Abstract
There is a lack of studies reporting on rhBMP-2 application in pediatric orthopaedics, although few reports demonstrated promising results of the use of rhBMP-2 in children, especially for spine fusion and for the treatment of congenital pseudarthrosis of the tibia. The objectives of this study were (1) to examine clinical and radiographic healing after rhBMP-2 application for the treatment of congenital pseudarthrosis of the tibia (CPT) or persistent tibial nonunion in children and adolescents, and (2) to investigate the safety of rhBMP-2 use in these cases. Therefore we reviewed the medical records of ten patients with a mean age of 8.6 years (2.3–21) with CPT (n = 7) or persistent tibial nonunion for at least six months (n = 3) who had been treated with rhBMP-2. Nine of ten patients had union at final follow-up, after a mean of 72.9 months (25–127). In the CPT group, primary healing of the pseudarthrosis occurred in six of seven patients at a mean of 5.2 months (3–12). Repeat rhBMP-2 application was performed in three patients; two patients had one additional application each, and one patient had three additional applications. Complications that may be attributed to the use of rhBMP-2 were seen in two of fifteen applications, including a compartmemt syndrome and a hematoma. In this retrospective case series rhBMP-2 has been used successfully to treat CPT or persistent tibial nonunion in pediatric patients. However, prospective randomized controlled trials are warranted to investigate the long-term efficacy and safety of rhBMP-2 use in these cases.
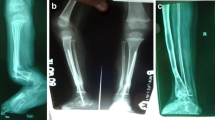
Graphical Abstract


Similar content being viewed by others
References
Dohin B, Dahan-Oliel N, Fassier F, Hamdy R. Enhancement of difficult non-union in children with osteogenic protein-1 (OP-1): early experience. Clin Orthop Relat Res. 1965;467(12):3230–38.
Urist M. Bone: formation by autoinduction. Science. 1965;150:893–9.
Dohin B, Kohler R. Masquelet’s procedure and bone morphogenetic protein in congenital pseudarthrosis of the tibia in children: a case series and meta-analysis. J Child Orthop. 2012;6(4):297–306.
Spiro AS, Beil FT, Baranowsky A, Barvencik F, Schilling AF, Nguyen K, et al. BMP-7-induced ectopic bone formation and fracture healing is impaired by systemic NSAID application in C57BL/6-mice. J Orthop Res. 2010;28(6):785–91.
Spiro AS, Beil FT, Timo Beil F, Schinke T, Schilling AF, Eulenburg C, et al. Short-term application of dexamethasone enhances bone morphogenetic protein-7-induced ectopic bone formation in vivo. J Trauma. 2010;69(6):1473–80.
Spiro AS, Babin K, Lipovac S, Stenger P, Mladenov K, Rupprecht M, et al. Combined treatment of congenital pseudarthrosis of the tibia, including recombinant human bone morphogenetic protein-2: a case series. J Bone Joint Surg Br. 2011;93(5):695–9.
Grill F, Bollini G, Dungl P, et al. Treatment approaches for congenital pseudarthrosis of tibia: results of the EPOS multicenter study. European paediatric orthopaedic society (EPOS). J Pediatr Orthop B. 2000;9:75–89.
Sampath TK, Maliakal JC, Hauschka PV, et al. Recombinant human osteogenic protein-1 (hOP-1) induces new bone formation in vivo with a specific activity comparable with natural bovine osteogenic protein and stimulates osteoblast proliferation and differentiation in vitro. J Biol Chem. 1992;267:20352–62.
Salkeld SL, Patron LP, Barrack RL, et al. The effect of osteogenic protein-1 on the healing of segmental bone defects treated with autograft or allograft bone. J Bone Joint Surg Am. 2001;83:803–16.
Kloen P, Di Paola M, Borens O, et al. BMP signaling components are expressed in human fracture callus. Bone. 2003;33:362–71.
Govender S, Csimma C, Genant HK, Valentin-Opran A, Amit Y, Arbel R, et al. Recombinant human bone morphogenetic protein-2 for treatment of open tibial fractures: a prospective, controlled, randomized study of four hundred and fifty patients. J Bone Joint Surg Am. 2002;84-A(12):2123–34.
Friedlaender GE, Perry CR, Cole JD, et al. Osteogenic protein-1 (bone morphogenetic protein-7) in the treatment of tibial nonunions. J Bone Joint Surg Am. 2001;83:151–8.
Courvoisier A, Sailhan F, Laffenêtre O, Obert L. French Study Group of BMP in Orthopedic Surgery. Bone morphogenetic protein and orthopaedic surgery: can we legitimate its off-label use? Int Orthop. 2014; 38(12):2601–05.
Das SP, Ganesh S, Pradhan S, Singh D, Mohanty RN. Effectiveness of recombinant human bone morphogenetic protein-7 in the management of congenital pseudoarthrosis of the tibia: a randomised controlled trial. Int Orthop. 2014;38(9):1987–92.
Nicolaou N, Ghassemi A, Hill RA. Congenital pseudarthrosis of the tibia: the results of an evolving protocol of management. J Child Orthop. 2013;7(4):269–76.
Shabtai L, Ezra E, Wientroub S, Segev E. Congenital tibial pseudarthrosis, changes in treatment protocol. J Pediatr Orthop B. 2015;24(5):444–9.
Fabeck L, Ghafil D, Gerroudj M, et al. Bone morphogenetic protein 7 in the treatment of congenital pseudarthrosis of the tibia. J Bone Joint Surg Br. 2006;88:116–8.
Anticevic D, Jelic M, Vukicevic S. Treatment of a congenital pseudarthrosis of the tibia by osteogenic protein-1 (bone morphogenetic protein-7): a case report. J Pediatr Orthop B. 2006;15:220–21.
Lee FY, Sinicropi SM, Lee FS, et al. Treatment of congenital pseudarthrosis of the tibia with recombinant human bone morphogenetic protein-7 (rhBMP-7). A report of five cases. J Bone Joint Surg Am. 2006;88:627–33.
Kujala S, Vähäsarja V, Serlo W, et al. Treatment of congenital pseudarthrosis of the tibia with native bovine BMP: a case report. Acta Orthop Belg. 2008;74:132–6.
Richards BS, Oetgen ME, Johnston CE. The use of rhBMP-2 for the treatment of congenital pseudarthrosis of the tibia: a case series. J Bone Joint Surg Am. 2010;92:177–85.
Burkhart KJ, Rommens PM. Intramedullary application of bone morphogenetic protein in the management of a major bone defect after an Ilizarov procedure. J Bone Joint Surg Br. 2008;90(6):806–9.
Traub JA, O’Connor W, Masso PD. Congenital pseudarthrosis of the tibia: a retrospective review. J Pediatr Orthop. 1999;19:735–8.
Guidera KJ, Raney EM, Ganey T, et al. Ilizarov treatment of congenital pseudarthroses of the tibia. J Pediatr Orthop. 1997;17:668–74.
Dobbs MB, Rich MM, Gordon JE, et al. Use of an intramedullary rod for treatment of congenital pseudarthrosis of the tibia. A long-term follow-up study. J Bone Joint Surg Am. 2004;86:1186–97.
Crawford AH. Neurofibromatosis in the pediatric patient. Orthop Clin N Am. 1978;9:11–23.
Oetgen ME, Richards BS. Complications associated with the use of bone morphogenetic protein in pediatric patients. J Pediatr Orthop. 2010;30(2):192–8.
Cho TJ, Choi IH, Lee SM, et al. Refracture after Ilizarov osteosynthesis in atrophic-type congenital pseudarthrosis of the tibia. J Bone Joint Surg Br. 2008;90:488–93.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Tim N. Hissnauer and Norbert Stiel have contributed equally to this work and therefore share first authorship.
Rights and permissions
About this article
Cite this article
Hissnauer, T.N., Stiel, N., Babin, K. et al. Bone morphogenetic protein-2 for the treatment of congenital pseudarthrosis of the tibia or persistent tibial nonunion in children and adolescents: A retrospective study with a minimum 2-year follow-up. J Mater Sci: Mater Med 28, 60 (2017). https://doi.org/10.1007/s10856-017-5868-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-017-5868-9