Abstract
Purpose
This study proves the possibility of targeted use of the nonsteroidal anti-inflammatory drug lornoxicam to prevent the development of proliferative vitreoretinopathy (PVR). Triamcinolone acetonide (TA) was selected as a reference substance.
Methods
Wistar rats (N = 400) were used. PVR was modeled by intravitreal injection of dispase or concanavalin A. Lornoxicam or TA intravitreal administration was performed 20 min later. On the second and the third day, drugs were administrated systemic. Enucleation was performed on the first, third, seventh and 42nd or 56th day of the experiment.
Results
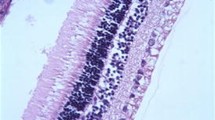
Pro-inflammatory substances led to the development of sub- and epiretinal membranes. Lornoxicam decreased the incidence of membrane formation by 43 and 31% in dispase and concanavalin models, respectively. Membranes, formed during its use, were smaller and contained less fibrotic components. At the end of the experiment, the thickness of retinal and choroidal layers among the animals which had received the therapy was the same as the thickness of the retina and choroid of intact rats. Lornoxicam administration normalized the cyclooxygenases (COXs) expression in the retina and the choroid at the early stages of the experiment. TA application was less effective in both models.
Conclusions
COXs blocking during the development of PVR, overwhelming inflammation in the eye and reducing its consequences, is proved to be a much more effective and safe influence than the suppression of the entire cascade of arachidonic acid metabolism. Lornoxicam did not only improve the condition of the retina and the choroid but also significantly reduced the frequency of membrane formation.








Similar content being viewed by others
References
Acar N, Kapran Z, Altan T, Unver YB, Pasaoglu E (2010) Pars plana vitrectomy with and without triamcinolone acetonide assistance in pseudophakic retinal detachment complicated with proliferative vitreoretinopathy. Jpn J Ophthalmol 54:331–337
Caspi RR (2010) A look at autoimmunity and inflammation in the eye. J Clin Invest 120:3073–3083
Charteris DG, Sethi CS, Lewis GP, Fisher SK (2002) Proliferative vitreoretinopathy—developments in adjunctive treatment and retinal pathology. Eye (Lond) 16:369–374
Chen W, Chen H, Hou P, Fok A, Hu Y, Lam D (2011) Midterm results of low-dose intravitreal triamcinolone as adjunctive treatment for proliferative vitreoretinopathy. Retina 31:1137–1142
Chennamaneni SR, Bohner A, Bernhisel A, Ambati BK (2014) Pharmacokinetics and efficacy of Bioerodible Dexamethasone implant in Concanavalin A-induced uveitic cataract model. Pharm Res 31:3179–3190
de Silva DJ, Kwan A, Bunce C, Bainbridge J (2008) Predicting visual outcome following retinectomy for retinal detachment. Br J Ophthalmol 92:954–958
de Souza CF, Kalloniatis M, Polkinghorne PJ, McGhee CNJ, Acosta ML (2012) Functional and anatomical remodeling in human retinal detachment. Exp Eye Res 97:73–89
Deng W, Montero AJ, Wu KK (2007) Interferon-γ suppresses cyclooxygenase-2 promoter activity by inhibiting C-Jun and C/EBPβ binding. Arterioscler Thromb Vasc Biol 27:1752–1759
Diakonis VF, Tsourdou A, Tzatzarakis MN, Tsika C, Charisis S, Naoumidi I, Plainis S, Tsilimbaris MK (2013) Evaluation of vitreous clearance and potential retinal toxicity of intravitreal lornoxicam (xefo). J Ocul Pharmacol Ther 29:627–632
Dodwell DG, Krimmel DA, Fiebre CM (2015) Sterile endophthalmitis rates and particle size analyses of different formulations of triamcinolone acetonide. Clin Ophthalmol 9:1033–1040
Er H, Uzmez E, Do N, Cumhurcu ANT (1999) The anti–inflammatory effects of NG–nitro l-arginine (L-NAME) and steroid in Concanavalin A—induced uveitis. Tr J Med Sci 29:233–236
Frenzel EM, Neely KA, Walsh AW, Cameron JD, Gregerson DS (1998) A new model of proliferative vitreoretinopathy. Invest Ophthalmol Vis Sci 39:2157–2164
Gavrilova S, Lipina T, Zagidullin T, Fominykh E, Golubeva A, Varenik E, Parnes E, Semenov P (2008) Protective effect of lornoxicam on development of myocardial infarction in rats under conditions of ischemia and ischemia-reperfusion. Kardiologiia 48:42–48
Gronert K (2010) Resolution, the grail for healthy ocular inflammation. Exp Eye Res 91:478–485
Gwon A, Mantras C, Gruber L, Cunanan C (1993) Concanavalin A-induced posterior subcapsular cataract: a new model of cataractogenesis. Invest Ophthalmol Vis Sci 34:3483–3488
Janse van Rensburg E (2013) Astute and safe use of topical ocular corticosteroids in general practice: practical guidelines. CME 31:127–129
Johnsen EO, Frøen RC, Albert R, Omdal BK, Sarang Z, Berta A, Nicolaissen B, Petrovski G, Moe MC (2012) Activation of neural progenitor cells in human eyes with proliferative vitreoretinopathy. Exp Eye Res 98:28–36
Kapin MA, Yanni JM, Brady MT et al (2003) Inflammation-mediated retinal edema in the rabbit is inhibited by topical nepafenac. Inflammation 27:281–291
Kon CH, Asaria RH, Occleston NL, Khaw PT, Aylward GW (2000) Risk factors for proliferative vitreoretinopathy after primary vitrectomy: a prospective study. Br J Ophthalmol 84:506–511
Langenbach R, Morham SG, Tiano HF et al (1995) Prostaglandin synthase 1 gene disruption in mice reduces arachidonic acid-induced inflammation and indomethacin-induced gastric ulceration. Cell 83:483–492
Morham SG, Langenbach R, Loftin CD et al (1995) Prostaglandin synthase 2 gene disruption causes severe renal pathology in the mouse. Cell 83:473–482
Nagata M, Matsumura T (1986) Action of the bacterial neutral protease, dispase, on cultured cells and its application to fluid suspension culture with a review on biomedical application of this protease. Jpn J Exp Med 56:297–307
Nakazawa T, Matsubara A, Noda K et al (2006) Characterization of cytokine responses to retinal detachment in rats. Mol Vis 12:867–878
Nicholson BP, Zhou M, Rostamizadeh M et al (2014) Epidemiology of epiretinal membrane in a large cohort of patients with uveitis. Ophthalmology 121:2393–2398
Nishijima K, Ng Y-S, Zhong L et al (2007) Vascular endothelial growth factor-A is a survival factor for retinal neurons and a critical neuroprotectant during the adaptive response to ischemic injury. Am J Pathol 171:53–67
Oberstein S, Byun J, Herrera D (2011) Cell proliferation in human epiretinal membranes: characterization of cell types and correlation with disease condition and duration. Mol Vis 17:1794–1805
Pastor J (1998) Proliferative vitreoretinopathy: an overview. Surv Ophthalmol 43:3–18
Pastor JC, Rojas J, Pastor-Idoate S, Di Lauro S, Gonzalez-Buendia L, Delgado-Tirado S (2016) Proliferative vitreoretinopathy: a new concept of disease pathogenesis and practical consequences. Prog Retin Eye Res 51:125–155
Prasad Byrav DS, Medhi B, Prakash A, Patyar S, Wadhwa S (2009) Lornoxicam: a newer NSAID. Indian J Phys Med Rehabil 20:27–31
Prete M, Dammacco R, Fatone CM, Racanelli V (2015) Autoimmune uveitis: clinical, pathogenetic, and therapeutic features. Clin Exp Med 16:125–136
Radi ZA (2012) Comparative pathophysiology and toxicology of cyclooxygenases. Wiley, Hoboken
Radi ZA, Render JA (2008) The pathophysiologic role of cyclooxygenases in the eye. J Ocul Pharmacol Ther 24:141–151
Rang HP, Dale MM, Ritter JM, Flower RJ (2007) Rang & Dale’s pharmacology, 6th edn. Churchill Livigstone, Edinburgh
Tikhonovich M, Lyskin P, Ioyleva E, Gavrilova S (2016) Expression of cyclooxygenases and trophic and growth factors in epiretinal membranes at late stages of proliferative vitreoretinopathy. Graefe’s Arch Clin Exp Ophthalmol 254:2277–2279
Valamanesh F, Berdugo M, Sennlaub F et al (2009) Effects of triamcinolone acetonide on vessels of the posterior segment of the eye. Mol Vis 15:2634–2648
Valamanesh F, Torriglia A, Savoldelli M, Gandolphe C, Jeanny J, BenEzra D, Behar-Cohen F (2007) Glucocorticoids induce retinal toxicity through mechanisms mainly associated with paraptosis. Mol Vis 13:1746–1757
Valeria CantÓ Soler M, Gallo JE, Dodds RA, Suburo AM (2002) A mouse model of proliferative vitreoretinopathy induced by dispase. Exp Eye Res 75:491–504
Vichai V, Suyarnsesthakorn C, Pittayakhajonwut D, Sriklung K, Kirtikara K (2005) Positive feedback regulation of COX-2 expression by prostaglandin metabolites. Inflamm Res 54:163–172
Wang H, Liu M, Weng S et al (2012) Immune mechanisms of Concanavalin A model of autoimmune hepatitis. World J Gastroenterol 18:119–125
Yang L (2004) Preventing retinal detachment-associated photoreceptor cell loss in Bax-deficient mice. Invest Ophthalmol Vis Sci 45:648–654
Yu S, Damico FM, Viola F, Amico DJD, Young LH (2006) Retinal toxicity of intravitreal triamcinolone acetonide. Retina 26:531–536
Acknowledgements
We thank A.A. Dementyeva and A.A. Kibitov for help in obtaining some of the immmunohistochemical results.
Funding
This work was supported by Russian Foundation for Basic Research grant (No. 14-04-01318-A). The funding organization had no role in the design or conduct of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Tikhonovich M. has a patent RU2558991 licensed to Lomonosov Moscow State University, and a patent RU2458656 licensed to The S.N. Fyodorov “Eye microsurgery” Federal State Institution. Erdiakov A. has a patent RU2563368 licensed to Lomonosov Moscow State University. Gavrilova S. has a patent RU2563368 licensed to Lomonosov Moscow State University, and a patent RU2558991 licensed to Lomonosov Moscow State University.
Ethical approval
All applicable international, national and/or institutional guidelines for the care and use of animals were followed.
Rights and permissions
About this article
Cite this article
Tikhonovich, M.V., Erdiakov, A.K. & Gavrilova, S.A. Nonsteroid anti-inflammatory therapy suppresses the development of proliferative vitreoretinopathy more effectively than a steroid one. Int Ophthalmol 38, 1365–1378 (2018). https://doi.org/10.1007/s10792-017-0594-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-017-0594-3