Abstract
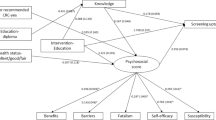
In a previous report, we demonstrated the efficacy of an educational intervention focused on increasing colorectal cancer screening rates among African Americans. Despite participating in the intervention, however, nearly two-thirds of participants did not seek and receive screening. Participants were African-Americans over age 49 (N = 257) who had not been screened for colorectal cancer according to guidelines. At baseline, participants completed tests measuring fatalism, perceived stress, self-esteem, attitudes/benefits/barriers, social support, and social network diversity. Those who completed the educational intervention were followed up by telephone to learn if they had been screened. We compared the scores on the psychometric tests of the participants who had been screened against the scores of those who had not. Only the mean scores on the attitudes, benefits, and barriers scale distinguished participants who had been screened from those who had not (p = 0.0816 on bivariate testing and p = 0.0276 in the logistic regression model). Social interaction among participants or social cognitive learning may have played a role in determining which participants were screened, but we were not able to demonstrate this. The major factor distinguishing participants who were not screened was their attitude toward screening at baseline. There is a subset of African Americans who are persistently resistant to screening, and their perspective in this regard must be addressed if colorectal cancer disparities are to be reduced.
Similar content being viewed by others
References
CDC Behavioral Risk Factor Surveillance System. http://nccd.cdc.gov/brfssprevalence/rdPage.aspx?rdReport=DPH_BRFSS.ExploreByLocation&islLocation=99&go=GO.
Blumenthal, D. S., Smith, S. A., Majett, C. D., & Alema-Mensah, E. (2010). A trial of 3 interventions to promote colorectal cancer screening in African Americans. Cancer, 116(4), 922–929.
Smith, S., Johnson, L., Wesley, D., Turner, K. B., McCray, G., Sheats, J., et al. (2012). Translation to practice of an intervention to promote colorectal cancer screening among African Americans. Clinical and Translational Science, 5(5), 412–415.
Shen, L., Condit, C. M., & Wright, L. (2009). The psychometric property and validation of a fatalism scale. Psychology and Health, 24(5), 597–613.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24(4), 385–396.
Rosenberg, Morris. (1965). Society and the adolescent self-image. Princeton, NJ: Princeton University Press.
Cohen, S., Doyle, W. J., Skoner, D. P., Rabin, B. S., & Gwaltney, J. M, Jr. (1997). Social ties and susceptibility to the common cold. JAMA, 277(24), 1940–1944.
Community Preventive Services Task Force. (2016). Cancer prevention and control. Accessed June 8, 2016, from www.thecommunityguide.org.
Sabatino, S. A., Lawrence, B., Elder, R., Mercer, S. L., et al. (2012). Effectiveness of interventions to increase screening for breast, cervical, and colorectal cancers: Nine updated systematic reviews for the guide to community preventive services. American Journal of Preventive Medicine, 43(1), 97–118.
Bandura, A. (1989). Social cognitive theory. In R. Vasta (Ed.), Annals of child development. Vol. 6. Six theories of child development (Vol. 6, pp. 1–60). Greenwich, CT: JAI Press.
Acknowledgments
Grants 5R01CA166785 (Efficacy-to-Effectiveness of an Intervention) from the National Cancer Institute (NCI). U57CCU42068 (Community Cancer Control) from the Centers for Disease Control and Prevention (CDC). 5U48DP000049 (Prevention Research Center) from the Centers for Disease Control and Prevention (CDC).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Smith, S.A., Alema-Mensah, E., Yoo, W. et al. Persons Who Failed to Obtain Colorectal Cancer Screening Despite Participation in an Evidence-Based Intervention. J Community Health 42, 30–34 (2017). https://doi.org/10.1007/s10900-016-0221-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-016-0221-7