Abstract
Purpose
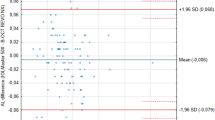
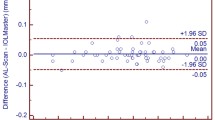
The purpose of the study was to assess the reproducibility of ocular biometry using the IOLMaster-700 in a healthy population.
Methods
This is a prospective, cross-sectional, observational reproducibility study. Ocular biometry was performed three times on each of 45 studied eyes. Flattest meridian (Kf) and the steepest meridian (Ks), central corneal thickness, axial length, anterior chamber depth, aqueous depth, lens thickness, and white-to-white distances were recorded. Reproducibility was evaluated using the coefficient of variation (CV), the within subject standard deviation, and the intraclass correlation coefficient (ICC).
Results
There was a high reproducibility in all parameters; CV was between 0.3 and 1 %, and the ICC was higher than 0.87 in all measurements.
Conclusions
IOLMaster-700 showed high reproducibility for ocular biometry.
Similar content being viewed by others
References
Feng YF, Wang DD, Zhao YE, Li JH, Savini G, Huang JH (2013) Surgical management of malignant glaucoma with white cataract in nanophthalmos. J Cataract Refract Surg 39(11):1774–1777. doi:10.1016/j.jcrs.2013.08.016
Jung KI, Yang JW, Lee YC, Kim SY (2012) Cataract surgery in eyes with nanophthalmos and relative anterior microphthalmos. Am J Ophthalmol 153(6):1161–1168. doi:10.1016/j.ajo.2011.12.006
Kaswin G, Rousseau A, Mgarrech M, Barreau E, Labetoulle M (2014) Biometry and intraocular lens power calculation results with a new optical biometry device: comparison with the gold standard. J Cataract Refract Surg 40(4):593–600. doi:10.1016/j.jcrs.2013.09.015
Srivannaboon S, Chirapapaisan C, Chonpimai P, Koodkaew S (2014) Comparison of ocular biometry and intraocular lens power using a new biometer and a standard biometer. J Cataract Refract Surg 40(5):709–715
Shen P, Zheng Y, Ding X, Liu B, Congdon N, Morgan I, He M (2013) Biometric measurements in highly myopic eyes. J Cataract Refract Surg 39(2):180–187
Rončević MB, Bušić M, Čima I, Elabjer BK, Bosnar D, Miletić D (2011) Comparison of optical low-coherence reflectometry and applanation ultrasound biometry on intraocular lens power calculation. Graefe’s Arch Clin Exp Ophthalmol 249(1):69–75
Nakhli FR (2014) Comparison of optical biometry and applanation ultrasound measurements of the axial length of the eye. Saudi J Ophthalmol 28(4):287–291
Alio JL, Grzybowski A, El Aswad A, Romaniuk D (2014) Refractive lens exchange. Surv Ophthalmol 59(6):579–598. doi:10.1016/j.survophthal.2014.04.004
Hua X, Yuan XY, Song H, Tang X (2013) Long-term results of clear lens extraction combined with piggyback intraocular lens implantation to correct high hyperopia. Int J Ophthalmol 6(5):650–655. doi:10.3980/j.issn.2222-3959.2013.05.18
Moyal L, Abrieu-Lacaille M, Bonnel S, Sendon D, de Rivoyre B, Berguiga M, Rambaud C, Froussart-Maille F, Rigal-Sastourne JC (2015) Comparison of two different surgical treatments of presbyopia for hyperopic patients over 55 years old: Presbylasik (Supracor) and Prelex (presbyopic lens exchange). J Fr Ophtalmol 38(4):306–315. doi:10.1016/j.jfo.2014.10.010
Brown RH, Zhong L, Lynch MG (2014) Clear lens extraction as treatment for uncontrolled primary angle-closure glaucoma. J Cataract Refract Surg 5(40):840–841
Man X, Chan NC, Baig N, Kwong YY, Leung DY, Li FC, Tham CC (2015) Anatomical effects of clear lens extraction by phacoemulsification versus trabeculectomy on anterior chamber drainage angle in primary angle-closure glaucoma (PACG) patients. Graefe’s Arch Clin Exp Ophthalmol 253(5):773–778
Mittal V, Mittal R, Maheshwari R (2014) Combined endothelial keratoplasty and clear lens extraction for corneal decompensation in irido-corneal endothelial syndrome. Indian J Ophthalmol 62(5):651–653. doi:10.4103/0301-4738.118435
Rao A (2013) Clear lens extraction in plateau iris with bilateral acute angle closure in young. J Glaucoma 22(9):e31–e32. doi:10.1097/IJG.0b013e31825c10c4
Taketani F, Matuura T, Yukawa E, Hara Y (2004) Influence of intraocular lens tilt and decentration on wavefront aberrations. J Cataract Refract Surg 30(10):2158–2162. doi:10.1016/j.jcrs.2004.02.072
Oshika T, Sugita G, Miyata K, Tokunaga T, Samejima T, Okamoto C, Ishii Y (2007) Influence of tilt and decentration of scleral-sutured intraocular lens on ocular higher-order wavefront aberration. Br J Ophthalmol 91(2):185–188. doi:10.1136/bjo.2006.099945
Korynta J, Bok J, Cendelin J, Michalova K (1999) Computer modeling of visual impairment caused by intraocular lens misalignment. J Cataract Refract Surg 25(1):100–105
Olsen T, Hoffmann P (2014) C constant: new concept for ray tracing-assisted intraocular lens power calculation. J Cataract Refract Surg 40(5):764–773. doi:10.1016/j.jcrs.2013.10.037
Al-Refaie A, Bata N (2010) Evaluating measurement and process capabilities by GR&R with four quality measures. Measurement 43(6):842–851
Senol S (2004) Measurement system analysis using designed experiments with minimum α–β Risks and n. Measurement 36(2):131–141
Nongpiur ME, He M, Amerasinghe N, Friedman DS, Tay WT, Baskaran M, Smith SD, Wong TY, Aung T (2011) Lens vault, thickness, and position in Chinese subjects with angle closure. Ophthalmology 118(3):474–479. doi:10.1016/j.ophtha.2010.07.025
Grulkowski I, Liu JJ, Zhang JY, Potsaid B, Jayaraman V, Cable AE, Duker JS, Fujimoto JG (2013) Reproducibility of a long-range swept-source optical coherence tomography ocular biometry system and comparison with clinical biometers. Ophthalmology 120(11):2184–2190. doi:10.1016/j.ophtha.2013.04.007
Lopez de la Fuente C, Sanchez-Cano A, Segura F, Pinilla I (2014) Comparison of anterior segment measurements obtained by three different devices in healthy eyes. BioMed Res Int 2014
Gonvers M, Bornet C, Othenin-Girard P (2003) Implantable contact lens for moderate to high myopia: relationship of vaulting to cataract formation. J Cataract Refract Surg 29(5):918–924
Zaldivar R, Davidorf JM, Oscherow S (1998) Posterior chamber phakic intraocular lens for myopia of -8 to -19 diopters. J Refract Surg 14(3):294–305
Alfonso JF, Lisa C, Palacios A, Fernandes P, Gonzalez-Meijome JM, Montes-Mico R (2009) Objective vs subjective vault measurement after myopic implantable collamer lens implantation. Am J Ophthalmol 147(6):978–983. doi:10.1016/j.ajo.2009.01.006
Martin R, Ortiz S, Rio-Cristobal A (2013) White-to-white corneal diameter differences in moderately and highly myopic eyes: partial coherence interferometry versus scanning-slit topography. J Cataract Refract Surg 39(4):585–589. doi:10.1016/j.jcrs.2012.11.021
De la Parra-Colín P, Garza-León M, Barrientos-Gutierrez T (2014) Repeatability and comparability of anterior segment biometry obtained by the Sirius and the Pentacam analyzers. Int Ophthalmol 34(1):27–33
Bao F, Wang Q, Cheng S, Savini G, Lu W, Feng Y, Yu Y, Huang J (2014) Comparison and evaluation of central corneal thickness using 2 new noncontact specular microscopes and conventional pachymetry devices. Cornea 33(6):576–581
Huang J, Liao N, Savini G, Li Y, Bao F, Yu Y, Yu A, Wang Q (2015) Measurement of central corneal thickness with optical low-coherence reflectometry and ultrasound pachymetry in normal and post-femtosecond laser in situ keratomileusis eyes. Cornea 34(2):204–208. doi:10.1097/ICO.0000000000000329
Murdoch IE, Morris SS, Cousens SN (1998) People and eyes: statistical approaches in ophthalmology. Br J Ophthalmol 82(8):971–973
Karakosta A, Vassilaki M, Plainis S, Elfadl NH, Tsilimbaris M, Moschandreas J (2012) Choice of analytic approach for eye-specific outcomes: one eye or two? Am J Ophthalmol 153(3):571–579. doi:10.1016/j.ajo.2011.08.032
Acknowledgements
We would like to thank the engineers Roberto Reza Nuñez and Manuel Reza Garza for their help in the statistical analysis done in this study.
Funding
The author received no funding for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author has no financial interest in any of the devices used in this study.
Rights and permissions
About this article
Cite this article
Garza-Leon, M., Fuentes-de la Fuente, H.A. & García-Treviño, A.V. Repeatability of ocular biometry with IOLMaster 700 in subjects with clear lens. Int Ophthalmol 37, 1133–1138 (2017). https://doi.org/10.1007/s10792-016-0380-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-016-0380-7