S. S., Wall, M. M., & Hasin, D. S. (2017). Trends in marijuana use among pregnant and nonpregnant reproductive-aged women, 2002–2014. JAMA, 317(2), 207–209.
Chun, J., Haug, N. A., Guydish, J. R., Sorensen, J. L., & Delucchi, K. (2009). Cigarette smoking among opioid-dependent clients in a therapeutic community. The American Journal on Addictions, 18(4), 316–320.
Cnattingius, S. (2004). The epidemiology of smoking during pregnancy: Smoking prevalence, maternal characteristics, and pregnancy outcomes. Nicotine & Tobacco Research, 6(Suppl 2), S125-S140.
Coleman-Cowger, V. H., Oga, E. A., Peters, E. N., Trocin, K., Koszowski, B., & Mark, K. (2018). Comparison and validation of screening tools for substance use in pregnancy: A cross-sectional study conducted in Maryland prenatal clinics. British Medical Journal Open, 8(2), e020248.
Coleman-Cowger, V. H., Schauer, G. L., & Peters, E. N. (2017). Marijuana and tobacco co-use among a nationally representative sample of US pregnant and non-pregnant women: 2005–2014 National Survey on Drug Use and Health findings. Drug & Alcohol Dependence, 177, 130–135.
Crume, T. L., Juhl, A. L., Brooks-Russell, A., Hall, K. E., Wymore, E., & Borgelt, L. M. (2018). Cannabis use during the perinatal period in a state with legalized recreational and medical marijuana: The association between maternal characteristics, breastfeeding patterns, and neonatal outcomes. The Journal of Pediatrics, 197, 90–96.
Curtin, S., & Matthews, T. (2016). Smoking prevalence and cessation before and during pregnancy: Data from the birth certificate, 2014. National Vital Statistics Reports, 65, 1–14.
DHHS. (2001). US Department of Health and Human Services. Women and smoking: A report of the Surgeon General. Rockville, MD: US Department of Health and Human Services, Public Health Service, Office of the Surgeon General.
DHHS. (2013). National survey on drug use and health, 2012. United States Department of Health and Human Services. Substance Abuse and Mental Health Services Administration. Center for Behavioral Health Statistics and Quality.
DHHS. (2014). The health consequences of smoking—50 years of progress: a report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
DHHS. (2017). National Survey on Drug Use and Health, 2016. 34481-v3. Research Triangle Park, NC: RTI International [distributor], 2016–04–02.: United States Department of Health and Human Services. Substance Abuse and Mental Health Services Administration. Center for Behavioral Health Statistics and Quality.
Ebrahim, S. H., & Gfroerer, J. (2003). Pregnancy-related substance use in the United States during 1996–1998. Obstetrics & Gynecology, 101(2), 374–379.
England, L. J., Anderson, B. L., Mahoney, J., Coleman-Cowger, V. H., Melstrom, P., & Schulkin, J. (2014). Screening practices and attitudes of obstetricians-gynecologists toward new and emerging tobacco products. American Journal of Obstetrics & Gynecology, 211(6), 695. e691-e697.
Forray, A. (2016). Substance use during pregnancy. F1000Research. https://doi.org/10.12688/f1000research.7645.1.
Havens, J. R., Simmons, L. A., Shannon, L. M., & Hansen, W. F. (2009). Factors associated with substance use during pregnancy: Results from a national sample. Drug and Alcohol Dependence, 99(1), 89–95.
Hayatbakhsh, M. R., Flenady, V. J., Gibbons, K. S., Kingsbury, A. M., Hurrion, E., Mamun, A. A., & Najman, J. M. (2012). Birth outcomes associated with cannabis use before and during pregnancy. Pediatric Research, 71(2), 215.
Hogue, C. J., Parker, C. B., Willinger, M., Temple, J. R., Bann, C. M., Silver, R. M., et al. (2013). A population-based case-control study of stillbirth: The relationship of significant life events to the racial disparity for African Americans. American Journal of Epidemiology, 177(8), 755–767.
Hogue, C. J. R., & Silver, R. M. (2011). Racial and ethnic disparities in United States: Stillbirth rates: Trends, risk factors, and research needs. Paper Presented at the Seminars in Perinatology.
Holland, C. L., Nkumsah, M. A., Morrison, P., Tarr, J. A., Rubio, D., Rodriguez, K. L., et al. (2016). “Anything above marijuana takes priority”: Obstetric providers’ attitudes and counseling strategies regarding perinatal marijuana use. Patient Education and Counseling, 99(9), 1446–1451.
Holland, C. L., Rubio, D., Rodriguez, K. L., Kraemer, K. L., Day, N., Arnold, R. M., & Chang, J. C. (2016). Obstetric health care providers’ counseling responses to pregnant patient disclosures of marijuana use. Obstetrics and Gynecology, 127(4), 681.
Jaques, S., Kingsbury, A., Henshcke, P., Chomchai, C., Clews, S., Falconer, J., et al. (2014). Cannabis, the pregnant woman and her child: Weeding out the myths. Journal of Perinatology, 34(6), 417.
Jarlenski, M., Barry, C. L., Gollust, S., Graves, A. J., Kennedy-Hendricks, A., & Kozhimannil, K. (2017). Polysubstance use among US women of reproductive age who use opioids for nonmedical reasons. American Journal of Public Health, 107(8), 1308–1310.
Kennare, R., Heard, A., & Chan, A. (2005). Substance use during pregnancy: Risk factors and obstetric and perinatal outcomes in South Australia. Australian and New Zealand Journal of Obstetrics and Gynaecology, 45(3), 220–225.
Keyes, K. M., Wall, M., Cerdá, M., Schulenberg, J., O’malley, P. M., Galea, S., et al. (2016). How does state marijuana policy affect US youth? Medical marijuana laws, marijuana use and perceived harmfulness: 1991–2014. Addiction, 111(12), 2187–2195.
Kharkova, O. A., Grjibovski, A. M., Krettek, A., Nieboer, E., & Odland, J. (2017). Effect of smoking behavior before and during pregnancy on selected birth outcomes among singleton full-term pregnancy: A Murmansk county birth registry study. International Journal of Environmental Research and Public Health, 14(8), 867.
Lai, S., Lai, H., Page, J. B., & McCoy, C. B. (2000). The association between cigarette smoking and drug abuse in the United States. Journal of Addictive Diseases, 19(4), 11–24.
MacDorman, M. F., Kirmeyer, S. E., & Wilson, E. C. (2012). Fetal and perinatal mortality, United States, 2006. National Vital Statistics Reports, 60(8), 1–22.
Mark, K., Desai, A., & Terplan, M. (2016). Marijuana use and pregnancy: Prevalence, associated characteristics, and birth outcomes. Archives of Women’s Mental Health, 19(1), 105–111.
Metz, V. E., Brown, Q. L., Martins, S. S., & Palamar, J. J. (2018). Characteristics of drug use among pregnant women in the United States: Opioid and non-opioid illegal drug use. Drug & Alcohol Dependence, 183, 261–266.
Michels, T. C., & Tiu, A. Y. (2007). Second trimester pregnancy loss. American Family Physician, 76(9), 1341–1346.
Mukherjee, S., Velez Edwards, D. R., Baird, D. D., Savitz, D. A., & Hartmann, K. E. (2013). Risk of miscarriage among black women and white women in a US Prospective Cohort Study. American Journal of Epidemiology, 177(11), 1271–1278.
Osmundson, S. S., Wiese, A., Griffin, M. R., & Grijalva, C. G. (2018). 769: Patterns of opioid use by trimester in pregnancy. American Journal of Obstetrics and Gynecology, 218(1), S460.
Patrick, S. W., Schumacher, R. E., Benneyworth, B. D., Krans, E. E., McAllister, J. M., & Davis, M. M. (2012). Neonatal abstinence syndrome and associated health care expenditures: United States, 2000–2009. JAMA, 307(18), 1934–1940.
Ram, A., Tuten, M., & Chisolm, M. S. (2016). Cigarette smoking reduction in pregnant women with opioid use disorder. Journal of Addiction Medicine, 10(1), 53.
Saitman, A., Park, H.-D., & Fitzgerald, R. L. (2014). False-positive interferences of common urine drug screen immunoassays: A review. Journal of Analytical Toxicology, 38(7), 387–396.
SAMHSA. (2009). The NSDUH report: Substance use among women during pregnancy and following childbirth. Rockville, MD: Substance Abuse and Mental Health Services Administration, Office of Applied Studies.
Terplan, M., & Minkoff, H. (2017). Neonatal abstinence syndrome and ethical approaches to the identifiction of pregnant women who use drugs. Obstetrics and Gynecology, 129(1), 164–167.
Tong, V. T., Dietz, P. M., Morrow, B., D’Angelo, D. V., Farr, S. L., Rockhill, K. M., & England, L. J. (2013). Trends in smoking before, during, and after pregnancy—Pregnancy risk assessment monitoring system, United States, 40 sites, 2000–2010. MMWR Surveillance Summaries, 62(6), 1–19.
USPSTF. (2015). Final update summary: Drug use, illicit: Screening. US Preventive Services Task Force.
Wilcox, A. J., Weinberg, C. R., O’connor, J. F., Baird, D. D., Schlatterer, J. P., Canfield, R. E., et al. (1988). Incidence of early loss of pregnancy. New England Journal of Medicine, 319(4), 189–194.
Acknowledgements
We would like to acknowledge Geraldine Baltazar, Sage Roth, Kathleen Trocin and Gabrielle Robinson for their help in conducting the study.
Funding
The research reported in this article is supported by the National Institute on Drug Abuse (NIDA) of the National Institutes of Health (NIH) Grant under Award Number R01DA041328 (PI-Coleman-Cowger). The content is solely the responsibility of the authors and does not represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Rights and permissions
About this article
Cite this article
Oga, E.A., Mark, K. & Coleman-Cowger, V.H. Cigarette Smoking Status and Substance Use in Pregnancy. Matern Child Health J 22, 1477–1483 (2018). https://doi.org/10.1007/s10995-018-2543-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-018-2543-9