Abstract
Purpose
The aim of this study was to evaluate the aqueous outflow system through channelography with fluorescein during non-penetrating glaucoma surgery (canaloplasty or phacocanaloplasty) and find correlations with preoperative and postoperative intraocular pressure (IOP).
Methods
Thirty-six patients (40 eyes) who had channelography while undergoing non-penetrating glaucoma surgery were included in this prospective study. Several parameters assessed during the channelography included: diffuse and superficial scleral staining, the number of visible superficial connections to collectors, trabecular permeability and number of micro-ruptures of the trabecular meshwork. IOP, the best-corrected visual acuity, the number of glaucoma medications was recorded at 1 day, 7 days, 3 months and 6 months after the operation.
Results
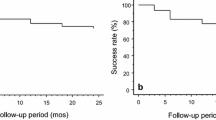
The change in IOP at 6 months from baseline significantly correlated with the number of visible superficial connections to collectors (r = 0.4, p = 0.021). Eyes with canaloplasty showed a mean baseline IOP of 19.4 (4.9) mmHg and mean glaucoma medication usage of 2.9 (1.0), which decreased to 13.2 (3.1) mmHg with 0.3 (0.8) medications, respectively, at 6 months postoperatively (p < 0.001). Eyes with phacocanaloplasty surgery showed a mean baseline IOP of 28.2 (9.6) mmHg with 2.6 (0.9) mean drugs, which decreased to IOP of 12.8 (3.4) mmHg with 0.5 (0.8) medications at 6 months (p < 0.001).
Conclusion
A larger number of defined visible superficial connections to collectors after injection of fluorescein into SC is related to a more pronounced IOP decrease after non-penetrating glaucoma surgery.


Similar content being viewed by others
References
Grieshaber MC (2012) Ab externo Schlemm’s canal surgery: viscocanalostomy and canaloplasty. Dev Ophthalmol 50:109–124
Baikstiene Daiva Paulaviciute, Vaiciuliene Renata, Jasinskas Vytautas, Januleviciene Ingrida (2016) Evaluation of outflow structures in vivo after the phacocanaloplasty. J Ophthalmol. doi:10.1155/2016/4519846
Hong J, Xu J, Wei A, Wen W, Chen J, Yu X et al (2013) Spectral-domain optical coherence tomographic assessment of Schlemm’s canal in Chinese subjects with primary open-angle glaucoma. Ophthalmology 120(4):709–715
Irshad FA, Mayfield MS, Zurakowski D, Ayyala RS (2010) Variation in Schlemm’s canal diameter and location by ultrasound biomicroscopy. Ophthalmology 117(5):916–920
Grieshaber MC, Pienaar A, Olivier J, Stegmann R (2010) Clinical evaluation of the aqueous outflow system in primary open-angle glaucoma for canaloplasty. Invest Ophthalmol Vis Sci 51(3):1498–1504
Grieshaber MC, Pienaar A, Olivier J, Stegmann R (2009) Channelography: imaging of the aqueous outflow pathway with flexible microcatheter and fluorescein in canaloplasty. Klin Monbl Augenheilkd 226(4):245–248
Grieshaber MC (2015) Channelography and mechanism of action in canaloplasty. Ophthalmologe 112(4):319–324
Smit BA, Johnstone MA (2002) Effects of viscoelastic injection into Schlemm’s canal in primate and human eyes: potential relevance to viscocanalostomy. Ophthalmology 109(4):786–792
Johnson DH, Johnson M (2002) Glaucoma surgery and aqueous outflow: how does nonpenetrating glaucoma surgery work? Arch Ophthalmol 120(1):67–70
Shingleton B, Tetz M, Körber N (2008) Circumferential viscodilation and tensioning of Schlemm canal (canaloplasty) with temporal clear corneal phacoemulsification cataract surgery for open-angle glaucoma and visually significant cataract; one-year results. J Cataract Refract Surg 34:433–440
Bull H, von Wolff K, Körber N, Tetz M (2011) Three-year canaloplasty outcomes for the treatment of open-angle glaucoma: European study results. Graefes Arch Clin Exp Ophthalmol 249:1537–1545
Wishart MS, Shergill T, Porooshani H (2002) Viscocanalostomy and phacoviscocanalostomy: long-term results. J Cataract Refract Surg 28(5):745–751
Lewis RA, von Wolff K, Tetz M, Koerber N, Kearney JR, Shingleton BJ, Samuelson TW (2011) Canaloplasty: three-year results of circumferential viscodilation and tensioning of Schlemm canal using a microcatheter to treat open-angle glaucoma. J Cataract Refract Surg 37:682–690
Peckar CO, Körber K (2008) Canaloplasty for open angle glaucoma: a three years critical evaluation and comparison with viscocanalostomy. Spektrum Augenheilkunde. doi:10.1007/s00717-008-0272-y
Shrivastava A, Singh K (2010) The effect of cataract extraction on intraocular pressure. Curr Opin Ophthalmol 21(2):118–122
Iancu R, Corbu C (2014) Intraocular pressure after phacoemulsification in patients with uncontrolled primary open angle glaucoma. J Med Life 7:11–16
Mathalone N, Hyams M, Neiman S, Buckman G, Hod Y, Geyer O (2005) Long-term intraocular pressure control after clear corneal phacoemulsification in glaucoma patients. J Cataract Refract Surg 31:479–483
Jamil AZ, Iqbal K, Ur Rahman F, Mirza KA (2011) Effect of phacoemulsification on intraocular pressure. J Coll Physicians Surg Pak 21:347–350
Shingleton BJ, Pasternack JJ, Hung JW, O’Donoghue MW (2006) Three and five year changes in intraocular pressures after clear corneal phacoemulsification in open angle glaucoma patients, glaucoma suspects, and normal patients. J Glaucoma 15:494–498
Levkovitch-Verbin H, Habot-Wilner Z, Burla N, Melamed S, Goldenfeld M, Bar-Sela SM, Sachs D (2008) Intraocular pressure elevation within the first 24 hours after cataract surgery in patients with glaucoma or exfoliation syndrome. Ophthalmology 115(1):104–108
Lin YP, Dg Zurakowski, Ayyalia RS (2007) Surgical outcomes of traditional limbal-based versus fornix-based trabeculectomy with corneal valve. Ohthalmic Surg Laser Imaging 38:471–477
Fontana H, Nouri-Mahdavi K, Lumba J, Ralli M, Caprioli J (2006) Trabeculectomy with mitomycin C: outcomes and risk factors for failure in phakic open-angle glaucoma. Ophthalmology 113:930–936
Ayyala RS, Chaudhry AL, Okogbaa CB, Zurakowski D (2011) Comparison of surgical outcomes between canaloplasty and trabeculectomy at 12 months’ follow-up. Ophthalmology 118:2427–2433
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Vaiciuliene, R., Körber, N. & Jasinskas, V. Clinical evaluation of aqueous outflow system in vivo and correlation with intraocular pressure before and after non-penetrating glaucoma surgery. Int Ophthalmol 38, 2141–2147 (2018). https://doi.org/10.1007/s10792-017-0715-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-017-0715-z