Abstract
Although rural communities have been hard-hit by the COVID-19 pandemic, there is limited evidence on COVID-19 outcomes in rural America using up-to-date data. This study aimed to estimate the associations between hospital admissions and mortality and rurality among COVID-19 positive patients who sought hospital care in South Carolina. We used all-payer hospital claims, COVID-19 testing, and vaccination history data from January 2021 to January 2022 in South Carolina. We included 75,545 hospital encounters within 14 days after positive and confirmatory COVID-19 testing. Associations between hospital admissions and mortality and rurality were estimated using multivariable logistic regressions. About 42% of all encounters resulted in an inpatient hospital admission, while hospital-level mortality was 6.3%. Rural residents accounted for 31.0% of all encounters for COVID-19. After controlling for patient-level, hospital, and regional characteristics, rural residents had higher odds of overall hospital mortality (Adjusted Odds Ratio – AOR = 1.19, 95% Confidence Intervals – CI = 1.04–1.37), both as inpatients (AOR = 1.18, 95% CI = 1.05–1.34) and as outpatients (AOR = 1.63, 95% CI = 1.03–2.59). Sensitivity analyses using encounters with COVID-like illness as the primary diagnosis only and encounters from September 2021 and beyond – a period when the Delta variant was dominant and booster vaccination was available - yielded similar estimates. No significant differences were observed in inpatient hospitalizations (AOR = 1.00, 95% CI = 0.75–1.33) between rural and urban residents. Policymakers should consider community-based public health approaches to mitigate geographic disparities in health outcomes among disadvantaged population subgroups.
Similar content being viewed by others
Introduction
Health inequalities between rural and urban populations have been a long-standing issue in the United States (US), and rural residents face more health challenges compared to their non-rural counterparts. Socioeconomic disadvantages and prevailing difficulties in access to care and utilization of healthcare services, increased disease prevalence and adverse health outcomes, hospital readmissions, and even mortality are disproportionately higher for rural residents compared to suburban and urban residents [1,2,3,4,5,6,7,8]. The distribution of healthcare facilities is also geographically uneven, with only 9% of US hospitals with intensive care unit (ICU) services accounting for 1% of all ICU beds being located in rural areas, while 14% of the population resides in such areas [9].
The onset of the coronavirus disease 19 (COVID-19) stretched the capacity of the US healthcare system and exacerbated rural and urban disparities in COVID-19-related health outcomes [10,11,12,13,14,15]. Almost 2,000 health centers, mostly serving low-income and racial/ethnic minority populations, temporarily closed in early 2020, which limited access to primary care services, and thus disproportionately affected access to care for marginalized and disadvantaged populations. Timely access to necessary and comprehensive care became and remained unattainable, particularly over the early stages of the pandemic, and resulted in increased delayed or foregone care for a large share of the population [16,17,18]. Although the availability of telehealth significantly increased during the pandemic to address gaps in access to care for outpatient medical conditions and to minimize existing disparities, the adoption and use of telemedicine services were lower in more isolated, rural, and socioeconomically vulnerable communities compared to urban settings, further hindering rural residents’ access to timely pre-hospital diagnosis [16, 19,20,21].
Rural and socioeconomically disadvantaged communities have been particularly hard-hit by the pandemic [10,11,12,13,14,15]. Rural areas had significantly higher COVID-19 related hospitalizations and mortality rates compared to urban areas [10,11,12,13,14,15]. Evidence across 44 hospitals systems suggests that among COVID-19 infected individuals, rural residents were more likely to die or be transferred to hospice compared to urban residents between January 2020 and June 2021 [11]. Geographic disparities in access to COVID-19 test to treat sites have also been recently documented, with about 60% of rural residents having to travel more than 60 minutes to the nearest site [22]. Vaccination rates against COVID-19 were also lower in rural compared to urban communities, which could further predispose and perpetuate rural-urban differences in adverse outcomes, given the documented effectiveness of vaccines [23,24,25].
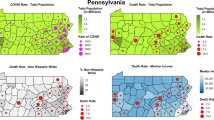
South Carolina is demographically unique compared to national averages, with almost two times higher rates of rural residents [26, 27]. Heavy reliance on private clinics and hospitals for screening and testing for COVID-19 may have exacerbated health disparities for rural residents, despite the strategically located public health clinics to serve rural communities in the state, resulting in increased mortality rates in rural areas, particularly among more socially vulnerable counties [28]. In addition, South Carolina ranked above national averages in COVID-19 death rates and was among the states with the lowest COVID-19 vaccination rates in 2021 [29]. Despite the important contributions of previous studies examining health outcomes by rurality among COVID-19-positive individuals, there is limited evidence regarding the association between COVID-19-related hospitalizations and mortality and rurality using up-to-date statewide hospital data.
The objective of this study was to estimate the variations in hospital admissions and mortality among COVID-19 positive patients by rurality from January 2021 to January 2022 in South Carolina, a period when vaccination against COVID-19 became available in the state. Our findings contribute to the knowledge of rurality as a separate social determinant of health and the need to enhance healthcare system capacity and to improve access to care and health outcomes among disadvantaged subgroups of the population.
Materials and Methods
Study Design and Data Sources
For this study, we used retrospective, secondary data from three sources, the South Carolina Department of Health and Environmental Control (DHEC), the Office of Revenue and Fiscal Affairs (RFA), and the Immunization Information System (IIS). The DHEC COVID-19 testing data were collated from the statewide Case Report Form (CRF; “Human Infection With 2019 Novel Coronavirus Case Report Form”) for SARS-CoV. The CRF contains information about laboratory-confirmed and probable cases of COVID-19, including case classification and identification, hospital admission, ICU and death information, case demographics, clinical course, symptoms, medical history, and social history. SC Law (44-29-10) and Regulations (61 − 20) require mandatory reporting of COVID-19 to DHEC [30]. The RFA hospital data included all-payer hospital claims data up to the 13th of January 2022, the most recent data available at the time of the study. This secondary database included sociodemographic and clinical information on all individuals hospitalized within the State. We restricted the data to January 2021 to account for COVID-19 vaccination roll-out in the State. DHEC uses IIS, called the Statewide Immunization Online Network (SIMON), to collect information on COVID-19 vaccine doses at the episode level. SIMON supports the Entire Immunization Partner Community in South Carolina, which includes private clinics, school nurses, local public health agencies, providers, and vendors and enables gathering and analysis of real-time vaccination data in vaccination clinics. SIMON is reliable and representative of all COVID-19 vaccinated individuals in SC.
Cohort Identification
We leveraged a unique and encrypted patient identifier to cross-link all three databases. All in-state residents with any hospital-level encounter (emergency department, outpatient, hospital admission) for COVID-19 were included in the analyses. We identified COVID-19-related visits as encounters within 14 days after laboratory confirmed COVID-19 tests [31]. Since an individual might have multiple hospital encounters (e.g. first seen in the emergency room and then admitted to the hospital) during the study period, we used the patient identifier across the data and created a patient-level dataset. Encounters with recurring dates up to 14 days from the index visit were classified as the same episode. We followed the STROBE guidelines for reporting observational studies [32].
Our study population included adults (≥ 18years of age) who resided and sought hospital care in South Carolina during the study period. Individuals with COVID-19 negative tests, those with COVID-19 positive tests but no hospital encounter, and those with COVID-19 positive tests and encounters beyond 14 days from a laboratory confirmed COVID-19 positive test were excluded similar to previous work [31]. We also excluded individuals who received any vaccine other than the BNT162b2 or mRNA-1273 vaccines (4% received other vaccines), and those with hospital encounters who had received one dose of the vaccine less than 14 days before the encounter or who had a third dose less than seven days before the encounter [31].
Outcomes of Interest and Measurement
Our main outcomes of interest were inpatient hospital admission and mortality among COVID-19 patients seeking care at hospitals in South Carolina [33]. Hospital admission (inpatient) was identified using a dichotomous variable that indicated whether the patient was admitted to the hospital as an inpatient. Mortality was identified from patients’ discharge status. The data were de-identified and the study protocol was determined to be not human subjects research by the University of South Carolina Institutional Review Board.
Main Independent Variable and Covariates
Our primary exposure variable was whether a patient resided in a rural or an urban area. We used a dichotomous measure that was available in the data and classified areas as rural or urban based on metropolitan statistical area delineation. We included multiple patient-level, hospital-level, and area of residence-level variables that could be related to hospitalizations and inpatient mortality as controls in our analyses, based on data availability and prior literature. Patient-level sociodemographic and clinical characteristics included sex, race, age, primary payor, COVID-19 vaccination status at the time of the encounter, immunocompromised status, and 7 comorbidities that have been previously associated with COVID-19-related hospitalizations and mortality [34]. Vaccination status was categorized as unvaccinated, partially vaccinated (1 dose of mRNA vaccines), and fully vaccinated (2 doses of mRNA vaccines) and boosted (3 doses of mRNA vaccines). Patients were considered partially or fully vaccinated if they received a second or third dose respectively at minimum 14 days from the hospital encounter [31].
To account for disease severity among hospitalized patients, we included admission to an ICU during hospitalization with or without intubation as an additional variable. Admission to the ICU was identified using two variables that were available in the data which indicated charges for ICU and length of stay in an ICU. Hospitalizations with positive values (> 0) on these variables were deemed as including an ICU admission. Intubation was identified using the Clinical Procedural Terminology (CPT) code for endotracheal intubation (0BH17EZ) across any of the available CPT codes during admission. Hospital- and geographic-level variables included the hospital’s teaching status, and patients’ distance from the nearest hospital and physician’s office. To estimate distances, our geographic unit of analysis was the ZIP Code Tabulation Area (ZCTA). The address of the hospitals with an emergency room was obtained from the 2019 American Hospital Association (AHA) Annual Survey. To calculate the distance of each ZCTA to its nearest hospital and physician office, we first geocoded the addresses into latitude and longitude, and then extracted the centroid (latitude, longitude) of each ZCTA. Then, we calculated the distance from each ZCTA’s centroid to all hospitals and physicians’ offices and selected the shortest distance from each as our two primary exposure measurements.
Statistical Analysis
We conducted a descriptive analysis of all COVID-19 patients who sought hospital care further stratified by the two outcomes of interest. Differences between cohorts were evaluated using chi-square tests for categorical variables and Mann-Whitney U tests for numeric variables. Multivariable logistic regression models were then used to estimate the associations between inpatient hospital admission and mortality and patients’ rural versus urban area of residence, controlling for all covariates mentioned above. We further replicated the regression models and explored inpatient and outpatient mortality and their association with rurality as separate outcomes. Hospital and time (4 periods based on variant prevalence in the state) fixed effects were used to control for unobserved variations and standard errors were clustered at the county level. Sensitivity analyses were conducted by restricting the study period from September 2021 onwards to account for the dominance of the Delta variant and booster vaccination roll-out in the state. Finally, we also conducted additional robustness checks by restricting our study sample to only COVID-19 positive patients with a COVID-like illness documented as the primary diagnosis, similar to previous work [31]. We tested for multicollinearity using the variance inflation factor across all models. Two-tailed tests were used, and statistical significance was considered at P < .05. We calculated distances from the nearest hospital and physician’s office using ArcGIS, managed the data using SAS version 9.4 (SAS Institute), and performed statistical analyses using Stata version 17.0 (StataCorp).
Results
Characteristics of all Hospital Encounters by COVID-19 Positive Patients in South Carolina Stratified by Hospitalization and Mortality
Table 1 presents descriptive information for all 75,545 COVID-19 hospital encounters overall and stratified by inpatient hospital admission and mortality. Most patients were females (55.5%), White (55.5%), with private insurance (30.5%) or Medicare (33.0%) as the primary payor and resided in urban areas (69.0%). About one-third of all encounters occurred at a teaching hospital (34.0%). The majority of SC patients with COVID-19 were not vaccinated against COVID-19 at the time of the encounter (86.4%). The most prevalent comorbidities were cardiovascular disease (45.6%), diabetes (21.5%), and chronic obstructive pulmonary disease (14.6%).
Overall, 41.8% of encounters resulted in an inpatient hospital admission with a median length of stay of 6 days (Interquartile Range: 4 to 11 days). Around one-quarter of inpatient hospital admissions (25.6%) also involved admissions to an ICU with or without intubation. Overall, hospital-level mortality was 6.3%, with the majority of deaths occurring during hospital admission (inpatient: 97.6%) and 73.1% of deaths also involved admissions to an ICU with or without intubation. Inpatient hospital admissions were relatively similar between rural and urban residents, while overall mortality was about 7.8% higher among rural residents (33.3% versus 30.9%).
Multivariable Regression Estimates
Figure 1 presents the multivariable logistic regression estimates. Compared to residents of urban areas, rural residents had significantly higher odds of overall hospital-level mortality (Adjusted Odds Ratio – AOR = 1.19, 95% Confidence Intervals = 1.04–1.37), after controlling for all covariates. In stratified analyses by setting, the adjusted odds of inpatient mortality (AOR = 1.18, 95% CI = 1.05–1.34) and outpatient mortality (AOR = 1.63, 95% CI = 1.03–2.59) were also higher for rural compared to urban residents. No statistically significant difference was observed between inpatient hospital admission and rurality (AOR = 1.00, 95% CI = 0.75–1.33). Sensitivity analyses by restricting the study period to September 2021 and beyond and by including only COVID-19 positive patients with a COVID-19 like illness as the primary diagnosis yielded similar estimates.
Additional factors positively associated with both outcomes included older age, male sex, congestive heart failure, cardiovascular disease, diabetes, COPD, chronic liver disease, neurological disease, and being immunocompromised (Table 2). In contrast, vaccinated individuals, particularly those with two or three (booster) doses had lower odds of experiencing both outcomes compared to unvaccinated patients. Finally, COVID-19 patients with an indigent or charitable organization as the designated primary payor were less likely to get admitted to a hospital as inpatients (AOR = 0.77, 95% CI = 0.70–0.85) but more likely to die during a hospital encounter (AOR = 1.56, 95% CI = 1.15–2.13) compared to those with private insurance.
Discussion
In our analysis of 75,545 hospital encounters for COVID-19 from January 2021 to January 2022 in South Carolina, we documented that overall hospital-level, inpatient, and outpatient mortality were significantly associated with rurality, after controlling for multiple patient, hospital, and geographic characteristics. Our estimates further indicated that COVID-19 vaccination mitigated the risks for inpatient hospital admission and mortality. Finally, we also found that patients with an indigent or charitable organization as their primary payor were less likely to get admitted to a hospital as inpatients but more likely to die compared to those with private health insurance coverage.
Our study extends the current literature and is in-line with previous work both in South Carolina and nationwide which has documented the differential impact of COVID-19 related mortality on urban and rural areas which are predominantly characterized by lower levels of community resilience [10,11,12,13,14,15]. Although certain characteristics of rural populations, such as older age and increased prevalence of chronic conditions predispose increased disease severity and mortality when infected with SARS-CoV-2, our adjustment for these factors did not change the finding of increased odds of mortality for rural compared to urban residents. It is possible that already at-risk rural residents presented to hospitals at later stages of the disease, which could explain the increased likelihood of outpatient mortality in particular [35, 36]. We note that we did not find a significant association between inpatient hospital admission and rurality, similar to prior work in South Carolina using 2020 data but unlike other studies using hospital-system or statewide data [11, 14]. This difference could be attributed to the geographic and population-level differences across different states and settings and highlights the importance of state specific analyses to guide local stakeholders and policies using up-to-date evidence.
Our findings indicate that rural residence is an additional social determinant of health and is distinctly associated with adverse health outcomes among patients with COVID-19 in particular. The increased odds of mortality documented in this study among COVID-19 positive patients who resided in rural areas contribute to existing evidence of rurality as a mechanism for downstream disparities in health outcomes and highlight long-standing inequalities in the built environment of healthcare facilities at the community level, particularly for residentially segregated and rural residents, beyond commonly cited unidimensional social determinants of health at the individual level [5, 14, 37,38,39].
Although decades of research have revealed the stepwise relationship between rurality and health, with increased social needs of rural residents predisposing poorer health outcomes, interest in tackling disparities has heightened due to the unequal impact of the COVID-19 pandemic on marginalized and residentially segregated populations, including the state of South Carolina [14, 38,39,−40]. Remedies to address prevailing social needs related to health should be tailored both at the healthcare system and the social system levels. At the healthcare system level, maintaining and even expanding the scope of practice and use of telemedicine services - desired by both patients and providers - is a first step to bolster access to timely care for certain conditions and mitigate prevailing disparities in healthcare utilization and outcomes [41]. Initiatives and legislation to enhance resources of safety net providers such as Federally Qualified Health Centers, which assist patients with access barriers to care among others, might also be a critical step towards connecting vulnerable populations with needed resources and thus reducing existing geographic disparities.
At the social system, federal and state agencies, policymakers, hospital systems, and health providers, are also uniquely positioned to contribute to narrowing health gaps [41]. Expansion of existing or implementation of new, targeted legislative acts and safety net programs, such as the American Rescue Plan Act, the Earned Income Tax Credit, the expanded Child Tax Credit and food stamps benefits, are critical to alleviate the burden of financial hardships [41]. However, many of these programs are costly short-term remedies to support vulnerable populations and to address long-standing disparities. Instead, directly investing in local marginalized communities and strengthening the social services sector coupled with multisector coalitions between private and public healthcare providers and community-wide social services that are collectively aligned around a specific location, population or a particular social determinant of health, can allocate resources towards a common goal of improving health outcomes in these communities [40, 41]. The importance of such provisions is further supported by our findings on the association between mortality and having indigent or charitable organizations as primary payors, as well as the protective effect of COVID-19 vaccinations against hospitalizations and mortality. To eliminate social disparities and ultimately promote health equity will require re-allocation and shifts of federal and state budgets from healthcare to underinvested social and educational services. These can improve access to care and population health by transforming the healthcare system from medical-care centered to patient-need centered and recognizing that health inequities are interrelated to social and structural factors [40, 41].
Our study is not without limitations. First, we used data only from one State, and thus our results might not be generalizable to other States due to state-level variability. Despite this, our results are in-line with previous studies that have examined the association between COVID-19 mortality and rurality. Second, it is possible that some encounters were for conditions unrelated to COVID-19, despite the positive COVID-19 test within 14 days from the encounter, which might have resulted in overestimations, due to the identification strategy used. However, we addressed potential selection bias by conducting additional analyses and restricting hospital encounters to only those with a COVID-like illness as the primary diagnosis beyond the positive test [31]. Similarly, the prevalence of patient-level comorbidities might be underestimated if these were not reported in the available diagnostic codes. In addition, we were not able to assess whether rural populations disproportionately delayed seeking care which could contribute to severe outcomes and partially explain differences in mortality. Finally, we were not able to specify certain variables in more detail (e.g. sex, income) due to data availability or include other factors which might predispose COVID-19-related outcomes as controls, such as more detailed clinical information, lab results, and socioeconomic status.
Our findings suggest that mortality among COVID-19 patients was associated with rurality in South Carolina between January 2021 to January 2022. Stakeholders and policymakers should consider enhancing community-based public health and social services’ centered approaches to improve health outcomes among disadvantaged subgroups of the population and mitigate long-lasting geographic disparities for underserved Southern populations.
Data Availability
The University of South Carolina Big Data Health Science Center is prohibited from making individual-level data available publicly due to provisions in the data use agreements with state agencies/data providers, institutional policy, and ethical requirements. To facilitate research, access to such data is made available via approved data access requests. Some University of South Carolina Big Data Health Science Center data is not available externally or for re-release due to prohibitions in data use agreements with state agencies or other data providers. Institutional policies stipulate that all external requests for data access require collaboration with a University of South Carolina Big Data Health Science Center researcher. For more information or to make a request, please contact Bankole Olatosi, PhD at Olatosi@mailbox.sc.edu. The underlying analytical codes are available from the authors on request.
References
Hung, P., Casey, M. M., Kozhimannil, K. B., Karaca-Mandic, P., & Moscovice, I. S. (2018 Jun). Rural-urban differences in access to hospital obstetric and neonatal care: How far is the closest one? Journal Of Perinatology, 38(6), 645–652.
Turrentine, F. E., Buckley, P. J., Sohn, M. W., & Williams, M. D. (2017 Jun). Travel time influences readmission risk: Geospatial mapping of surgical readmissions. American Surgeon, 83(6), 573–582.
Buchmueller, T. C., Jacobson, M., & Wold, C. (2006 Jul). How far to the hospital? The effect of hospital closures on access to care. Journal of Health Economics, 25(4), 740–761.
LaVela, S. L., Smith, B., Weaver, F. M., & Miskevics, S. A. (2004 Dec). Geographical proximity and health care utilization in veterans with SCI&D in the USA. Social Science and Medicine, 59(11), 2387–2399.
Eberth, J. M., Hung, P., Benavidez, G. A., et al. (2022 Feb). The problem of the Color line: Spatial access to hospital services for minoritized racial and ethnic groups: Study examines spatial access to hospital services for minoritized racial and ethnic groups. Health Affairs, 41(2), 237–246.
Advisory Committee on Training in Primary Care Medicine and Dentistry. Improving access to care in underserved rural communities. Eighteenth annual report to the Secretary of the US Department of Health and Human Services and the US Congress. Human Resources and Services Administration. Nov 2021. Accessed October 17 (2022). https://www.hrsa.gov/sites/default/files/hrsa/advisory-committees/primarycare-dentist/reports/actpcmd-18th-report.pdf
Garcia, M. C., Rossen, L. M., Brigham, B., et al. (2019). Potentially excess deaths from the five leading causes of death in Metropolitan and Nonmetropolitan Counties — United States, 2010–2017. Morbidity and Mortality Weekly Report. Surveillance Summaries, 68(10), 1–11.
Harrington, R. A., Califf, R. M., Balamurugan, A., et al. (2020 Feb). Call to action: Rural health: A presidential advisory from the American Heart Association and American Stroke Association. Circulation, 141(10), e615–e644.
Diaz, A., Schoenbrunner, A., & Pawlik, T. M. (2021 Jan). Trends in the geospatial distribution of inpatient adult surgical services across the United States. Annals of Surgery, 273(1), 121–127.
Lakhani, H. V., Pillai, S. S., Zehra, M., Sharma, I., & Sodhi, K. (2020 Jun). Systematic review of clinical insights into novel coronavirus (CoVID-19) pandemic: Persisting challenges in US rural population. International Journal of Environmental Research and Public Health, 17(12), 4279.
Anzalone, A. J., Horswell, R., Hendricks, B., et al. (2023 Jan). Higher hospitalization and mortality rates among SARS-CoV-2 infected persons in Rural America. Journal of Rural Health, 39(1), 39–54.
Denslow, S., Wingert, J. R., Hanchate, A. D., et al. (2022 Aug). Rural-urban outcome differences associated with COVID-19 hospitalizations in North Carolina. PloS One, 17(8), e0271755.
Magesh, S., John, D., Li, W. T., et al. (2021 Nov). Disparities in COVID-19 outcomes by race, ethnicity, and socioeconomic status: A systematic-review and meta-analysis. JAMA Network Open, 4(11), e2134147–e2134147.
Yang, X., Zhang, J., Chen, S., et al. (2021 Aug). Demographic disparities in clinical outcomes of COVID-19: Data from a statewide cohort in South Carolina. Open Forum Infectious Diseases, 8(9), ofab428.
Grome, H. N., Raman, R., Katz, B. D., et al. (2022 Sep). Disparities in COVID-19 mortality rates: Implications for rural health policy and preparedness. Journal of Public Health Management and Practice, 28(5), 478–485.
Patel, S. Y., & Mehrotra, A. (Oct 2021). The surge of telehealth during the pandemic is exacerbating urban-rural disparities in access to mental health care. Health Affairs Forefront.
Giannouchos, T. V., Brooks, J. M., Andreyeva, E., & Ukert, B. (2022 Feb). Frequency and factors associated with foregone and delayed medical care due to COVID-19 among nonelderly US adults from August to December 2020. Journal of Evaluation in Clinical Practice, 28(1), 33–42.
Anderson, K. E., McGinty, E. E., Presskreischer, R., & Barry, C. L. (2021 Jan). Reports of forgone medical care among US adults during the initial phase of the COVID-19 pandemic. JAMA Network Open, 4(1), e2034882–e2034882.
Patel, S. Y., Rose, S., Barnett, M. L., Huskamp, H. A., Uscher-Pines, L., & Mehrotra, A. (2021 May). Community factors associated with telemedicine use during the COVID-19 pandemic. JAMA Network Open, 4(5), e2110330–e2110330.
Chu, C., Cram, P., Pang, A., Stamenova, V., Tadrous, M., & Bhatia, R. S. (2021 Apr). Rural telemedicine use before and during the COVID-19 pandemic: Repeated cross-sectional study. Journal of Medical Internet Research, 23(4), e26960.
Patel, S. Y., Mehrotra, A., Huskamp, H. A., Uscher-Pines, L., Ganguli, I., & Barnett, M. L. (2021 Feb). Variation in telemedicine use and outpatient care during the COVID-19 pandemic in the United States: Study examines variation in total US outpatient visits and telemedicine use across patient demographics, specialties, and conditions during the COVID-19 pandemic. Health Affairs, 40(2), 349–358.
Khazanchi, R., Strumpf, A., Essien, U. R., Powers, S. D., & McManus, K. A. (2022 Nov). Geographic accessibility of COVID-19 test to treat sites by race, ethnicity, age, and rurality. JAMA Network Open, 5(11), e2241144–e2241144.
Mann, S., Christini, K., Chai, Y., Chang, C. P., Hashibe, M., & Kepka, D. (2022 Aug). Vaccine hesitancy and COVID-19 immunization among rural young adults. Preventive Medicine Reports, 28, 101845.
Sun, Y., & Monnat, S. M. (2022 Sep). Rural-urban and within‐rural differences in COVID‐19 vaccination rates. Journal of Rural Health, 38(4), 916–922.
Tenforde, M. W., Self, W. H., Gaglani, M., et al. (2022). Effectiveness of mRNA vaccination in preventing COVID-19–associated invasive mechanical ventilation and death—United States, March 2021–January 2022. Morbidity and Mortality Weekly Report, 71(12), 459.
Kaiser Family Foundation. State Health Facts: Demographics and the Economy. Accessed October 12 (2022). https://www.kff.org/state-category/demographics-and-the-economy/population/
United States Census Bureau. Rural America. Accessed on October 12 (2022). https://mtgis-portal.geo.census.gov/arcgis/apps/MapSeries/index.html?appid=49cd4bc9c8eb444ab51218c1d5001ef6
Huang, Q., Jackson, S., Derakhshan, S., et al. (2021). Urban-rural differences in COVID-19 exposures and outcomes in the South: A preliminary analysis of South Carolina. PloS One, 16(2), e0246548.
US Coronavirus vaccination tracker. USA Facts. Accessed October 15 (2022). https://usafacts.org/visualizations/covid-vaccine-tracker-states
South Carolina Department of Health and Environmental Control. South Carolina list of reportable conditions 2021. Accessed September 28 (2022). https://scdhec.gov/health-professionals/south-carolina-list-reportable-conditions
Ferdinands, J. M., Rao, S., Dixon, B., et al. (2022 Oct). Waning of vaccine effectiveness against moderate and severe covid-19 among adults in the US from the VISION network: Test negative, case-control study. BMJ, 379, e072141.
Von Elm, E., Altman, D. G., Egger, M., et al. (2008 Apr). The strengthening the reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. Annals of Internal Medicine, 61(4), 344–349.
Acosta, A. M., Garg, S., Pham, H., et al. (2021 Oct). Racial and ethnic disparities in rates of COVID-19–associated hospitalization, intensive care unit admission, and in-hospital death in the United States from March 2020 to February 2021. JAMA Network Open, 4(10), e2130479–e2130479.
Centers for Disease Control and Prevention. COVID-19: Evidence for Conditions that Increase Risk of Severe Illness (Jun 2022). Accessed August 18, 2022. https://www.cdc.gov/coronavirus/2019-ncov/science/science-briefs/underlying-evidence-table.html
Razzaghi, H., Wang, Y., Lu, H., et al. (2020). Estimated county-level prevalence of selected underlying medical conditions associated with increased risk for severe COVID-19 illness—United States, 2018. Morbidity and Mortality Weekly Report, 69(29), 945.
Peters, D. J. (2020 Jun). Community susceptibility and resiliency to COVID-19 across the rural‐urban continuum in the United States. Journal of Rural Health, 36(3), 446–456.
Long, C. L., Franklin, S. M., Hagan, A. S., et al. (2022 Apr). Health-related social needs among older adults enrolled in medicare advantage: Study examines the health-related social needs of older adults enrolled in medicare advantage. Health Affairs, 41(4), 557–562.
Jones, K. G., Roth, S. E., & Vartanian, K. B. (2022 Apr). Health and health care use strongly associated with cumulative burden of social determinants of health. Population Health Management, 25(2), 218–226.
Poteat, T., Millett, G. A., Nelson, L. E., & Beyrer, C. (2020 Jul). Understanding COVID-19 risks and vulnerabilities among black communities in America: The lethal force of syndemics. Annals of Epidemiology, 47, 1–3.
Allen, M., Brown, E., Gottlieb, L. M., & Fichtenberg, C. (2022 Oct). Community-level actions on the social determinants of health: A typology for hospitals. Health Affairs Forefront.
Hamad, R., & Galea, S. (2022 Jul). The role of Health Care Systems in bolstering the Social Safety Net to address Health Inequities in the wake of the COVID-19 pandemic. Journal of the American Medical Association, 328(1), 17–18.
Funding
BDD CIS: Big Data Driven Clinical Informatics & Surveillance - A Multimodal Database Focused Clinical, Community, & Multi-Omics Surveillance Plan for COVID-19 (NIH NIAID R01AI127203-4S1).
Drs. Giannouchos and Hung have received other funding from the Health Resources and Services Administration. Drs. Li and Olatosi have received other funding from the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
Dr. Giannouchos had full access to all the data in the study and takes responsibility for the accuracy of the data analysis.
Concept and design: Giannouchos, Olatosi.
Acquisition, analysis, or interpretation of the data: Giannouchos, Olatosi, Li, Hung, Li.
Drafting of the manuscript: Giannouchos.
Critical revision of the manuscript for important intellectual content: All authors.
Statistical analyses: Giannouchos.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Giannouchos, T.V., Li, Z., Hung, P. et al. Rural-Urban Disparities in Hospital Admissions and Mortality Among Patients with COVID-19: Evidence from South Carolina from 2021 to 2022. J Community Health 48, 824–833 (2023). https://doi.org/10.1007/s10900-023-01216-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-023-01216-6