Abstract
Background
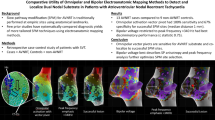
Pulsed field ablation (PFA) is a new, non-thermal technology in the treatment of atrial fibrillation (AF). Early investigations have shown a promising safety profile with durable pulmonary vein isolation (PVI) and large antral lesions. However, clinical data remains scarce.
Methods
We investigated a cohort of 43 patients. Twenty-three patients underwent PVI with PFA in our hospital and we analyzed them with regard to procedural characteristics and with regard to the size of acute antral lesion which was estimated by using an electroanatomical map of the left atrium (LA). We compared these data with data of 20 patients who had undergone cryoballon (CB) PVI in our hospital.
Results
We could show acute isolation of all veins in all patients (100% PFA, 100% CB). Post-ablation high-density mapping revealed no early reconnection (0%). The acute antral lesion size of PFA was significantly higher compared to the CB (67.03 ± 12.69% vs. 57.39 ± 10.91%, p = 0.01). In the PFA group, we found no acute phrenic nerve injury, no major or minor bleeding, and no tamponade but one (4.34%) patient suffered from a stroke. Transient hypotension was observed frequently as well as transient bradycardia or asystole episodes requiring right ventricular pacing. In the CB group, no complications occurred. Furthermore, we discuss practical issues on PFA procedures.
Conclusions
PFA is a promising technology with high acute PV isolation rate and large antral lesions compared to CB. However, larger trials with more patients and data on long-term freedom of AF but also complications are needed.






Similar content being viewed by others
References
Iwasaki YK, Nishida K, Kato T, Nattel S. Atrial fibrillation pathophysiology: implications for management. Circulation. 2011;124:2264–74. https://doi.org/10.1161/CIRCULATIONAHA.111.019893.
Kim MH, Johnston SS, Chu BC, Dalal MR, Schulman KL. Estimation of total incremental health care costs in patients with atrial fibrillation in the United States. Circ Cardiovasc Qual Outcomes. 2011;4:313–20. https://doi.org/10.1161/CIRCOUTCOMES.110.958165.
Hindricks G, Potpara T, Dagres N, Arbelo E, Bax JJ, Blomstrom-Lundqvist C, Boriani G, Castella M, Dan GA, Dilaveris PE et al, 2020 ESC guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association of Cardio-Thoracic Surgery (EACTS). Eur Heart J 2020https://doi.org/10.1093/eurheartj/ehaa612
Verma A, Boersma L, Haines DE, Natale A, Marchlinski FE, Sanders P, Calkins H, Packer DL, Hummel J, Onal B, et al. First-in-human experience and acute procedural outcomes using a novel pulsed field ablation system: the PULSED AF pilot trial. Circ Arrhythm Electrophysiol. 2022;15:e010168. https://doi.org/10.1161/CIRCEP.121.010168.
Reddy VY, Neuzil P, Koruth JS, Petru J, Funosako M, Cochet H, Sediva L, Chovanec M, Dukkipati SR, Jais P. Pulsed field ablation for pulmonary vein isolation in atrial fibrillation. J Am Coll Cardiol. 2019;74:315–26. https://doi.org/10.1016/j.jacc.2019.04.021.
Reddy VY, Dukkipati SR, Neuzil P, Anic A, Petru J, Funasako M, Cochet H, Minami K, Breskovic T, Sikiric I, et al. Pulsed field ablation of paroxysmal atrial fibrillation: 1-year outcomes of IMPULSE, PEFCAT, and PEFCAT II. JACC Clin Electrophysiol. 2021;7:614–27. https://doi.org/10.1016/j.jacep.2021.02.014.
Cochet H, Nakatani Y, Sridi-Cheniti S, Cheniti G, Ramirez FD, Nakashima T, Eggert C, Schneider C, Viswanathan R, Derval N, et al. Pulsed field ablation selectively spares the oesophagus during pulmonary vein isolation for atrial fibrillation. Europace. 2021;23:1391–9. https://doi.org/10.1093/europace/euab090.
Howard B, Haines DE, Verma A, Packer D, Kirchhof N, Barka N, Onal B, Fraasch S, Miklavcic D, Stewart MT. Reduction in pulmonary vein stenosis and collateral damage with pulsed field ablation compared with radiofrequency ablation in a canine model. Circ Arrhythm Electrophysiol. 2020;13:e008337. https://doi.org/10.1161/CIRCEP.120.008337.
Kawamura I, Neuzil P, Shivamurthy P, Petru J, Funasako M, Minami K, Kuroki K, Dukkipati SR, Koruth JS, Reddy VY. Does pulsed field ablation regress over time? A quantitative temporal analysis of pulmonary vein isolation. Heart Rhythm. 2021;18:878–84. https://doi.org/10.1016/j.hrthm.2021.02.020.
Proietti R, Santangeli P, Di Biase L, Joza J, Bernier ML, Wang Y, Sagone A, Viecca M, Essebag V, Natale A. Comparative effectiveness of wide antral versus ostial pulmonary vein isolation: a systematic review and meta-analysis. Circ Arrhythm Electrophysiol. 2014;7:39–45. https://doi.org/10.1161/CIRCEP.113.000922.
Kenigsberg DN, Martin N, Lim HW, Kowalski M, Ellenbogen KA. Quantification of the cryoablation zone demarcated by pre- and postprocedural electroanatomic mapping in patients with atrial fibrillation using the 28-mm second-generation cryoballoon. Heart Rhythm. 2015;12:283–90. https://doi.org/10.1016/j.hrthm.2014.11.012.
Perrotta L, Konstantinou A, Bordignon S, Fuernkranz A, Dugo D, Chun KJ, Schmidt B. What is the acute antral lesion size after pulmonary vein isolation using different balloon ablation technologies? Circ J. 2017;81:172–9. https://doi.org/10.1253/circj.CJ-16-0345.
Wakamatsu Y, Nakahara S, Nagashima K, Fukuda R, Nishiyama N, Watanabe R, Arai M, Otsuka N, Kurokawa S, Sato H, et al. Hot balloon versus cryoballoon ablation for persistent atrial fibrillation: lesion area, efficacy, and safety. J Cardiovasc Electrophysiol. 2020;31:2310–8. https://doi.org/10.1111/jce.14646.
Gunawardene MA, Schaeffer BN, Jularic M, Eickholt C, Maurer T, Akbulak RO, Flindt M, Anwar O, Pape UF, Maasberg S, et al. Pulsed-field ablation combined with ultrahigh-density mapping in patients undergoing catheter ablation for atrial fibrillation: practical and electrophysiological considerations. J Cardiovasc Electrophysiol. 2022;33:345–56. https://doi.org/10.1111/jce.15349.
Blockhaus C, Waibler HP, Gulker JE, Klues H, Bufe A, Shin DI. Evasion maneuver for transseptal approach during cryoballoon pulmonary vein isolation. J Saudi Heart Assoc. 2018;30:301–4. https://doi.org/10.1016/j.jsha.2018.05.002.
Alkhouli M, Rihal CS, Holmes DR Jr. Transseptal techniques for emerging structural heart interventions. JACC Cardiovasc Interv. 2016;9:2465–80. https://doi.org/10.1016/j.jcin.2016.10.035.
Chen S, Schmidt B, Bordignon S, Bologna F, Perrotta L, Nagase T, Chun KRJ. Atrial fibrillation ablation using cryoballoon technology: recent advances and practical techniques. J Cardiovasc Electrophysiol. 2018;29:932–43. https://doi.org/10.1111/jce.13607.
Arentz T, Weber R, Burkle G, Herrera C, Blum T, Stockinger J, Minners J, Neumann FJ, Kalusche D. Small or large isolation areas around the pulmonary veins for the treatment of atrial fibrillation? Results from a prospective randomized study. Circulation. 2007;115:3057–63. https://doi.org/10.1161/CIRCULATIONAHA.107.690578.
Neven K, van Es R, van Driel V, van Wessel H, Fidder H, Vink A, Doevendans P, Wittkampf F, Acute and long-term effects of full-power electroporation ablation directly on the porcine esophagus. Circ Arrhythm Electrophysiol 2017; 10, https://doi.org/10.1161/CIRCEP.116.004672.
Magni FT, Mulder BA, Rienstra M, Klinkenberg TJ, Mariani MA, Blaauw Y. Pulsed field (endocardial) ablation as part of convergent hybrid ablation for the treatment of long-standing persistent atrial fibrillation. J Interv Card Electrophysiol. 2022. https://doi.org/10.1007/s10840-022-01183-3.
van Driel VJ, Neven KG, van Wessel H, du Pre BC, Vink A, Doevendans PA, Wittkampf FH. Pulmonary vein stenosis after catheter ablation: electroporation versus radiofrequency. Circ Arrhythm Electrophysiol. 2014;7:734–8. https://doi.org/10.1161/CIRCEP.113.001111.
Gunawardene MA, Schaeffer BN, Jularic M, Eickholt C, Maurer T, Akbulak RO, Flindt M, Anwar O, Hartmann J, Willems S. Coronary spasm during pulsed field ablation of the mitral isthmus line. JACC Clin Electrophysiol. 2021;7:1618–20. https://doi.org/10.1016/j.jacep.2021.08.016.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. All authors read and approved the final manuscript. Conceptualization: Christian Blockhaus and Jan-Erik Guelker; formal analysis and investigation: Christian Blockhaus and Ludger Feyen; writing—original draft preparation: Christian Blockhaus and Jan-Erik Guelker; writing—review and editing: Alexander Bufe and Dong-In Shin; supervision: Dong-In Shin and Melchior Seyfarth.
Corresponding author
Ethics declarations
Ethical approval
Waived by the local Institutional Review Board (Ärztekammer Nordrhein, Düsseldorf, Germany) in view of the retrospective nature of this study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Blockhaus, C., Guelker, JE., Feyen, L. et al. Pulsed field ablation for pulmonary vein isolation: real-world experience and characterization of the antral lesion size compared with cryoballoon ablation. J Interv Card Electrophysiol 66, 567–575 (2023). https://doi.org/10.1007/s10840-022-01359-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-022-01359-x