Abstract
Purpose
Anti-interferon (IFN)-γ autoantibodies (anti-IFN-γ Abs) is an emerging adult-onset immunodeficiency syndrome. Immune dysfunction in this distinct disorder remains to be clarified.
Methods
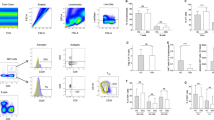
We prospectively collected blood samples of 20 patients with anti-IFN-γ Abs and 40 healthy normal subjects. The percentages of lymphocyte subpopulations, most relevant to T, B, and NK cells, and the percentages of stimulated lymphocytes with cytokine production were assessed using eight-color flow cytometry. The results were adjusted to age and absolute lymphocyte counts.
Results
Most (85%) patients presented nontuberculous mycobacterial infection. Skin lesions were predominantly manifested by neutrophilic dermatoses. The involved lymph nodes had granulomatous inflammation, except 22.2% showing atypical lymphoid hyperplasia without granuloma formation. The percentages of CD4 + T cells and nonactivated subpopulations (recent thymic emigrants and naïve subtypes) decreased significantly with increased expression of activation markers and polarization to differentiated cells. The percentage of NK cells increased, but that of two major NK subpopulations, CD161 + CD56bright and CD161 + CD56 + CD16 + subsets, decreased. Increased CD161dim, CD161 + CD56 − CD16 + , and CD57 + NK cell subsets coupled with the decreased expression of NKp30 and NKp46 indicate reconfiguration of the NK cell population and acquisition of adaptive features. Intracellular cytokine production of the lymphocyte subpopulations was significantly low in the patients compared with the control group.
Conclusion
We conclude that the immune system in patients with anti-IFN-γ Abs could be exhausted in T cells and be adaptive in NK cells, contributing to the distinct clinicopathologic features.



Similar content being viewed by others
Data Availability
Upon request.
Code Availability
Upon request.
References
Batoni G, Esin S, Favilli F, Pardini M, Bottai D, Maisetta G, et al. Human CD56bright and CD56dim natural killer cell subsets respond differentially to direct stimulation with Mycobacterium bovis bacillus Calmette-Guerin. Scand J Immunol. 2005;62(6):498–506.
Boldt A, Borte S, Fricke S, Kentouche K, Emmrich F, Borte M, et al. Eight-color immunophenotyping of T-, B-, and NK-cell subpopulations for characterization of chronic immunodeficiencies. Cytometry B Clin Cytom. 2014;86(3):191–206.
Browne SK, Burbelo PD, Chetchotisakd P, Suputtamongkol Y, Kiertiburanakul S, Shaw PA, et al. Adult-onset immunodeficiency in Thailand and Taiwan. N Engl J Med. 2012;367(8):725–34.
Chawansuntati K, Rattanathammethee K, Wipasa J. Minireview: Insights into anti-interferon-gamma autoantibodies. Exp Biol Med (Maywood). 2021;246(7):790–5.
Chi CY, Chu CC, Liu JP, Lin CH, Ho MW, Lo WJ, Lin PC, Chen HJ, Chou CH, Feng JY, et al. Anti-IFN-gamma autoantibodies in adults with disseminated nontuberculous mycobacterial infections are associated with HLA-DRB1*16:02 and HLA-DQB1*05:02 and the reactivation of latent varicella-zoster virus infection. Blood. 2013;121(8):1357–66.
Chi CY, Lin CH, Ho MW, Ding JY, Huang WC, Shih HP, et al. Clinical manifestations, course, and outcome of patients with neutralizing anti-interferon-gamma autoantibodies and disseminated nontuberculous mycobacterial infections. Med (Baltim). 2016;95(25):e3927
Chruewkamlow N, Mahasongkram K, Pata S, Chaiwarith R, Salee P, Supparatpinyo K, et al. Immune alterations in patients with anti-interferon-gamma autoantibodies. PLOS ONE. 2016;11(1):e0145983
Duah M, Li L, Shen J, Lan Q, Pan B, Xu K. Thymus degeneration and regeneration. Front Immunol. 2021;12:706244
Fink PJ. The biology of recent thymic emigrants. Annu Rev Immunol. 2013;31:31–50.
Forconi CS, Oduor CI, Oluoch PO, Ong’echa JM, Munz C, Bailey JA, et al. A new hope for CD56(neg)CD16(pos) NK cells as unconventional cytotoxic mediators: an adaptation to chronic diseases. Front Cell Infect Microbiol. 2020;10:162.
Gonzalez SM, Taborda NA, Rugeles MT. Role of different subpopulations of CD8+ T cells during HIV exposure and infection. Front Immunol. 2017;8:936.
Guo J, Ning XQ, Ding JY, Zheng YQ, Shi NN, Wu FY, Lin YK, Shih HP, Ting HT, Liang G et al. Anti-IFN-gamma autoantibodies underlie disseminated Talaromyces marneffei infections. J Exp Med. 2020; 217(12)
Hong GH, Ortega-Villa AM, Hunsberger S, Chetchotisakd P, Anunnatsiri S, Mootsikapun P, et al. Natural history and evolution of anti-interferon-gamma autoantibody-associated immunodeficiency syndrome in Thailand and the United States. Clin Infect Dis. 2020;71(1):53–62.
Jutivorakool K, Sittiwattanawong P, Kantikosum K, Hurst CP, Kumtornrut C, Asawanonda P, et al. Skin manifestations in patients with adult-onset immunodeficiency due to anti-interferon-gamma autoantibody: a relationship with systemic infections. Acta Derm Venereol. 2018;98(8):742–7.
Kared H, Martelli S, Ng TP, Pender SL, Larbi A. CD57 in human natural killer cells and T-lymphocytes. Cancer Immunol Immunother. 2016;65(4):441–52.
Koizumi Y, Mikamo H. Anti-Interferon-gamma autoantibody and disseminated nontuberculous mycobacteria infection. What should be done to improve its clinical outcome? Clin Infect Dis. 2021;72(12):2209–11
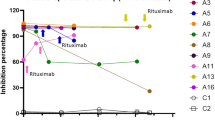
Krisnawati DI, Liu YC, Lee YJ, Wang YT, Chen CL, Tseng PC, et al. Functional neutralization of anti-IFN-gamma autoantibody in patients with nontuberculous mycobacteria infection. Sci Rep. 2019;9(1):5682.
Ku CL, Chi CY, von Bernuth H, Doffinger R. Autoantibodies against cytokines: phenocopies of primary immunodeficiencies? Hum Genet. 2020;139(6–7):783–94.
Kurioka A, Cosgrove C, Simoni Y, van Wilgenburg B, Geremia A, Bjorkander S, et al. CD161 defines a functionally distinct subset of pro-inflammatory natural killer cells. Front Immunol. 2018;9:486.
Lim A, Allison C, Tan DB, Oliver B, Price P, Waterer G. Immunological markers of lung disease due to non-tuberculous mycobacteria. Dis Markers. 2010;29(2):103–9.
Li WS, Huang WC, Ku CL, Lee CH. Osteolytic lesions resulting from opportunistic infections. Kaohsiung J Med Sci. 2017;33(7):365–6.
Liu TT, Weng SW, Wang MC, Huang WT. Nontuberculous mycobacterial infection with concurrent IgG4-related lymphadenopathy. APMIS. 2016;124(3):216–20.
Long EO, Kim HS, Liu D, Peterson ME, Rajagopalan S. Controlling natural killer cell responses: integration of signals for activation and inhibition. Annu Rev Immunol. 2013;31:227–58.
Lopez-Vergès S, Milush JM, Pandey S, York VA, Arakawa-Hoyt J, Pircher H, et al. CD57 defines a functionally distinct population of mature NK cells in the human CD56dimCD16+ NK-cell subset. Blood. 2010;116(19):3865–74.
Mavilio D, Lombardo G, Benjamin J, Kim D, Follman D, Marcenaro E, et al. Characterization of CD56−/CD16+ natural killer (NK) cells: a highly dysfunctional NK subset expanded in HIV-infected viremic individuals. Proc Natl Acad Sci U S A. 2005;102(8):2886–91.
Michel T, Poli A, Cuapio A, Briquemont B, Iserentant G, Ollert M, et al. Human CD56bright NK cells: an update. J Immunol. 2016;196(7):2923–31.
Moore JW, Beattie L, Osman M, Owens BM, Brown N, Dalton JE, et al. CD4+ recent thymic emigrants are recruited into granulomas during Leishmania donovani infection but have limited capacity for cytokine production. PLOS ONE. 2016;11(9):e0163604
Nielsen CM, White MJ, Goodier MR, Riley EM. Functional significance of CD57 expression on human NK cells and relevance to disease. Front Immunol. 2013;4:422.
Pithukpakorn M, Roothumnong E, Angkasekwinai N, Suktitipat B, Assawamakin A, Luangwedchakarn V, Umrod P, Thongnoppakhun W, Foongladda S, Suputtamongkol Y. HLA-DRB1 and HLA-DQB1 are associated with adult-onset immunodeficiency with acquired anti-interferon-gamma autoantibodies. PLOS ONE. 2015; 10(5):e0128481
Shih HP, Ding JY, Yeh CF, Chi CY, Ku CL. Anti-interferon-gamma autoantibody-associated immunodeficiency. Curr Opin Immunol. 2021;72:206–14.
Wang Z, Zhu L, Nguyen THO, Wan Y, Sant S, Quiñones-Parra SM, et al. Clonally diverse CD38+HLA-DR+CD8+ T cells persist during fatal H7N9 disease. Nat Commun. 2018;9(1):824.
Wipasa J, Wongkulab P, Chawansuntati K, Chaiwarit R, Supparatpinyo K. Cellular immune responses in HIV-negative immunodeficiency with anti-interferon-gamma antibodies and opportunistic intracellular microorganisms. PLOS ONE. 2014;9(10):e110276
Wu UI, Holland SM. Host susceptibility to non-tuberculous mycobacterial infections. Lancet Infect Dis. 2015;15(8):968–80.
Wu UI, Wang JT, Sheng WH, Sun HY, Cheng A, Hsu LY, et al. Incorrect diagnoses in patients with neutralizing anti-interferon-gamma-autoantibodies. Clin Microbiol Infect. 2020;26(12):1684.e1-6.
Acknowledgements
We acknowledge Mr. Yu-Shiang Hu (senior product specialist, BD Biosciences, Taiwan) for his help with the experimental setting and Biostatistics Center, Kaohsiung Chang Gung Memorial Hospital for statistics work.
Funding
This study was supported by the Chang Gung Memorial Hospital (grant number CMRPG8K0341).
Author information
Authors and Affiliations
Contributions
WTH conceptualized and designed the study. CLK and JYD designed and performed the experiments to detect neutralizing anti-IFN-γ antibodies. WCH and HLY acquired the data. YCC, CHL, and WTH interpreted the data. YCC and WTH conducted the literature review and wrote the draft manuscript. SWW performed the statistical analysis. All authors critically reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
This study was approved by the Ethics Committee of the Chang Gung Memorial Hospital, Kaohsiung, Taiwan, in accordance with the Declaration of Helsinki (IRB201901509B0C501).
Consent to Participate
All participants provided written informed consent.
Consent for Publication
Obtained.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, YC., Weng, SW., Ding, JY. et al. Clinicopathological Manifestations and Immune Phenotypes in Adult-Onset Immunodeficiency with Anti-interferon-γ Autoantibodies. J Clin Immunol 42, 672–683 (2022). https://doi.org/10.1007/s10875-022-01210-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-022-01210-y