Abstract
Purpose
To evaluate the impact of a single-step (SS) warming versus standard warming (SW) protocol on the survival/expansion of vitrified blastocysts and their clinical outcomes post-frozen embryo transfer (FET).
Methods
Retrospective analysis was performed on 200 vitrified/warmed research blastocysts equally divided amongst two thawing protocols utilizing the Fujifilm Warming NX kits (Fujifilm, CA). SW utilized the standard 14-minute manufacturer’s guidelines. SS protocol required only a one-minute immersion in thaw solution (TS) before the embryos were transferred to culture media. A time-interrupted study was performed evaluating 752 FETs (SW: 376 FETs, SS 376 FETs) between April 2021-December 2022 at a single academic fertility clinic in Boston, Massachusetts. Embryologic, clinical pregnancy, and live birth outcomes were assessed using generalized estimated equation (GEE) models, which accounted for potential confounders.
Results
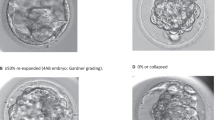
There was 100% survival for all blastocysts (n = 952 embryos) with no differences in blastocyst re-expansion regardless of PGT status. Adjusted analysis showed no differences in implantation, clinical pregnancy, spontaneous abortion, or biochemical pregnancy rate. A higher odds of multiple gestation [AdjOR(95%CI) 1.06 (1.01, 1.11), p = 0.019] were noted, even when adjusting for number of embryos transferred [AdjOR(95%CI) 1.05 (1.01, 1.10)]. Live birth outcomes showed no differences in live birth rates or birthweight at delivery.
Conclusions
The study found equivalent outcomes for SS and SW in all parameters except for a slight rise in the rate of multiple gestations. The results suggest that SS warming is an efficient, viable alternative to SW, reducing thaw times without adverse effects on live birth rates or neonatal birth weights.

Similar content being viewed by others
Data availability
Data regarding an of the subjects in the study has not been previously published. The datasets and R (v4.1.3; The R Foundation for Statistical Computing) statistical code used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Vajta G, Nagy ZP. Are programmable freezers still needed in the embryo laboratory? Review on vitrification. Reprod Biomed Online. 2006;12:779–96.
Rienzi L, Gracia C, Maggiulli R, LaBarbera AR, Kaser DJ, Ubaldi FM et al. Oocyte, embryo and blastocyst cryopreservation in ART: systematic review and meta-analysis comparing slow-freezing versus vitrification to produce evidence for the development of global guidance. Hum Reprod Update. 2016;humupd;dmw038v1.
Li Z, Wang YA, Ledger W, Edgar DH, Sullivan EA. Clinical outcomes following cryopreservation of blastocysts by vitrification or slow freezing: a population-based cohort study. Hum Reprod. 2014;29:2794–801.
Roy TK, Bradley CK, Bowman MC, McArthur SJ. Single-embryo transfer of vitrified-warmed blastocysts yields equivalent live-birth rates and improved neonatal outcomes compared with fresh transfers. Fertil Steril. 2014;101:1294–1301e2.
Zaat T, Zagers M, Mol F, Goddijn M, Van Wely M, Mastenbroek S. Fresh versus frozen embryo transfers in assisted reproduction. Cochrane Gynaecology and Fertility Group, editor. Cochrane Database of Systematic Reviews. 2021 [cited 2024 Jan 17];2021. https://doi.org/10.1002/14651858.CD011184.pub3.
Nagy ZP, Shapiro D, Chang C-C. Vitrification of the human embryo: a more efficient and safer in vitro fertilization treatment. Fertil Steril. 2020;113:241–7.
Canosa S, Parmegiani L, Charrier L, Gennarelli G, Garello C, Granella F, et al. Are commercial warming kits interchangeable for vitrified human blastocysts? Further evidence for the adoption of a universal warming protocol. J Assist Reprod Genet. 2022;39:67–73.
Parmegiani L, Minasi MG, Arnone A, Casciani V, Cognigni GE, Viñoles R, et al. Universal warming protocol for vitrified oocytes to streamline cell exchange for transnational donation programs: a multi-center study. J Assist Reprod Genet. 2020;37:1379–85.
Manns JN, Katz S, Whelan J, Patrick JL, Holt T, Merline AM, Ultra-fast blastocyst, warming technique reduces warming times to 1 min and yields similar survival and re-expansion compared to blastocysts warmed using a standard method, et al. Fertil Steril. 2021;116:e165.
Du Q-Y, Wang E-Y, Huang Y, Guo X-Y, Xiong Y-J, Yu Y-P, et al. Blastocoele expansion degree predicts live birth after single blastocyst transfer for fresh and vitrified/warmed single blastocyst transfer cycles. Fertil Steril. 2016;105:910–919e1.
Shu Y, Watt J, Gebhardt J, Dasig J, Appling J, Behr B. The value of fast blastocoele re-expansion in the selection of a viable thawed blastocyst for transfer. Fertil Steril. 2009;91:401–6.
Hershko-Klement A, Raviv S, Nemerovsky L, Rom T, Itskovich A, Bakhshi D, et al. Standardization of Post-vitrification Human blastocyst expansion as a Tool for Implantation Prediction. JCM. 2022;11:2673.
Cimadomo D, Capalbo A, Levi-Setti PE, Soscia D, Orlando G, Albani E, et al. Associations of blastocyst features, trophectoderm biopsy and other laboratory practice with post-warming behavior and implantation. Hum Reprod. 2018;33:1992–2001.
Parmegiani L, Beilby KH, Arnone A, Bernardi S, Maccarini AM, Nardi E, et al. Testing the efficacy and efficiency of a single universal warming protocol for vitrified human embryos: prospective randomized controlled trial and retrospective longitudinal cohort study. J Assist Reprod Genet. 2018;35:1887–95.
Serdarogullari M, Coban O, Boynukalin FK, Bilgin EM, Findikli N, Bahceci M. Successful application of a single warming protocol for embryos cryopreserved by either slow freezing or vitrification techniques. Syst Biology Reproductive Med. 2019;65:12–9.
Parmegiani L, Tatone C, Cognigni GE, Bernardi S, Troilo E, Arnone A, et al. Rapid warming increases survival of slow-frozen sibling oocytes: a step towards a single warming procedure irrespective of the freezing protocol? Reprod Biomed Online. 2014;28:614–23.
Funding
There was no funding received on behalf of the research team or any listed authors to conduct this project.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Charles Bormann, Victoria Jiang, and Panagiotis Cherouveim. The first draft of the manuscript was written by Victoria Jiang and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Informed consent was obtained from each individual before participation. Study protocols were approved by the Institutional Review Board (IRB#2022P001227) at Massachusetts General Hospital.
Consent for publication
Not applicable.
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jiang, V.S., Cherouveim, P., Naert, M.N. et al. Live birth outcomes following single-step blastocyst warming technique – optimizing efficiency without impacting live birth rates. J Assist Reprod Genet (2024). https://doi.org/10.1007/s10815-024-03069-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10815-024-03069-x