Abstract
Objectives
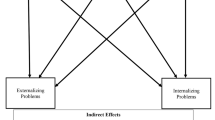
Bereaved siblings experience more externalizing problems compared to non-bereaved peers and norms; however, the mechanisms explaining this phenomenon have not been empirically examined. This study tested the serial indirect effects of sibling bereavement on adolescents’ externalizing problems through parent distress (i.e., internalizing symptoms) and parenting (i.e., parenting behaviors, parent-adolescent communication).
Methods
During home visits, 72 bereaved adolescents (ages 10–18) whose brother/sister died from cancer and 60 comparison peers reported about their externalizing problems and their mothers’ and fathers’ parenting behaviors (warmth, behavioral control, psychological control) and parent-adolescent communication (open communication, problematic communication). Mothers and fathers reported their own internalizing symptoms.
Results
Bereaved siblings reported more externalizing problems (p = 0.048) and bereaved mothers reported more internalizing symptoms relative to the comparison group (p = 0.015). Serial multiple mediation models indicated that elevated externalizing problems were partially explained by both bereaved mothers’ internalizing symptoms and parenting and communication (less warmth [CI: 0.04, 0.86], more psychological control [CI: 0.03, 0.66], and more problematic mother-adolescent communication [CI: 0.03, 0.79]), with a significant indirect effect also emerging for open mother-adolescent communication [CI: 0.05, 1.59]. Bereaved fathers did not significantly differ in internalizing symptoms from comparison fathers (p = 0.453), and no significant indirect effects emerged for fathers.
Conclusions
Elevated externalizing problems in bereaved siblings may result from mothers’ distress and the impact on their parenting and communication. Targeting adjustment and parenting in bereaved mothers following a child’s death may reduce externalizing problems in bereaved siblings. Research to evaluate family-centered interventions is needed.

Similar content being viewed by others
References
Achenbach, T. M., & Rescorla, L. (2001). ASEBA school-age forms & profiles. Burlington, VT: Aseba.
Achenbach, T. M., & Rescorla, L. A. (2003). Manual for the ASEBA adult forms & profiles. Burlington, VT: University of Vermont, Research Center for Children, Youth, & Families.
Alam, R., Barrera, M., D’Agostino, N., Nicholas, D., & Schneiderman, G. (2012). Bereavement experience of mothers and fathers overtime after the death of a child due to cancer: gender of caregiver differences. Death Studies, 36, 1–22. https://doi.org/10.1080/07481187.2011.553312.
Arnold, J., & Gemma, P. B. (2008). The continuing process of parental grief. Death Studies, 32, 658–673. https://doi.org/10.1080/07481180802215718.
Barnes, H. L., & Olson, D. H. (1985). Parent-adolescent communication and the circumplex model. Child Development, 56, 438–447. https://doi.org/10.2307/1129732.
Barrera, M., Alam, R., Mammone, D., Agostino, N., Nicholas, D. B., & Schneiderman, G. (2013). Parental reports of siblings’ grieving after a childhood cancer death: a longitudinal study. Death Studies, 37, 35–46. https://doi.org/10.1080/07481187.2012.678262.
Barrera, M., D'Agostino, N. M., Schneiderman, G., Tallett, S., Spencer, L., & Jovcevska, V. (2007). Patterns of parental bereavement following the loss of a child and related factors. Omega-Journal of Death and Dying, 55, 145–167. https://doi.org/10.2190/OM.55.2.d.
Barrera, M., O'connor, K., D'Agostino, N. M., Spencer, L., Nicholas, D., Jovcevska, V., & Schneiderman, G. (2009). Early parental adjustment and bereavement after childhood cancer death. Death Studies, 33, 497–520. https://doi.org/10.1080/07481180902961153.
Barry, L. C., Kasl, S. V., & Prigerson, H. G. (2002). Psychiatric disorders among bereaved persons: the role of perceived circumstances of death and preparedness for death. The American journal of geriatric psychiatry, 10, 447–457. https://doi.org/10.1097/00019442-200207000-00011.
Bergman, A. S., Axberg, U., & Hanson, E. (2017). When a parent dies–a systematic review of the effects of support programs for parentally bereaved children and their caregivers. BMC Palliative Care, 16, 39. https://doi.org/10.1186/s12904-017-0223-y.
Beveridge, R. M., & Berg, C. A. (2007). Parent–adolescent collaboration: an interpersonal model for understanding optimal interactions. Clinical Child and Family Psychology Review, 10, 25–52. https://doi.org/10.1007/s10567-006-0015-z.
Birenbaum, L. K., Robinson, M. A., Phillips, D. S., Stewart, B. J., & McCown, D. E. (1990). The response of children to the dying and death of a sibling. OMEGA-Journal of Death and Dying, 20, 213–228. https://doi.org/10.2190/DHGK-NMG8-FFR4-UFW9.
Cacciatore, J., Lacasse, J. R., Lietz, C. A., & McPherson, J. (2013–2014). A parent’s tears: primary results from the traumatic experiences and resiliency study. OMEGA-Journal of Death and Dying, 68, 183–205.
deCinque, N., Monterosso, L., Dadd, G., Sidhu, R., Macpherson, R., & Aoun, S. (2006). Bereavement support for families following the death of a child from cancer: experience of bereaved parents. Journal of Psychosocial Oncology, 24, 65–83. https://doi.org/10.1300/J077v24n02_05.
Fanos, J. H., & Nickerson, B. G. (1991). Long-term effects of sibling death during adolescence. Journal of Adolescent Research, 6, 70–82. https://doi.org/10.1177/074355489161006.
Foster, T. L., Gilmer, M. J., Vannatta, K., Barrera, M., Davies, B., Dietrich, M. S., & Gerhardt, C. A. (2012). Changes in siblings after the death of a child from cancer. Cancer Nursing, 35, 347–354. https://doi.org/10.1097/NCC.0b013e3182365646.
Gerhardt, C. A., Fairclough, D. L., Grossenbacher, J. C., Barrera, M., Jo Gilmer, M., Foster, T. L., & Vannatta, K. (2012). Peer relationships of bereaved siblings and comparison classmates after a child's death from cancer. Journal of Pediatric Psychology, 37, 209–219. https://doi.org/10.1093/jpepsy/jsr082.
Gerhardt, C. A., Lehmann, V., Long, K. A., & Alderfer, M. A. (2015). Supporting siblings as a standard of care in pediatric oncology. Pediatric Blood & Cancer, 62(S5), S750–S804. https://doi.org/10.1002/pbc.25821.
Gilmer, M. J., Foster, T. L., Vannatta, K., Barrera, M., Davies, B., Dietrich, M. S., & Gerhardt, C. A. (2012). Changes in parents after the death of a child from cancer. Journal of Pain and Symptom Management, 44, 572–582. https://doi.org/10.1016/j.jpainsymman.2011.10.017.
Giovanola, J. (2005). Sibling involvement at the end of life. Journal of Pediatric Oncology Nursing, 22, 222–226. https://doi.org/10.1177/1043454205276956.
Haine, R. A., Ayers, T. S., Sandler, I. N., & Wolchik, S. A. (2008). Evidence-based practices for parentally bereaved children and their families. Professional Psychology, Research and Practice, 39, 113–121. https://doi.org/10.1037/0735-7028.39.2.113.
Hayes, A. F. (2013). Introduction to mediation, moderation, and conditional process analysis: a regression-based approach. New York, NY: Guilford Press.
Hoffmann, R., Kaiser, J., & Kersting, A. (2018). Psychosocial outcomes in cancer‐bereaved children and adolescents: a systematic review. Psycho‐Oncology, 27, 2327–2338. https://doi.org/10.1002/pon.4863.
Hogan, N. S., & Greenfield, D. B. (1991). Adolescent sibling bereavement symptomatology in a large community sample. Journal of Adolescent Research, 6, 97–112. https://doi.org/10.1177/074355489161008.
Hogan, N. S., Greenfield, D. B., & Schmidt, L. A. (2001). Development and validation of the Hogan Grief reaction checklist. Death Studies, 25, 1–32. https://doi.org/10.1080/07481180125831.
Horsley, H., & Patterson, T. (2006). The effects of a parent guidance intervention on communication among adolescents who have experienced the sudden death of a sibling. The American Journal of Family Therapy, 34, 119–137. https://doi.org/10.1080/01926180500301519.
Hutton, C. J., & Bradley, B. S. (1994). Effects of sudden infant death on bereaved siblings; a comparative Study. Journal of Child Psychology and Psychiatry, 35, 723–732. https://doi.org/10.1111/j.1469-7610.1994.tb01217.x.
Kwok, O. M., Haine, R. A., Sandler, I. N., Ayers, T. S., Wolchik, S. A., & Tein, J. Y. (2005). Positive parenting as a mediator of the relations between parental psychological distress and mental health problems of parentally bereaved children. Journal of Clinical Child and Adolescent Psychology, 34, 260–271. https://doi.org/10.1207/s15374424jccp3402_5.
Leinonen, J. A., Solantaus, T. S., & Punamäki, R. L. (2003). Parental mental health and children's adjustment: The quality of marital interaction and parenting as mediating factors. Journal of Child Psychology and Psychiatry, 44, 227–241.
Lichtenthal, W. G., Corner, G. W., Sweeney, C. R., Wiener, L., Roberts, K. E., Baser, R. E., & Prigerson, H. G. (2015). Mental health services for parents who lost a child to cancer: If we build them, will they come? Journal of Clinical Oncology, 33, 2246–2253. https://doi.org/10.1200/JCO.2014.59.0406.
Lohan, J. A., & Murphy, S. A. (2002). Parents' perceptions of adolescent sibling grief responses after an adolescent or young adult child's sudden, violent death. Omega-Journal of Death and Dying, 44, 77–95. https://doi.org/10.2190/M9LW-4RJY-QKYF-H8BE.
Long, K. A., Marsland, A. L., & Alderfer, M. A. (2013). Cumulative family risk predicts sibling adjustment to childhood cancer. Cancer, 119, 2503–2510. https://doi.org/10.1002/cncr.28077.
Lövgren, M., Jalmsell, L., Eilegård Wallin, A., Steineck, G., & Kreicbergs, U. (2016). Siblings' experiences of their brother's or sister's cancer death: a nationwide follow‐up 2–9 years later. Psycho-Oncology, 25, 435–440. https://doi.org/10.1002/pon.3941.
Lövgren, M., Sveen, J., Nyberg, T., Eilegård Wallin, A., Prigerson, H. G., Steineck, G., & Kreicbergs, U. (2018). Care at end of life influences grief: a nationwide long-term follow-up among young adults who lost a brother or sister to childhood cancer. Journal of palliative medicine, 21, 156–162.
McCown, D. E., & Davies, B. (1995). Patterns of grief in young children following the death of a sibling. Death Studies, 19, 41–53. https://doi.org/10.1080/07481189508252712.
Morris, A. T., Gabert-Quillen, C., Friebert, S., Carst, N., & Delahanty, D. L. (2016). The indirect effect of positive parenting on the relationship between parent and sibling bereavement outcomes after the death of a child. Journal of Pain and Symptom Management, 51, 60–70. https://doi.org/10.1016/j.jpainsymman.2015.08.011.
Packman, W., Horsley, H., Davies, B., & Kramer, R. (2006). Sibling bereavement and continuing bonds. Death Studies, 30, 817–841. https://doi.org/10.1080/07481180600886603.
Papp, L. M., Cummings, E. M., & Goeke-Morey, M. C. (2005). Parental psychological distress, parent-child relationship qualities, and child adjustment: direct, mediating, and reciprocal pathways. Parenting: Science and Practice, 5, 259–283. https://doi.org/10.1207/s15327922par0503_2.
Robila, M., & Krishnakumar, A. (2006). The impact of maternal depression and parenting behaviors on adolescents' psychological functioning in Romania. Journal of Child and Family Studies, 15, 70–81. https://doi.org/10.1007/s10826-005-9009-6.
Rosenberg, A. R., Baker, K. S., Syrjala, K., & Wolfe, J. (2012). Systematic review of psychosocial morbidities among bereaved parents of children with cancer. Pediatric Blood & Cancer, 58, 503–512. https://doi.org/10.1002/pbc.23386.
Rosenberg, A. R., Postier, A., Osenga, K., Kreicbergs, U., Neville, B., Dussel, V., & Wolfe, J. (2015). Long-term psychosocial outcomes among bereaved siblings of children with cancer. Journal of Pain and Symptom Management, 49, 55–65. https://doi.org/10.1016/j.jpainsymman.2014.05.006.
Samson, K., Rourke, M., & Alderfer, M. (2016). A qualitative analysis of the impact of childhood cancer on the lives of siblings at school, inextracurricular activities, and with friends. Clinical Practice in Pediatric Psychology, 4, 362–372.
Schludermann, E. H., & Schludermann, S. M. (1988). Children’s report of parent behavior inventory (CRPBI-30) for older children and adolescents (Technical Report). Winnipeg, MB, Canada: University of Manitoba, Department of Psychology.
Shankar, S., Nolte, L., & Trickey, D. (2017). Continuing bonds with the living: bereaved parents’ narratives of their emotional relationship with their children. Bereavement Care, 36, 103–111. https://doi.org/10.1080/02682621.2017.1386400.
Sood, A. B., Razdan, A., Weller, E. B., & Weller, R. A. (2006). Children’s reactions to parental and sibling death. Current Psychiatry Reports, 8, 115–120. https://doi.org/10.1007/s11920-006-0008-0.
Walsh, F., & McGoldrick, M. (2013). Bereavement: a family life cycle perspective. Family Science, 4, 20–27. https://doi.org/10.1080/19424620.2013.819228.
Wilkins, K. L., & Woodgate, R. L. (2005). A review of qualitative research on the childhood cancer experience from the perspective of siblings: a need to give them a voice. Journal of Pediatric Oncology Nursing, 22, 305–319. https://doi.org/10.1177/10434542052780.
Acknowledgements
This research was supported by grants from the National Institutes of Health (R01 CA98217), The Research Institute at Nationwide Children's Hospital, and Cincinnati Children's Hospital Medical Center. Portions of this work were presented at the 16th Biennial Meeting of the Society for Research on Adolescence, Baltimore, Maryland (April, 2016). The authors would like to thank the families who generously participated in this work.
Author Contributions
KMHS: analyzed the data and wrote the paper. EAM: assisted with data analyses and contributed to writing and editing of the final manuscript. MCK: assisted with data analyses and contributed to writing and editing of the final manuscript. AMW: assisted with data analyses and contributed to writing and editing of the final manuscript. MB: collaborated in the execution of the study and editing of the final manuscript. MJG: collaborated in the execution of the study and editing of the final manuscript. TFA: collaborated in the execution of the study and editing of the final manuscript. BEC: collaborated in the execution of the study. DLF: collaborated in the execution of the study and management of the data. BD: collaborated in the design of the study and editing of the final manuscript. NH: collaborated in the design of the study and editing of the final manuscript. KV: collaborated in the design and execution of the study. CAG: designed and executed the study and contributed to editing of the final manuscript.
Funding
Grants from the National Institutes of Health (grant number R01 CA98217), The Research Institute at Nationwide Children's Hospital, and Cincinnati Children’s Hospital Medical Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Howard Sharp, K.M., Meadows, E.A., Keim, M.C. et al. The Influence of Parent Distress and Parenting on Bereaved Siblings’ Externalizing Problems. J Child Fam Stud 29, 1081–1093 (2020). https://doi.org/10.1007/s10826-019-01640-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10826-019-01640-0