Abstract
Purpose
Non-White workers face more frequent, severe, and disabling occupational and non-occupational injuries and illnesses when compared to White workers. It is unclear whether the return-to-work (RTW) process following injury or illness differs according to race or ethnicity.
Objective
To determine racial and ethnic differences in the RTW process of workers with an occupational or non-occupational injury or illness.
Methods
A systematic review was conducted. Eight academic databases - Medline, Embase, PsycINFO, CINAHL, Sociological Abstracts, ASSIA, ABI Inform, and Econ lit - were searched. Titles/abstracts and full texts of articles were reviewed for eligibility; relevant articles were appraised for methodological quality. A best evidence synthesis was applied to determine key findings and generate recommendations based on an assessment of the quality, quantity, and consistency of evidence.
Results
15,289 articles were identified from which 19 studies met eligibility criteria and were appraised as medium-to-high methodological quality. Fifteen studies focused on workers with a non-occupational injury or illness and only four focused on workers with an occupational injury or illness. There was strong evidence indicating that non-White and racial/ethnic minority workers were less likely to RTW following a non-occupational injury or illness when compared to White or racial/ethnic majority workers.
Conclusions
Policy and programmatic attention should be directed towards addressing racism and discrimination faced by non-White and racial/ethnic minority workers in the RTW process. Our research also underscores the importance of enhancing the measurement and examination of race and ethnicity in the field of work disability management.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Purpose
Race and ethnicity may be differentiating markers of the return-to-work (RTW) experience for injured workers. Research shows inequities in occupational and non-occupational injury and illness across racial and ethnic groups; non-White (or, depending on the context, ‘ethnic minority’) workers face more frequent, severe, and disabling injuries and illnesses when compared to White workers [1,2,3]. RTW represents a series of clinical, policy and organizational activities that transition injured workers back to meaningful employment [4, 5]. Fostering optimal RTW practices represents a critical public health and social policy priority as it ensures that workers can re-enter the labor market following a health-related disruption and regain their financial livelihood, productivity, and well-being. Currently, it is unclear whether the RTW process differs according to race or ethnicity.
Among countries which collect and publish labor market data according to race and ethnicity, including the United States (US), United Kingdom (UK), and Canada, it is estimated that up to a quarter of the workforce consists of non-White workers [6,7,8]. Data also indicate that non-White workers experience significantly greater occupational morbidity [9]. For example, Seabury, Terp and Boden (2016) utilized two large US population-representative datasets to estimate the prevalence of work-related injury and disability by race and ethnicity [1]. Findings indicated that Black and Hispanic workers had a higher prevalence of injury and disability when compared to non-Hispanic White workers in models that adjusted for sex, age, and education. These findings have been replicated in other studies conducted in the US and in other developed labor markets [2, 3]. Research on a range of non-occupational chronic health conditions, such as cancer, cardiovascular disease and depression also indicates that non-White people are more likely to report severe disease symptoms, disability and mortality when compared to their White counterparts [1, 10,11,12,13].
Researchers have sought to examine the factors that contribute to racial and ethnic health inequities. Despite lacking a sound scientific evidence basis, the role of genetics has been routinely brought up as a primary factor that contributes to racial and ethnic differences in health outcomes inside and outside of the workplace. It is important to highlight that while genes might explain why an individual is susceptible to a disease, they cannot explain differences across social groups [13,14,15,16]. Indeed, race and ethnicity are social constructs associated with power and status that play a prominent role in shaping the distribution of social, economic, and health-related resources, including decent and safe work [17]. In cases of occupational morbidity and mortality, which are primarily attributed to workplace conditions, a genetic argument for racial differences cannot be entertained. Studies consistently find that non-White workers are disproportionately employed in occupations characterized by high physical and psychological job demands, and have hazardous working conditions and limited regulatory and labor protections when compared to White workers – a form of racial occupational segregation [12, 17,18,19,20]. Other research highlights that non-White people are exposed to a greater number of risk factors for disease and disability including lower levels of healthcare access, greater levels of stress, lower socioeconomic status, and more barriers to the performance of health-enhancing behaviours when compared to White people [11, 12, 21]. These inequities are widely understood to be the outcomes of systemic racism – or structures, policies, practices, and norms that disadvantage persons of color and contribute to racial health inequities [22, 23].
Despite the disproportionate burden of occupational and non-occupational injury and illness on non-White workers, it is unclear how race and ethnicity impact the RTW process. The RTW process is a series of steps that include injury reporting, seeking medical care and workers’ compensation benefits, accessing rehabilitation services, accommodation planning, work re-integration and stay-at-work [5, 24]. The RTW process occurs within a complex system that includes workplace, clinical and legal settings and a range of actors including workers and their employers, healthcare providers, workers’ compensation representatives and legislators [4, 25]. In an ideal scenario an injured worker will progress through RTW phases in a stepwise fashion [5]. However, some injured workers can face extended or intermittent work disability that results in significant employer and societal costs and can significantly disrupt a worker’s access to income and resources that are important to health and quality of life [26, 27]. Structural and interpersonal racism has the potential to operate throughout the RTW system and in a worker’s interactions with different actors and lead to adverse RTW outcomes [28]. Accordingly, racism may result in disparate RTW outcomes between workers of color and their White counterparts. Using a systematic review process, our study sought to assess whether racial and ethnic inequities contribute to differences in the RTW process among workers with an occupational or non-occupational injury or illness.
Methods
We conducted a systematic review of the literature using a process developed by the Cochrane Collaboration which was adapted by the Institute for Work & Health (IWH) Systematic Review Program [29]. The review methods were registered with PROSPERO and met the 2020 Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) statement guidelines.
Literature Search
The search strategy followed a Population (P), Exposure (E), Comparator, (C) and Outcome (O) (PECO) framework and was designed to capture studies that examined the working population within OECD countries with an occupational or non-occupational injury or illness (P), non-White workers (E), a White worker comparison group (C) and measured any RTW outcome (O) (Table 1). To elaborate on the impact of discrimination according to ethnicity and race in different OECD contexts, we also included studies which compared racial/ethnic minority and majority groups. Research team members provided feedback and helped refine the search strategy. Database-specific controlled vocabulary terms and keywords were included and are available in Supplement 1. The terms within each category were combined using a Boolean OR operator and terms across the four main categories were combined using a Boolean AND operator. Medline (OVID), Embase (OVID), PsycINFO (OVID), CINAHL, Sociological Abstracts, ASSIA, ABI Inform, and Econ lit were searched for English, French or Spanish language articles that were published between January 2001-April 2021. Our decision to focus on articles published after 2000 was made to reflect the growing research on the impact racial and ethnic inequities can play in determining the health of the working population[30]. After removing duplicates, the search yields were combined and imported into the review software DistillerSR to facilitate relevance screening [31].
Relevance Screen
Relevancy screening was informed by our PECO framework. Also, articles were included if they involved primary research, were published ≥ 2001, focused on workers in OECD countries who experienced work disability from an occupational or non-occupational injury or illness, collected information on the race or ethnicity of study participants and measured any dimension of RTW. We included quantitative study designs where RTW outcomes were examined according to race or ethnicity and where a statistical effect estimate was reported. Studies were excluded if they were secondary research, commentaries, editorials, or case studies.
Relevance screening occurred over two steps. First, titles and abstracts of references identified in the search were divided among research team members and were screened independently by two reviewers for relevancy. Due to the large number of studies retrieved by the search, the artificial intelligence (AI) capabilities of DistillerSR were used for title and abstract screening. To train the AI, the first 15% of titles and abstracts were screened independently by two human reviewers to identify studies of relevance to the review. Once the AI was trained, it served as a secondary reviewer to a single human reviewer. Any disagreements between a human reviewer and the AI were resolved by a third (human) reviewer. Articles that met relevance at the first level of screening were carried forward for a full-text review, which was carried out by two human reviewers. Disagreements between the two reviewers were discussed in team meetings. Relevance decisions on title and abstract and full-text screening demonstrated high moderate to high inter-rater reliability, suggesting that reviewers were consistently applying inclusion/exclusion criteria to the screening processes. Reference lists of articles that were examined during full-text review were checked to ensure no relevant articles were missed.
Quality Appraisal and data Extraction
A modified version of a quality assessment tool developed by IWH for systematic reviews in the field of work disability management was used to conduct quality appraisal (Supplement 2). The quality assessment tool consisted of 15 questions that examined internal, external, and statistical validity of each article through an assessment of study design and objectives, recruitment procedures, outcome and exposure measurement and analysis. Questions were added to the tool by the research team to examine the quality of measurement of race and ethnicity and assess sample heterogeneity. Using the tool, each relevant article was appraised by two independent reviewers. A final weighted sum score of the quality criteria was generated and converted to a percentage score. Using the percentage score, studies were categorized as high (≥ 85%), medium (50–84%) or low quality (< 50%). Research team members held meetings to reach consensus on final appraisal scores and rankings. Only studies appraised as high and medium quality were utilized in the evidence synthesize phase. Data were extracted from relevant articles to create summary tables that presented sample description and racial and ethnic breakdown of the study sample, study design, and RTW outcomes.
Evidence Synthesis
Given that studies varied in their length of observation, design, sample characteristics, confounding variables collected and RTW outcomes measured, pooled effect estimates were not calculated. Instead, we undertook a best evidence synthesis approach to examine the impact of race and ethnicity on RTW and generate applied practice messages based on available evidence [32]. Evidence was synthesized to determine levels of evidence using an algorithm that considers the methodological quality (i.e., high, medium, or low methodological quality) and quantity of studies (i.e., number of studies with similar sample characteristics and outcome measures) and the consistency of study findings (i.e., number of studies which produce similar findings) (Table 2). As an example, findings with a strong level of evidence are those where there is a minimum of three high quality studies which have consistent findings. Refer to Table 2 for additional details on how the best evidence synthesis was utilized to determine levels of evidence. According to the best evidence synthesis approach, with a strong level of evidence specific recommendations for policy and practice can be generated. Results supported by a moderate level of evidence contribute to practice considerations. On the other hand, limited, mixed or insufficient evidence levels contribute to a lack of evidence to guide policies or practices.
Results
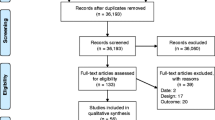
Our search yielded 15,289 articles that were published between 2001 and 2021 after duplicates were removed. After title/abstract screening, 446 articles met initial selection criteria and were carried forward for full-text review. A total of 23 studies were found to meet eligibility criteria. Four sets of studies were grouped together as they utilized the same study sample and asked similar study questions [32,33,34,35,36,37,38,39]. Using the quality appraisal tool, ten studies were of high quality (≥ 85% quality appraisal score) and nine articles were of medium quality (50–84% quality appraisal score). No articles were appraised as being of low quality (< 50% quality appraisal score) (see Fig. 1). When compared to high quality studies, those that were appraised as medium quality had poorly defined recruitment procedures, low study participation rates, were limited in their assessment of race or ethnicity, did not report sample characteristic differences between participants and non-participants and did not collect information on important confounders.
Study Descriptions
A description of studies is presented in Table 3. Most studies were conducted in the US (n = 16); the remaining were conducted in the UK (n = 1) and Israel (n = 2). Fifteen studies focused on workers with non-occupational injury or illness including spine injury (n = 3), cancer (n = 3), limb trauma (n = 2), burn injury (n = 2) and stroke (n = 2). Of the four studies on workers with occupational injury or illness, most focused on low back pain (n = 3) and one examined a broad cohort of compensation claimants. In most studies, White workers were the comparison group (n = 15). An examination of the racial and ethnic breakdown of participants in the studies revealed limited heterogeneity. Thirteen studies included Black, Black non-Hispanic or African American samples (hereafter, collectively referred to as Black) (n = 13). Several studies included samples who were categorized as non-White or other race (n = 8). Eight studies included Hispanic, Latinx or Mexican Americans participants (hereafter, collectively referred to as Latinx). One study consisted of participants who were categorized as American Indian and Alaskan Native, Asian, multiracial and Native Hawaiian and Pacific Islander. Two sets of studies conducted in Israel examined RTW differences between Jewish Israeli and racial/ethnic minority workers including Arab Israelis, immigrants from Soviet Union, and Ethiopian immigrants.
As a primary outcome measure, most studies measured whether workers reported RTW or were employed following injury or illness (n = 13). Other outcomes uncovered in our review included work disability duration (n = 4), receipt of income support following injury or illness (n = 3), total cost and length of workers’ compensation claim (n = 3), hours worked/week following injury or illness (n = 1), involvement in RTW services (n = 1), and financial struggle following injury or illness (n = 1).
Race, Ethnicity and RTW Outcomes
As presented in Table 4, studies consistently showed that non-White or racial/ethnic minority groups reported adverse RTW outcomes following an occupational or non-occupational injury or illness when compared to White or racial/ethnic majority workers.
RTW or Employment Status Following Injury or Illness
Non-White and racial/ethnic minority workers were less likely to report returning to work or being employed following an occupational or non-occupational injury or illness when compared to White and racial/ethnic majority workers. Seven studies indicated that Black workers were less likely to report RTW or being employed following an injury or illness when compared to White workers [35, 39,40,41,42,43,44,45]. One study found that the relationship between race and RTW was statistically significant among those reporting poor quality of surgical outcomes. In this study, no differences in RTW existed between Black or other race participants and White participants among those with favorable surgical outcomes [44]. Also, when compared to White workers, studies found that non-White (n = 2), other race (n = 1), and Latinx (n = 4) workers were less likely to RTW[33, 34, 40, 43, 45,46,47,48]. Studies from Israel highlighted mixed findings. One study found that Arab Israelis were less likely to report RTW at one-month, one-year and 2-years post injury when compared to Jewish Israelis [38, 39]. Another study found that, while differences between Arab and Jewish Israeli workers existed in the likelihood of returning to work, the relationship was not significant when controlling for educational attainment, disability severity or access to legal counsel [36, 37].
Cost and Length of Workers’ Compensation Claim
Two studies indicated that Black workers experiencing an occupational injury or illness were more likely to report a shorter claim duration when compared to their White counterparts [48,49,50,51]. Similarly, Latinx, and other race workers experiencing an occupational injury reported shorter claim durations when compared to White workers with a workplace injury [50, 51]. Additionally, total awarded workers’ compensation settlement following an occupational injury were less for Black, Latinx, and other race workers when compared to White workers [51]. One study of workers’ compensation claimants in the US found that in the absence of legal representation, Black workers indicated lower temporary total disability costs related to low back pain when compared to White workers [52].
Length of Disability Absence
One study using a large US-based population-level dataset found that Black male workers were more likely to report more missed workdays due to injury or illness when compared White workers. On the other hand, no significant difference existed between Black women when compared to White women. The same study found that Latinx men experienced more missed workdays when compared to White men, but this difference was not statistically significant in multivariable models [53]. Another study found that Arab Israelis and Ethiopian Immigrants in Israel experienced a longer disability duration when compared to Jewish Israeli workers [38, 39].
Income Support
Studies of workers experiencing a work disability due to an occupational injury or illness found that Black workers were more likely to receive social security disability insurance, or a temporary disability payment compared to White workers [35, 49, 50].
Work Hours Following RTW
One study indicated that Black participants worked fewer hours following a non-occupational injury when compared to White participants [41].
Financial Struggle
A single study found that Black workers injured on the job were more likely to report post-settlement financial struggle when compared to White workers [49, 50].
Involvement in RTW Services
Only one study examined the relationship between race and involvement in RTW services [54]. In a study of disability insurance beneficiaries, Black and Latinx participants were more likely to be enrolled in employment services when compared to White participants. Additionally, Black participants were more likely to start and complete a trial work period when compared to White participants [54].
Evidence Synthesis
For each RTW outcome identified in our review results were synthesized to generate key messages and practice recommendations when an adequate quantity and quality of studies existed (Table 5). Findings were first pooled broadly to compare differences between non-White or racial/ethnic minority workers and White or racial/ethnic majority workers. A strong level of evidence existed which highlighted that non-White or racial/ethnic minority workers were less likely to RTW following a non-occupational injury or illness when compared to White or racial/ethnic majority workers (3 high quality studies [H] and 7 medium quality studies [M]). Of note, from the samples of studies there were a sufficient quantity of studies focusing specifically on Black and Latinx workers to synthesize evidence. Findings from these studies indicated that Black worker (moderate levels of evidence; 2 H and 3 M) and Latinx workers (limited levels of evidence; 1 H and 1 M) were less likely to report RTW when compared to White workers following a non-occupational injury or illness. Limited, mixed, or insufficient evidence exists on racial or ethnic inequities on the other RTW outcomes identified and corresponding practice messages could not be developed. Of note, there was insufficient evidence examining racial or ethnic differences across RTW outcomes for studies focusing on workers with occupational injuries or illnesses.
Discussion
Examining and addressing the barriers to RTW following injury or illness represents a critical labor market priority and has important population health implications. Our study sought to examine the relationship between race and ethnicity and RTW. Despite the disproportionate burden of occupational and non-occupational injury or illness faced by non-White and minority ethnic workers highlighted in past research [1,2,3], our systematic review showed that race and ethnicity have been underexplored when it comes to RTW. The research we uncovered highlighted disadvantages faced by non-White and racial/ethnic minority workers in returning to work after a non-occupational injury or illness. Strategies addressing the unique RTW obstacles faced by non-White and ethnic minority workers re-entering employment following an injury or illness are critical. Our research also highlights the importance of enhancing the measurement and examination of race and ethnicity in the work disability management field.
Research has consistently highlighted that non-White workers report more frequent and severe occupational injury or illness when compared to their White counterparts [1,2,3]. Racism and discrimination have been at the heart of these health inequities and represent structural determinants that shape physical and mental health among non-White and racial/ethnic minority workers [22, 23]. To our knowledge, this systematic review is the first of its kind to synthesize evidence concerning the impact of racial and ethnic inequities on the RTW process. Our research uncovered 19 published studies that examined racial and ethnic difference in RTW. The relatively small number of studies offers a limited evidence base that can inform the design of organizational work disability management programs and policies to meet the needs of non-White and minority racial/ethnic workers. It is also important to highlight that most studies in our review examined RTW among workers with a non-occupational injury or illness. Less information was available on the experiences of those injured at work. Also, limited research addressed a broader range of RTW outcomes including healthcare utilization, access to workers’ compensation and income support, accommodation planning and stay-at-work. It is recommended that data on race and ethnicity be routinely collected to enhance our understanding of the challenges faced by workers across different phases of the RTW process and to enhance strategies that address inequities in work disability management that are related to race and ethnicity [55].
A key finding from our study was that non-White and racial/ethnic minority workers with a non-occupational injury were less likely to RTW when compared to White or majority racial/ethnic workers. When looking at specific racial groups, our review found a moderate level of evidence suggesting that Black workers with a non-occupational injury or illness were less likely to RTW when compared to White workers. Our findings align with a body of evidence which show disadvantage faced by Black and non-White people in accessing care and social policy supports stemming from racism and discrimination [55,56,57,58]. Unclear from the available research is an explanation of how racial inequities specifically impact RTW. Non-White workers may be more likely to be exposed to a system of forces that contribute to more severe and disabling injury or illness and create obstacles to accessing healthcare access and other resources that support work re-entry when compared to their White counterparts [23]. Findings can also be contextualized through the theory of racial capitalism which describe racism as an underlying dimension of the design of capitalist labor markets [59]. Racial divisions of labor can reinforce adverse working conditions for non-White and racial/ethnic minority workers and mean that they are more likely to work in demanding and less supportive employment environments when compared to White or racial/ethnic majority workers. Through the lens of racial capitalism, it can be posited that non-White workers are more likely to be exposed to work disability managements systems that are disadvantageous and may make returning to work more challenging [60, 61]. More research is required to understand the mechanisms by which racial inequities may contribute to barriers at different phases of the RTW process.
Through the application of a best evidence synthesis approach, our systematic review points to the importance of designing policies and programs which address the RTW challenges of non-White and racial/ethnic minorities with a non-occupational injury or illness. To address racial and ethnic inequities in RTW, an anti-racist approach to work disability management may be adopted [62]. Anti-racism interventions are defined as action-oriented educational or policy-level strategies that identify racial inequities and make systemic and political change to addresses interlocking systems of social oppression [23]. Increasingly, anti-racism interventions are being applied to diverse healthcare settings to address the multiple pathways in which racism can impact access to healthcare services, including individual (e.g., training on providing culturally competent care), community (e.g., actively engage non-White and racial/ethnic minority communities in program planning and delivery), organizational (e.g., leadership towards anti-racist strategic goals) and policy change (e.g., meaningful involvement of non-White and racial/ethnic minority people in policy change) [63]. An anti-racist approach can provide a multifaced and action-oriented view for work disability management professionals to address the diverse structural challenges faced by non-White and minority racial/ethnic workers in the RTW process.
Strengths of this review included the utilization of a rigorous systematic review methodology that was designed specifically for the field of work disability management. There were also limitations that should be considered. To address our research objectives, we included peer-reviewed quantitative studies and excluded qualitative studies and gray literature. Additional research is required to synthesize other forms of evidence to enhance our understanding of the RTW experience following an occupational or non-occupational injury or illness for non-White and ethnic minority workers and to expand on the role of racism and discrimination. We utilized a quality appraisal tool to evaluate the internal, external, and statistical validity of each study. At the same time, the tool may have been limited in its ability to assess the measurement of race and ethnicity. It is recommended that quality appraisal tools be enhanced through the design and inclusion of questions which appropriately assess the racial and ethnic diversity of study samples and quality of measurement of racism and discrimination.
RTW following an injury or illness is a complex process that can be shaped by worker characteristics and contextual factors. Our systematic review brings to the forefront the role that race and ethnicity play in the RTW process and the structural conditions that can disadvantage different worker groups. RTW inequities for non-White and minority racial/ethnic workers experiencing a non-occupational injury or illness identified in our review underscore the need for RTW policies and programs that are sensitive to race and ethnicity. Importantly, our study calls for greater attention to the measurement of race and ethnicity in RTW and the generation of an evidence base that can inform the design of equitable work disability management practices.
References
Seabury SA, Terp S, Boden LI. Racial and ethnic differences in the frequency of workplace injuries and prevalence of work-related disability. Health Aff (Millwood). 2017;36(2):266–73.
Baron SL, Steege AL, Marsh SM, Menéndez CC, Myers JR, Centers for Disease Control and Prevention (CDC). Nonfatal work-related injuries and illnesses—United States, 2010. MMWR Suppl. 2013;62(3):35–40.
Marsh SM, Menéndez CC, Baron SL, Steege AL, Myers JR, Control CfD, et al. Fatal work-related injuries-United States, 2005–2009. MMWR Suppl. 2013;62(3):41–5.
Jetha A, Pransky G, Fish J, Hettinger LJ. Return-to-work within a complex and dynamic organizational work disability system. J Occup Rehabil. 2016;26(3):276–85.
Young AE, Roessler RT, Wasiak R, McPherson KM, van Poppel MNM, Anema JR. A developmental conceptualization of return to work. J Occup Rehabil. 2005;15(4):557–68.
US Bureau of Labor Statistics. Labor force characteristics by race and ethnicity, 2020 Washington (DC): US Department of Labor; 2021 [updated 2021 Nov; cited 2022 Oct 1]. Available from: https://www.bls.gov/opub/reports/race-and-ethnicity/2020/home.htm.
UK Government. Employment [Internet]. England, Wales and Scotland (UK): Office for National Statistics; 2022 [updated 2022 Nov 3; cited 2022 Oct 1]. Available from: https://www.ethnicity-facts-figures.service.gov.uk/work-pay-and-benefits/employment/employment/latest#:~:text=76%25%20of%20people%20aged%2016,out%20of%20all%20ethnic%20groups.
Statistics Canada. Labour force characteristics by visible minority group, three-month moving averages, monthly, unadjusted for seasonality [database]. Ottawa (ON): Statistics Canada; 2022 [updated 2022 Nov 4; cited 2022 Oct 1]. Available from: https://www150.statcan.gc.ca/t1/tbl1/en/tv.action?pid=1410037301&pickMembers%5B0%5D=2.2&pickMembers%5B1%5D=3.1&pickMembers%5B2%5D=4.1&cubeTimeFrame.startMonth=04&cubeTimeFrame.startYear=2022&cubeTimeFrame.endMonth=08&cubeTimeFrame.endYear=2022&referencePeriods=20220401%2C20220801.
Sabbath EL, Boden LI, Williams JA, Hashimoto D, Hopcia K, Sorensen G. Obscured by administrative data? Racial disparities in occupational injury. Scand J Work Environ Health. 2017;43(2):155–62.
National Cancer Institute. Prostate - recent trends in SEER age-adjusted incidence rates, 2000–2019 [Interent]. Bethesda (MD): National Institutes of Health (USA); 2022 [cited 2022 Oct 1]. Available from: https://seer.cancer.gov/statistics-network/explorer/application.html?site=66&data_type=1&graph_type=2&compareBy=race&chk_race_6=6&chk_race_5=5&chk_race_4=4&chk_race_3=3&chk_race_2=2&rate_type=1&hdn_sex=2&age_range=1&stage=101&advopt_precision=1&advopt_show_ci=on&hdn_view=0&advopt_display=2#graphArea
Kurian AK, Cardarelli KM. Racial and ethnic differences in cardiovascular disease risk factors: a systematic review. Ethn Dis. 2007;17(1):143–52.
Phelan JC, Link BG. Is racism a fundamental cause of inequalities in health? Annu Rev Sociol. 2015;41:311–30.
Vaughn IA, Terry EL, Bartley EJ, Schaefer N, Fillingim RB. Racial-ethnic differences in osteoarthritis pain and disability: a meta-analysis. J Pain. 2019;20(6):629–44.
American Medical Association. New AMA policies recognize race as a social, not biological, construct [Internet]. Chicago (IL): American Medical Association; 2020 [updated 2022 Nov 16; cited 2022 Oct 1]. Available from: https://www.ama-assn.org/press-center/press-releases/new-ama-policies-recognize-race-social-not-biological-construct.
Cruickshank J, Mbanya J, Wilks R, Balkau B, McFarlane-Anderson N, Forrester T. Sick genes, sick individuals or sick populations with chronic disease? The emergence of diabetes and high blood pressure in african-origin populations. Int J Epidemiol. 2001;30(1):111–7.
ASHG Perspective. ASHG denounces attempts to link genetics and racial supremacy. Am J Hum Genet. 2018;103(5):P636.
Flanagin A, Frey T, Christiansen SL, AMA Manual of Style Committee. Updated guidance on the reporting of race and ethnicity in medical and science journals. JAMA. 2021;326(7):621–7.
Murray LR. Sick and tired of being sick and tired: scientific evidence, methods, and research implications for racial and ethnic disparities in occupational health. Am J Public Health. 2003;93(2):221–6.
Lloyd JW. Long-term mortality study of steelworkers. V. Respiratory cancer in coke plant workers. J Occup Med. 1971;13(2):53–68.
Landsbergis PA, Grzywacz JG, LaMontagne AD. Work organization, job insecurity, and occupational health disparities. Am J Ind Med. 2014;57(5):495–515.
Williams DR, Mohammed SA, Leavell J, Collins C. Race, socioeconomic status, and health: complexities, ongoing challenges, and research opportunities. Ann N Y Acad Sci. 2010;1186(1):69–101.
Brondolo E, Gallo LC, Myers HF. Race, racism and health: disparities, mechanisms, and interventions. J Behav Med. 2009;32(1):1–8.
Bailey ZD, Krieger N, Agénor M, Graves J, Linos N, Bassett MT. Structural racism and health inequities in the USA: evidence and interventions. The Lancet. 2017;389(10077):1453–63.
Loisel P, Durand M-J, Berthelette D, Vézina N, Baril R, Gagnon D, et al. Disability prevention: new paradigm for the management of occupational back pain. Dis Manage Health Outcomes. 2001;9(7):351–60.
Jetha A, Yanar B, Lay AM, Mustard C. Work disability management communication bottlenecks within large and complex public service organizations: a sociotechnical systems study. J Occup Rehabil. 2019;29(4):754–63.
MacEachen E, Kosny A, Ferrier S, Chambers L. The “toxic dose” of system problems: why some injured workers don’t return to work as expected. J Occup Rehabil. 2010;20(3):349–66.
MacEachen E, Kosny A, Ferrier S. Unexpected barriers in return to work: lessons learned from injured worker peer support groups. Work. 2007;29(2):155–64.
Rucker JM, Richeson JA. Toward an understanding of structural racism: implications for criminal justice. Science. 2021;374(6565):286–90.
Irvin E, Van Eerd D, Amick BC III, Brewer S. Introduction to special section: systematic reviews for prevention and management of musculoskeletal disorders. J Occup Rehabil. 2010;20(2):123–6.
Gewin V. The rise of inequality research: can spanning disciplines help tackle injustice? Nature. 2022;606(7915):827–9.
DistillerSR. DistillerSR Software Version 2.35 [software]. DistillerSR Inc. ; 2022 [cited 2022 Nov 1]. Available from: https://www.evidencepartners.com.
Slavin RE. Best-evidence synthesis: an alternative to meta-analytic and traditional reviews. Educ Res. 1986;15(9):5–11.
Blinder V, Patil S, Eberle C, Griggs J, Maly RC. Early predictors of not returning to work in low-income breast cancer survivors: a 5-year longitudinal study. Breast Cancer Res Treat. 2013;140(2):407–16.
Blinder VS, Patil S, Thind A, Diamant A, Hudis CA, Basch E, et al. Return to work in low-income Latina and non-Latina white breast cancer survivors: a 3-year longitudinal study. Cancer. 2012;118(6):1664–74.
Chibnall JT, Tait RC. Long-term adjustment to work-related low back pain: associations with socio-demographics, claim processes, and post-settlement adjustment. Pain Med. 2009;10(8):1378–88.
Marom BS, Ratzon NZ, Carel RS, Sharabi M. Return-to-work barriers among manual workers after hand injuries: 1-year follow-up cohort study. Arch Phys Med Rehabil. 2019;100(3):422–32.
Marom BS, Sharabi M, Carel RS, Ratzon NZ. Returning to work after a hand injury: does ethnicity matter? PLoS ONE. 2020;15(3):e0229982.
Savitsky B, Radomislensky I, Goldman S, Gitelson N, Frid Z, Peleg K. Socio-economic disparities and returning to work following an injury. Isr J Health Policy Res. 2020;9(1):35.
Savitsky B, Radomislensky I, Goldman S, Gitelson N, Frid Z, Peleg K. Returning to work following an injury: practical usage of a predictive model based on a nationwide study. J Community Health. 2020;45(1):183–93.
Asher AL, Devin CJ, Archer KR, Chotai S, Parker SL, Bydon M, et al. An analysis from the Quality Outcomes Database, Part 2. Predictive model for return to work after elective surgery for lumbar degenerative disease. J Neurosurg Spine. 2017;27(4):370–81.
Bradley CJ, Wilk A. Racial differences in quality of life and employment outcomes in insured women with breast cancer. J Cancer Surviv. 2014;8(1):49–59.
Busch MA, Coshall C, Heuschmann PU, McKevitt C, Wolfe CD. Sociodemographic differences in return to work after stroke: the South London Stroke Register (SLSR). J Neurol Neurosurg Psychiatry. 2009;80(8):888–93.
Carrougher GJ, Bamer AM, Mandell SP, Brych S, Schneider JC, Ryan CM, et al. Factors affecting employment after burn injury in the United States: a burn model system national database investigation. Arch Phys Med Rehabil. 2020;101(Suppl 1):71–S85.
Khan I, Bydon M, Archer KR, Sivaganesan A, Asher AM, Alvi MA, et al. Impact of occupational characteristics on return to work for employed patients after elective lumbar spine surgery. Spine J. 2019;19(12):1969–76.
Meade MA, Lewis A, Jackson MN, Hess DW. Race, employment, and spinal cord injury. Arch Phys Med Rehabil. 2004;85(11):1782–92.
MacKenzie EJ, Bosse MJ, Kellam JF, Pollak AN, Webb LX, Swiontkowski MF, et al. Early predictors of long-term work disability after major limb trauma. J Trauma. 2006;61(3):688–94.
Sanchez KM, Richardson JL, Mason HRC. The return to work experiences of colorectal cancer survivors. AAOHN J. 2004;52(12):500–10.
Skolarus LE, Wing JJ, Morgenstern LB, Brown DL, Lisabeth LD. Mexican Americans are less likely to return to work following stroke: clinical and policy implications. J Stroke Cerebrovasc Dis. 2016;25(8):1851–5.
Chibnall JT, Tait RC, Andresen EM, Hadler NM. Race and socioeconomic differences in post-settlement outcomes for african american and caucasian workers’ compensation claimants with low back injuries. Pain. 2005;114(3):462–72.
Tait RC, Chibnall JT, Andresen EM, Hadler NM. Management of occupational back injuries: differences among african Americans and Caucasians. Pain. 2004;112(3):389–96.
Friedman LS, Ruestow P, Forst L. Analysis of ethnic disparities in workers’ compensation claims using data linkage. J Occup Environ Med. 2012;54(10):1246–52.
Tait RC, Chibnall JT. Work injury management of refractory low back pain: relations with ethnicity, legal representation and diagnosis. Pain. 2001;91(1):47–56.
Strong LL, Zimmerman FJ. Occupational injury and absence from work among african american, hispanic, and non-hispanic white workers in the national longitudinal survey of youth. Am J Public Health. 2005;95(7):1226–32.
Ben-Shalom Y, Mamun AA. Return-to-work outcomes among Social Security Disability Insurance program beneficiaries. J Disabil Policy Stud. 2015;26(2):100–10.
Jones CP. Confronting institutionalized racism. Phylon. 2002;50(1/2):7–22.
Williams DR, Rucker TD. Understanding and addressing racial disparities in health care. Health Care Financ Rev. 2000;21(4):75–90.
Hostetter M, Klein S. Confronting racism in health care: moving from proclamations to new practices [Interent]. New York (NY): The Commonwealth Fund; 2021 [updated 2021 Oct 18; cited 2022 Oct 1]. Available from: https://www.commonwealthfund.org/publications/2021/oct/confronting-racism-health-care.
Bailey ZD, Feldman JM, Bassett MT. How structural racism works — racist policies as a root cause of U.S. racial health inequities. N Engl J Med. 2020;384(8):768–73.
Melamed J. Racial capitalism. Crit Ethnic Stud. 2015;1(1):76–85.
McClure ES, Vasudevan P, Bailey Z, Patel S, Robinson WR. Racial capitalism within public health—how occupational settings drive COVID-19 disparities. Am J Epidemiol. 2020;189(11):1244–53.
Berdahl TA. Racial/ethnic and gender differences in individual workplace injury risk trajectories: 1988–1998. Am J Public Health. 2008;98(12):2258–63.
Calliste AM, Dei GJS. Power, knowledge and anti-racism education: a critical reader. Halifax: Fernwood; 2000.
Hassen N, Lofters A, Michael S, Mall A, Pinto AD, Rackal J. Implementing anti-racism interventions in healthcare settings: a scoping review. Int J Environ Res Public Health. 2021;18(6):2993.
Acknowledgements
Dr. Arif Jetha’s salary is partially supported by a Stars Career Development Award from the Arthritis Society (Canada). The Institute for Work & Health is supported through funding from the Ontario Ministry of Labour, Immigration, Training and Skills Development (MLITSD). The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the MLITSD; no endorsement is intended or should be inferred. The funding bodies had no role in study design, data collection, data interpretation or manuscript writing. We would like to acknowledge Meagan Parmassar and Dr. Amir Mofidi for their support with title/abstract screening and full-text reviews. We would like to thank Amna Qureshi for their support with the preparation of the manuscript.
Funding
Dr. Arif Jetha’s salary is partially supported by a Stars Career Development Award from the Arthritis Society (Canada). The Institute for Work & Health is supported through funding from the Ontario Ministry of Labour, Immigration, Training and Skills Development (MLITSD). The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the MLITSD; no endorsement is intended or should be inferred. The funding bodies had no role in study design, data collection, data interpretation or manuscript writing. The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Arif Jetha = Study conceptualization and led methodological development and implementation, relevance screening, data extraction and synthesis and writing. Lahmea Navaratnerajah = Managed methodological implementation, relevance screening, data extraction and synthesis and writing. Faraz Vahid Shahidi, Nancy Carnide, Aviroop Biswas, Basak Yanar, Arjumand Siddiqi = Contributed to methodological implementation, relevance screening, data extraction and synthesis and writing. All authors reviewed final manuscript.
Corresponding author
Ethics declarations
Competing Interests
Dr. Arif Jetha is a scientific advisory panel member of GainLife Inc. Dr. Jetha’s advisory involvement is not specifically related to the research presented in this manuscript and did not influence the presentation and synthesis of the findings.
Conflict of Interest
Dr. Arif Jetha is a scientific advisory panel member of GainLife Inc.. Dr. Jetha’s advisory involvement is not specifically related to the research presented in this manuscript and did not influence the presentation and synthesis of the findings Lahmea Navaratnerajah, Faraz Vahid Shahidi, Nancy Carnide, Aviroop Biswas, Basak Yanar, and Arjumand Siddiqi have no conflicts of interests to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jetha, A., Navaratnerajah, L., Shahidi, F.V. et al. Racial and Ethnic Inequities in the Return-to-Work of Workers Experiencing Injury or Illness: A Systematic Review. J Occup Rehabil 33, 432–449 (2023). https://doi.org/10.1007/s10926-023-10119-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10926-023-10119-1