Abstract
Purpose
To compare the efficacy of nepafenac on anterior chamber flare and intraocular pressure(IOP) in healthy (group 1) and uveitic eyes (group 2) undergoing cataract surgery.
Methods
A retrospective, consecutive case series study.
Results
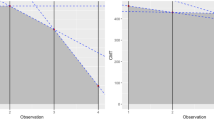
Among 54 the patients, 14 had a history of uveitis. The groups were similar in age and gender. There were significant changes in flare values in both groups. When the temporal changes of flare values were compared, there was no difference between the two groups. There were no significant changes in IOP values in both group. When the temporal changes of IOP values were compared, there was no difference between the groups.
Conclusions
Nepafenac 0.1% has been shown to be effective in suppressing inflammation after cataract surgery in uveitic eyes as well as in healthy eyes. In addition, it has been observed that it does not increase intraocular pressure in both healthy and uveitic eyes and it is safe to use with this regard.


Similar content being viewed by others
References
Congdon N, Vingerling JR, Klein BE, West S, Friedman DS, Kempen J, O'Colmain B, Wu SY, Taylor HR, Eye Diseases Prevalence Research G (2004) Prevalence of cataract and pseudophakia/aphakia among adults in the United States. Arch Ophthalmol 122(4):487–494. https://doi.org/10.1001/archopht.122.4.487
Mangione CM, Phillips RS, Lawrence MG, Seddon JM, Orav EJ, Goldman L (1994) Improved visual function and attenuation of declines in health-related quality of life after cataract extraction. Arch Ophthalmol 112(11):1419–1425. https://doi.org/10.1001/archopht.1994.01090230033017
McGwin G Jr, Scilley K, Brown J, Owsley C (2003) Impact of cataract surgery on self-reported visual difficulties: comparison with a no-surgery reference group. J Cataract Refract Surg 29(5):941–948. https://doi.org/10.1016/s0886-3350(02)01846-1
Sandoval HP, Fernandez de Castro LE, Vroman DT, Solomon KD (2007) A review of the use of ketorolac tromethamine 0.4% in the treatment of post-surgical inflammation following cataract and refractive surgery. Clin Ophthalmol 1(4):367–371
Kim SJ, Flach AJ, Jampol LM (2010) Nonsteroidal anti-inflammatory drugs in ophthalmology. Surv Ophthalmol 55(2):108–133. https://doi.org/10.1016/j.survophthal.2009.07.005
O'Brien TP (2005) Emerging guidelines for use of NSAID therapy to optimize cataract surgery patient care. Curr Med Res Opin 21(7):1131–1137. https://doi.org/10.1185/030079905X50651
Wolf EJ, Braunstein A, Shih C, Braunstein RE (2007) Incidence of visually significant pseudophakic macular edema after uneventful phacoemulsification in patients treated with nepafenac. J Cataract Refract Surg 33(9):1546–1549. https://doi.org/10.1016/j.jcrs.2007.05.018
Tugal-Tutkun I, Herbort CP (2010) Laser flare photometry: a noninvasive, objective, and quantitative method to measure intraocular inflammation. Int Ophthalmol 30(5):453–464. https://doi.org/10.1007/s10792-009-9310-2
Isik MU, Yalcindag N (2020) Comparison of spectral domain optical coherence tomography (SD OCT) Findings with Laser Flare Photometry (LFP) Measurements in Behcet's Uveitis. Ocul Immunol Inflamm 28(2):194–199. https://doi.org/10.1080/09273948.2018.1552976
Ahuja M, Dhake AS, Sharma SK, Majumdar DK (2008) Topical ocular delivery of NSAIDs. AAPS J 10(2):229–241. https://doi.org/10.1208/s12248-008-9024-9
Colin J (2007) The role of NSAIDs in the management of postoperative ophthalmic inflammation. Drugs 67(9):1291–1308. https://doi.org/10.2165/00003495-200767090-00004
Schalnus R (2003) Topical nonsteroidal anti-inflammatory therapy in ophthalmology. Ophthalmologica 217(2):89–98. https://doi.org/10.1159/000068563
Abel R Jr, Abel AD (1997) Perioperative antibiotic, steroid, and nonsteroidal anti-inflammatory agents in cataract intraocular lens surgery. Curr Opin Ophthalmol 8(1):29–32
Tzelikis PF, Vieira M, Hida WT, Motta AF, Nakano CT, Nakano EM, Alves MR (2015) Comparison of ketorolac 0.4% and nepafenac 0.1% for the prevention of cystoid macular oedema after phacoemulsification: prospective placebo-controlled randomised study. Br J Ophthalmol 99(5):654–658. https://doi.org/10.1136/bjophthalmol-2014-305803
Lane SS (2006) Nepafenac: a unique nonsteroidal prodrug. Int Ophthalmol Clin 46(4):13–20. https://doi.org/10.1097/01.iio.0000212129.53019.49
Wilson DJ, Schutte SM, Abel SR (2015) Comparing the efficacy of ophthalmic NSAIDs in common indications: a literature review to support cost-effective prescribing. Ann Pharmacother 49(6):727–734. https://doi.org/10.1177/1060028015574593
Lane SS, Modi SS, Lehmann RP, Holland EJ (2007) Nepafenac ophthalmic suspension 0.1% for the prevention and treatment of ocular inflammation associated with cataract surgery. J Cataract Refract Surg 33(1):53–58. https://doi.org/10.1016/j.jcrs.2006.08.043
Nardi M, Lobo C, Bereczki A, Cano J, Zagato E, Potts S, Sullins G, Notivol R (2007) Analgesic and anti-inflammatory effectiveness of nepafenac 0.1% for cataract surgery. Clin Ophthalmol 1(4):527–533
Zhao X, Xia S, Wang E, Chen Y (2017) Comparison of the efficacy and patients' tolerability of Nepafenac and Ketorolac in the treatment of ocular inflammation following cataract surgery: A meta-analysis of randomized controlled trials. PLoS ONE 12(3):e0173254. https://doi.org/10.1371/journal.pone.0173254
Cagini C, Pellegrino A, Cerquaglia A, Iaccheri B, Lupidi M, Fiore T (2020) Comparison of the effect of diclofenac 0.1% and nepafenac 0.1% on aqueous flare in patients undergoing cataract surgery: a prospective randomized study. Curr Eye Res. https://doi.org/10.1080/02713683.2020.1725061
Duan P, Liu Y, Li J (2017) The comparative efficacy and safety of topical non-steroidal anti-inflammatory drugs for the treatment of anterior chamber inflammation after cataract surgery: a systematic review and network meta-analysis. Graefes Arch Clin Exp Ophthalmol 255(4):639–649. https://doi.org/10.1007/s00417-017-3599-8
Kessel L, Tendal B, Jorgensen KJ, Erngaard D, Flesner P, Andresen JL, Hjortdal J (2014) Post-cataract prevention of inflammation and macular edema by steroid and nonsteroidal anti-inflammatory eye drops: a systematic review. Ophthalmology 121(10):1915–1924. https://doi.org/10.1016/j.ophtha.2014.04.035
Ray S, D'Amico DJ (2002) Pseudophakic cystoid macular edema. Semin Ophthalmol 17(3–4):167–180
Dave P, Shah K, Ramchandani B, Jain R (2014) Effect of nepafenac eye drops on intraocular pressure: a randomized prospective study. Am J Ophthalmol 157(3):735–738. https://doi.org/10.1016/j.ajo.2013.12.015
Acknowledgements
There are no sources of support including sponsorship (e.g., university, charity, commercial organization) and sources of material (e.g., novel drugs) not available commercially.
Funding
The authors did not receive any financial support from any public or private sources. The authors have no financial or proprietary interest in a product, method, or material described herein.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
There is no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The article has been not presented in a meeting.
Rights and permissions
About this article
Cite this article
Işık, M.U., Yalçındağ, N.F. Comparison of the efficacy of nepafenac 0.1% in quiescent Behçet’s uveitis and non-uveitic healthy patients after phacoemulsification surgery. Int Ophthalmol 40, 2345–2351 (2020). https://doi.org/10.1007/s10792-020-01419-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01419-z