Abstract
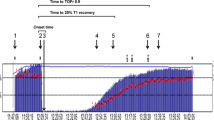
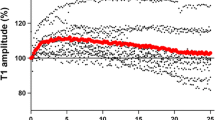
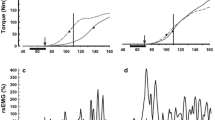
Acceleromyography is characterised by an increase of the twitch response T1 (first twitch of the train-of-four [TOF]) during first 30 min of monitoring known as the staircase phenomenon. In adults the staircase phenomenon can be avoided by tetanic prestimulation. This study examined, if tetanic prestimulation eliminates the staircase phenomenon in children. After written informed consent, the neuromuscular function of 80 children, 10 in each age group (< 6 months, 6–12 months, 12–24 months, 2–3 years, 3–6 years, 6–12 years, 12–18 years, and ≥ 18 years) was measured on both arms simultaneously over 30 min under general anaesthesia. The ulnaris nerve was stimulated using the TOF technique every 15 s. The twitch response (T1, TOF ratio [TOFR]) was measured by acceleromyography. Before calibration, tetanic prestimmulation (50 Hz for 5 s) was administered to one randomly selected arm. The effect of tetanic prestimulation and age was analysed using general linear models based on the normalized T1 and TOFRs of both arms. Tetanic prestimulation significantly affected T1 values avoiding the staircase phenomenon (p < 0.0001). After 5.8 min [1.0–17.2 min] the normalized T1 values increased to 117% [102–147%] without prestimulation (p < 0.0001) independent of the age group (p = 0.539). The normalized TOFR was stable throughout the observation period of 30 min 100% [95–107%]. Infants (> 12 weeks), children, and young adults (< 18 years) develop similar characteristics of the staircase phenomenon than adults. Tetanic prestimulation prevents the staircase phenomenon in these age groups. The stability of the TOFR reading confirms its value to monitor neuromuscular function over time.
Registration: The study was registered as NCT02552875 on Clinical Trials.gov on July 29, 2014.



Similar content being viewed by others
References
Kirmeier E, Eriksson LI, Lewald H, Jonsson Fagerlund M, Hoeft A, Hollmann M, Meistelman C, Hunter JM, Ulm K, Blobner M, Contributors P. Post-anaesthesia pulmonary complications after use of muscle relaxants (POPULAR): a multicentre, prospective observational study. Lancet Respir Med. 2018. https://doi.org/10.1016/S2213-2600(18)30294-7.
Fuchs-Buder T, Claudius C, Skovgaard LT, Eriksson LI, Mirakhur RK, Viby-Mogensen J, 8th International Neuromuscular M. Good clinical research practice in pharmacodynamic studies of neuromuscular blocking agents II: the Stockholm revision. Acta Anaesthesiol Scand. 2007;51(7):789–808. https://doi.org/10.1111/j.1399-6576.2007.01352.x.
Mazzinari G, Errando CL, Diaz-Cambronero O, Martin-Flores M. Influence of tetanic stimulation on the staircase phenomenon and the acceleromyographic time-course of neuromuscular block: a randomized controlled trial. J Clin Monit Comput. 2019;33(2):325–32. https://doi.org/10.1007/s10877-018-0157-9.
Krarup C. Enhancement and diminution of mechanical tension evoked by staircase and by tetanus in rat muscle. J Physiol. 1981;311:355–72.
Ritchie JM, Wilkie DR. The effect of previous stimulation on the active state of muscle. J Physiol. 1955;130(2):488–96.
Deschamps S, Trager G, Mathieu PA, Hemmerling TM. The staircase phenomenon at the corrugator supercilii muscle in comparison with the hand muscles. Br J Anaesth. 2005;95(3):372–6. https://doi.org/10.1093/bja/aei183.
Lee GC, Iyengar S, Szenohradszky J, Caldwell JE, Wright PM, Brown R, Lau M, Luks A, Fisher DM. Improving the design of muscle relaxant studies. Stabilization period and tetanic recruitment. Anesthesiology. 1997;86(1):48–54.
Driessen JJ, Robertson EN, Booij LH. Acceleromyography in neonates and small infants: baseline calibration and recovery of the responses after neuromuscular blockade with rocuronium. Eur J Anaesthesiol. 2005;22(1):11–5.
Zhou ZJ, Wang X, Zheng S, Zhang XF. The characteristics of the staircase phenomenon during the period of twitch stabilization in infants in TOF mode. Paediatr Anaesth. 2013;23(4):322–7. https://doi.org/10.1111/pan.12041.
Kopman AF, Kumar S, Klewicka MM, Neuman GG. The staircase phenomenon: implications for monitoring of neuromuscular transmission. Anesthesiology. 2001;95(2):403–7.
Claudius C, Skovgaard LT, Viby-Mogensen J. Is the performance of acceleromyography improved with preload and normalization? A comparison with mechanomyography. Anesthesiology. 2009;110(6):1261–70. https://doi.org/10.1097/ALN.0b013e3181a4f239.
Liang SS, Stewart PA, Phillips S. An ipsilateral comparison of acceleromyography and electromyography during recovery from nondepolarizing neuromuscular block under general anesthesia in humans. Anesth Analg. 2013;117(2):373–9. https://doi.org/10.1213/ANE.0b013e3182937fc4.
McCoy EP, Mirakhur RK, Connolly FM, Loan PB. The influence of the duration of control stimulation on the onset and recovery of neuromuscular block. Anesth Analg. 1995;80(2):364–7.
Rassier DE, Macintosh BR. Coexistence of potentiation and fatigue in skeletal muscle. Braz J Med Biol Res. 2000;33(5):499–508.
Rassier DE, Tubman LA, MacIntosh BR. Staircase in mammalian muscle without light chain phosphorylation. Braz J Med Biol Res. 1999;32(1):121–9.
Curless RG. Developmental patterns of peripheral nerve, myoneural junction and muscle: a review. Prog Neurobiol. 1977;9(4):197–209.
Round JM, Jones DA, Chapman SJ, Edwards RH, Ward PS, Fodden DL. The anatomy and fibre type composition of the human adductor pollicis in relation to its contractile properties. J Neurol Sci. 1984;66(2–3):263–72.
Krarup C. Electrical and mechanical responses in the platysma and in the adductor pollicis muscle: in normal subjects. J Neurol Neurosurg Psychiatry. 1977;40(3):234–40.
Diaz-Cambronero O, Flor Lorente B, Mazzinari G, Vila Montanes M, Garcia Gregorio N, Robles Hernandez D, Olmedilla Arnal LE, Argente Navarro MP, Schultz MJ, Errando CL, group IPs. A multifaceted individualized pneumoperitoneum strategy for laparoscopic colorectal surgery: a multicenter observational feasibility study. Surg Endosc. 2019;33(1):252–60. https://doi.org/10.1007/s00464-018-6305-y.
Ali HH, Utting JE, Gray C. Stimulus frequency in the detection of neuromuscular block in humans. Br J Anaesth. 1970;42(11):967–78.
Suzuki T, Fukano N, Kitajima O, Saeki S, Ogawa S. Normalization of acceleromyographic train-of-four ratio by baseline value for detecting residual neuromuscular block. Br J Anaesth. 2006;96(1):44–7. https://doi.org/10.1093/bja/aei273.
Motamed C, Donati F. Sevoflurane and isoflurane, but not propofol, decrease mivacurium requirements over time. Can J Anaesth. 2002;49(9):907–12. https://doi.org/10.1007/BF03016872.
Hemmerling TM, Schuettler J, Schwilden H. Desflurane reduces the effective therapeutic infusion rate (ETI) of cisatracurium more than isoflurane, sevoflurane, or propofol. Can J Anaesth. 2001;48(6):532–7. https://doi.org/10.1007/BF03016828.
Miller RD, Eger EI 2nd, Way WL, Stevens WC, Dolan WM. Comparative neuromuscular effects of Forane and halothane alone and in combination with d-tubocurarine in man. Anesthesiology. 1971;35(1):38–42.
Goudsouzian NG. Maturation of neuromuscular transmission in the infant. Br J Anaesth. 1980;52(2):205–14.
Funding
There was no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
CU, MW, TM, RZ, SK, TS, BG, FZ, BS declare that they have no conflict of interest. MB received honoraria for board services and lectures from GE Health Care (Helsinki, Finland), MSD (Haar, Germany), and Grünenthal (Aachen, Germany).
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (Institutional Ethics Committee,University of Regensburg, Regensburg, Germany; protocol No. 14-101-0114) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Unterbuchner, C., Werkmann, M., Ziegleder, R. et al. Shortening of the twitch stabilization period by tetanic stimulation in acceleromyography in infants, children and young adults (STSTS-Study): a prospective randomised, controlled trial. J Clin Monit Comput 34, 1343–1349 (2020). https://doi.org/10.1007/s10877-019-00435-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-019-00435-4