Abstract
Purpose
To compare keratometry data between the handheld Retinomax K-plus 3 and the table-mounted IOLMaster 700.
Methods
Healthy adult volunteers were prospectively recruited to the study. All participants underwent 3 consecutive keratometry measurements using the Retinomax K-plus 3 and a single biometry assessment using the IOLMaster 700. Differences between the Retinomax K-plus 3 and the IOLMaster 700 were assessed using Wilcoxon test for paired samples, Spearman correlation, Bland–Altman and mountain plots.
Result
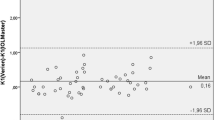
Twenty-eight healthy subjects with a median age of 37 years (interquartile range (IQR) 28–44 years) were included in the study. The median mean keratometry (mean K) reading was higher using the Retinomax K-plus 3 (44.04D; IQR 42.96–45.61D) compared to the IOLMaster 700 (43.78D; IQR 43.22–44.90D, p < 0.01), with a mean difference of 0.18D (95% confidence interval (CI) 0.11–0.23D). Mean K readings were highly correlated between the 2 devices (r = 0.995, p < 0.01). Bland–Altman plots showed 95% limits of agreement between −0.14D and 0.49D. Frequency histogram of mean K reading differences between the Retinomax K-plus 3 and the IOLMaster 700 showed that 56% of cases were between ± 0.2D, 93% of cases were between ± 0.4D and all cases were between ± 0.5D. Mean corneal astigmatism measurement was higher using the Retinomax K-plus 3 (1.01 ± 0.40D) compared to the IOLMaster 700 (0.77 ± 0.36D), with a mean difference of 0.23 ± 0.37D (p < 0.01) between the devices.
Conclusions
A good agreement exists between the Retinomax K-plus 3 and the IOLMaster 700 regarding keratometry readings. This enables cataract surgeons to safely use the Retinomax K-plus 3 device when indicated.





Similar content being viewed by others
Data availability
Accesses to data will be given upon request from the corresponding author.
Abbreviations
- IQR:
-
Interquartile range
- K:
-
Keratometry
- CI:
-
Confidential interval
- IOL:
-
Intraocular lens
- SS-OCT:
-
Swept source ocular coherence tomography
- K1:
-
Minimum keratometry
- K2:
-
Maximum keratometry
- ICC:
-
Intraclass correlation coefficient
- D:
-
Diopter
References
Kolega MS et al (2015) Comparison of IOL–master and ultrasound biometry in preoperative intra ocular lens (IOL) power calculation. Coll Antropol 39(1):233–235
Lee AC, Qazi MA, Pepose JS (2008) Biometry and intraocular lens power calculation. Curr Opin Ophthalmol 19(1):13–17
Shajari M et al (2017) Comparison of axial length, corneal curvature, and anterior chamber depth measurements of 2 recently introduced devices to a known biometer. Am J Ophthalmol 178:58–64
Roessler GF et al (2012) Accuracy of intraocular lens power calculation using partial coherence interferometry in patients with high myopia. Ophthalmic Physiol Opt 32(3):228–233
Kunavisarut P et al (2012) Accuracy and reliability of IOL master and A-scan immersion biometry in silicone oil-filled eyes. Eye (Lond) 26(10):1344–1348
Yu SS, Song H, Tang X (2017) Repeatability of ophtha top topography and comparison with IOL-master and Lenstarls900 in cataract patients. Int J Ophthalmol 10(11):1703–1709
Borchert M et al (2008) Testability of the Retinomax autorefractor and IOLMaster in preschool children: the Multi-ethnic Pediatric Eye Disease Study. Ophthalmology 115(8):1422–1425
Akman A, Asena L, Gungor SG (2016) Evaluation and comparison of the new swept source OCT-based IOLMaster 700 with the IOLMaster 500. Br J Ophthalmol 100(9):1201–1205
Wang Q et al (2012) A comprehensive assessment of the precision and agreement of anterior corneal power measurements obtained using 8 different devices. PLoS One. 7(9):e45607
Kiraly L et al (2017) Repeatability and agreement of central corneal thickness and keratometry measurements between four different devices. J Ophthalmol 2017:6181405
Karakosta A et al (2012) Choice of analytic approach for eye-specific outcomes: one eye or two? Am J Ophthalmol 153(3):571–579
Koo TK, Li MY (2016) A Guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15(2):155–163
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1(8476):307–310
Monti KL (1995) Folded empirical distribution function curves—mountain plots. Am Stat 49(4):342–345
Liang CL et al (2004) Comparison of the handheld Retinomax K-Plus2 and on-table autokeratometers in children with and without cycloplegia. J Cataract Refract Surg 30(3):669–674
Gauvin M, Wallerstein A (2018) AstigMATIC: an automatic tool for standard astigmatism vector analysis. BMC Ophthalmol 18(1):255
Cordonnier M (2006) Screening for refractive errors in children. Compr Ophthalmol Update 7(2):63–75
Cordonnier M et al (1998) How accurate is the hand-held refractor Retinomax(R) in measuring cycloplegic refraction: a further evaluation. Strabismus 6(3):133–142
Cordonnier M, Kallay O (2001) Non-cycloplegic screening for refractive errors in children with the hand-held autorefractor Retinomax: final results and comparison with non-cycloplegic photoscreening. Strabismus 9(2):59–70
Steele G, Ireland D, Block S (2003) Cycloplegic autorefraction results in pre-school children using the nikon retinomax plus and the welch allyn suresight. Optom Vis Sci 80(8):573–577
Ying GS et al (2011) ROC analysis of the accuracy of noncycloplegic retinoscopy, retinomax autorefractor, and suresight vision screener for preschool vision screening. Invest Ophthalmol Vis Sci 52(13):9658–9664
Isenberg SJ et al (2004) Corneal topography of neonates and infants. Arch Ophthalmol 122(12):1767–1771
Funding
The authors have no financial or proprietary interests in any material discussed in this article.
Author information
Authors and Affiliations
Contributions
Uri Elbaz contributed to conceptualization; Uri Elbaz, Irit Bahar, Raimo Tuuminen and Gad Dotan were involved in methodology; Hagar Olshaker, Ortal Buhbut, Asaf Achiron, Gad Dotan, Issac Levy and Assaf Gershoni contributed to formal analysis and investigation; Hagar Olshaker and Ortal Buhbut were involved in writing—original draft preparation; Asaf Achiron, Gad Dotan, Issac Levy, Raimo Tuuminen, Assaf Gershoni, Irit Bahar, and Uri Elbaz contributed to writing—review and editing; and Uri Elbaz, Irit Bahar, Raimo Tuuminen and Gad Dotan were involved in supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no interests that are directly or indirectly related to the work submitted for publication.
Consent to participate
Freely given, informed consent to participate in the study was obtained from participants.
Consent to publish
Consent from participants to publish their data prior to submitting their paper to a journal was granted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Olshaker, H., Buhbut, O., Achiron, A. et al. Comparison of keratometry data using handheld and table-mounted instruments in healthy adults. Int Ophthalmol 41, 3451–3458 (2021). https://doi.org/10.1007/s10792-021-01909-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-01909-8