Abstract
Purpose
To evaluate live birth rates (LBRs) for in vitro fertilization (IVF) cycles with ≤5 follicles at trigger, with the goal of helping patients with low follicle counts decide whether to proceed to retrieval.
Methods
This is a retrospective cohort study from an urban, university-affiliated fertility center. All IVF cycles that yielded <10 oocytes between 2016 and 2020 were reviewed. Cycles were included if <5 follicles measuring >14 mm were verified on trigger day. The primary outcome was LBR per retrieval after fresh or frozen transfer. Secondary outcomes were number of oocytes, mature oocytes, 2-pronuclear zygotes (2-PNs), blastocysts for transfer/biopsy, and euploid blastocysts (if preimplantation genetic testing for aneuploidy (PGT-A) was used).
Results
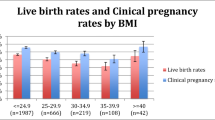
1502 cycles (900 with PGT-A) from 972 patients were included. Mean number of oocytes, mature oocytes, 2-PNs, blastocysts for transfer/biopsy, and euploid blastocysts differed by follicle number (p < 0.001). Across all age groups, there were differences in LBR associated with follicle number (p < 0.001). However, within age groups, not all results were significant. For example, for patients <35 years, LBR did not differ by follicle number and among patients 35–37 years; LBR with two or three follicles was lower than with five (p < 0.02). LBR for patients 35–40 years was <20% with 1–3 follicles and 25–40% with 4–5 follicles. LBR for patients >41 years was <5% with 1–3 follicles and <15% with 4–5 follicles.
Conclusion
As expected, LBR is higher with more follicles. Providing patients with <5 follicles with specific data can help them weigh the emotional, physical, and financial costs of retrieval.


Similar content being viewed by others
Data availability
Data for this study can be made available upon request.
References
Peipert BJ, Montoya MN, Bedrick BS, Seifer DB, Jain T. Impact of in vitro fertilization state mandates for third party insurance coverage in the United States: a review and critical assessment. Reprod Biol Endocrinol. 2022;20:111.
Klinkert ER, Broekmans FJ, Looman CW, Te Velde ER. A poor response in the first in vitro fertilization cycle is not necessarily related to a poor prognosis in subsequent cycles. Fertil Steril. 2004;81:1247–53.
Biljan MM, Buckett WM, Dean N, Phillips SJ, Tan SL. The outcome of IVF-embryo transfer treatment in patients who develop three follicles or less. Hum Reprod. 2000;15:2140–4.
Shrem G, Salmon-Divon M, Mahfoudh AM, Balayla J, Volodarsky-Perel A, Henderson S, et al. Influence of maternal age and ovarian reserve on the decision to continue or to cancel IVF cycles in patients with one or two large follicles: a dual effect. Reprod Sci. 2022;29:291–300.
Reichman DE, Gunnala V, Meyer L, Spandorfer S, Schattman G, Davis OK, et al. In vitro fertilization versus conversion to intrauterine insemination in the setting of three or fewer follicles: how should patients proceed when follicular response falls short of expectation? Fertil Steril. 2013;100:94–9.
Ferraretti AP, La Marca A, Fauser BC, Tarlatzis B, Nargund G, Gianaroli L. ESHRE consensus on the definition of ‘poor response’ to ovarian stimulation for in vitro fertilization: the Bologna criteria. Hum Reprod. 2011;26:1616–24.
Cohen Y, Tannus S, Alzawawi N, Son WY, Dahan M, Buckett W. Poor ovarian response as a predictor for live birth in older women undergoing IVF. Reprod Biomed Online. 2018;36:435–41.
Poseidon Group (Patient-Oriented Strategies Encompassing Individualized Oocyte Number), Alviggi C, Andersen CY, Buehler K, Conforti A, De Placido G, et al. A new more detailed stratification of low responders to ovarian stimulation: from a poor ovarian response to a low prognosis concept. Fertil Steril. 2016;105:1452–3.
Barnhart KT. Live birth is the correct outcome for clinical trials evaluating therapy for the infertile couple. Fertil Steril. 2014;101:1205–8.
NYU Langone Fertility Center preliminary clinic summary report. Society for Assisted Reproductive Technology. 2021. https://sartcorsonline.com/Csr/PublicSnapshotReport?ClinicPKID=1895&reportingYear=2021&fromDisclaimer=true. Accessed 1 Sept 2023.
Roberts SA, Wilkinson J, Vail A, Brison DR. Does PGT-A improve assisted reproduction treatment success rates: what can the UK Register data tell us? J Assist Reprod Genet. 2022;39:2547–54.
Kucherov A, Fazzari M, Lieman H, Ball GD, Doody K, Jindal S. PGT-A is associated with reduced cumulative live birth rate in first reported IVF stimulation cycles age ≤ 40: an analysis of 133,494 autologous cycles reported to SART CORS. J Assist Reprod Genet. 2023;40:137–49.
Munné S, Kaplan B, Frattarelli JL, Child T, Nakhuda G, Shamma FN, Silverberg K, Kalista T, Handyside AH, Katz-Jaffe M, Wells D, Gordon T, Stock-Myer S, Willman S, STAR Study Group. Preimplantation genetic testing for aneuploidy versus morphology as selection criteria for single frozen-thawed embryo transfer in good-prognosis patients: a multicenter randomized clinical trial. Fertil Steril. 2019;112:1071-1079.e7.
Fujii DT, Quesnell JL, Heitmann RJ. Conversion to IUI versus continuance with IVF in low responder patients: a systematic review. Eur J Obstet Gynecol Reprod Biol. 2018;227:35–40.
Shahine LK, Lathi RB, Baker VL. Oocyte retrieval versus conversion to intrauterine insemination in patients with poor response to gonadotropin therapy. Fertil Steril. 2009;92:1315–7.
Delbos L, Parot-Schinkel E, El Hachem H, Legendre G, Descamps P, Boucret L, et al. ConFIRM trial – conversion of in vitro fertilization cycles to intrauterine inseminations in patients with a poor ovarian response to stimulation: a protocol for a multicentric, prospective randomized trial. Trials. 2018;19:565.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. McCulloh has the following conflicts of interest: Director at Biogenetics Laboratory in Mountainside, NJ; Director at the Sperm and Embryo Bank of New York in New York, NY; Director at Biogenetics Laboratory in Brooklyn, NY; Director of Clinical Science at ReproART: the Georgian-American Center for Reproductive Medicine in Tblilis, Georgia; consulting services through McCulloh Associates in Port Washington, NY; recent Scientific Advisory Board member of GranataBio in Duxbury, MA. The other authors of this study have no conflicts of interest to report.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bayefsky, M.J., Cascante, S.D., McCulloh, D.H. et al. Live birth rates in in vitro fertilization cycles with five or fewer follicles. J Assist Reprod Genet 41, 223–229 (2024). https://doi.org/10.1007/s10815-023-02985-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-023-02985-8