Abstract
Purpose
Multisite cardiac resynchronization therapy (MSCRT) with dual-vein left ventricular (LV) pacing has theoretical advantages over conventional CRT in faster and more physiological LV activation. We aimed to define indications, feasibility, safety, acute, and long-term results of MSCRT.
Methods
All patients implanted with MSCRT during 2008–2014 in a single center were reviewed and analyzed.
Results
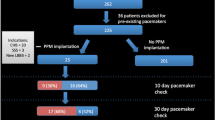
Thirty-nine patients (90% CRT-defibrillators, 64 ± 9 years, 85% male, 74% ischemic etiology) were included. Four groups of indications were recognized: (1) significant tricuspid regurgitation (TR) in patients planned for device implantation without right ventricular lead (n = 3). Follow-up (f/u) of 4 ± 3 years showed major symptomatic improvement in all, with stable LV size and function and deferral of valve surgery; (2) severe heart failure with reduced ejection fraction (HFrEF) and refractory ventricular tachycardia (VT) (n = 4). Except for 1 early death for acute renal failure, all others showed no VT episodes and HF improvement (f/u 4.5 ± 0.5 years); (3) severe HFrEF and wide QRS (≥ 150 ms) or failure of biventricular pacing to narrow QRS during implantation (n = 5). One patient had periprocedural mortality. The others had major clinical improvement; (4) severe HF and narrow QRS/RBBB (n = 27). 23/24 patients with available f/u of 3 ± 1.7 years improved clinically and 57% had EF improvement. In 3 patients, LV1 was disabled and one had LV2 dislodgement.
Conclusions
MSCRT is feasible, safe, and valuable in selected patients with a need to avoid RV lead during device implantation, refractory VT with no other solution, severe HFrEF with wide QRS or CRT non-responsiveness, and severe HF without LBBB. Randomized controlled studies are required.


Similar content being viewed by others
References
Cleland JG, Daubert JC, Erdmann E, Freemantle N, Gras D, Kappenberger L, et al. Cardiac Resynchronization-Heart Failure (CARE-HF) Study Investigators. The effect of cardiac resynchronization on morbidity and mortality in heart failure. N Engl J Med. 2005;352(15):1539–49. https://doi.org/10.1056/NEJMoa050496.
Mullens W, Grimm RA, Verga T, Dresing T, Starling RC, Wilkoff BL, et al. Insights from a cardiac resynchronization optimization clinic as part of a heart failure disease management program. J Am Coll Cardiol. 2009;53(9):765–73. https://doi.org/10.1016/j.jacc.2008.11.024.
Rinaldi CA, Burri H, Thibault B, Curnis A, Rao A, Gras D, et al. A review of multisite pacing to achieve cardiac resynchronization therapy. Europace. 2015;17(1):7–17. https://doi.org/10.1093/europace/euu197.
Pappone C, Rosanio S, Oreto G, Tocchi M, Gulletta S, Salvati A, et al. Cardiac pacing in heart failure patients with left bundle branch block: impact of pacing site for optimizing left ventricular resynchronization. Ital Heart J. 2000;1(7):464–9.
Leclercq C, Gadler F, Kranig W, Ellery S, Gras D, Lazarus A, et al. A randomized comparison of triple-site versus dual-site ventricular stimulation in patients with congestive heart failure. J Am Coll Cardiol. 2008;51(15):1455–62. https://doi.org/10.1016/j.jacc.2007.11.074.
Rogers DP, Lambiase PD, Lowe MD, Chow AW. A randomized double-blind crossover trial of triventricular versus biventricular pacing in heart failure. Eur J Heart Fail. 2012;14(5):495–505. https://doi.org/10.1093/eurjhf/hfs004.
Lenarczyk R, Kowalski O, Kukulski T, Szulik M, Pruszkowska-Skrzep P, Zielinska T, et al. Triple-site biventricular pacing in patients undergoing cardiac resynchronization therapy: a feasibility study. Europace. 2007;9(9):762–7. https://doi.org/10.1093/europace/eum140.
Padeletti L, Colella A, Michelucci A, Pieragnoli P, Ricciardi G, Porciani MC, et al. Dual-site left ventricular cardiac resynchronization therapy. Am J Cardiol. 2008;102(12):1687–92. https://doi.org/10.1016/j.amjcard.2008.08.016.
Ogano M, Iwasaki YK, Tanabe J, Takagi H, Umemoto T, Hayashi M, et al. Antiarrhythmic effect of cardiac resynchronization therapy with triple-site biventricular stimulation. Europace. 2013;15(10):1491–8. https://doi.org/10.1093/europace/eut134.
Ploux S, Whinnett Z, Bordachar P. Left ventricular endocardial pacing and multisite pacing to improve CRT response. J Cardiovasc Transl Res. 2012;5(2):213–8. https://doi.org/10.1007/s12265-011-9342-7.
Ginks MR, Duckett SG, Kapetanakis S, Bostock J, Hamid S, Shetty A, et al. Multi-site left ventricular pacing as a potential treatment for patients with postero-lateral scar: insights from cardiac magnetic resonance imaging and invasive hemodynamic assessment. Europace. 2012;14(3):373–9. https://doi.org/10.1093/europace/eur336.
Bordachar P, Labrousse L, Thambo JB, Reant P, Lafitte S, O'Neill MD, et al. Hemodynamic impact of the left ventricular pacing site during graded ischemia in an open-chest pig model. Europace. 2008;10(2):242–8. https://doi.org/10.1093/europace/eum285.
Köbe J, Dechering DG, Rath B, Reinke F, Mönnig G, Wasmer K, et al. Prospective evaluation of electrocardiographic parameters in cardiac resynchronization therapy: detecting non-responders by left ventricular pacing. Heart Rhythm. 2012;9(4):499–504. https://doi.org/10.1016/j.hrthm.2011.11.009.
Ruschitzka F, Abraham WT, Singh JP, Bax JJ, Borer JS, Brugada J, et al. Cardiac-resynchronization therapy in heart failure with a narrow QRS complex. NEJM. 2013;369(15):1395–405. https://doi.org/10.1056/NEJMoa1306687.
Al-Bawardy R, Krishnaswamy A, Bhargava M, Dunn J, Wazni O, Murat Tuzcu E, et al. Tricuspid regurgitation in patients with pacemakers and implantable cardiac defibrillators: a comprehensive review. Clin Cardiol. 2013;36(5):249–54. https://doi.org/10.1002/clc.22104.
Vaturi M, Kusniec J, Shapira Y, Nevzorov R, Yedidya I, Weisenberg D, et al. Right ventricular pacing increases tricuspid regurgitation grade regardless of the mechanical interference to the valve by the electrode. Eur J Echocardiogr. 2010;11(6):550–3. https://doi.org/10.1093/ejechocard/jeq018.
Sadreddini M, Haroun M, Buikema L, Morillo C, Ribas S, Divarakaramenon S, et al. Tricuspid valve regurgitation induced by temporary or permanent endocardial lead insertion, and the impact of cardiac resynchronization therapy. Open Cardiovasc Med J. 2014;8:83–7.
Pfannmueller B, Hirnle G, Seeburger J, Davierwala P, Schroeter T, Borger MA, et al. Tricuspid valve repair in the presence of a permanent ventricular pacemaker lead. Eur J Cardiothorac Surg. 2011;39(5):657–61. https://doi.org/10.1016/j.ejcts.2010.08.051.
McCarthy PM, Bhudia SK, Rajeswaran J, Hoercher KJ, Lytle BW, Cosgrove DM, et al. Tricuspid valve repair: durability and risk factors for failure. J Thorac Cardiovasc Surg. 2004;127(3):674–85. https://doi.org/10.1016/j.jtcvs.2003.11.019.
Restivo M, Gough WB, el-Sherif N. Reentrant ventricular rhythms in the late myocardial infarction period: prevention of reentry by dual stimulation during basic rhythm. Circulation. 1988;77(2):429–44. https://doi.org/10.1161/01.CIR.77.2.429.
Barsheshet A, Wang PJ, Moss AJ, Solomon SD, Al-Ahmad A, McNitt S, et al. Reverse remodeling and the risk of ventricular tachyarrhythmias in the MADIT-CRT. J Am Coll Cardiol. 2011;57(24):2416–23. https://doi.org/10.1016/j.jacc.2010.12.041.
Sundaram V, Sahadevan J, Waldo AL, Stukenborg GJ, Reddy YNV, Asirvatham SJ, et al. Implantable cardioverter-defibrillators with versus without resynchronization therapy in patients with a QRS duration >180 ms. J Am Coll Cardiol. 2017;69(16):2026–36. https://doi.org/10.1016/j.jacc.2017.02.042.
Stockburger M, Moss AJ, Klein HU, Zareba W, Goldenberg I, Biton Y, et al. Sustained clinical benefit of cardiac resynchronization therapy in non-LBB patients with prolonged PR-interval. MADIT-CRT long-term follow-up. Clin Res Cardiol. 2016;105(11):944–52. https://doi.org/10.1007/s00392-016-1003-z.
Haghjoo M, Bagherzadeh A, Farahani MM, Haghighi ZO, Sadr-Ameli MA. Significance of QRS morphology in determining the prevalence of mechanical dyssynchrony in heart failure patients eligible for cardiac resynchronization: particular focus on patientswith right bundle branch block and without coexisting left-sided conduction defects. Europace. 2008;10(5):566–71. https://doi.org/10.1093/europace/eun081.
Bordachar P, Ploux S, Ritter P. Three left ventricular leads required for improved hemodynamic and clinical status of a patient with very severe heart failure and a narrow QRS duration. Europace. 2011 Mar;13(3):439. https://doi.org/10.1093/europace/euq370.
Daubert JC. Triple-site Biventricular Stimulation in the Optimization of CRT (TRIUMPH-CRT) ClinicalTrials.gov Identifier: NCT02350842.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the local research ethics committee and all patients gave their written informed consent to the procedure.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Laish-Farkash, A., Bruoha, S., Khalameizer, V. et al. Multisite cardiac resynchronization therapy for traditional and non-traditional indications. J Interv Card Electrophysiol 51, 143–152 (2018). https://doi.org/10.1007/s10840-018-0316-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-018-0316-4