Abstract
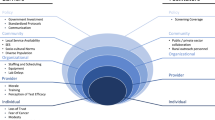
Although cervical cancer is highly preventable through screening, it remains the number one cause of cancer-related death in Kenyan women due to lack of funding and infrastructure for prevention programs. In 2012, Family AIDS Care and Education Services in partnership with the Kenya Ministry of Health began offering free screening at eleven rural health facilities. We sought to explore why screening coverage remains low at some sites. We examined the barriers to screening through a survey of 106 healthcare staff. The most frequently cited barriers to service delivery included staffing shortages, lack of trained staff, insufficient space, and supply issues. The patient barriers commonly perceived by the staff included inadequate knowledge, wait time, discomfort with male providers, and fear of pain with the speculum exam. Despite multilateral efforts to implement cervical cancer screening, staff face significant challenges to service provision and increased education is needed for both providers and patients.
Similar content being viewed by others
References
Human Papillomavirus and Related Cancers. Summary Report 2010: WHO/ICO Information Center on HPV and Cervical Cancer (HPV Information Centre) 2010.
Jemal, A., Bray, F., Center, M. M., Ferlay, J., Ward, E., & Forman, D. (2011). Global cancer statistics. CA: A Cancer Journal for Clinicians, 61(2), 69–90.
Louie, K. S., de Sanjose, S., & Mayaud, P. (2009). Epidemiology and prevention of human papillomavirus and cervical cancer in Sub-Saharan Africa: A comprehensive review. Tropical Medicine & International Health, 14(10), 1287–1302.
Huchko, M. J., Bukusi, E. A., & Cohen, C. R. (2011). Building capacity for cervical cancer screening in outpatient HIV clinics in the Nyanza province of western Kenya. International Journal of Gynaecology and Obstetrics, 114(2), 106–110.
Mwanahamuntu, M. H., Sahasrabuddhe, V. V., Kapambwe, S., et al. (2011). Advancing cervical cancer prevention initiatives in resource-constrained settings: Insights from the Cervical Cancer Prevention Program in Zambia. PLoS Medicine, 8(5), e1001032.
Were, E., Nyaberi, Z., & Buziba, N. (2010). Integrating cervical cancer and genital tract infection screening into mother, child health and family planning clinics in Eldoret, Kenya. African Health Sciences, 10(1), 58–65.
African Population and Health Research Center IAfRoC, World Health Organization. Prevention of cervical cancer through screening using visual inspection with acetic acid (VIA) and treatment with cryotherapy: A demonstration project in six African countries: Malawi, Madagascar, Nigeria, Uganda, the United Republic of Tanzania, and Zambia. 2012 (October 30, 2013). Available from: http://www.who.int/reproductivehealth/publications/cancers/9789241503860/en/.
Arbyn, M., Sankaranarayanan, R., Muwonge, R., et al. (2008). Pooled analysis of the accuracy of five cervical cancer screening tests assessed in eleven studies in Africa and India. International Journal of Cancer, 123(1), 153–160.
Stormo, A. R., Altamirano, V. C., Perez-Castells, M., et al. (2012). Bolivian health providers’ attitudes toward alternative technologies for cervical cancer prevention: A focus on visual inspection with acetic acid and cryotherapy. Journal of Women’s Health, 21(8), 801–808.
Kim, Y. M., Ati, A., Kols, A., et al. (2012). Influencing women’s actions on cervical cancer screening and treatment in Karawang District, Indonesia. Asian Pacific Journal of Cancer Prevention, 13(6), 2913–2921.
Liese, B. (2004). The state of the health workforce in Sub-Saharan Africa: Evidence of crisis and analysis of contributing factors. Washington, DC: World Bank Africa Region Human Development.
National Coordinating Agency for Population and Development (NCAPD) [Kenya], Ministry of Medical Services (MOMS) [Kenya], Ministry of Public Health and Sanitation (MOPHS) [Kenya], Kenya National Bureau of Statistics (KNBS) [Kenya], ICF Macro. (2011). Kenya Service Provision Assessment Survey 2010. Nairobi, Kenya: National Coordinating Agency for Population and Development, Ministry of Medical Services, Ministry of Public Health and Sanitation, Kenya National Bureau of Statistics, and ICF Macro.
Gatune, J. W., & Nyamongo, I. K. (2005). An ethnographic study of cervical cancer among women in rural Kenya: Is there a folk causal model? International Journal of Gynecological Cancer, 15(6), 1049–1059.
McFarland, D. M. (2003). Cervical cancer and Pap smear screening in Botswana: Knowledge and perceptions. International Nursing Review, 50(3), 167–175.
Nwankwo, K. C., Aniebue, U. U., Aguwa, E. N., Anarado, A. N., & Agunwah, E. (2011). Knowledge attitudes and practices of cervical cancer screening among urban and rural Nigerian women: A call for education and mass screening. European Journal of Cancer Care, 20(3), 362–367.
White, H. L., Mulambia, C., Sinkala, M., Mwanahamuntu, M. H., Parham, G. P., Moneyham, L., et al. (2012). ‘Worse than HIV’ or ‘not as serious as other diseases’? Conceptualization of cervical cancer among newly screened women in Zambia. Social Science and Medicine, 74(10), 1486–1493.
Districts of Kenya [database on the Internet]. Gwillim Law. 2013 [cited 14 April 2013]. Available from: http://www.statoids.com/yke.html.
Open Data Kit. [September 2011]. Available from: http://www.opendatakit.org.
Mutyaba, T., Mmiro, F. A., & Weiderpass, E. (2006). Knowledge, attitudes and practices on cervical cancer screening among the medical workers of Mulago Hospital, Uganda. BMC Medical Education, 6, 13.
Gichangi, P., De Vuyst, H., Estambale, B., Rogo, K., Bwayo, J., & Temmerman, M. (2002). HIV and cervical cancer in Kenya. International Journal of Gynaecology and Obstetrics, 76(1), 55–63.
Lyimo, F. S., & Beran, T. N. (2012). Demographic, knowledge, attitudinal, and accessibility factors associated with uptake of cervical cancer screening among women in a rural district of Tanzania: Three public policy implications. BMC Public Health, 12, 22.
Acknowledgments
This work was supported by a grant from the Doris Duke Charitable Foundation to the University of California, San Francisco to fund Clinical Research Fellow Joelle Rosser. While working on this project, M.J.H. was supported through a National Institutes of Health career development award (KL2 RR024130-04).
Conflict of interest
The authors do not have any conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosser, J.I., Hamisi, S., Njoroge, B. et al. Barriers to Cervical Cancer Screening in Rural Kenya: Perspectives from a Provider Survey. J Community Health 40, 756–761 (2015). https://doi.org/10.1007/s10900-015-9996-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-015-9996-1