Abstract
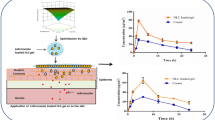
This study was designed to develop neem oil nanoemulsion of tea tree oil (TTO-NO-NE) using design of experiment based Box–Behnken design, which provided thermodynamic stable NE with globule size of 174 nm, and PDI 0.28, respectively. Whereas the zeta potential of optimized NE has occurred as − 20 mV with spherical and non-segregated in shape. Next, TTO-NO-NE-loaded nanogel and conventional gel were prepared, and initially, a comparative evaluation was performed for homogeneity, pH, spreadability, extrudability, and drug content. Furthermore, in vitro release pattern, ex vivo dermatokinetic profile, in vivo skin safety study, and stability of nanogel was determined. Comparative in vitro release study showed significantly sustained release of drug from nanogel (p < 0.005) when compared to the conventional gel. Simultaneously, a comparative ex vivo dermatokinetic study demonstrated significantly maximum drug deposition for nanogel (p < 0.05) than conventional gel. Moreover, in vivo skin safety study exhibited no signs of toxicity in terms of zero scoring for nanogel and was considered safe for future use. Finally, a stability study showed no significant (p > 0.05) variation in the pH, spreadability, extrudability, and drug content of optimized nanogel, which claims good stability for nanogel after 6 months of storage in prescribed environmental conditions. Thus, it can be concluded that the developed novel nanogel is a promising therapeutic asset that can mitigate dermal infections effectively.







Similar content being viewed by others
References
C. Flohr and R. Hay (2021). Putting the burden of skin diseases on the global map. Br. J. Dermatol. 184, 189–190. https://doi.org/10.1111/bjd.19704.
K. J. Pulsipher, M. D. Szeto, C. W. Rundle, C. L. Presley, M. R. Laughter, and R. P. Dellavalle (2021). Global burden of skin disease representation in the literature: bibliometric analysis. JMIR Dermatol. 4, e29282. https://doi.org/10.2196/29282.
A. R. Hilles, S. Mahmood, M. A. Kaderi, and R. Hashim (2019). Review of fungal skin infections and their invasion. Fungal Territ. 2, 3–5. https://doi.org/10.36547/ft.2019.2.2.3-5.
R. J. Hay, M. Augustin, C. E. M. Griffiths, and W. Sterry (2015). The global challenge for skin health. Br. J. Dermatol. 172, 1469–1472. https://doi.org/10.1111/bjd.13854.
NIAMS, Skin diseases, U.S. Department of Health & Human Services (2021). https://www.niams.nih.gov/health-topics/skin-diseases. Accessed 9 Jan 2021.
I. E. Cock and S. F. Van Vuuren (2020). A review of the traditional use of southern African medicinal plants for the treatment of fungal skin infections. J. Ethnopharmacol. 251, 112539. https://doi.org/10.1016/j.jep.2019.112539.
A. Garg, G. S. Sharma, A. K. Goyal, G. Ghosh, S. C. Si, and G. Rath (2020). Recent advances in topical carriers of anti-fungal agents. Heliyon 6, 1–12. https://doi.org/10.1016/j.heliyon.2020.e04663.
J. Roana, N. Mandras, D. Scalas, P. Campagna, and V. Tullio (2021). Antifungal activity of Melaleuca alternifolia essential oil (Tto) and its synergy with itraconazole or ketoconazole against Trichophyton rubrum. Molecules 26, 1–10. https://doi.org/10.3390/molecules26020461.
N. S. Lam, X. Long, X. Z. Su, and F. Lu (2020). Melaleuca alternifolia (tea tree) oil and its monoterpene constituents in treating protozoan and helminthic infections. Biomed. Pharmacother. 130, 110624. https://doi.org/10.1016/j.biopha.2020.110624.
M. Wróblewska, E. Szymańska, and K. Winnicka (2021). The influence of tea tree oil on antifungal activity and pharmaceutical characteristics of Pluronic® F-127 gel formulations with ketoconazole. Int. J. Mol. Sci. 22, 11326. https://doi.org/10.3390/ijms222111326.
P. Sudan, M. Goswami, and J. Singh (2020). Exploration of antifungal potential of Azadirachta indica against Microsporum gypseum. Biomed. Pharmacol. J. 13, 921–925. https://doi.org/10.13005/bpj/1960.
S. Uzzaman (2020). Pharmacological activities of neem (Azadirachta indica): a review. Int. J. Pharmacogn. Life Sci. 1, 38–41. https://doi.org/10.33545/27072827.2020.v1.i1a.8.
A. Eqbal, V. A. Ansari, A. Hafeez, F. Ahsan, M. Imran, and S. Tanweer (2021). Recent applications of nanoemulsion based drug delivery system: a review. Res J Pharm Technol. https://doi.org/10.52711/0974-360X.2021.00502.
S. Verma and P. Utreja (2019). Vesicular nanocarrier based treatment of skin fungal infections: potential and emerging trends in nanoscale pharmacotherapy. Asian J. Pharm. Sci. 14, 117–129. https://doi.org/10.1016/j.ajps.2018.05.007.
B. P. Manjula, V. G. Joshi, R. S. Setty, and M. Geetha (2021). Simultaneous estimation of tea tree oil and neem seed oil in bulk and cosmeceutical formulation by UV spectrophotometry. Int. J. Pharm. Sci. Res. 12, 3264–3271. https://doi.org/10.13040/IJPSR.0975-8232.12(6).3264-71.
K. Patel, S. Padhye, and M. Nagarsenker (2011). Duloxetine HCl lipid nanoparticles: preparation, characterization, and dosage form design. AAPS PharmSciTech. 13, 125–133. https://doi.org/10.1208/s12249-011-9727-6.
K. M. Hosny, A. M. Sindi, H. M. Alkhalidi, M. Kurakula, A. H. Hassan, R. B. Bakhaidar, W. A. Abualsunun, A. M. Almehmady, A. Khames, W. Y. Rizg, R. A. Khallaf, N. K. Alruwaili, and N. A. Alhakamy (2021). Development of omega-3 loxoprofen-loaded nanoemulsion to limit the side effect associated with NSAIDs in treatment of tooth pain. Drug Deliv. 28, 741–751. https://doi.org/10.1080/10717544.2021.1909179.
S. Kumar, J. Ali, and S. Baboota (2016). Design Expert® supported optimization and predictive analysis of selegiline nanoemulsion via the olfactory region with enhanced behavioural performance in Parkinson’s disease. Nanotechnology 27, 1–24. https://doi.org/10.1088/0957-4484/27/43/435101.
S. Md, N. A. Alhakamy, H. M. Aldawsari, M. Husain, S. Kotta, S. T. Abdullah, U. A. Fahmy, M. A. Alfaleh, and H. Z. Asfour (2020). Formulation design, statistical optimization, and in vitro evaluation of a naringenin nanoemulsion to enhance apoptotic activity in a549 lung cancer cells. Pharmaceuticals 13, 1–21. https://doi.org/10.3390/ph13070152.
M. U. Ashhar, S. Kumar, J. Ali, and S. Baboota (2021). CCRD based development of bromocriptine and glutathione nanoemulsion tailored ultrasonically for the combined anti-Parkinson effect. Chem. Phys. Lipids 235, 1–14. https://doi.org/10.1016/j.chemphyslip.2020.105035.
M. K. Iqubal, A. Iqubal, K. Imtiyaz, M. M. A. Rizvi, M. M. Gupta, J. Ali, and S. Baboota (2021). Combinatorial lipid-nanosystem for dermal delivery of 5-fluorouracil and resveratrol against skin cancer: delineation of improved dermatokinetics and epidermal drug deposition enhancement analysis. Eur. J. Pharm. Biopharm. 163, 223–239. https://doi.org/10.1016/j.ejpb.2021.04.007.
S. Kotta, A. W. Khan, S. H. Ansari, R. K. Sharma, and J. Ali (2015). Formulation of nanoemulsion: a comparison between phase inversion composition method and high-pressure homogenization method. Drug Deliv. 22, 455–466. https://doi.org/10.3109/10717544.2013.866992.
V. Bali, M. Ali, and J. Ali (2010). Study of surfactant combinations and development of a novel nanoemulsion for minimising variations in bioavailability of ezetimibe. Colloids Surf. B 76, 410–420. https://doi.org/10.1016/j.colsurfb.2009.11.021.
A. S. Rabelo, F. K. Sutili, J. O. Meneses, P. Severino, E. B. Souto, R. Y. Fujimoto, and J. C. Cardoso (2021). 23 Central composite rotatable design for the production of neem oil nanoemulsion for antifungal and antiparasitic applications. J. Chem. Technol. Biotechnol. 96, 2159–2167. https://doi.org/10.1002/jctb.6623.
J. Shah, A. B. Nair, S. Jacob, R. K. Patel, H. Shah, T. M. Shehata, and M. A. Morsy (2019). Nanoemulsion based vehicle for effective ocular delivery of moxifloxacin using experimental design and pharmacokinetic study in rabbits. Pharmaceutics 11, 230. https://doi.org/10.3390/pharmaceutics11050230.
M. S. Alam, M. S. Algahtani, J. Ahmad, K. Kohli, S. Shafiq-Un-Nabi, M. H. Warsi, and M. Z. Ahmad (2020). Formulation design and evaluation of aceclofenac nanogel for topical application. Ther. Deliv. 11, 767–778. https://doi.org/10.4155/tde-2020-0076.
R. Aiyalu, A. Govindarjan, and A. Ramasamy (2016). Formulation and evaluation of topical herbal gel for the treatment of arthritis in animal model, Brazilian. J. Pharm. Sci. 52, 493–507. https://doi.org/10.1590/s1984-82502016000300015.
M. K. Iqubal, A. Iqubal, H. Anjum, M. M. Gupta, J. Ali, and S. Baboota (2021). Determination of in vivo virtue of dermal targeted combinatorial lipid nanocolloidal based formulation of 5-fluorouracil and resveratrol against skin cancer. Int. J. Pharm. 610, 121179. https://doi.org/10.1016/j.ijpharm.2021.121179.
A. Qadir, M. Aqil, A. Ali, M. H. Warsi, M. Mujeeb, F. J. Ahmad, S. Ahmad, and S. Beg (2020). Nanostructured lipidic carriers for dual drug delivery in the management of psoriasis: systematic optimization, dermatokinetic and preclinical evaluation. J. Drug Deliv. Sci. Technol. 57, 101775. https://doi.org/10.1016/j.jddst.2020.101775.
R. Gupta and G. Das Gupta (2017). Formulation development and evaluation of anti-inflammatory potential of cordia obliqua topical gel on animal model. Pharmacogn. J. 9, s93–s98. https://doi.org/10.5530/pj.2017.6s.163.
V. Thakur, B. Prashar, and S. Arora (2012). Formulation and in vitro evaluation of gel for topical delivery of antifungal agent fluconazole using different penetration enhancers. Drug Invent. Today 4, 414–419.
T. Moolakkadath, M. Aqil, A. Ahad, S. S. Imam, A. Praveen, Y. Sultana, M. Mujeeb, and Z. Iqbal (2019). Fisetin loaded binary ethosomes for management of skin cancer by dermal application on UV exposed mice. Int. J. Pharm. 560, 78–91. https://doi.org/10.1016/j.ijpharm.2019.01.067.
S. Uprit, R. Kumar Sahu, A. Roy, and A. Pare (2013). Preparation and characterization of minoxidil loaded nanostructured lipid carrier gel for effective treatment of alopecia. Saudi Pharm. J. 21, 379–385. https://doi.org/10.1016/j.jsps.2012.11.005.
R. Hamed, A. Farhan, R. Abu-Huwaij, N. N. Mahmoud, and A. Kamal (2020). Lidocaine microemulsion-laden organogels as lipid-based systems for topical delivery. J. Pharm. Innov. 15, 521–534. https://doi.org/10.1007/s12247-019-09399-z.
P. Negi, B. Singh, G. Sharma, S. Beg, and O. P. Katare (2015). Biocompatible lidocaine and prilocaine loaded-nanoemulsion system for enhanced percutaneous absorption: QbD-based optimisation, dermatokinetics and in vivo evaluation. J. Microencapsul. 32, 419–431. https://doi.org/10.3109/02652048.2015.1046513.
K. Raza, B. Singh, S. Lohan, G. Sharma, P. Negi, Y. Yachha, and O. P. Katare (2013). Nano-lipoidal carriers of tretinoin with enhanced percutaneous absorption, photostability, biocompatibility and anti-psoriatic activity. Int. J. Pharm. 456, 65–72. https://doi.org/10.1016/j.ijpharm.2013.08.019.
D. K. Gupta, M. Aqil, A. Ahad, S. S. Imam, A. Waheed, A. Qadir, M. K. Iqubal, and Y. Sultana (2020). Tailoring of berberine loaded transniosomes for the management of skin cancer in mice. J. Drug Deliv. Sci. Technol. 60, 102051. https://doi.org/10.1016/j.jddst.2020.102051.
Ç. Tas, Y. Özkan, A. Savaser, and T. Baykara (2003). In vitro release studies of chlorpheniramine maleate from gels prepared by different cellulose derivatives. Il Farmaco 58, 605–611. https://doi.org/10.1016/S0014-827X(03)00080-6.
F. I. Abd-Allah, H. M. Dawaba, and A. M. Ahmed (2010). Preparation, characterization, and stability studies of piroxicam-loaded microemulsions in topical formulations. Drug Discov. Ther. 4, 267–275.
T. Z. da Silva Marques, R. Santos-Oliveira, L. B. de Oliveira de Siqueira, V. da Silva Cardoso, Z. M. F. de Freitas, R. de Cássiada S. A. Barros, A. L. V. Villa, M. S. de Satode B. Monteiro, E. P. Dos Santos, and E. Ricci-Junior (2018). Development and characterization of a nanoemulsion containing propranolol for topical delivery. Int. J. Nanomed. 13, 2827–2837. https://doi.org/10.2147/IJN.S164404.
L. M. Negi, M. Jaggi, and S. Talegaonkar (2014). Development of protocol for screening the formulation components and the assessment of common quality problems of nano-structured lipid carriers. Int. J. Pharm. 461, 403–410. https://doi.org/10.1016/j.ijpharm.2013.12.006.
T. Muta, A. Parikh, K. Kathawala, H. Haidari, Y. Song, J. Thomas, and S. Garg (2020). Quality-by-design approach for the development of nano-sized tea tree oil formulation-impregnated biocompatible gel with antimicrobial properties. Pharmaceutics 12, 1–16. https://doi.org/10.3390/pharmaceutics12111091.
Acknowledgements
This project was funded by the Deanship of Scientific Research (DSR) at King Abdulaziz University, Jeddah, under Grant No. (G: 104-140-1442). The authors, therefore, acknowledge with thanks to DSR for technical and financial support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research Involving Human Participants
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asfour, H.Z., Alhakamy, N.A., Alam, M.S. et al. Design of Experiment Navigated Methodical Development of Neem Oil Nanoemulsion Containing Tea Tree Oil for Dual Effect Against Dermal Illness: Ex Vivo Dermatokinetic and In Vivo. J Clust Sci 34, 1311–1323 (2023). https://doi.org/10.1007/s10876-022-02301-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10876-022-02301-x