Abstract
Amid the rise of antibiotic-resistant bacterial strains in human populations, novel solutions are necessary. Nanoparticles, renowned for their adaptability, offer a diverse range of research avenues, notably as antibacterial agents. Coupling antibiotics with nanoparticles stands out as a potential strategy, effectively intriguing drug delivery challenges and circumventing antibiotic resistance. This review focuses on studies of nanoparticles in conjugation with the aminoglycoside antibiotic gentamicin and their effectiveness as novel nanoparticle conjugates, their applications in drug delivery and enhanced bactericidal effects. In most cases, the nanoparticle conjugates were found to efficiently kill different bacterial strains, which was mainly dependent on the size, stability and concentration of the nanoparticles. Despite the several limitations such as nanotoxicity, accumulation of intravenously injected nanomaterials in tissues and organs, the urge and potential for the advancement of nanoparticle-drug conjugates still demands more scientific advancements.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Despite the scientific advancements of antibiotics, the ever-growing bacterial species gaining resistance to commercially available antibiotics are now a major threat throughout the world as antibiotics become more endangered in terms of efficiency [1, 2]. Ever since the use of antibiotics in therapeutic settings began in the 1930s, there has been an epidemic of antibiotic resistance [3]. Alexander Fleming warned that the overuse of antibiotics will lead to the development of drug-resistant microorganisms in the future following his discovery of penicillin in 1945 [4]. We are currently dealing with serious complications that, according to many experts, would prevent the value of today’s antibiotics from being used in 100 years, contrary to what he predicted decades earlier [5, 6].
Overuse and misuse of antibiotics mainly due to the inappropriate prescription of drugs by medical professionals is one of the leading causes of increasing microbial resistance [7]. Extensive use of antibiotics in the agricultural field and the availability of a few novel antibiotics also contribute to this crisis [8]. Thus, the need for novel bactericidal components is an alternative approach to address the current situation.
Nanobiotics, where nanoparticles themselves have manipulable antimicrobial properties, have been considered a promising approach [9,10,11]. Nanoparticles can evade drug resistance compared to commercially available antibiotics in certain cases [12]. Conjugation of nanoparticles with antimicrobial properties to certain antibiotics that are readily available in the market has shown promising outcomes towards antibiotic resistance, drug delivery, long-term imaging and tracking [13, 14].
The issue of organ toxicity linked with metallic nanoparticle conjugates remains a dynamic area of investigation and advancement. Researchers are actively engaged in comprehending the mechanisms of toxicity, enhancing nanoparticle design, and devising tactics to reduce their adverse impacts [15]. Multiple strategies have been employed, concentrating particularly on the modification of nanoparticle surfaces to alleviate their toxicity. Through the incorporation of biocompatible coatings for example polymers, a protective shield is established, effectively diminishing direct interaction between the nanoparticles and biological systems. Petrow et al. produced core-shell nanoparticles by enveloping Ag NPs with a cross-linked poly (L-lysine) coat containing doxorubicin. The study exhibited favorable biocompatibility and the induction of cancer cell death upon drug release [16]. The concern of nanoparticle biodegradability has also been acknowledged as a notable limitation. In response, liposomal nanoparticles have been introduced as a strategy to overcome this hurdle [17].
Gentamicin, an aminoglycoside that was first isolated from M. purpurea species in 1963, provided a breakthrough in treating infections caused by gram-negative aerobes such as P. aeruginosa [18]. Since then, gentamicin has been commonly used in a range of medical applications as a broad-spectrum antibiotic [19]. In the recent past, there have been good clinical outcomes of gentamicin as well as the opposite in some situations. It is still one of the most commonly used antibiotics in the medical field due to its low cost and broad-spectrum efficiency [20]. However, intramuscular or intravenous application is required since it is poorly absorbed by the gastrointestinal tract [21]. Moreover, its cationic structure and accumulation in tissues are linked to tissue-specific toxicities, including nephrotoxicity and ototoxicity [22]. Gentamicin also exhibits vestibulotoxicity, inducing harm to the vestibular system [23].
Gentamicin, an aminoglycoside antibiotic, is employed to treat severe infections caused by aerobic gram-negative bacteria. Instead of being a singular compound, gentamicin is composed of three main components - gentamicin C1, C1a, and C2- as well as several minor components. The major components differ in the level of methylation within the 2-amino-hexose (purpurosamine) ring. In this ring, gentamicin C1a lacks methyl groups, while both C1 and C2 possess a methyl group at the 6′ position. Additionally, gentamicin C1 is N-methylated at this position, whereas C1a and C2 have free amines. The C2 component consists of two stereoisomers [24]. The level of distinct gentamicin components varies depending on the drug’s manufacturing method and the manufacturer, making it difficult to investigate aspects such as pharmacokinetics and bactericidal effects due to an unknown combination of chemically related compounds [25]. Gentamicin is accessible through diverse trade names, contingent on the pharmaceutical producer and geographic location. A few of the renowned trade names associated with gentamicin comprise Garamycin, Gentak, Cidomycin etc. It has been effectively employed in treating a wide spectrum of infections such as eye, ear, and bloodstream infections caused by bacteria [15]. Gentamicin is also combined with other drugs to treat various infections. The combination drugs is available in diverse formats, including tablets, capsules, syrups, creams, gels, ointments, liquids, and injections. Presently, there are 26 brands listed in the drug directory (https://www.medindia.net/drug-price/gentamicin-combination.htm) that offer generic versions of gentamicin combination, each marketed under distinct brand names for example, Beclotis-CG, Pred-G, Valisone-G and Dermitop etc. Gentamicin is commonly used to treat various bacterial infections, including serious conditions like peritonitis (inflammation in peritoneum), endocarditis, sepsis and septic shock, pneumonic plague (infection in lungs), and meningitis (inflammation of meninges). (Fig. 1)
The trade names, composition, and specific formulations of gentamicin are compared in Table 1.
The different infections and microbes treated using gentamicin. Parts of the figure were drawn by using pictures from Servier Medical Art. Servier Medical Art by Servier is licensed under a Creative Commons Attribution 3.0 Unported License (https://creativecommons.org/licenses/by/3.0/)
Nanoparticle Conjugates with Gentamicin
The chemical make-up and arrangement of nanoparticles assist in the active targeting of antibiotics, extended binding and protection from enzyme degradation. These properties eliminate the use of higher doses of antibiotics, leading to fewer side effects. Many scientists have produced novel classes of antimicrobial agents, such as nanoparticle conjugates, to narrow the complications and development of multidrug-resistant infectious bacteria. Nanoparticles that have bactericidal effects themselves, for example, gold, silicon dioxide, iron oxide, titanium dioxide, etc., and organic nanoparticles such as liposomes fused with commercially accessible antibiotics have been examined against many multidrug resistant bacteria [26]. These nanoparticle conjugates are synthesized by two classes of interactions: chemical and physical. Some of the chemical reactions include amine surface-functionalized nanoparticles adjoined to antibiotics containing succinimide ester or isothiocyanate groups, aldehyde functionalized nanoparticles conjugated with antibiotics containing a hydrazine group, etc. Similarly, physical interactions include electrostatic, hydrophobic and biotin-avidin interactions [27]. Possible applications of NPs-gentamicin conjugations are depicted in Fig. 2.
Various applications of Gentamicin conjugated nanoparticles. Parts of the figure were drawn by using pictures from Servier Medical Art. Servier Medical Art by Servier is licensed under a Creative Commons Attribution 3.0 Unported License (https://creativecommons.org/licenses/by/3.0/)
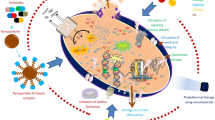
Nanoparticle-antibiotic conjugates represent a remarkable advancement in the field of targeted drug delivery and enhanced therapeutic efficacy. These conjugates involve the integration of antibiotics with nanoparticles, creating a synergistic approach to combat infections. The mechanism of action of nanoparticle-antibiotic conjugates revolves around several key aspects that collectively contribute to their effectiveness [15]. Schematic representation of mechanism of action of nanoparticle-antibiotic conjugates are shown in Fig. 3.
The design of an effective therapeutic system necessitates the consideration of both spatial and temporal parameters. One widely utilized approach involves employing nanoparticles as carriers for drug delivery. During the process of transporting molecules from one location to another within an organism, it becomes crucial to comprehend the time frame associated with the delivery procedure, as well as to gain insight into how these molecules interact within the intricate biological milieu. This task becomes particularly challenging when dealing with targeted drug delivery systems, given the intricate nature of the system, which can impose limitations on the movement of cargoes within a living organism. A successful design for nanoparticle-based drug delivery hinges on the ability to precisely navigate the drug to its intended destination within the appropriate timeframe, even amidst the turbulent currents like blood flow and various layers of biological barriers [28]. Also, a three-fold increase in biofilm reduction was observed, with silver-Polymyxin B nanoparticle conjugate systems, compared to neat Ag nanoparticles. This signifies how nanoparticle conjugates improve the efficacy of drugs [29].
This review emphasizes studies using various nanoparticle and gentamicin conjugates against different bacterial strains to analyse the increased antibacterial action in comparison to free gentamicin, as well as their applications in drug delivery.
Gold Nanoparticles
Gold nanoparticles have been used to treat various conditions, such as diarrhea, epilepsy, leprosy, mental diseases, plague and syphilis [30, 31, 32, 33]. However, in 1971, two researchers from Britain, Faulk and Taylor, introduced colloidal gold-antibody conjugation to visualize the surface antigens in salmonellae. Thereafter, it has been successfully used in several other applications, such as diagnosis, imaging, and cancer treatment [34].
Mixtures of gentamycin with gold nanoparticles (15 nm) were assessed for enhanced bactericidal activity. The formation of the conjugates was confirmed by UV spectroscopic analysis as well as the blue to red color conversion of the solution. Antimicrobial activity was evaluated by the disk diffusion method which exhibited no difference in antimicrobial activity between mixtures and free gentamicin. When compared with available literature, it is known that the nanoparticles should be stabilized, where in this study the color of the nanoparticle solution did not match with the corresponding single-particle non-aggregated colloidal color, which could be the reason that the conjugates did not show enhanced antibacterial activity [35].
Several studies have investigated the potency of gentamicin-gold nanoparticle conjugates to effectively target certain bacterial species. For example, gold nanospheres (10–12 nm) conjugated to gentamicin were successfully synthesized and used to assess their use in drug delivery to staphylococcal infected foci. Conjugation was confirmed by both UV‒Vis spectroscopic analysis and by the color change from red to purple‒blue. Approximately 347 gentamicin molecules were coupled to each gold nanosphere, and this combination showed a significantly enhanced antibacterial effect when compared to free gentamicin against S. aureus bacterial species. The effect of the conjugates on BALB/c mice indicates a considerable accumulation of conjugates in the site of infection compared to uninfected muscle after 30 min [36].
In another study, gentamicin was covalently bound to gold nanoparticles by the capping agents cysteine and glutathione and characterized using Fourier transform infrared spectroscopy (FTIR), UV‒Vis spectroscopy and transmission electron microscopy (TEM) analysis. Glutathione-capped nanoparticles showed higher antibacterial activity than cysteine, owing to the elevated amounts of gentamicin released from the nanocarrier. Moreover, glutathione-capped gold nanoparticles showed drug release for at least 48 h, whereas cysteine showed a maximum of 24 h. However, the conjugates showed a lower minimum inhibitory concentration (MIC) value against methicillin-resistant S. aureus and S. aureus strains [37].
Gold nanorods were conjugated with gentamicin using the Nanothink acid linker to facilitate the targeted delivery of gentamicin to infection sites caused by Staphylococcus aureus. The gentamicin-gold nanorod conjugate exhibited an enhanced antibacterial effect, as evidenced by the minimal inhibitory concentration and minimum bactericidal concentration values. Moreover, in a mouse model, a biodistribution study demonstrated the specific localization of the gentamicin-GNR complex at the site of staphylococcal infection with a high level of sensitivity [38]. The efficacy of gold nanocages loaded with gentamicin along with other antibiotics was tested against P. aeruginosa in a study. The results showed the choice of antibiotic to be critical and that the gentamicin-loaded gold nanocages targeted a conserved superficial protein of the bacterial cell membrane, being highly effective against biofilms of P. aeruginosa [39]. In addition, another approach used gold nanoparticles functionalized with chitosan and loaded with gentamicin to demonstrate their antibacterial activity. Analysis was performed through a novel computational approach that could realistically describe controlled antibiotic release from complex hybrid systems. Based on modelling data, it was noted that the amount of gentamicin bound to the gold nanoparticles was minor, but the conjugates were able to show very efficient and slower release of the drug [40].
To investigate the antibacterial efficacy of gentamicin-attached gold nanoparticles against E. coli, another study was conducted. It was observed that in the case of larger gold nanoparticles, the ratios for inhibition regions with gentamicin were higher with respect to gentamicin alone. Gentamicin-conjugated gold nanoparticles were also more successful than the other categories in preventing bacterial growth [41]. Immediate antibacterial therapy of wounds minimizes the risk of infection and enhances wound healing. On the other hand, the products used to treat wounds frequently fail to provide both sterilization (particularly for super bacteria) and hydration, and some may even induce additional wound harm. As a wound dressing, gold nanoparticles were combined with gentamicin sulfate (GS) and put into a mixture of konjac glucomannan (KGM) and gelatin (KGM/Gelatin@Au NPs/GS). Antibacterial tests revealed that gold nanoparticles enhanced the antibacterial activity of GS, with Au NPs/GS effectively eradicating bacteria, particularly super bacteria [42]. One-pot synthesis produces gentamicin-coupled gold nanoparticles (G-GNPs) that are easy, resilient and environmentally acceptable, with gentamicin acting both as a reducing and stabilizing agent. G-GNPs further demonstrated superior antibacterial properties when compared to pure gentamicin, and G-GNPs also showed tremendous effects towards gentamicin-resistant E. fergusonii ATCC 35,469 [43].
The chemical structures of different capping agents coupled with gold nanoparticles are given in Fig. 4.
Summary of size of the gold nanoparticles used in gentamycin conjugation, experiments conducted, bacterial species used and applications of the nanoconjugates are given in Table 2.
Silver Nanoparticles
Silver nanoparticles are used in numerous sectors, such as biomedicine, industrial purposes, and health care. The exceptional physical and chemical properties, such as electrical and optical properties, of silver nanoparticles allow them to be used in various fields [44].
Several approaches have employed antibiotic-conjugated silver nanoparticles for antimicrobial applications. For instance, in a 2019 study, silver nanoparticles 60–80 nm in size were biosynthesized from P. glomerate species, and the combined effect of these nanoparticles with gentamicin was tested against P. aeruginosa, S. aureus and E. coli. The combination of silver nanoparticles with gentamicin showed increased inhibition for all three species. The study also stated that the synthesis of nanoparticles using P. glomerata can certainly eradicate the problem of using harsh chemicals, which can have unfavorable effects in its applications and implementations, hence allowing the nanoparticles to become more biocompatible [45].
In another study, silver nanoparticles, 5–30 nm in size, were biologically synthesized using (A) flavus and conjugated with 5 different antibiotics, including gentamicin, and these were tested against 8 different strains of bacteria, namely, K. pneumoniae, E. coli, M. luteus, S. aureus, P. aeruginosa, E. faecalis, (B) subtilis and A. baumannii. A potent range from 12 to 25 mm zone of inhibition was indicated by gentamicin infused with nanoparticles, while free gentamicin showed an average of 11.3 mm zone of inhibition and regular silver nanoparticles showed an average of 14.8 mm zone of inhibition [46]. Similarly, a combination of gentamicin and biosynthesized silver nanoparticles from Bacillus species, with a diameter range of 14–42 nm, showed a slight increase in antibacterial activity when tested against several bacterial species. Gentamicin alone showed a zone of inhibition of 14 mm, whereas gentamicin with silver nanoparticles showed a 15 mm inhibition zone, resulting in a fold increase of 0.15, particularly against the S. epidermidis strain 73. The mixture also showed a 1.04-fold increase in the zone of inhibition against S. epidermidis strain 145, with inhibition areas of 7 and 10 mm for gentamicin alone and the mixture, respectively. Gentamicin loaded silver nanoparticles have not significantly boosted the antibacterial activity [47].
Magnetic nanoparticles (MNPs) composed of polyacrylic acid (PAA) were fabricated. These MNPs were then coated with multidimensional films comprising gentamicin along with tannic acid (TA) and silver nanoparticles (Ag NPs). This intricate synthesis aimed to evaluate the antibiofilm characteristics and controlled drug release properties of the particles, ultimately enhancing biocompatibility. In vitro drug release models showed that the MNP + gentamicin + Ag NP complex showed pH-responsive release properties, proving that the complex may be used to deliver gentamicin molecules on demand to the infection foci. The complex also showed a significant increase in biofilm disruption in both E. coli and S. aureus due to the use of magnetic field navigation that guided the nanoparticles to penetrate the biofilm, showing the dual responsive release of gentamicin. The proposed mechanism of action was excess production of reactive oxygen species (ROS) produced by the complex, which aided in biofilm disruption and eradication [48]. Another study was conducted to observe the antimicrobial properties of AgNPs generated by Bacillus sp. (SJ14) in conjunction with ciprofloxacin, methicillin, gentamicin and rifampicin. Multidrug-resistant and biofilm-forming coagulase-negative bacteria were evaluated with the conjugates, namely, isolates of S. epidermidis and S. haemolyticus. Almost all of the conjugates’ MICs (minimum inhibitory concentrations) were lowered, except for methicillin, which was lowered from 250 g/mL to 7.8 g/mL against S. epidermidis. Except for rifampicin, the synergistic effect of nanoparticles and antibiotics could be demonstrated by fractional inhibitory concentration (FIC) measurement [49].
A summary of the size of the silver nanoparticles used in gentamycin conjugation, experiments conducted, bacterial species and applications of nanoconjugates are given in Table 3.
Bimetallic Nanoparticles
Nanoparticles comprising two dissimilar metals are called bimetallic nanoparticles. Their constituent metals and nanometric size determine their properties. These are increasingly gaining interest because they allow optimization of the plasmon absorption band energy that can be utilized as a versatile tool for biosensing [50].
Bimetallic nanoparticles of silver and gold were synthesized biologically by P. veronii in a study with a size range of 5–50 nm, and their antibacterial effects were tested. It was reported that the combination of nanoparticles with gentamicin showed an 11.15% increase in antibacterial effect compared to the antibiotic alone against S. aureus, B. subtilis, E. coli and K. pneumoniae bacterial strains [51].
Silica Nanoparticles
Silica (silicon dioxide, SiO2) is yet another inorganic compound with a wide variety of biomedical applications. It possesses flexible surfaces that can be easily modified and easily synthesized and has inert chemical properties. Mesoporous silica particles are one of the three highly manufactured nanomaterials. However, continued exposure to silica nanoparticles poses adverse health effects affecting the immune system [52].
SiO2 nanoparticles sized 327 nm, when conjugated to gentamicin and used as carriers for the antibiotic, aided in the prolonged release of gentamicin. The key purpose of the study was the chemical synthesis of SiO2 nanoparticles, conjugation with gentamicin and characterization of the conjugates for their potential antimicrobial administration, especially in orthopaedic applications [53]. Moreover, antimicrobial assays conducted on SiO2 nanoparticles, free gentamicin and SiO2 gentamicin nanoconjugates separately against three bacterial species (B. subtilis, P. fluorescens and E. coli) showed that the conjugate systems showed a higher antibiotic effect towards gram-positive bacteria. SiO2 nanoparticles themselves did not show any antimicrobial effect, and the conjugates had a higher MIC value than free gentamicin [53].
In another study, thin films embedded with mesoporous silica nanoparticles and filled with gentamicin were used to assess their antibacterial efficiency as well as antibiofilm activity for a prolonged period. The persistence of the inhibition zone around the thin film for up to 103 days proved that the thin film complex could prevent bacterial growth for a long period. Additionally, the antibiofilm activity of the nanocomposites against S. aureus species remained active for more than two months [54].
Iron Oxide Nanoparticles
Iron oxide nanoparticles possess unique magnetic properties, in addition to their nontoxic and biodegradable behavior. These properties enable them to be used in various fields, mainly in diagnosis and therapy [55].
For instance, magnetic mesoporous bioactive glass nanoparticles (MMBG) were prepared in a study from iron oxide (Fe3O4) with a particle size of 15–30 nm and a pore size of 5.4 nm. MMBG showed a higher loading efficiency of 65.7–68.6% than nonmesoporous nanoparticles, which were 14.3–19.6%. This meant that the higher drug encapsulation and high surface area were due to the mesoporous property of the nanoparticles. Additionally, MMBG had a higher drug release rate during the first 12 h and showed prolonged release for more than 6 days [56].
Another investigation employed iron oxide nanoparticles with a size of 10–14 nm and coated them with gentamicin to analyse their bactericidal effects. The nanoparticles showed superparamagnetic character and a coercivity close to zero according to the magnetization curve. Furthermore, an initial outburst of release followed by a sustained release for approximately 250 h was observed. Simultaneously, antibacterial experiments against S. aureus, B. subtilis, P. aeruginosa and E. coli indicated colony reduction at a concentration of 2–3 mg/ml, leading to 99% bacterial cell death. Amino acid leakage studies depicted that cellular RNA and DNA were distorted by the conjugated systems [57].
Similarly, Fe3O4 nanoparticles were capped with sodium alginate, and gentamicin was loaded into these magnetic nanoparticles in a 2018 study. On average, 56.7% of gentamicin was loaded into the sodium alginate-capped magnetic nanoparticles. The MIC values of the conjugates showed that they could inhibit all visible growth against P. aeruginosa and were relatively more effective than free gentamicin [58].
A different investigation analysed carboxyl surface-functionalized iron oxide nanoparticles conjugated with gentamicin for their antibiofilm properties and checked the importance of the homogenous distribution of the drug throughout the thickness of the biofilm. The nanoparticles had an average diameter of 60 nm. This small size allowed prevention of reticular rejection of the complex Additionally, a clear scattered distribution of nanoparticles along the biofilms was noted, which depended on the time of exposure to the magnetic field. Five minutes of exposure to an external magnetic field showed a homogenous distribution of the drug as well as higher antibacterial efficiency when compared to the complex without exposure. On assessing the conjugate-mediated eradication of biofilms of bacterial species E. cloacae, S. aureus, K. pneumonia, A. baumannii, P. aeruginosa and E. faecalis, similar minimum bactericidal concentration (MBC) values of the conjugates and free gentamicin were obtained. Therefore, clinical applications of magnetic nanoparticle complexes are feasible once the magnetic field exposure time is optimized and drug-loaded nanoparticles are distributed uniformly throughout the biofilm [59].
A technique was employed wherein gentamicin was mixed with iron oxide nanoparticles and a polymer known as polyethylene glycol along with Fe3O4 NPs. The results indicated a remarkable enhancement in the antibacterial activity of the nanoparticles against the tested bacterial strains. In particular, the Fe3O4 NPs + PEG + Gen formulation exhibited significant inhibitory effects on P. mirabilis and S. epidermidis [60]. The agar well diffusion method was used to study the antibacterial activity of chloramphenicol and gentamicin and their formulation with encapsulated iron oxide nanoparticles. Escherichia coli and Staphylococcus aureus strains were resistant to the antibacterial effects of drug-encapsulated Fe2O3 NPs, possibly in a dose-dependent manner [61].
A summary of the size of the iron oxide nanoparticles used in gentamycin conjugation, experiments conducted, bacterial species used and applications of nanoconjugates are given in Table 4.
Polymeric Nanoparticles
Synthetic and natural polymers are commonly used nanomaterials to construct nanoparticle-based drug carriers. These are also used in imaging and detection of apoptosis [62].
Poly lactic-co-glycolic acid (PLGA) nanoparticles loaded with gentamicin were prepared to assess the enhanced antimicrobial activity against P. aeruginosa. PLGA nanoparticles 251 nm in size were chemically synthesized by a water-in-oil-in-water (w/o/w) emulsion, each encapsulating approximately 22.4 µg of the drug at pH 7.4. The PLGA-gentamicin complex showed higher MIC, MBC and minimum biofilm eradication concentration (MBEC) values than free gentamicin. This is more likely due to the interaction of the biofilm anionic polysaccharide with the cationic gentamicin, which limits the availability of the drug to act against the resident bacteria. Moreover, the PLGA-gentamicin complex provided continuous and controlled release of the drug for up to 16 days [63].
In another study, PLGA nanoparticles loaded with gentamicin were used to assess their efficacy as a drug delivery system to treat osteomyelitis infection. Zeta sizer analysis showed that the PLGA-loaded gentamicin molecules had a diameter in the range of 200–400 nm, as well as a low polydispersity index, showing that all the nanoparticles had a uniform size distribution. The size of the nanoparticle was also seen to decrease with increasing surfactant concentration (polyvinyl alcohol). Drug release analysis showed an initial burst of release, where 26% of the drug was released during the first 12 h, followed by sustained release for more than 30 days. When the antibacterial effects against S. aureus and S. epidermidis species were analysed, both species showed similar average zones of inhibition, and MIC values for S. epidermidis were 0.064 µg/ml and S. aureus had a higher value of 0.500 µg/ml [64].
In the same manner, a study was conducted on PLGA nanoparticles loaded with gentamicin (with a diameter of 227 nm) for the treatment of intracellular K. pneumoniae infection in the lungs. Evidence proved that K. pneumoniae could survive inside macrophages both in vitro and in vivo. Since gentamicin alone was less permeable through the cell membrane, it limited the clinical effectiveness of the drug when treating intracellular pathogens. The overall objective of this study was to examine the competence of PLGA-loaded gentamicin complexes to deliver their antibiotic payload more efficiently than free gentamicin. However, the results of the antimicrobial assay showed a reduced effect when compared with free gentamicin, as determined by the MIC values. It was postulated that this was due to the encapsulation of the drug inside the nanoparticle, preventing immediate exposure to the bacteria. Drug release analysis showed that over a 120-hour period, 80% of the drug was released, further validating the hypothesis [65]. A double emulsion approach was used in a separate study to combine PLGA and GS. Gentamicin-loaded PLGA nanoparticles exhibited outstanding antibacterial characteristics and many prospects in making smart wound dressings [66].
A different study prepared gentamicin loaded with polydopamine nanoparticles to assess its antibacterial efficiency. Gentamicin was added to polydopamine using in situ polymerization techniques at various monomer and gentamicin concentrations. Gentamicin’s amine group and polydopamine’s hydroxyl group formed hydrogen bonds, resulting in conjugation. Additionally, conjugates made with a monomer to drug ratio of 1:1 demonstrated the maximum loading capacity. Gentamicin had an MIC value of 1.90 g/ml, and the polydopamine-gentamicin complex had an MIC value of 0.6 mg/ml when the bactericidal activity was tested against P. aeruginosa and S. aureus. By themselves, polydopamine nanoparticles did not exhibit any bactericidal properties. The possibility that certain drug molecules were trapped inside the nanoparticles appeared to be the cause of the higher MIC value. Therefore, further possible release mechanisms needed to be implied to increase gentamicin release from polydopamine nanoparticles [67].
Another work focused on nanoparticles composed of maleic anhydride-comethyl vinyl ether to assess their efficiency in ophthalmic drug delivery. These polymeric nanoparticles were created using the solvent evaporation approach. The amine groups of gentamicin facilitated ionic interactions with the nanoparticle, yielding an average nanoparticle size of 150 nm. The efficiency of encapsulation also dramatically increased with increasing ionic strength and pH. In vivo drug release analysis of the complex showed a significantly extended release of gentamicin when injected into rabbit cornea [68]. Chitosan nanoparticles have a positive surface charge and mucoadhesive properties, which help them adhere to mucus membranes and continuously release the drug. They are used in the treatment of various conditions, such as pulmonary diseases, cancer and gastrointestinal diseases [69].
In a study, gentamicin- and salicylic acid-loaded spherical chitosan nanoparticles were synthesized with a high zeta potential ( > + 30 mV) and an average size of 148–345 nm. In vitro drug release results indicated that in phosphate buffer saline at pH 7.4, initially, an outburst of release was observed, followed by slow release [70]. In a 2016 study, a chitosan/fucoidan nanoparticle conjugate system for the pulmonary delivery of gentamicin was developed with a size range of 270–300 nm. Drug release results showed biphasic release with zero-order kinetics during the initial 10 h of the experiment and sustained release for the next 75 h [71].
Chitosan nanoparticles, when prepared by the gelation method, could also be used as a nanocarrier for gentamicin. Cotton fabrics and blends with polyester were treated with gentamicin and chitosan conjugates to obtain increased antibacterial activity. Testing of the antibacterial properties was performed on S. aureus and E. coli. The disk diffusion test revealed that, due to a larger concentration of the drug at the bacterial cell membrane, the antibiotic’s activity shifted from bacteriostatic to bactericidal as the antibiotic load increased. Due to the nature of the cell membrane, the composites had stronger antibacterial activity against gram-positive bacteria [72].
In another study, gentamicin-loaded phosphatidylcholine-chitosan nanoparticles were synthesized to assess their effects on biofilms and intracellular bacteria. These nanoparticles varied in size from 76 to 137 nm. Through FTIR analysis, it was seen that phosphatidylcholine was absorbed onto the chitosan nanoparticles and that gentamicin occupied the outermost layer of the system. The standard amount of gentamicin per nanoparticle was 20 µg/ml. The MIC values were further obtained against four strains of bacteria, namely, P. aeruginosa, L. monocytogenes, E. coli and S. aureus. A dramatic decrease in biofilm formation was also reported by L. monocytogenes species when treated with the conjugates compared to free gentamicin, and similar effects were observed with the P. aeruginosa biofilm [73].
In a 2020 study, cranberry proanthocyanidin-chitosan nanoparticles with gentamicin were synthesized and assessed for their antibacterial efficiency. Different ratios of proanthocyanidin, chitosan and gentamicin were used to form four different complexes with a size range of 242–277 nm. Antimicrobial assays showed that the nanoparticles with gentamicin could agglutinate E. coli, S. aureus, and P. aeruginosa species and that the proanthocyanidin-chitosan nanoparticles with gentamicin showed greater antibacterial activity than gentamicin alone [74].
Ascorbic acid (AA) and gentamicin sulphate (GM) were delivered using chitosan nanoparticles (CSNPs) as a carrier. The in vitro antibacterial activity and cytotoxicity of the produced particles were assessed. The produced particles (GM-AA-CSNPs) demonstrated encapsulation effectiveness and loading capacities of 89% and 22%, respectively, under the ideal conditions of 4:1:1 of chitosan to drug ratio [75].
A summary of the size of the polymer nanoparticles used in gentamycin conjugation, experiments conducted, bacterial species used and applications of nanoconjugates are given in Table 5.
Calcium Carbonate/Calcium Silicate Nanoparticles
Researchers extensively utilize calcium carbonate (CaCO3) in biomedical applications due to its well-known characteristics, including widespread availability, affordability, safety, biocompatibility, pH sensitivity, and slow biodegradability. Recently, there has been a surge of interest in using it as a drug delivery system for various categories of medications [76].
Gentamicin-loaded calcium carbonate (CaCO3) nanoparticles were synthesized in a study to assess their drug delivery against the bacterium S. aureus. The nanoparticles were prepared by the microemulsion method with a particle size of 113–120 nm and characterized by dynamic light scattering, SEM, XRD analysis, differential scanning calorimetry, FTIR and drug release profiles. An in vitro drug release study showed slow release for 12 h. Additionally, both free gentamicin and the conjugate systems, on the basis of their MIC values, showed similar bactericidal effects against S. aureus species [77].
In another study, mesoporous calcium silicate nanoparticles were prepared by a sol-gel method and loaded with gentamicin. These were then used to assess and increase the osteogenic drug delivery efficiency for endodontic materials. The nanoparticles had an average diameter of 200 nm, with an average pore size of 3.05 nm and a high surface area to volume ratio. In vitro, drug release experiments indicated that the nanoparticles maintained sustained release [78].
Another study was conducted to assess the synergistic effect of gentamicin-loaded CaCO3. The synthesized nanoparticles exhibited a chain-like structure with a good polydispersity index and a size range from 60 to 80 nm. The interaction between gentamicin and the nanoparticles was assessed by FTIR analysis, where a hydrogen bond interaction between the two molecules was speculated. In vitro drug release results showed that 50% of the drug was released within the first hour, and the total amount of drug was released after 24 h, showing that the release of the drug was slower compared to the free form of gentamicin. When assessing the antimicrobial activity of the conjugates, the conjugate system showed enhanced antibacterial effects compared to free gentamicin against B. subtilis. The proposed mechanism of action of the conjugates was that, due to the overall negative charge and size, the conjugates are absorbed into the cell wall by intermolecular forces, increasing cell wall damage and permeability [79].
A summary of the size of the calcium carbonate/calcium silicate nanoparticles used in gentamycin conjugation, experiments conducted, bacterial species used and applications of nanoconjugates are given in Table 6.
Liposomes
Liposomes are phospholipid vesicles containing more than one concentric lipid bilayer surrounding distinct aqueous spaces. It can trap lipophilic and hydrophilic compounds. This property of liposomes allows them to encapsulate a wide range of various drug molecules. Therefore, they are well-studied nanocarriers for targeted drug delivery with excellent cellular and tissue uptake and enhanced biodistribution of compounds [80].
Various studies have investigated the improved antibacterial efficacy of antibiotics, specifically gentamicin-conjugated liposomes. For instance, in a study, liposomes made from different lipid compositions and cholesterol were encapsulated with gentamicin, resulting in nanoparticles having an average diameter range from 408 to 418 nm with 4–5% drug encapsulation efficiency. These liposomal complexes could retain 70% of the drug up to 48 h, where liposomes incubated at 4 ℃ could retain more antibiotics compared to liposomes incubated at 30 ℃ [81]. Gentamicin-encapsulated liposomes were compared with free gentamicin to assess the antibiotic activity against P. aeruginosa. The liposomes had an average size of 420–440 nm and an encapsulation efficiency of 4.51%. The MIC values for the complex were significantly lower than those for free gentamicin [82].
In another study, liposomes encapsulated with gentamicin and gallium metal were used to assess their enhanced antimicrobial effects. The synthesized liposomes had a diameter of 310–335 nm. The MIC and MBC showed that the complex of liposomes and gentamicin was more effective than free gentamicin against P. aeruginosa biofilms. The cell viability assay using A549 cells suggested that encapsulated gentamicin was much safer than free gentamicin [83].
Liposomes were synthesized to evaluate the stability of the composite as a nanocarrier of gentamicin in another study. The outcomes demonstrated prolonged drug release for smaller gentamicin liposomes [84].
The efficacy of gentamicin and liposomal formulations with distinct surface charges was tested against K. oxytoca and P. aeruginosa in a different investigation. The liposomal drug complex was synthesized by the dehydration method, which yielded a liposomal structure size of 620–840 nm. A 1.8–43.6% drug encapsulation efficiency was seen by the complex, which could retain 60% of the drug content during the initial 48 h. The MIC values of neutral liposomes were less than those of gentamicin alone, and the MBC values were twofold-fold lower than those of gentamicin alone. Moreover, negatively charged liposomes showed similar results as free gentamicin [85].
A summary of the size of liposomes used in gentamycin conjugation, experiments conducted, bacterial species used and applications of nanoconjugates are given in Table 7.
Selenium Nanoparticles
Selenium, an essential nutrient element with significant biological roles, presents an intriguing opportunity for integration with antibacterial agents. It is a trace element necessary for maintaining health and promoting growth through dietary intake. Elemental selenium, being the least toxic form of selenium, has gained considerable interest in its nano form. Recent research has highlighted the anticancer, antioxidant, antibacterial, and antibiofilm properties of selenium nanoparticles. Notably, these nanoparticles have exhibited remarkable antimicrobial activity against pathogenic bacteria, fungi, and yeasts in various studies [86].
The antibacterial and antibiofilm properties of biogenic selenium nanoparticles (Se NPs) created by green technologies that are both cost-effective and environmentally acceptable were analysed in a study. The production of Se NPs was discussed in this work using 2 distinct techniques: a biogenic procedure employing Penicillium chrysogenum filtrate and a gentamicin medication after gamma irradiation. In comparison to biogenic Se NPs, synthetic Se NPs-CN have a promising antibacterial ability against all urinary tract infections (UTIs) caused by the microorganisms tested. Se NPs-CN has shown antibacterial activity against C. albicans with a zone of inhibition (ZOI) of 26.0 mm, 23.0 mm for E. coli and 20.0 mm for S. aureus [87].
Mechanism of Action
Understanding the mechanism of action of nanoparticle-antibiotic conjugates aids in the improvement and development of more viable composites and predicts more efficient designs to mitigate antimicrobial resistance. However, the exact mechanism of action of the nanoparticle composites contributing to the enhanced bactericidal effects remains unknown [88]. It is important to know both the mechanisms of action of antibacterial nanoparticles alone and their action in conjugation with gentamicin. To predict the exact mechanism of action of different nanoparticle-conjugated gentamicin, many studies have been conducted exploring the bactericidal effects of nanoparticles. The ability of nanoparticles to infiltrate biofilms and alter bacterial metabolism are two of their most potent strategies for causing cell death [11]. Oxidative stress, nonoxidative processes, and metal ion release in metal oxide nanoparticles are the other often hypothesized modes of action [89].
To achieve bactericidal effects, nanoparticles should be in contact with bacterial cell walls by electrostatic attraction, van der Waal forces, receptor‒ligand or hydrophobic interactions. The nanoparticles then cross the bacterial membrane and gather along the metabolic pathway, which influences the function and shape of the cell membrane. This is followed by the nanoparticles interacting with the bacterial cells’ basic components such as DNA, lysosomes, ribosomes and enzymes that lead to oxidative stress, changes in the permeability of the membrane, heterogeneous alterations, enzyme inhibition, protein deactivation and changes in gene expression [90]. The bactericidal mechanisms of action of nanoparticles are generally described as one of three models, namely, the induction of oxidative stress [91], the release of metal ions [92] and nonoxidative mechanisms [93], with the possibility of all three mechanisms occurring simultaneously. The major processes underlying the bactericidal effects of nanoparticles are (1) cell membrane disruption, (2) generation of reactive oxygen species, (3) bacterial cell membrane penetration, and (4) intracellular induction of antibacterial effects-interaction with proteins and DNA.
The antibacterial effects of nanoparticles depend on their stability, size, and concentration in the medium [94]. Smaller nanoparticles typically exhibit greater antibacterial activity; the reason for this, according to one concept, is that they have a higher surface area to volume ratio than larger nanoparticles, which leads to an increase in the production of ROS that damage DNA, lipids, and proteins essential for bacterial cell growth [95]. However, some studies have shown that large nanoparticles are equally as effective, showing that size is not the most important factor in inducing bacterial toxicity [96]. The charge of the nanoparticle is another important factor that affects the antimicrobial activity. A study showed that positively charged amine-functionalized nanoparticles were able to change the function of the electron transport chain of bacteria. Nanoparticles with a positive charge can electrostatically attach to the negatively charged bacterial cell wall, causing them to exhibit enhanced toxicity [97, 98]. The acidic nature of nanoparticles has been found to aid in attachment to the bacterial cell wall, which can further enhance the bactericidal effects [99].
The chemical structure of aminoglycosides also facilitates their antibacterial effects. They are considered polycationic species; that is, they contain multiple electrolyte groups. Due to this property, they show binding affinity to the negatively charged moieties in the outer membrane of gram-negative aerobes and nucleic acids. The bactericidal activity is mainly due to the inhibition of protein synthesis where the drug binds to the 16 S rRNA and eventually disrupts the integrity of the cell membrane of the bacterium where the Mg2+ bridges between the adjacent lipopolysaccharide molecules are disrupted [100].
Nanoparticles influence cellular functions such as cellular differentiation and adhesion in bacterial cells [101]. Metal oxide nanoparticles such as copper, zinc, iron, titanium, etc., with smaller particle sizes have been reported to show promising bactericidal effects. Similarly, the antibacterial effect of SiO2 nanoparticles is more significant at smaller sizes due to the increased surface area [102]. Metal oxide nanoparticles follow two major mechanisms of action when exhibiting bactericidal effects. The first mechanism is the direct contact of the nanoparticles with the cell wall of the bacteria and their destruction by the oxidation reaction, which produces ROS. The second mechanism involves nanoparticles acting as free radical scavengers [103].
A study conducted on silver-polyethyleneimine nanoparticles showed that the composite attached to the bacterial cell wall and some fused within the bacterial cell wall. In contrast, negatively charged silver-citrate nanoparticles showed no attachment. Silver nanoparticles exhibit bactericidal effects by disrupting the disulfide linkages of the proteins present in the transmembrane layer of the bacterial cell wall following the decreased rate of metabolic processes that eventually lead to cell death [104]. Silver metal ions catalyze the formation of free radicals that can oxidize cellular macromolecules. These free radicals can diffuse and travel through the bloodstream. As the microbes are not exposed to the radicals for a long period, the ability of the bacteria to gain resistance is reduced. However, gold nanoparticles act by breaking down the bacterial cell wall, which can aid some antibiotics that are less penetrative through the cell membrane. Gold nanoparticles, when combined with a small amount of gentamicin, showed that the mixture of nanoparticles and antibiotic showed a significant enhancement in its antibacterial effect when compared to gentamicin alone [105]. Another experiment carried out on gold nanoparticles showed that these nanoparticles exhibit toxicity as a result of cell wall rupture induced by direct contact between the nanoparticle and the cell wall, rather than the generation of ROS [106]. Gold nanoparticles also induce cytoderm damage, which results from the electrostatic attraction between the negatively charged cytoderm and the positively charged nanoparticles [107]. The results of scanning electron microscopy of gold nanoparticles labelled with cefradine showed damage to the cell wall through direct physical contact. Furthermore, fluorescent probe analysis of the nanoparticles ruled out the possibility of ROS formation leading to the loss of cell viability [108].
Discussion
The need for novel antibiotic agents that are effective against resistant bacterial strains is gaining much attention around the world [109, 110]. Many scientific groups have tried to create potential commercial antibiotic or antimicrobial peptides by combining antimicrobial nanoparticles with a drug [111].
In this review, we describe nanoparticle conjugate systems with one of the aminoglycoside antibiotics, gentamicin, and its application in drug delivery and enhanced antibacterial activity. Gentamicin is hydrophilic and tends to penetrate less through the hydrophobic bacterial cell wall; thus, higher concentrations are prescribed, which leads to harmful side effects such as nephrotoxicity and ototoxicity [100]. When gentamicin is conjugated with nanoparticles, the nanohybrids have a higher antimicrobial activity than the free antibiotic itself [53]. The produced composites might have some mechanism that could enhance the bactericidal activity, such as their potential to attach to or penetrate the cell wall, resulting in the delivery of a greater number of gentamicin molecules into a highly localized volume as each nanoparticle is surrounded by several drug moieties acting as a sole group [112]. A wide field of novel antimicrobial agents can offer a considerable outlook for the expansion of therapeutic agents in the treatment of bacterial infectious diseases that have an alternative mechanism of action, thus overcoming the current mechanism of antibiotic resistance [113].
Many conjugate systems have a good bactericidal effect against infectious bacteria, but the exact mechanism of many is not known [10]. Understanding the mechanism of the bactericidal effects of existing antibiotics and their nanoconjugate systems is one of the salient parts to originate more modern and biocompatible nanohybrids that may aid in coping with the difficulty of bacteria gaining resistance in the future [114, 115]. The tracking and movement of the conjugates can be aided using fluorescent peptides and nanoparticles, which will be useful in understanding their binding sites, parameters that need to be well analysed for high efficiency and mode of action [116, 117]. Proper understanding and advanced research on nanohybrids can lead to the progress of a novel, triumphant plan of action as a cure for human bacterial infections.
Conclusion
Antibacterial resistance is a great concern, and it can be handled by enhancing the drug efficiency using novel nanotechnology methods. Many studies summarised in this review indicated that gentamicin-nanoparticle conjugates shown better anti bactericidal effects and and also efficient drug delivery strategies. Understanding the mechanism of enhanced activity may lead to discovery of novel antibiotics which will address the growing problem of antibacterial resistance. However, a thorough research on safety is essential for the success of these approaches.
Data Availability
Data used for manuscript have been retrieved from published studies and other publications available online. Data sourced are listed in the reference section.
References
Fair RJ, Tor Y (2014) Antibiotics and bacterial resistance in the 21st century. Perspect Medicin Chem 6: 25–64. https://doi.org/10.4137/PMC.S14459
Aslam B, Wang W, Arshad, MI, Khurshid M, Muzammil S, Rasool MH, Nisar MA, Alvi RF, Aslam MA, Qamar MU, Salamat MKF (2018) Antibiotic resistance: a rundown of a global crisis. Infect Drug Resist 11: 1645–1658. https://doi.org/10.2147/IDR.S173867
Carlet J, Jarlier V, Harbarth S, Voss A, Goossens H, Pittet D (2012) Ready for a world without antibiotics? The pensières antibiotic resistance call to action. Antimicrob. Resist. Infect. Control 11: 1–11. https://doi.org/10.1186/2047-2994-1-11
Aminov RI (2010) A brief history of the antibiotic era: lessons learned and challenges for the future. Front. Microbiol 1: 134–141. https://doi.org/10.3389/fmicb.2010.00134
Davies J, Davies D (2010) Origins and evolution of antibiotic resistance. Microbiol Mol Biol Rev 74: 417–433. https://doi.org/10.1128/MMBR.00016-10
Ventola CL (2015) The antibiotic resistance crisis: part 1: causes and threats. P T. 40: 277–283. 25859123
Llor C, Bjerrum L (2014) Antimicrobial resistance: risk associated with antibiotic overuse and initiatives to reduce the problem. Ther Adv Drug Saf 5: 229–241. https://doi.org/10.1177/2042098614554919
Durso LM, Cook KL (2014) Impacts of antibiotic use in agriculture: what are the benefits and risks?. Curr Opin Microbiol 19: 37–44. https://doi.org/10.1016/j.mib.2014.05.019
Azarsina M, Kasraei S, Yousefi-Mashouf R, Dehghani N, Shirinzad M (2013) The antibacterial properties of composite resin containing nanosilver against Streptococcus mutans and Lactobacillus. J Contemp Dent Pract 14: 1014–1018. https://doi.org/10.5005/jp-journals-10024-1442
Beyth N, Houri-Haddad Y, Domb A, Khan W, Hazan R (2015) Alternative antimicrobial approach: nano-antimicrobial materials. Evid. Based Complementary Altern. Med 1: 1–16. https://doi.org/10.1155/2015/246012
Wang L, Hu C, Shao L (2017) The antimicrobial activity of nanoparticles: present situation and prospects for the future. Int J Nanomedicine 12: 1227–1249. https://doi.org/10.2147/IJN.S121956
Okkeh, M., Bloise, N., Restivo, E., De Vita, L., Pallavicini, P., & Visai, L. (2021). Gold nanoparticles: can they be the next magic bullet for multidrug-resistant bacteria?. Nanomater 11: 312–340. https://doi.org/10.3390/nano11020312
Thakur BK, Kumar A, Kumar D (2019) Green synthesis of titanium dioxide nanoparticles using Azadirachta indica leaf extract and evaluation of their antibacterial activity. S Afr J Bot 124: 223–227. https://doi.org/10.1016/j.sajb.2019.05.024
Yeh YC, Huang TH, Yang SC, Chen CC, Fang JY (2020) Nano-based drug delivery or targeting to eradicate bacteria for infection mitigation: a review of recent advances. Front Chem 8: 286–308. https://doi.org/10.3389/fchem.2020.00286
Lee NY, Ko WC, amp, Hsueh PR (2019) Nanoparticles in the treatment of infections caused by multidrug-resistant organisms. Frontiers in pharmacology, 10, 1153–1163. https://doi.org/10.3389/fphar.2019.01153
Długosz O, Szostak K, Staroń A, Pulit-Prociak J, Banach M (2020) Methods for reducing the toxicity of metal and metal oxide NPs as biomedicine. Materials 13: 279–298. https://doi.org/10.3390/ma13020279
Zhang Z, Yao S, Hu Y, Zhao X, Lee RJ (2022) Application of lipid-based nanoparticles in cancer immunotherapy. Front Immunol 13: 967505–967521. https://doi.org/10.3389/fimmu.2022.967505.
Gonzalez III LS, Spencer JP (1998) Aminoglycosides: a practical review: Am Fam Physician, 1811–1820. 9835856
Chen C, Chen Y, Wu P, Chen B (2014) Update on new medicinal applications of gentamicin Evidence-based review. J Formos Med Assoc. 113: 72–82. https://doi.org/10.1016/j.jfma.2013.10.002
Tiwari A, Sharma P, Vishwamitra B, Singh G (2021) Review on Surface Treatment for Implant Infection via Gentamicin and Antibiotic Releasing Coatings. Coatings 11: 1006–1027. https://doi.org/10.3390/coatings11081006
Crcek M, Zdovc J, Kerec Kos M (2019) A review of population pharmacokinetic models of gentamicin in paediatric patients. J Clin Pharm Ther 44: 659–674. https://doi.org/10.1111/jcpt.12850
Lopez-Novoa JM, Quiros Y, Vicente L, Morales AI, Lopez-Hernandez FJ (2011) New insights into the mechanism of aminoglycoside nephrotoxicity: an integrative point of view. Kidney Int 79: 33–45. https://doi.org/10.1038/ki.2010.337
Hayward RS, Harding J, Molloy R, Land L, Longcroft-Neal K, Moore D, Ross JD (2018) Adverse effects of a single dose of gentamicin in adults: a systematic review. Br J Clin Pharmacol 84: 223–238. https://doi.org/10.1111/bcp.13439
Isoherranen N, Lavy E, Soback S. (2000) Pharmacokinetics of gentamicin C(1), C(1a), and C(2) in beagles after a single intravenous dose. Antimicrob Agents Chemother. 44: 1443–1450. https://doi.org/10.1128/aac.44.6.1443-1447.2000
Tamma, PD, Cosgrove SE, Maragakis LL (2012) Combination therapy for treatment of infections with gram-negative bacteria. Clin microbiol rev 25: 450–470. https://doi.org/10.1128/CMR.05041-11
Alizadeh A, Salouti M, Alizadeh H, Kazemizadeh AR, Safari AA, Mahmazi S (2017) Enhanced antibacterial effect of azlocillin in conjugation with silver nanoparticles against Pseudomonas aeruginosa. IET Nanobiotechnol 11: 942–947. https://doi.org/10.1049/iet-nbt.2017.0009
Ijaz, I., Gilani, E., Nazir, A., & Bukhari, A. (2020) Detail review on chemical, physical and green synthesis, classification, characterizations and applications of nanoparticles. Green Chem Lett Rev 13: 223–245. https://doi.org/10.1080/17518253.2020.1802517
Kumar A, Zhang X, Liang XJ (2013) Gold nanoparticles: emerging paradigm for targeted drug delivery system. Biotechnology advances 31: 593–606. https://doi.org/10.1016/j.biotechadv.2012.10.002
Aflakian F, Mirzavi F, Aiyelabegan HT, Soleimani A, Navashenaq JG, Karimi-Sani I, Vakili-Ghartavol R (2023) Nanoparticles-based therapeutics for the management of bacterial infections: a special emphasis on FDA approved products and clinical trials. Eur J Pharm Sci 188: 106515–106531. https://doi.org/10.1016/j.ejps.2023.106515
Yilmaz CU, Emik S, Orhan N, Temizyurek A, Atis M, Akcan U, Kaya M (2020) Targeted delivery of lacosamide-conjugated gold nanoparticles into the brain in temporal lobe epilepsy in rats. Life Sciences 257: 118081–118091. https://doi.org/10.1016/j.lfs.2020.118081
Zhu S, Jiang X, Boudreau MD, Feng G, Miao Y, Dong S, Yin JJ (2018) Orally administered gold nanoparticles protect against colitis by attenuating Toll-like receptor 4-and reactive oxygen/nitrogen species-mediated inflammatory responses but could induce gut dysbiosis in mice. J nanobiotechnology 16: 1–18. https://doi.org/10.1186/s12951-018-0415-5
Yang D, Ma J, Zhang Q, Li N, Yang J, Raju PA, Cui Y (2013) Polyelectrolyte-coated gold magnetic nanoparticles for immunoassay development: Toward point of care diagnostics for syphilis screening. Analytical chemistry 85: 6688–6695. https://doi.org/10.1021/ac400517e
Daraee, H., Eatemadi, A., Abbasi, E., Fekri Aval, S., Kouhi, M., & Akbarzadeh, A. (2016). Application of gold nanoparticles in biomedical and drug delivery. Artif Cells Nanomed Biotechnol, 44: 410–422. https://doi.org/10.3109/21691401.2014.955107
Dykman LA, Khlebtsov NG (2011) Gold nanoparticles in biology and medicine: recent advances and prospects. Acta Nat 3: 34–55. https://doi.org/10.32607/20758251-2011-3-2-34-55
Burygin GL, Khlebtsov BN, Shantrokha AN, Dykman LA, Bogatyrev VA, Khlebtsov NG (2009) On the Enhanced Antibacterial Activity of Antibiotics Mixed with Gold Nanoparticles. Nanoscale Res Lett 4: 794–801. https://doi.org/10.1007/s11671-009-9316-8
Ahangari A, Salouti M, Heidari Z, Kazemizadeh AR, Safari AA (2013) Development of gentamicin-gold nanospheres for antimicrobial drug delivery to Staphylococcal infected foci. Drug Deliv 20: 34–39. https://doi.org/10.3109/10717544.2012.746402
Perni S, Prokopovich P (2014) Continuous release of gentamicin from gold nanocarriers. RSC Adv 4: 51904–51910. https://doi.org/10.1039/C4RA10023A
Salout M, Heidari Z, Ahangari A, Zare S (2016) Enhanced delivery of gentamicin to infection foci due to Staphylococcus aureus using gold nanorods. Drug Deliv 23: 49–54. https://doi.org/10.3109/10717544.2014.903533
Meeker DG, Wang T, Harrington WN, Zharov VP, Johnson SA, Jenkins SV, Oyibo S E, Walker CM, Mills WB, Shirtliff ME, Beenken KE,Chen J, Smeltzer MS (2018) Versatility of targeted antibiotic-loaded gold nanoconstructs for the treatment of biofilm-associated bacterial infections. Int J Hyperthermia 34: 209–219. https://doi.org/10.1080/02656736.2017.1392047
Monti S, Jose J, Sahajan A, Kalarikkal N, Thomas S (2019) Structure and dynamics of gold nanoparticles decorated with chitosan-gentamicin conjugates: ReaxFF molecular dynamics simulations to disclose drug delivery. Phys Chem Chem Phys 21: 13099–13108. https://doi.org/10.1039/C9CP02357G
Mohanta B, Chakraborty A, Selvara S, Roy A (2020) Bactericidal effect of gentamicin conjugated gold nanoparticles. Micro Nano Lett 15: 657–661. https://doi.org/10.1049/mnl.2020.0194
Zou Y, Xie R, Hu E, Qian P, Lu B, Lan G, Lu F (2020) Protein-reduced gold nanoparticles mixed with gentamicin sulfate and loaded into konjac/gelatin sponge heal wounds and kill drug-resistant bacteria. Int. J. Biol. Macromol 148: 921–931. https://doi.org/10.1016/j.ijbiomac.2020.01.190
Sharma D, Chaudhary A (2021) One Pot Synthesis of Gentamicin Conjugated Gold Nanoparticles as an Efficient Antibacterial Agent. J. Clust Sci 32: 995–1002. https://doi.org/10.1016/j.colsurfb.2013.01.061
Zhang XF, Liu ZG, Shen W, Gurunathan, S. (2016) Silver nanoparticles: synthesis, characterization, properties, applications, and therapeutic approaches. Int J Mol Sci 17: 1534–1568. https://doi.org/10.3390/ijms17091534
Birla SS, Tiwari VV, Gade AK, Ingle AP, Yadav AP, Rai MK (2009) Fabrication of silver nanoparticles by Phoma glomerata and its combined effect against Escherichia coli, Pseudomonas aeruginosa and Staphylococcus aureus. Lett Appl Microbiol 48: 173–179. https://doi.org/10.1111/j.1472-765X.2008.02510.x
Naqvi S Z, Kiran U, Ali MI, Jamal A, Hameed A, Ahmed S, Ali N (2013) Combined efficacy of biologically synthesized silver nanoparticles and different antibiotics against multidrug-resistant bacteria. Int J Nanomedicine 8: 3187–3195. https://doi.org/10.2147/IJN.S49284
Thomas R, Nair AP, Kr S, Mathew J, Ek R (2014) Antibacterial activity and synergistic effect of biosynthesized AgNPs with antibiotics against multidrug-resistant biofilm-forming coagulase-negative staphylococci isolated from clinical samples. Appl Biochem Biotechnol 173: 449–460. https://doi.org/10.1007/s12010-014-0852-z
Wang X (2018) Microenvironment-Responsive Magnetic Nanocomposites Based on Silver Nanoparticles/Gentamicin for Enhanced Biofilm Disruption by Magnetic Field. ACS Appl. Mater. Interfaces. 10: 34905–34915. https://doi.org/10.1021/acsami.8b10972
Thomas R, Jishma P, Snigdha S, Soumya KR, Mathew J, Radhakrishnan EK (2020) Enhanced antimicrobial efficacy of biosynthesized silver nanoparticle based antibiotic conjugates. Inorg. Chem. Commun 117: 107978–107983. https://doi.org/10.1016/j.inoche.2020.107978
Sharma G, Kumar A, Sharma S, Naushad M, Dwivedi RP, ALOthman ZA; Mola GT (2019) Novel development of nanoparticles to bimetallic nanoparticles and their composites: a review. J Nanosci Nanotechnol 31: 257–269. https://doi.org/10.1016/j.jksus.2017.06.012
Baker S, Pasha A, Satish S (2015) Biogenic nanoparticles bearing antibacterial activity and their synergistic effect with broad spectrum antibiotics: Emerging strategy to combat drug resistant pathogens. SAUDI Pharm. J 25: 44–51. https://doi.org/10.1016/j.jsps.2015.06.011
Chen L, Liu J, Zhang Y, Zhang G, Kang Y, Chen A, Feng X, Shao L (2018) The toxicity of silica nanoparticles to the immune system. Nanomedicine 13: 1939–1962. https://doi.org/10.2217/nnm-2018-0076
Mosselhy DA. Ge Y, Gasik M, Nordström K, Natri O, Hannula SP (2016) Silica-gentamicin nanohybrids: synthesis and antimicrobial action. Materials 9: 170–186. https://doi.org/10.3390/ma9030170
Tamanna T, Landersdorfer CB, Ng HJ, Bulitta JB, Wood P, Yu A (2018) Prolonged and continuous antibacterial and anti-biofilm activities of thin films embedded with gentamicin-loaded mesoporous silica nanoparticles. Appl Nanosci 8: 1471–1482. https://doi.org/10.1007/s13204-018-0807-8
Cotin G, Piant S, Mertz D, Felder-Flesch D, Begin-Colin S (2018) Iron oxide nanoparticles for biomedical applications: synthesis, functionalization, and application. In: Laurent S, Mahmoudi M (ed) In Iron Oxide Nanoparticles for Biomedical Applications, 1st edn. Elsevier, Amsterdam, The Netherlands, 43–88. https://doi.org/10.1016/B978-0-08-101925-2.00002-4
Liu YZ, LiY, Yu XB, Liu LN, Zhu ZA, Guo YP (2014) Drug delivery property, bactericidal property and cytocompatibility of magnetic mesoporous bioactive glass. Mater Sci Eng C Mater Biol Appl 41: 196–205. https://doi.org/10.1016/j.msec.2014.04.037
Bhattacharya B, Neogi S (2017) Gentamicin coated iron oxide nanoparticles as novel antibacterial agents. Mater Res Express 4: 095005–095033. https://doi.org/10.1088/2053-1591/aa8652
Douzandeh-Mobarrez B, Ansari-Dogaheh, M, Eslaminejad T, Kazemipour M, Shakibaie M (2018) Preparation and Evaluation of the Antibacterial Effect of Magnetic Nanoparticles Containing Gentamicin: A Preliminary In vitro Study. Iran J Biotechnol 16: 287–293. https://doi.org/10.21859/ijb.1559
Quan K, Zhang Z, Ren Y, Busscher HJ, Van Der Mei HC, Peterson BW (2020) Homogeneous Distribution of Magnetic, Antimicrobial-Carrying Nanoparticles through an Infectious Biofilm Enhances Biofilm-Killing Efficacy. ACS Biomater Sci Eng. 6: 205–212. https://doi.org/10.1021/acsbiomaterials.9b01425
Abdulsada FM, Hussein NN, Sulaiman GM, Al Ali A, Alhujaily M (2022) Evaluation of the Antibacterial Properties of Iron Oxide, Polyethylene Glycol, and Gentamicin Conjugated Nanoparticles against Some Multidrug-Resistant Bacteria. J Funct Biomater 13: 138–155. https://doi.org/10.3390/jfb13030138
Sharma, V., Sharma, J. K., Kansay, V., Sharma, V. D., Sheoran, R., Singh, M., … Bera, M. K. (2023). Chloramphenicol and Gentamycin-encapsulated Iron Oxide Nanoparticles as a Nanocarrier for Antibacterial Efficacy via Targeted Drug Delivery. Nano Biomed Eng 15: 170–178. https://doi.org/10.26599/NBE.2023.9290029
Bolhassani A, Javanzad S, Saleh T, Hashemi M, Aghasadeghi MR, Sadat SM (2014) Polymeric nanoparticles: potent vectors for vaccine delivery targeting cancer and infectious diseases. Hum Vaccin Immunother 10: 321–332. https://doi.org/10.4161/hv.26796
Abdelghany SM, Quinn DJ, Ingram RJ, Gilmore BF, Donnelly RF, Taggart CC, Scott CJ (2012) Gentamicin-loaded nanoparticles show improved antimicrobial effects towards Pseudomonas aeruginosa infection. Int J Nanomedicine 7: 4053–4063. https://doi.org/10.2147/IJN.S34341
Posadowska U, Brzychczy-Włoch M, Pamuła E (2015) Gentamicin loaded PLGA nanoparticles as local drug delivery system for the osteomyelitis treatment. Acta Bioeng Biomech 17: 41–48. https://doi.org/10.5277/ABB-00188-2014-02
Jiang L, Greene MK, Insua JL, Pessoa JS, Small DM, Smyth P, McCann AP, Cogo, F, Bengoechea JA, Taggart CC, Scott CJ (2018) Clearance of intracellular Klebsiella pneumoniae infection using gentamicin-loaded nanoparticles. J Control Release 279: 316–325. https://doi.org/10.1016/j.jconrel.2018.04.040
Sun Y, Bhattacharjee A, Reynolds M, Li YV (2021) Synthesis and characterizations of gentamicin-loaded poly-lactic-co-glycolic (PLGA) nanoparticles J Nanopart Res 23: 1–15. https://doi.org/10.4161/biom.22494
Batul R, Bhave M, Mahon PJ, Yu A (2020) Polydopamine Nanosphere with In-Situ Loaded Gentamicin and Its Antimicrobial Activity. Molecules 25: 1–13. https://doi.org/10.3390/molecules25092090
Basu A, Domb A (2020) Ion Exchange Nanoparticles for Ophthalmic Drug Delivery. Bioconjug Chem 31: 2726–2736. https://doi.org/10.1021/acs.bioconjchem.0c00521
Mohammed MA, Syeda J, Wasan KM, Wasan EK (2017) An overview of chitosan nanoparticles and its application in non-parenteral drug delivery. Pharmaceutics 9: 53–79. https://doi.org/10.3390/pharmaceutics9040053
Ji J, Hao S, Wu D, Huang R, Xu Y (2011) Preparation, characterization and in vitro release of chitosan nanoparticles loaded with gentamicin and salicylic acid. Carbohydr Polym 85:803–808. https://doi.org/10.1016/j.carbpol.2011.03.051
Huang YC, Li RY, Chen JY, Chen JK (2016) Biphasic release of gentamicin from chitosan/fucoidan nanoparticles for pulmonary delivery. Carbohydr Polym 138:114–122. https://doi.org/10.1016/j.carbpol.2015.11.072
El-Alfy EA, El-Bisi MK, Taha GM, Ibrahim HM (2020) Preparation of biocompatible chitosan nanoparticles loaded by tetracycline, gentamycin and ciprofloxacin as novel drug delivery system for improvement the antibacterial properties of cellulose-based fabrics. Int J Biol Macromol 161: 1247–1260. https://doi.org/10.1016/j.ijbiomac.2020.06.118
Qiu Y, Xu D, Sui G, Wang D, Wu M, Han L, Mu H, Duan J (2020) Gentamicin decorated phosphatidylcholine-chitosan nanoparticles against biofilms and intracellular bacteria. Int J Biol Macromol 156: 640–647. https://doi.org/10.1016/j.ijbiomac.2020.04.090
Alfaro-Viquez E, Esquivel-Alvarado D, Madrigal-Carballo S, Krueger CG, Reed JD (2020) Antimicrobial proanthocyanidin-chitosan composite nanoparticles loaded with gentamicin. Int J Biol Macromol 162: 1500–1508. https://doi.org/10.1016/j.ijbiomac.2020.07.213
Abdel-Hakeem, M. A., Abdel Maksoud, A. I., Aladhadh, M. A., Almuryif, K. A., Elsanhoty, R. M., & Elebeedy, D. (2022). Gentamicin–Ascorbic Acid Encapsulated in Chitosan Nanoparticles Improved In Vitro Antimicrobial Activity and Minimized Cytotoxicity. Antibiotics, 11: 1530–1543. https://doi.org/10.3390/antibiotics11111530
Maleki Dizaj S, Barzegar-Jalali M, Zarrintan MH, Adibkia K, Lotfipour F (2015) Calcium carbonate nanoparticles as cancer drug delivery system. Exp opinion on drug delivery, 12, 1649–1660. https://doi.org/10.1517/17425247.2015.1049530
Maleki Dizaj S, Lotfipour F, Barzegar-Jalali M, Zarrintan MH, Adibkia K (2016) Physicochemical characterization and antimicrobial evaluation of gentamicin-loaded CaCO3 nanoparticles prepared via microemulsion method. J Drug Deliv Sci. Technol 35:16–23. https://doi.org/10.1016/j.jddst.2016.05.004
Huang C, Huang T, Kao C, Wu Y, Chen, W (2017) Mesoporous Calcium Silicate Nanoparticles with Drug Delivery and Odontogenesis Properties. J Endod 43:69–76. https://doi.org/10.1016/j.joen.2016.09.012
Pan X, Chen S, Li D, Rao W, Zheng Y, Yang Z, Li L, Guan X, Chen Z (2018) The synergistic antibacterial mechanism of gentamicin-loaded CaCO3 nanoparticles. Front Chem 5:1–9. https://doi.org/10.3389/fchem.2017.00130
Sercombe L, Veerati T, Moheimani F, Wu SY, Sood AK, Hua S (2015) Advances and challenges of liposome assisted drug delivery. Front Pharmacol 6:1–18. https://doi.org/10.3389/fphar.2015.00286
Mugabe C, Azghani A, Omri A (2005) Liposome-mediated gentamicin delivery: Development and activity against resistant strains of Pseudomonas aeruginosa isolated from cystic fibrosis patients. J Antimicrob Chemother 55:269–271. https://doi.org/10.1093/jac/dkh518
Rukholm G, Mugabe C, Azghani AO, Omri A (2006) Antibacterial activity of liposomal gentamicin against Pseudomonas aeruginosa: A time-kill study. Int J Antimicrob Agents 27:247–252. https://doi.org/10.1016/j.ijantimicag.2005.10.021
Halwani M, Yebio B, Suntres ZE, Alipour M, Azghani AO, Omri A (2008) Co-encapsulation of gallium with gentamicin in liposomes enhances antimicrobial activity of gentamicin against Pseudomonas aeruginosa. J Antimicrob Chemother 62:1291–1297. https://doi.org/10.1093/jac/dkn422
Jia Y, Joly H, Omri A (2008) Liposomes as a carrier for gentamicin delivery: Development and evaluation of the physicochemical properties. Int J Pharm 359:254–263. https://doi.org/10.1016/j.ijpharm.2008.03.035
Alhariri M, Majrashi MA, Bahkali AH, Almajed FS, Azghani AO, Khiyami MA, Alyamani EJ, Aljohani SM, Halwani MA (2017) Efficacy of neutral and negatively charged liposome-loaded gentamicin on planktonic bacteria and biofilm communities. Int J Nanomedicine 12:6949–6961. https://doi.org/10.2147/IJN.S141709
Vahdati M, Tohidi Moghadam T (2020) Synthesis and characterization of selenium nanoparticles-lysozyme nanohybrid system with synergistic antibacterial properties. Sci rep10, 1–10. https://doi.org/10.1038/s41598-019-57333-7
El-Sayyad GS, El-Bastawisy HS, Gobara M, El-Batal AI (2020) Gentamicin-assisted mycogenic selenium nanoparticles synthesized under gamma irradiation for robust reluctance of resistant urinary tract infection-causing pathogens. Biol Trace Elem Res 195:323–342. https://doi.org/10.1007/s12011-019-01842-z
Vazquez-Muñoz R, Meza-Villezcas A, Fournier PGJ, Soria-Castro E, Juarez-Moreno, K, Gallego-Hernández AL, Huerta-Saquero A (2019) Enhancement of antibiotics antimicrobial activity due to the silver nanoparticles impact on the cell membrane. PLoS One 14:1–18. https://doi.org/10.1371/journal.pone.0224904
Michael CA, Dominey-Howes D, Labbate M (2014) The antimicrobial resistance crisis: Causes, consequences, and management. Public Health Front 2:1–8. https://doi.org/10.3389/fpubh.2014.00145
Xu Y, Wei MT, Ou-Yang HD, Walker SG, Wang HZ, Gordon CR, Guterman S, Zawacki E, Applebaum E, Brink PR, Rafailovich M, Mironava T (2016) Exposure to TiO2 nanoparticles increases Staphylococcus aureus infection of HeLa cells. J. Nanobiotechnology14:29–31. https://doi.org/10.1186/s12951-016-0184-y
Gurunathan S, Han JW, Dayem AA, Eppakayala V, Kim JH 2012 Oxidative stress-mediated antibacterial activity of graphene oxide and reduced graphene oxide in Pseudomonas aeruginosa. Int J Nanomedicine 7:5901. https://doi.org/10.2147/IJN.S37397
Nagy A, Harrison A, Sabbani S, Munson Jr RS, Dutta PK, Waldman WJ 2011 Silver nanoparticles embedded in zeolite membranes: release of silver ions and mechanism of antibacterial action. Int J Nanomedicine 6:1833. https://doi.org/10.2147/IJN.S24019
Leung YH, Ng AM, Xu X, Shen Z, Gethings LA, Wong MT, Leung FC 2014 Mechanisms of antibacterial activity of MgO: non-ROS mediated toxicity of MgO nanoparticles towards Escherichia coli. Small 10:1171–1183. https://doi.org/10.1002/smll.201302434
Jones N, Ray B, Ranjit KT, Manna AC 2008 Antibacterial activity of ZnO nanoparticle suspensions on a broad spectrum of microorganisms. FEMS Microbiol Lett 279:71–76. https://doi.org/10.1111/j.1574-6968.2007.01012.x
Karakoti AS, Hench LL, Seal S (2006) The potential toxicity of nanomaterials - The role of surfaces on NM toxicity. JOM 58:77–82. https://doi.org/10.1007/s11837-006-0147-0
Slavin YN, Asnis J, Häfeli UO, Bach H (2017) Metal nanoparticles: understanding the mechanisms behind antibacterial activity. J Nanobiotechnology 15:1–20. https://doi.org/10.1186/s12951-017-0308-z
El Badawy AM, Silva RG, Morris B, Scheckel KG, Suidan MT, Tolaymat TM (2011) Surface charge-dependent toxicity of silver nanoparticles. Environ Sci Technol 45:283–287. https://doi.org/10.1021/es1034188
Ivask A, ElBadawy A, Kaweeteerawat C, Boren D, Fischer H, Ji Z, Godwin HA (2014) Toxicity mechanisms in Escherichia coli vary for silver nanoparticles and differ from ionic silver. ACS nano 8:374–386. https://doi.org/10.1021/nn4044047
Mu H, Tang J, Liu Q, Sun C, Wang T, Duan J 2016 Potent antibacterial nanoparticles against biofilm and intracellular bacteria. Sci Rep 6:1–9. https://doi.org/10.1038/srep18877
Germovsek, E., Barker, C.I., Sharland, M. 2017. What do I need to know about aminoglycoside antibiotics? Arch. Dis. Child. Educ. Pract. Ed. 102, 89–93. https://doi.org/10.1136/archdischild-2015-309069
Yamamoto O, Ohira T, Alvarez K, Fukuda M (2010) Antibacterial characteristics of CaCO3-MgO composites. Materials Science and Engineering B: Solid-State. Adv Mater Technol 173:208–212. https://doi.org/10.1016/j.mseb.2009.12.007
Dhapte V, Kadam S, Pokharkar V, Khanna PK, Dhapte V (2014) Versatile SiO 2 Nanoparticles@Polymer Composites with Pragmatic Properties. ISRN inorg chem 1:1–8. https://doi.org/10.1155/2014/170919
Parham S, Wicaksono DH, Bagherbaigi S, Lee SL, Nur H (2016) Antimicrobial treatment of different metal oxide nanoparticles: a critical review. J Chin Chem Soc 63:385–393. https://doi.org/10.1002/jccs.201500446
Chichiriccò G, Poma A (2015) Penetration and toxicity of nanomaterials in higher plants 5:851–873. https://doi.org/10.3390/nano5020851
Zhou L, Yu K, Lu F, Lan G, Dai F, Shang S, Hu E (2020) Minimizing antibiotic dosage through in situ formation of gold nanoparticles across antibacterial wound dressings: a facile approach using silk fabric as the base substrate. J Clean Prod 243:1–10. https://doi.org/10.1016/j.jclepro.2019.118604
Wang Y, Wang F, Xu S, Wang R, Chen W (2018) Genetically engineered bi-functional silk material with improved cell proliferation and anti-inflammatory activity for medical application. Acta Biomaterialia 86:148–157. https://doi.org/10.1016/j.actbio.2018.12.036
Gu X, Xu Z, Gu L, Xu H, Han F, Chen B, Pan X (2021) Preparation and antibacterial properties of gold nanoparticles: a review. Environ Chem Lett 19:167–187. https://doi.org/10.1007/s10311-020-01071-0
Sondi I, Salopek-Sondi B (2004) Silver nanoparticles as antimicrobial agent: a case study on E. coli as a model for Gram-negative bacteria. J Colloid Interface Sci 275:177–182. https://doi.org/10.1016/j.jcis.2004.02.012
Prestinaci F, Pezzotti P, Pantosti A (2015) Antimicrobial resistance: a global multifaceted phenomenon. Pathog Glob Health 109:309–318. https://doi.org/10.1179/2047773215Y.0000000030
Theuretzbacher U, Outterson K, Engel A, Karlén A (2020) The global preclinical antibacterial pipeline. Nat Rev Microbiol 18:275–285. https://doi.org/10.1038/s41579-019-0288-0
Annunziato G (2019) Strategies to overcome antimicrobial resistance (AMR) making use of non-essential target inhibitors: a review. Int J Mol Sci 20:5844–5869. https://doi.org/10.3390/ijms20235844
Han C, Romero N, Fischer S, Dookran J, Berger A, Doiron AL (2017) Recent developments in the use of nanoparticles for treatment of biofilms. Nanotechnol Rev 6:383–404. https://doi.org/10.1515/ntrev-2016-0054
Kumar M, Sarma DK, Shubham S, Kumawat M, Verma V, Nina PB, Jp D, Kumar S, Singh B, Tiwari RR (2021) Futuristic Non-antibiotic Therapies to Combat Antibiotic Resistance: A Review. Front Microbiol 12:1–15. https://doi.org/10.3389/fmicb.2021.609459
Munita JM, Arias CA (2016) Mechanisms of antibiotic resistance. Microbiol Spectr 4:4–2. https://doi.org/10.1128/microbiolspec.vmbf-0016-2015
Baptista PV, McCusker MP, Carvalho A, Ferreira DA, Mohan NM, Martins M, Fernandes AR (2018) Nano-strategies to fight multidrug resistant bacteria—“A Battle of the Titans”. Front Microbiol 9:1441–1467. https://doi.org/10.3389/fmicb.2018.01441
Patra JK, Das G, Fraceto LF, Campos EVR, del Pilar Rodriguez-Torres M, Acosta-Torres LS, Diaz-Torres LA, Grillo R, Swamy MK. Sharma S, Habtemariam S (2018) Nano based drug delivery systems: recent developments and future prospects. J Nanobiotechnology 16:1–33. https://doi.org/10.1186/s12951-018-0392-8
Pal I, Bhattacharyya D, Kar RK, Zarena D, Bhunia A, Atreya HS (2019) A peptide-nanoparticle system with improved efficacy against multidrug resistant bacteria. Sci Rep 9:1–11. https://doi.org/10.1038/s41598-019-41005-7. Websites: https://www.drugs.com/ingredient/gentamicin.html. https://www.medindia.net/drug-price/gentamicin-combination.html.
Acknowledgements
Authors are grateful to DBT, Government of India for providing DBT BioCare Fellowship. The authors would like to express sincere gratitude to Technology Information, Forecasting and Assessment Council (TIFAC)-CORE, Government of India and Manipal Academy of Higher Education (MAHE), Manipal, India for infrastructure.
Funding
Authors are grateful to Department of Biotechnology (DBT), Government of India for providing DBT BioCare Fellowship. The authors would like to express sincere gratitude to Technology Information, Forecasting and Assessment Council (TIFAC)-CORE, Government of India and Manipal Academy of Higher Education (MAHE), Manipal, India for infrastructure.
Open access funding provided by Manipal Academy of Higher Education, Manipal
Author information
Authors and Affiliations
Contributions
Isuri Dinara Athauda: Writing - Original draft, Review and Editing, Manasa Gangadhar Shetty: Writing - Original draft, Review and Editing; Padmini Pai: Writing - Original draft, Review and Editing, Madhu Hegde: Writing - Review and Editing, Sangam Chandrasekhar Gurumurthy: Writing - Supervision, Review and Editing, Kampa Sundara Babitha: Conceptualization, Supervision, Writing - Review and Editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical Approval
Not Applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Athauda, I.D., Shetty, M.G., Pai, P. et al. Enhanced Bactericidal Effects and Drug Delivery with Gentamicin-Conjugated Nanoparticles. J Clust Sci 35, 371–390 (2024). https://doi.org/10.1007/s10876-023-02501-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10876-023-02501-z