Abstract
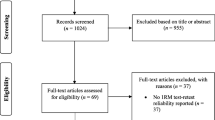
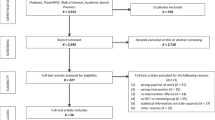
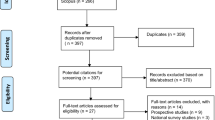
Purpose Chronic musculoskeletal pain can have a major impact on ability to work. The work ability score is a commonly used single-item question to assess work ability but has not been fully validated yet. The aim of the present study was to evaluate test–retest reliability, agreement, construct validity, and responsiveness of the work ability score among sick-listed workers with chronic musculoskeletal pain. Methods Data of sick-listed workers with chronic musculoskeletal pain was routinely collected at seven rehabilitation centres in the Netherlands. Assessments included a set of questionnaires, administered at admission and discharge from a fifteen-week vocational rehabilitation program. Test–retest reliability was determined with the intraclass correlation coefficient. For agreement, the standard error of measurement and smallest detectable changes were calculated. Construct validity was assessed by testing hypotheses regarding Spearman rank correlation coefficient. Area under the curve obtained from the receiver operating characteristic curve and minimal clinically important change were determined for the total sample and work ability score baseline tertile groups to assess responsiveness. Results In total, 34 workers were analyzed for reliability and agreement, 1291 workers for construct validity, and 590 responded to the responsiveness questionnaire. Reliability reached an intraclass correlation coefficient of 0.89; 95% CI 0.77–0.94, a standard error of measurement of 0.69 points, and the smallest detectable change of 1.92 points. For construct validity, six of the seven predefined hypotheses were not refuted. The area under the curve was 0.76 (95% CI 0.71–0.81) allowing for discrimination between stable and improved workers, with a minimal clinically important change of 2.0 points for the total sample. Conclusion The work ability score showed good measurement properties among sick-listed workers with chronic musculoskeletal pain.


Similar content being viewed by others
References
Cimmino MA, Ferrone C, Cutolo M. Epidemiology of chronic musculoskeletal pain. Best Pract Res Clin Rheumatol. 2011;25(2):173–83.
van Hecke O, Torrance N, Smith BH. Chronic pain epidemiology and its clinical relevance. Br J Anaesth. 2013;111(1):13–8.
Treede RD, Rief W, Barke A, Aziz Q, Bennett MI, Benoliel R, et al. Chronic pain as a symptom or a disease: the IASP Classification of Chronic Pain for the International Classification of Diseases (ICD-11). Pain. 2019;160(1):19–27.
Bevan S. Economic impact of musculoskeletal disorders (MSDs) on work in Europe. Best Pract Res Clin Rheumatol. 2015;29(3):356–73.
Mather L, Ropponen A, Mittendorfer-Rutz E, Narusyte J, Svedberg P. Health, work and demographic factors associated with a lower risk of work disability and unemployment in employees with lower back, neck and shoulder pain. BMC Musculoskelet Disord. 2019;20(1):622.
Tengland PA. The concept of work ability. J Occup Rehabil. 2011;21(2):275–85.
Ilmarinen J, Tuomi K, Seitsamo J. New dimensions of work ability. Int Congr Ser. 2005;1280:3–7.
Mokkink LB, Terwee CB, Patrick DL, et al. The COSMIN checklist for assessing the methodological quality of studies on measurement properties of health status measurement instruments: an international Delphi study. Qual Life Res. 2010;19(4):539–49.
van den Berg TI, Elders LA, de Zwart BC, Burdorf A. The effects of work-related and individual factors on the Work Ability Index: a systematic review. Occup Environ Med. 2009;66(4):211–20.
Radkiewicz P, Widerszal-Bazyl M. Psychometric properties of Work Ability Index in the light of comparative survey study. Int Congr Ser. 2005;1280:304–9.
Ebener M, Hasselhorn HM. Validation of short measures of work ability for research and employee surveys. Int J Environ Res Public Health. 2019;16(18):3386.
Abdolalizadeh M, Arastoo AA, Ghsemzadeh R, Montazeri A, Ahmadi K, Azizi A. The psychometric properties of an Iranian translation of the Work Ability Index (WAI) questionnaire. J Occup Rehabil. 2012;22(3):401–8.
Blik op werk. Available from: https://www.blikopwerk.nl/werkgever/duurzame-inzetbaarheid/work-ability-index/the-wai-in-the-netherlands [Accessed: May 2020].
Bascour-Sandoval C, Soto-Rodríguez F, Muñoz-Poblete C, Marzuca-Nassr GN. Psychometric properties of the Spanish version of the Work Ability Index in working individuals. J Occup Rehabil. 2020;30(2):288–97.
Kaewboonchoo O, Ratanasiripong P. Psychometric properties of the Thai version of the work ability index (Thai WAI). J Occup Health. 2015;57(4):371–7.
Alexopoulos E. Work Ability Index: validation of the Greek version and descriptive data in heavy industry employees. Br J Med Med Res. 2013;3(3):608–21.
Ahlstrom L, Grimby-Ekman A, Hagberg M, Dellve L. The Work Ability Index and single-item question: associations with sick leave, symptoms, and health–a prospective study of women on long-term sick leave. Scand J Work Environ Health. 2010;36(5):404–12.
El Fassi M, Bocquet V, Majery N, Lair ML, Couffignal S, Mairiaux P. Work ability assessment in a worker population: comparison and determinants of Work Ability Index and Work Ability score. BMC Public Health. 2013;13:305.
Torgén M. Experiences of WAI in a random sample of the Swedish working population. Int Congr Ser. 2005;1280:328–32.
Lundin A, Kjellberg K, Leijon O, Punnett L, Hemmingsson T. The association between self-assessed future work ability and long-term sickness absence, disability pension and unemployment in a general working population: A 7-year follow-up study. J Occup Rehabil. 2016;26(2):195–203.
Mokkink LB, Terwee CB, Patrick DL, et al. The COSMIN study reached international consensus on taxonomy, terminology, and definitions of measurement properties for health-related patient-reported outcomes. J Clin Epidemiol. 2010;63(7):737–45.
Mokkink LB, Prinsen CAC, Patrick DL, Alonso J, Bouter LM, de Vet HCW, et al. COSMIN Study Design checklist for patient-reported outcome measurement instruments [PDF file]. Department of Epidemioly and Biostatistics: Amsterdam University Medical Centers, Location VUmc; 2019. p. 1–32.
Beemster TT, van Velzen JM, van Bennekom CA, Frings-Dresen MH, Reneman MF. Cost-effectiveness of 40-hour versus 100-hour vocational rehabilitation on work participation for workers on sick leave due to subacute or chronic musculoskeletal pain: study protocol for a randomized controlled trial. Trials. 2015;16:317.
Reneman MF, Beemster TT, Edelaar MJ, van Velzen JM, van Bennekom C, Escorpizo R. Towards an ICF- and IMMPACT-based pain vocational rehabilitation core set in the Netherlands. J Occup Rehabil. 2013;23(4):576–84.
van den Heuvel SG, Geuskens GA, Hooftman WE, Koppes LL, van den Bossche SN. Productivity loss at work; health-related and work-related factors. J Occup Rehabil. 2010;20(3):331–9.
Bouwmans C, Krol M, Severens H, Koopmanschap M, Brouwer W, Hakkaart-van RL. The iMTA productivity cost questionnaire: a standardized instrument for measuring and valuing health-related productivity losses. Value Health. 2015;18(6):753–8.
Beemster T, van Bennekom C, van Velzen J, Reneman M, Frings-Dresen M. The interpretation of change score of the pain disability index after vocational rehabilitation is baseline dependent. Health Qual Life Outcomes. 2018;16(1):182.
Krops LA, Wolthuizen L, Dijkstra PU, Jaarsma EA, Geertzen JHB, Dekker R. Reliability of translation of the RAND 36-item health survey in a post-rehabilitation population. Int J Rehabil Res. 2018;41(2):128–37.
Van der Zee KI, Sanderman R. Het meten van de algemene gezondheidstoestand met de RAND-36, een handleiding. 2nd ed. Research Institute SHARE; 2012.
Rabin R, de Charro F. EQ-5D: a measure of health status from the EuroQol Group. Ann Med. 2001;33(5):337–43.
Farrar JT, Young JP Jr, LaMoreaux L, Werth JL, Poole RM. Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. Pain. 2001;94(2):149–58.
Kamper SJ, Ostelo RWJG, Knol DL, Maher CG, de Vet HCW, Hancock MJ. Global perceived effect scales provided reliable assessments of health transition in people with musculoskeletal disorders, but ratings are strongly influenced by current status. J Clin Epidemiol. 2010;63(7):760–6.
Mishra P, Pandey CM, Singh U, Gupta A, Sahu C, Keshri A. Descriptive statistics and normality tests for statistical data. Ann Card Anaesth. 2019;22(1):67–72.
Beemster TT, van Velzen JM, van Bennekom CAM, Reneman MF, Frings-Dresen MHW. Test-retest reliability, agreement and responsiveness of productivity loss (iPCQ-VR) and healthcare utilization (TiCP-VR) questionnaires for sick workers with chronic musculoskeletal pain. J Occup Rehabil. 2019;29(1):91–103.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15(2):155–63.
Terwee CB, Bot SD, de Boer MR, et al. Quality criteria were proposed for measurement properties of health status questionnaires. J Clin Epidemiol. 2007;60(1):34–42.
Scholtes VA, Terwee CB, Poolman RW. What makes a measurement instrument valid and reliable? Injury. 2011;42(3):236–40.
van Schaaijk A, Nieuwenhuijsen K, Frings-Dresen MHW, Sluiter JK. Work ability and work functioning: measuring change in individuals recently returned to work. Int Arch Occup Environ Health. 2019;92(3):423–33.
Voltmer JB, Deller J. Measuring work ability with its antecedents: evaluation of the Work Ability Survey. J Occup Rehabil. 2018;28(2):307–21.
Karlsson ML, Busch H, Aboagye E, Jensen I. Validation of a measure of health-related production loss: construct validity and responsiveness - a cohort study. BMC Public Health. 2015;15:1148.
Vänni K, Virtanen P, Luukkaala T, Nygård CH. Relationship between perceived work ability and productivity loss. Int J Occup Saf Ergon. 2012;18(3):299–309.
Marfeo EE, Haley SM, Jette AM, Eisen SC, et al. Conceptual foundation for measures of physical function and behavioral health function for Social Security work disability evaluation. Arch Phys Med Rehabil. 2013;94(9):1645–52.
Mänty M, Kouvonen A, Lallukka T, Lahti J, Lahelma E, Rahkonen O. Changes in working conditions and physical health functioning among midlife and ageing employees. Scand J Work Environ Health. 2015;41(6):511–8.
Froud R, Abel G. Using ROC curves to choose minimally important change thresholds when sensitivity and specificity are valued equally the forgotten lesson of pythagoras theoretical considerations and an example application of change in health status. PLoS ONE. 2014;9(12):e114468.
Olsen MF, Bjerre E, Hansen MD, Tendal B, Hilden J, Hróbjartsson A. Minimum clinically important differences in chronic pain vary considerably by baseline pain and methodological factors systematic review of empirical studies. J Clin Epidemiol. 2018;101:87–106.
Akobeng AK. Understanding diagnostic tests 3: Receiver operating characteristic curves. Acta Paediatr. 2007;96(5):644–7.
Adel M, Akbar R, Ehsan G. Validity and reliability of Work Ability Index (WAI) questionnaire among Iranian workers; a study in petrochemical and car manufacturing industries. J Occup Health. 2019;61(2):165–74.
Sell L, Lund HL, Holtermann A, Søgaard K. The interactions between pain, pain-related fear of movement and productivity. Occup Med (Lond). 2014;64(5):376–81.
Escobar A, Riddle DL. Concordance between important change and acceptable symptom state following knee arthroplasty: the role of baseline scores. Osteoarthritis Cartilage. 2014;22(8):1107–10.
Acknowledgements
The authors thank the following vocational rehabilitation centers for their help with the data collection: Adelante (Hoensbroek), Heliomare (Wijk aan Zee), Klimmendaal – Zintens (Arnhem), Libra revalidatie en audiologie (Eindhoven & Tilburg), Merem medische revalidatie (Almere), Roessingh, centrum voor revalidatie (Enschede), and UMCG centrum voor revalidatie, Beatrixoord (Groningen). The following researchers and clinicians have actively contributed to the research and agreed to be acknowledged for their contribution: Timo Beemster, Judith van Velzen, Coen van Bennekom, Janneke Nachtegaal, Lucienne van der Meer, Marlique Langkamp, Noelle Muller, Tristan Erens, Margaret Lam, Levijn Romp, Saskia Koning, Clement Roos, Karin Karstens, Sanny Rakers, Simone Akkerman, Gabrielle Rovers, Sabrine du Bois, Barbara Strang and Arne Martens.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical Approval
This retrospective study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declarations and its later amendments or comparable ethical standards.
Consent to Participate
Informed consent was obtained from all workers being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Stienstra, M., Edelaar, M.J.A., Fritz, B. et al. Measurement Properties of the Work Ability Score in Sick-Listed Workers with Chronic Musculoskeletal Pain. J Occup Rehabil 32, 103–113 (2022). https://doi.org/10.1007/s10926-021-09982-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10926-021-09982-7