Abstract
Background
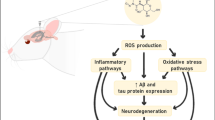
Alzheimer’s disease (AD) is a prominent cause of dementia, resulting in neurodegeneration and memory impairment. This condition imposes a considerable public health burden on both patients and their families due to the patients’ functional impairments as well as the psychological and financial constraints. It has been well demonstrated that its aetiology involves proteinopathy, mitochondriopathies, and enhanced reactive oxygen species (ROS) generation, which are some of the key features of AD brains that further result in oxidative stress, excitotoxicity, autophagy, and mitochondrial dysfunction.
Objective
The current investigation was created with the aim of elucidating the neurological defence mechanism of trans,trans-Farnesol (TF) against intracerebroventricular-streptozotocin (ICV-STZ)-induced Alzheimer-like symptoms and related pathologies in rodents.
Materials and methods
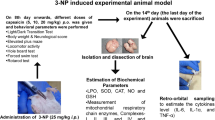
The current investigation involved male SD rats receiving TF (25–100 mg/kg, per oral) consecutively for 21 days in ICV-STZ-treated animals. An in silico study was carried out to explore the possible interaction between TF and NADH dehydrogenase and succinate dehydrogenase. Further, various behavioural (Morris water maze and novel object recognition test), biochemical (oxidants and anti-oxidant markers), activities of mitochondrial enzyme complexes and acetylcholinesterase (AChE), pro-inflammatory (tumor necrosis factor-alpha; TNF-α) levels, and histopathological studies were evaluated in specific brain regions.
Results
Rats administered ICV-STZ followed by treatment with TF (25, 50, and 100 mg/kg) for 21 days had significantly better mental performance (reduced escape latency to access platform, extended time spent in target quadrant, and improved differential index) in the Morris water maze test and new object recognition test models when compared to control (ICV-STZ)-treated groups. Further, TF treatment significantly restored redox proportion, anti-oxidant levels, regained mitochondrial capacities, attenuated altered AChE action, levels of TNF-α, and histopathological alterations in certain brain regions in comparison with control. In in silico analysis, TF caused greater interaction with NADH dehydrogenase and succinate dehydrogenase.
Conclusion
The current work demonstrates the neuroprotective ability of TF in an experimental model with AD-like pathologies. The study further suggests that the neuroprotective impacts of TF may be related to its effects on TNF-α levels, oxidative stress pathways, and mitochondrial complex capabilities.























Similar content being viewed by others
Data availability
Data will be made available on request.
Abbreviations
- 5XTC:
-
Cryo-EM structure of human respiratory complex I transmembrane arm
- 4YTP:
-
Crystal structure of porcine heart mitochondrial complex II bound with N-[(4-tert-butylphenyl)methyl]-2-(trifluoromethyl)benzamide
- AChE:
-
Acetylcholinesterase
- ACSF:
-
Artificial cerebrospinal fluid
- AD:
-
Alzheimer’s disease
- ANOVA:
-
Analysis of variance
- APP:
-
Amyloid-protein precursor
- ATP:
-
Adenosine triphosphate
- BSA:
-
Bovine serum albumin
- Bw:
-
Body weight
- CPCSEA:
-
Committee for purpose of control and supervision of experiments on animals
- DCFH-DA:
-
2′, 7′ -Dichlorofluorescin diacetate
- DG:
-
Dentate gyrus
- DPX:
-
Distrene plasticizer xylene
- EGTA:
-
Ethylene glycol-bis(β-aminoethyl ether)-N,N,N′,N′-tetraacetic acid
- ELISA:
-
Enzyme-linked immunosorbent assay
- ETC:
-
Electron transport chain
- FAD:
-
Familial Alzheimer’s disease
- Gala:
-
Galantamine
- GSH:
-
Reduced glutathione
- H2O2:
-
Hydrogen peroxide
- HEPES:
-
(4-(2-Hydroxyethyl)-1-piperazineethanesulfonic acid)
- IAEC:
-
Institutional Animal Ethics Committee
- ICV-STZ:
-
Intracerebroventricular-streptozotocin
- IL-6:
-
Interleukin-6
- KOH:
-
Potassium hydroxide solution
- LPO:
-
Lipid peroxidation
- MDA:
-
Malondialdehyde
- mtDNA:
-
Mitochondrial DNA
- MTT:
-
3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyl-H-tetrazolium bromide
- MWM:
-
Morris water maze
- NADH:
-
Nicotinamide adenine dinucleotide
- NOR or NORT:
-
Novel object recognition test
- OH•:
-
Hydroxyl radicals
- ONOO− :
-
Peroxynitrite
- OXPHOS:
-
Oxidative phosphorylation
- PLIP:
-
Protein–Ligand Interaction Profiler
- PMS:
-
Post mitochondrial supernatant
- PNS:
-
Post nuclear supernatant
- PS 1 or 2:
-
Presenilin 1 or 2
- RNS:
-
Reactive nitrogen species
- ROS:
-
Reactive oxygen species
- SAD:
-
Sporadic Alzheimer’s disease
- SD:
-
Sprague–Dawley
- SDH:
-
Succinate dehydrogenase
- SEM:
-
Standard error of the mean
- SOD:
-
Superoxide dismutase
- TBA:
-
Thiobarbituric acid
- TBARS:
-
Thiobarbituric-acid reactive substance
- TF:
-
Trans,trans-Farnesol
- TNF-α:
-
Tumor necrosis factor- alpha
- TSTQ:
-
Time spent in target quadrant
- UV–Vis:
-
Ultraviolet–visible
References
Abukhalil MH, Hussein OE, Bin-Jumah M, Saghir SAM, Germoush MO, Elgebaly HA, Mosa NM, Hamad I, Qarmush MM, Hassanein EM, Kamel EM, Hernandez-Bautista R, Mahmoud AM (2020) Farnesol attenuates oxidative stress and liver injury and modulates fatty acid synthase and acetyl-CoA carboxylase in high cholesterol-fed rats. Environ Sci Pollut Res Int 27(24):30118–30132. https://doi.org/10.1007/s11356-020-09296-w
Agrawal I, Jha S (2020) Mitochondrial Dysfunction and Alzheimer’s Disease: Role of Microglia. Front Aging Neurosci 12:252. https://doi.org/10.3389/fnagi.2020.00252
Akhtar A, Dhaliwal J, Sah SP (2021) 7,8-Dihydroxyflavone improves cognitive functions in ICV-STZ rat model of sporadic Alzheimer’s disease by reversing oxidative stress, mitochondrial dysfunction, and insulin resistance. Psychopharmacology 238:1991–2009. https://doi.org/10.1007/s00213-021-05826-7
Antunes M, Biala G (2012) The novel object recognition memory: neurobiology, test procedure, and its modifications. Cogn Process 13(2):93–110. https://doi.org/10.1007/s10339-011-0430-z
Araújo Delmondes G, Pereira Lopes MJ, Araújo IM, de Sousa BA, Batista PR, Melo Coutinho HD, Alencar de Menezes IR, Barbosa-Filho JM, Bezerra Felipe CF, Kerntopf MR (2022) Possible mechanisms involved in the neuroprotective effect of Trans, trans-farnesol on pilocarpine-induced seizures in mice. Chem Biol Interact 365:110059. https://doi.org/10.1016/j.cbi.2022.110059
Armijo E, Gonzalez C, Shahnawaz M, Flores A, Davis B, Soto C (2017) Increased susceptibility to Aβ toxicity in neuronal cultures derived from familial Alzheimer’s disease (PSEN1-A246E) induced pluripotent stem cells. Neurosci Lett 639:74–81. https://doi.org/10.1016/j.neulet.2016.12.060
Bali J, Gheinani AH, Zurbriggen S, Rajendran L (2012) Role of genes linked to sporadic Alzheimer’s disease risk in the production of β-amyloid peptides. Proc Natl Acad Sci U S A 109(38):15307–15311. https://doi.org/10.1073/pnas.1201632109
Bhatia V, Sharma S (2021) Role of mitochondrial dysfunction, oxidative stress and autophagy in progression of Alzheimer’s disease. J Neurol Sci 421:117253
Birnbaum JH, Wanner D, Gietl AF, Saake A, Kündig TM, Hock C, Nitsch RM, Tackenberg C (2018) Oxidative stress and altered mitochondrial protein expression in the absence of amyloid-β and tau pathology in iPSC-derived neurons from sporadic Alzheimer’s disease patients. Stem Cell Res 27:121–130. https://doi.org/10.1016/j.scr.2018.01.019
Brown MR, Sullivan PG, Dorenbos KA, Modafferi EA, Geddes JW, Steward O (2004) Nitrogen disruption of synaptoneurosomes: an alternative method to isolate brain mitochondria. J Neurosci Methods 137(2):299–303. https://doi.org/10.1016/j.jneumeth.2004.02.028
Chen Y, Liang Z, Blanchard J, Dai CL, Sun S, Lee MH, Grundke-Iqbal I, Iqbal K, Liu F, Gong CX (2013) A non-transgenic mouse model (icv-STZ mouse) of Alzheimer’s disease: similarities to and differences from the transgenic model (3xTg-AD mouse). Mol Neurobiol 47(2):711–725. https://doi.org/10.1007/s12035-012-8375-5
Chen ZR, Huang JB, Yang SL, Hong FF (2022) Role of cholinergic signaling in Alzheimer’s disease. Molecules 27(6):1816. https://doi.org/10.3390/molecules27061816
Cho SY, Lim S, Ahn KS, Kwak HJ, Park J, Um JY (2021) Farnesol induces mitochondrial/peroxisomal biogenesis and thermogenesis by enhancing the AMPK signaling pathway in vivo and in vitro. Pharmacol Res 163:105312
Clark RE, Zola SM, Squire LR (2000) Impaired recognition memory in rats after damage to the hippocampus. J Neurosci 20(23):8853–8860. https://doi.org/10.1523/JNEUROSCI.20-23-08853.2000. https://pubmed.ncbi.nlm.nih.gov/11102494/
Correia SC, Santos RX, Santos MS, Casadesus G, Lamanna JC, Perry G, Smith MA, Moreira PI (2013) Mitochondrial abnormalities in a streptozotocin-induced rat model of sporadic Alzheimer’s disease. Curr Alzheimer Res 10(4):406–419. https://doi.org/10.2174/1567205011310040006
Cunningham AJ, Murray CA, O'Neill LA, Lynch MA, O'Connor JJ (1996) Interleukin-1 beta (IL-1 beta) and tumour necrosis factor (TNF) inhibit long-term potentiation in the rat dentate gyrus in vitro. Neurosci Lett 203(1):17–20. https://doi.org/10.1016/0304-3940(95)12252-4. https://pubmed.ncbi.nlm.nih.gov/8742036/
de Araújo DG, Bezerra DS, de Queiroz DD, de Souza BA, Araújo IM, Lins CG, Bandeira PFR, Barbosa R, Coutinho HDM, Felipe CFB, Barbosa-Filho JM, Alencar de Menezes IR, Kerntopf MR (2019) Toxicological and pharmacologic effects of farnesol (C15H26O): a descriptive systematic review. Food Chem Toxicol 129:169–200
de Oliveira JS, Abdalla FH, Dornelles GL, Adefegha SA, Palma TV, Signor C, da Silva BJ, Baldissarelli J, Lenz LS, Magni LP, Rubin MA, Pillat MM, de Andrade CM (2016) Berberine protects against memory impairment and anxiogenic-like behavior in rats submitted to sporadic Alzheimer’s-like dementia: Involvement of acetylcholinesterase and cell death. Neurotoxicology 57:241–250. https://doi.org/10.1016/j.neuro.2016.10.008
de Delmondes Araújo G, Bezerra DS, de Queiroz Dias D, de Souza Borges A, Araújo IM, da Cunha GL, Bandeira PF, Barbosa R, Coutinho HD, Felipe CF, Barbosa-Filho JM (2019) Toxicological and pharmacologic effects of farnesol (C15H26O): A descriptive systematic review. Food Chem Toxicol 129:169–200. https://doi.org/10.1016/j.fct.2019.04.037
Dhull DK, Kumar A (2018) Tramadol ameliorates behavioural, biochemical, mitochondrial and histological alterations in ICV-STZ-induced sporadic dementia of Alzheimer’s type in rats. Inflammopharmacol 26:925–938. https://doi.org/10.1007/s10787-017-0431-3
Du LL, Chai DM, Zhao LN, Li XH, Zhang FC, Zhang HB, Liu LB, Wu K, Liu R, Wang JZ, Zhou XW (2015) AMPK activation ameliorates Alzheimer's disease-like pathology and spatial memory impairment in a streptozotocin-induced Alzheimer's disease model in rats. J Alzheimers Dis 43(3):775–784. https://doi.org/10.3233/JAD-140564. https://pubmed.ncbi.nlm.nih.gov/25114075/
Duan L, Bhattacharyya BJ, Belmadani A, Pan L, Miller RJ, Kessler JA (2014) Stem cell derived basal forebrain cholinergic neurons from Alzheimer’s disease patients are more susceptible to cell death. Mol Neurodegener 9:3. https://doi.org/10.1186/1750-1326-9-3
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82(1):70–77. https://doi.org/10.1016/0003-9861(59)90090-6.h
Ellman GL, Courtney KD, Andres V Jr, Feather-Stone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95. https://doi.org/10.1016/0006-2952(61)90145-9
Erdoğan ME, Aydın S, Yanar K, Mengi M, Kansu AD, Cebe T, Belce A, Çelikten M, Çakatay U (2017) The effects of lipoic acid on redox status in brain regions and systemic circulation in streptozotocin-induced sporadic Alzheimer’s disease model. Metab Brain Dis 32(4):1017–1031. https://doi.org/10.1007/s11011-017-9983-6
Frackowiak RS, Pozzilli C, Legg NJ, Du Boulay GH, Marshall J, Lenzi GL, Jones T (1981) Regional cerebral oxygen supply and utilization in dementia. a clinical and physiological study with oxygen-15 and positron tomography. Brain 104:753–778. https://doi.org/10.1093/brain/104.4.753
Fronza MG, Baldinotti R, Martins MC, Goldani B, Dalberto BT, Kremer FS, Begnini K, Pinto LDS, Lenardão EJ, Seixas FK, Collares T, Alves D, Savegnago L (2019) Rational design, cognition and neuropathology evaluation of QTC-4-MeOBnE in a streptozotocin-induced mouse model of sporadic Alzheimer’s disease. Sci Rep 9(1):7276. https://doi.org/10.1038/s41598-019-43532-9
Fukui K, Omoi NO, Hayasaka T, Shinnkai T, Suzuki S, Abe K, Urano S (2002) Cognitive impairment of rats caused by oxidative stress and aging, and its prevention by vitamin E. Ann N Y Acad Sci 959:275–284. https://doi.org/10.1111/j.1749-6632.2002.tb02099.x
Fukuyama H, Ogawa M, Yamauchi H, Yamaguchi S, Kimura J, Yonekura Y, Konishi J (1994) Altered cerebral energy metabolism in Alzheimer’s disease: a PET study. J Nucl Med 35(1):1–6
Gabbita SP, Lovell MA, Markesbery WR (1998) Increased nuclear DNA oxidation in the brain in Alzheimer’s disease. J Neurochem 71(5):2034–2040. https://doi.org/10.1046/j.1471-4159.1998.71052034.x
Ghosh R, Sil S, Gupta P, Ghosh T (2020) Optimization of intracerebroventricular streptozotocin dose for the induction of neuroinflammation and memory impairments in rats. Metab Brain Dis 35(8):1279–1286. https://doi.org/10.1007/s11011-020-00588-1
Gibson GE, Starkov A, Blass JP, Ratan RR, Beal MF (1802) (2010) Cause and consequence: mitochondrial dysfunction initiates and propagates neuronal dysfunction, neuronal death and behavioral abnormalities in age-associated neurodegenerative diseases. Biochim Biophys Acta 1:122–134. https://doi.org/10.1016/j.bbadis.2009.08.010
Golan H, Levav T, Mendelsohn A, Huleihel M (2004) Involvement of tumor necrosis factor alpha in hippocampal development and function. Cereb Cortex 14(1):97–105. https://doi.org/10.1093/cercor/bhg108
Green LC, Wagner DA, Glogowski J, Skipper PL, Wishnok JS, Tannenbaum SR (1982) Analysis of nitrate, nitrite, and [15N]nitrate in biological fluids. Anal Biochem 126(1):131–138. https://doi.org/10.1016/0003-2697(82)90118-x
Grieb P (2016) Intracerebroventricular streptozotocin Injections as a model of Alzheimer’s Disease: in search of a relevant mechanism. Mol Neurobiol 53(3):1741–1752. https://doi.org/10.1007/s12035-015-9132-3
Guo R, Zong S, Wu M, Gu J, Yang M (2017) Architecture of human mitochondrial respiratory megacomplex I2III2IV2. Cell 170(6):1247-1257.e12. https://doi.org/10.1016/j.cell.2017.07.050
Hirai K, Aliev G, Nunomura A, Fujioka H, Russell RL, Atwood CS, Johnson AB, Kress Y, Vinters HV, Tabaton M, Shimohama S, Cash AD, Siedlak SL, Harris PL, Jones PK, Petersen RB, Perry G, Smith MA (2001) Mitochondrial abnormalities in Alzheimer’s disease. J Neurosci 21(9):3017–3023. https://doi.org/10.1523/JNEUROSCI.21-09-03017.2001
Imamura T, Yanagihara YT, Ohyagi Y, Nakamura N, Iinuma KM, Yamasaki R, Asai H, Maeda M, Murakami K, Irie K, Kira JI (2020) Insulin deficiency promotes formation of toxic amyloid-β42 conformer co-aggregating with hyper-phosphorylated tau oligomer in an Alzheimer’s disease model. Neurobiol Dis 137:104739. https://doi.org/10.1016/j.nbd.2020.104739
Inaoka DK, Shiba T, Sato D, Balogun EO, Sasaki T, Nagahama M, Oda M, Matsuoka S, Ohmori J, Honma T, Inoue M (2015) Structural insights into the molecular design of flutolanil derivatives targeted for fumarate respiration of parasite mitochondria. Int J Mol Sci 16(7):15287–15308
Ishrat T, Khan MB, Hoda MN, Yousuf S, Ahmad M, Ansari MA, Ahmad AS, Islam F (2006) Coenzyme Q10 modulates cognitive impairment against intracerebroventricular injection of streptozotocin in rats. Behav Brain Res 171(1):9–16. https://doi.org/10.1016/j.bbr.2006.03.009
Ishrat T, Parveen K, Khan MM, Khuwaja G, Khan MB, Yousuf S, Ahmad A, Shrivastav P, Islam F (2009) Selenium prevents cognitive decline and oxidative damage in rat model of streptozotocin-induced experimental dementia of Alzheimer’s type. Brain Res 1281:117–127. https://doi.org/10.1016/j.brainres.2009.04.010
Islam MT (2017) Oxidative stress and mitochondrial dysfunction-linked neurodegenerative disorders. Neurol Res 39(1):73–82. https://doi.org/10.1080/01616412.2016.1251711
Javed H, Vaibhav K, Ahmed ME, Khan A, Tabassum R, Islam F, Safhi MM, Islam F (2015) Effect of hesperidin on neurobehavioral, neuroinflammation, oxidative stress and lipid alteration in intracerebroventricular streptozotocin induced cognitive impairment in mice. J Neurol Sci 348(1–2):51–59. https://doi.org/10.1016/j.jns.2014.10.044
Johannsen DL, Ravussin E (2009) The role of mitochondria in health and disease. Curr Opin Pharmacol 9(6):780–786. https://doi.org/10.1016/j.coph.2009.09.002
Jung YY, Hwang ST, Sethi G, Fan L, Arfuso F, Ahn KS (2018) Potential anti-inflammatory and anti-cancer properties of farnesol. Molecules 23(11):2827. https://doi.org/10.3390/molecules23112827
Kamat PK (2015) Streptozotocin induced Alzheimer’s disease like changes and the underlying neural degeneration and regeneration mechanism. Neural Regen Res 10(7):1050–1052. https://doi.org/10.4103/1673-5374.160076
Kamat PK, Kalani A, Rai S, Tota SK, Kumar A, Ahmad AS (2016) Streptozotocin intracerebroventricular-induced neurotoxicity and brain insulin resistance: a therapeutic intervention for treatment of sporadic Alzheimer’s Disease (sAD)-like pathology. Mol Neurobiol 53(7):4548–4562. https://doi.org/10.1007/s12035-015-9384-y
Khan R, Sultana S (2011) Farnesol attenuates 1,2-dimethylhydrazine induced oxidative stress, inflammation and apoptotic responses in the colon of Wistar rats. Chem Biol Interact 192(3):193–200. https://doi.org/10.1016/j.cbi.2011.03.009
Kheradmand E, Hajizadeh Moghaddam A, Zare M (2018) Neuroprotective effect of hesperetin and nano-hesperetin on recognition memory impairment and the elevated oxygen stress in rat model of Alzheimer’s disease. Biomed Pharmacother 97:1096–1101. https://doi.org/10.1016/j.biopha.2017.11.047
King TE, Howard RL (1967) Preparations and properties of soluble NADH dehydrogenases from cardiac muscle. In: Pullman R (ed) Estabrook. Academic Press, New York, Methods in enzymology, pp 275–294. https://www.sciencedirect.com/science/article/abs/pii/0076687967100554
Kondo T, Asai M, Tsukita K, Kutoku Y, Ohsawa Y, Sunada Y, Imamura K, Egawa N, Yahata N, Okita K, Takahashi K, Asaka I, Aoi T, Watanabe A, Watanabe K, Kadoya C, Nakano R, Watanabe D, Maruyama K, Hori O, Hibino S, Choshi T, Nakahata T, Hioki H, Kaneko T, Naitoh M, Yoshikawa K, Yamawaki S, Suzuki S, Hata R, Ueno S, Seki T, Kobayashi K, Toda T, Murakami K, Irie K, Klein WL, Mori H, Asada T, Takahashi R, Iwata N, Yamanaka S, Inoue H (2013) Modeling Alzheimer’s disease with iPSCs reveals stress phenotypes associated with intracellular Aβ and differential drug responsiveness. Cell Stem Cell 12(4):487–496. https://doi.org/10.1016/j.stem.2013.01.009
Kono Y (1978) Generation of superoxide radical during autoxidation of hydroxylamine and an assay for superoxide dismutase. Arch Biochem Biophys 186(1):189–195. https://doi.org/10.1016/0003-9861(78)90479-4
Kraska A, Santin MD, Dorieux O, Joseph-Mathurin N, Bourrin E, Petit F, Jan C, Chaigneau M, Hantraye P, Lestage P, Dhenain M (2012) In vivo cross-sectional characterization of cerebral alterations induced by intracerebroventricular administration of streptozotocin. PLoS ONE 7(9):e46196. https://doi.org/10.1371/journal.pone.0046196
Ku CM, Lin JY (2013) Anti-inflammatory effects of 27 selected terpenoid compounds tested through modulating Th1/Th2 cytokine secretion profiles using murine primary splenocytes. Food Chem 141(2):1104–1113. https://doi.org/10.1016/j.foodchem.2013.04.044
Kumar P, Padi SS, Naidu PS, Kumar A (2007) Possible neuroprotective mechanisms of curcumin in attenuating 3-nitropropionic acid-induced neurotoxicity. Methods Find Exp Clin Pharmacol 29(1):19–25. https://doi.org/10.1358/mf.2007.29.1.1063492
Latina V, Giacovazzo G, Calissano P, Atlante A, La Regina F, Malerba F, Dell’Aquila M, Stigliano E, Balzamino BO, Micera A, Coccurello R, Amadoro G (2021) Tau cleavage contributes to cognitive dysfunction in strepto-zotocin-induced sporadic Alzheimer’s disease (sAD) mouse model. Int J Mol Sci 22(22):12158. https://doi.org/10.3390/ijms222212158
LeBel CP, Ischiropoulos H, Bondy SC (1992) Evaluation of the probe 2’,7’-dichlorofluorescin as an indicator of reactive oxygen species formation and oxidative stress. Chem Res Toxicol 5(2):227–231
Levine RL, Wehr N, Williams JA, Stadtman ER, Shacter E (2000) Determination of carbonyl groups in oxidized proteins. Methods Mol Biol 99:15–24. https://doi.org/10.1385/1-59259-054-3:15
Li L, Qin L, Lu HL, Li PJ, Song YJ, Yang RL (2017) Methylene blue improves streptozotocin-induced memory deficit by restoring mitochondrial function in rats. Brain Res 1657:208–214. https://doi.org/10.1016/j.brainres.2016.12.024
Liu Y, Peterson DA, Kimura H, Schubert D (1997) Mechanism of cellular 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) reduction. J Neurochem 69(2):581–593. https://doi.org/10.1046/j.1471-4159.1997.69020581.x
Liu M, Liao K, Yu C, Li X, Liu S, Yang S (2014) Puerarin alleviates neuropathic pain by inhibiting neuroinflammation in spinal cord. Mediat Inflamm 2014:485927. https://doi.org/10.1155/2014/485927
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193(1):265–275
Luck H (1965) Catalase. In: Bergmeyer HU (ed) Method of enzymatic analysis. Academic Press, New York and London, pp 885–894
Luo H, Xiang Y, Qu X, Liu H, Liu C, Li G, Han L, Qin X (2019) Apelin-13 Suppresses neuroinflammation against cognitive deficit in a streptozotocin-induced rat model of alzheimer’s disease through activation of BDNF-TrkB signaling pathway. Front Pharmacol 10:395. https://doi.org/10.3389/fphar.2019.00395
Maurer I, Zierz S, Möller HJ (2000) A selective defect of cytochrome c oxidase is present in brain of Alzheimer disease patients. Neurobiol Aging 21(3):455–462. https://doi.org/10.1016/s0197-4580(00)00112-3
Misrani A, Tabassum S, Yang L (2021) Mitochondrial dysfunction and oxidative stress in alzheimer’s disease. Front Aging Neurosci 13:617588. https://doi.org/10.3389/fnagi.2021.617588
Moreira PI, Cardoso SM, Santos MS, Oliveira CR (2006) The key role of mitochondria in Alzheimer’s disease. J Alzheimers Dis 9(2):101–110. https://doi.org/10.3233/jad-2006-9202
Moreira PI, Santos MS, Oliveira CR (2007) Alzheimer’s disease: a lesson from mitochondrial dysfunction. Antioxid Redox Signal 9(10):1621–1630. https://doi.org/10.1089/ars.2007.1703
Moreira PI, Duarte AI, Santos MS, Rego AC, Oliveira CR (2009) An integrative view of the role of oxidative stress, mitochondria and insulin in Alzheimer’s disease. J Alzheimers Dis 16(4):741–761. https://doi.org/10.3233/JAD-2009-0972
Morris R (1984) Developments of a water-maze procedure for studying spatial learning in the rat. J Neurosci Methods 11(1):47–60. https://doi.org/10.1016/0165-0270(84)90007-4
Mutisya EM, Bowling AC, Beal MF (1994) Cortical cytochrome oxidase activity is reduced in Alzheimer’s disease. J Neurochem 63(6):2179–2184. https://doi.org/10.1046/j.1471-4159.1994.63062179.x
Nabavi Zadeh F, Nazari M, Amini A, Adeli S, Barzegar Behrooz A, Fahanik Babaei J (2023) Pre- and post-treatment of α-Tocopherol on cognitive, synaptic plasticity, and mitochondrial disorders of the hippocampus in icv-streptozotocin-induced sporadic Alzheimer’s-like disease in male Wistar rat. Front Neurosci 17:1073369. https://doi.org/10.3389/fnins.2023.1073369
Navarro A, Boveris A (2007) The mitochondrial energy transduction system and the aging process. Am J Physiol Cell Physiol 292(2):C670–C686. https://doi.org/10.1152/ajpcell.00213.2006
Niedzielska E, Smaga I, Gawlik M, Moniczewski A, Stankowicz P, Pera J, Filip M (2016) Oxidative stress in neurodegenerative diseases. Mol Neurobiol 53:4094–4125
Nunomura A, Perry G, Aliev G, Hirai K, Takeda A, Balraj EK, Jones PK, Ghanbari H, Wataya T, Shimohama S, Chiba S, Atwood CS, Petersen RB, Smith MA (2001) Oxidative damage is the earliest event in Alzheimer disease. J Neuropathol Exp Neurol 60(8):759–767. https://doi.org/10.1093/jnen/60.8.759
Ochalek A, Mihalik B, Avci HX, Chandrasekaran A, Téglási A, Bock I, Giudice ML, Táncos Z, Molnár K, László L, Nielsen JE, Holst B, Freude K, Hyttel P, Kobolák J, Dinnyés A (2017) Neurons derived from sporadic Alzheimer’s disease iPSCs reveal elevated TAU hyperphosphorylation, increased amyloid levels, and GSK3B activation. Alzheimers Res Ther 9(1):90. https://doi.org/10.1186/s13195-017-0317-z
Paidi RK, Nthenge-Ngumbau DN, Singh R, Kankanala T, Mehta H, Mohanakumar KP (2015) Mitochondrial deficits accompany cognitive decline following single bilateral intracerebroventricular streptozotocin. Curr Alzheimer Res 12(8):785–795. https://doi.org/10.2174/1567205012666150710112618
Parker WD Jr, Filley CM, Parks JK (1990) Cytochrome oxidase deficiency in Alzheimer’s disease. Neurology 40(8):1302–1303. https://doi.org/10.1212/wnl.40.8.1302
Paxinos G, Watson C (2007) The rat brain in stereotaxic coordinates, 6th edn. Academic Press, San Diego
Penney J, Ralvenius WT, Tsai LH (2020) Modeling Alzheimer’s disease with iPSC-derived brain cells. Mol Psychiatry 25:148–167. https://doi.org/10.1038/s41380-019-0468-3
Qamar W, Sultana S (2008) Farnesol ameliorates massive inflammation, oxidative stress and lung injury induced by intratracheal instillation of cigarette smoke extract in rats: an initial step in lung chemoprevention. Chem Biol Interact 176(2–3):79–87. https://doi.org/10.1016/j.cbi.2008.08.011
Rai S, Kamat PK, Nath C, Shukla R (2013) A study on neuroinflammation and NMDA receptor function in STZ (ICV) induced memory impaired rats. J Neuroimmunol 254(1–2):1–9. https://doi.org/10.1016/j.jneuroim.2012.08.008
Rai S, Kamat PK, Nath C, Shukla R (2014) Glial activation and post-synaptic neurotoxicity: the key events in Streptozotocin (ICV) induced memory impairment in rats. Pharmacol Biochem Behav 117:104–117. https://doi.org/10.1016/j.pbb.2013.11.035
Rajasekar N, Nath C, Hanif K, Shukla R (2017) Intranasal insulin administration ameliorates streptozotocin (ICV)-induced insulin receptor dysfunction, neuroinflammation, amyloidogenesis, and memory impairment in rats. Mol Neurobiol 54(8):6507–6522. https://doi.org/10.1007/s12035-016-0169-8
Ray PD, Huang BW, Tsuji Y (2012) Reactive oxygen species (ROS) homeostasis and redox regulation in cellular signaling. Cell Signal 24(5):981–990. https://doi.org/10.1016/j.cellsig.2012.01.008
Retinasamy T, Shaikh MF, Kumari Y, Abidin SAZ, Othman I (2020) Orthosiphon stamineus standardized extract reverses streptozotocin-induced Alzheimer’s disease-like condition in a rat model. Biomedicines 8(5):104. https://doi.org/10.3390/biomedicines8050104
Salentin S, Schreiber S, Haupt VJ, Adasme MF, Schroeder M (2015) PLIP: fully automated protein-ligand interaction profiler. Nucleic Acids Res 43(W1):W443–W447. https://doi.org/10.1093/nar/gkv315
Santos TO, Mazucanti CH, Xavier GF, Torrão AS (2012) Early and late neurodegeneration and memory disruption after intracerebroventricular streptozotocin. Physiol Behav 107(3):401–413. https://doi.org/10.1016/j.physbeh.2012.06.019
Saxena G, Patro IK, Nath C (2011) ICV STZ induced impairment in memory and neuronal mitochondrial function: A protective role of nicotinic receptor. Behav Brain Res 224(1):50–57. https://doi.org/10.1016/j.bbr.2011.04.039
Shahnouri M, Abouhosseini Tabari M, Araghi A (2016) Neuropharmacological properties of farnesol in Murine model. Iran J Vet Res 17(4):259–264
Sharma M, Gupta YK (2003) Effect of alpha lipoic acid on intracerebroventricular streptozotocin model of cognitive impairment in rats. Eur Neuropsychopharmacol 13(4):241–247. https://doi.org/10.1016/s0924-977x(03)00008-7
Sharma C, Kim SR (2021) Linking Oxidative Stress and Proteinopathy in Alzheimer’s Disease. Antioxidants (basel) 10(8):1231. https://doi.org/10.3390/antiox10081231
Sims NR, Finegan JM, Blass JP, Bowen DM, Neary D (1987) Mitochondrial function in brain tissue in primary degenerative dementia. Brain Res 436(1):30–38. https://doi.org/10.1016/0006-8993(87)91553-8
Singh A, Kumar A (2018) The possible neuroprotective potential of galantamine along with Soya-lecithin and hydroxychloroquine against ICV-STZ-induced cognitive dysfunction in rats. Alzheimers Dement 14(7S):P1523-1524. https://doi.org/10.1016/j.jalz.2018.07.037
Singh A, Kukreti R, Saso L, Kukreti S (2019) Oxidative stress: a key modulator in neurodegenerative diseases. Molecules 24(8):1583. https://doi.org/10.3390/molecules24081583
Sottocasa GL, Kuylenstierna B, Ernster L, Bergstrand A (1967) An electron-transport system associated with the outer membrane of liver mitochondria. a biochemical and morphological study. J Cell Biol 32(2):415–438. https://doi.org/10.1083/jcb.32.2.415
Souza DS, Barreto TO, Menezes-Filho JER, Heimfarth L, Rhana P, Rabelo TK, Santana MNS, Durço AO, Conceição MRL, Quintans-Júnior LJ, Guimarães AG, Cruz JS, Vasconcelos CML (2020) Myocardial hypertrophy is prevented by farnesol through oxidative stress and ERK1/2 signaling pathways. Eur J Pharmacol 887:173583. https://doi.org/10.1016/j.ejphar.2020.173583
Špičáková A, Szotáková B, Dimunová D, Myslivečková Z, Kubíček V, Ambrož M, Lněničková K, Krasulová K, Anzenbacher P, Skálová L (2017) Nerolidol and farnesol inhibit some cytochrome P450 activities but did not affect other xenobiotic-metabolizing enzymes in rat and human hepatic subcellular fractions. Molecules 22(4):509. https://doi.org/10.3390/molecules22040509
Stefanova NA, Ershov NI, Maksimova KY, Muraleva NA, Tyumentsev MA, Kolosova NG (2019) The rat prefrontal-cortex transcriptome: effects of aging and sporadic alzheimer’s disease-like pathology. J Gerontol A Biol Sci Med Sci 74(1):33–43. https://doi.org/10.1093/gerona/gly198
Su B, Wang X, Nunomura A, Moreira PI, Lee HG, Perry G, Smith MA, Zhu X (2008) Oxidative stress signaling in Alzheimer’s disease. Curr Alzheimer Res 5(6):525–532. https://doi.org/10.2174/156720508786898451
Swerdlow RH, Parks JK, Cassarino DS, Maguire DJ, Maguire RS, Bennett JP Jr, Davis RE, Parker WD Jr (1997) Cybrids in Alzheimer’s disease: a cellular model of the disease? Neurology 49(4):918–925. https://doi.org/10.1212/wnl.49.4.918
Tancredi V, D'Arcangelo G, Grassi F, Tarroni P, Palmieri G, Santoni A, Eusebi F (1992) Tumor necrosis factor alters synaptic transmission in rat hippocampal slices. Neurosci Lett 146(2):176–178. https://doi.org/10.1016/0304-3940(92)90071-e. https://pubmed.ncbi.nlm.nih.gov/1337194/
Tian Z, Wang J, Xu M, Wang Y, Zhang M, Zhou Y (2016) Resveratrol improves cognitive impairment by regulating apoptosis and synaptic plasticity in streptozotocin-induced diabetic rats. Cell Physiol Biochem 40(6):1670–1677. https://doi.org/10.1159/000453216
Tyumentsev MA, Stefanova NA, Muraleva NA, Rumyantseva YV, Kiseleva E, Vavilin VA, Kolosova NG (2018) Mitochondrial dysfunction as a predictor and driver of alzheimer’s disease-like pathology in OXYS rats. J Alzheimers Dis 63(3):1075–1088. https://doi.org/10.3233/JAD-180065
Uttara B, Singh AV, Zamboni P, Mahajan RT (2009) Oxidative stress and neurodegenerative diseases: a review of upstream and downstream antioxidant therapeutic options. Curr Neuropharmacol 7(1):65–74. https://doi.org/10.2174/157015909787602823
Wallace AC, Laskowski RA, Thornton JM (1995) LIGPLOT: a program to generate schematic diagrams of protein-ligand interactions. Protein Eng 8(2):127–134. https://doi.org/10.1093/protein/8.2.127
Wang X, Wang W, Li L, Perry G, Lee HG, Zhu X (2014) Oxidative stress and mitochondrial dysfunction in Alzheimer's disease. Biochim Biophys Acta 1842(8):1240–1247. https://doi.org/10.1016/j.bbadis.2013.10.015. https://pubmed.ncbi.nlm.nih.gov/24189435/
Wang J, Markesbery WR, Lovell MA (2006) Increased oxidative damage in nuclear and mitochondrial DNA in mild cognitive impairment. J Neurochem 96(3):825–832. https://doi.org/10.1111/j.1471-4159.2005.03615.x
Wang X, Su B, Lee HG, Li X, Perry G, Smith MA, Zhu X (2009) Impaired balance of mitochondrial fission and fusion in Alzheimer’s disease. J Neurosci 29(28):9090–9103. https://doi.org/10.1523/JNEUROSCI.1357-09.2009
Wang T, Fu F, Han B, Zhang L, Zhang X (2012) Danshensu ameliorates the cognitive decline in streptozotocin-induced diabetic mice by attenuating advanced glycation end product-mediated neuroinflammation. J Neuroimmunol 245(1–2):79–86. https://doi.org/10.1016/j.jneuroim.2012.02.008
Wills ED (1966) Mechanisms of lipid peroxide formation in animal tissues. Biochem J 99(3):667–676. https://doi.org/10.1042/bj0990667
Xiang X, Wang X, Jin S, Hu J, Wu Y, Li Y, Wu X (2022) Activation of GPR55 attenuates cognitive impairment and neurotoxicity in a mouse model of Alzheimer’s disease induced by Aβ1-42 through inhibiting RhoA/ROCK2 pathway. Prog Neuropsychopharmacol Biol Psychiatry 112:110423. https://doi.org/10.1016/j.pnpbp.2021.110423
Zhou Y, Lian S, Zhang J, Lin D, Huang C, Liu L, Chen Z (2018) Mitochondrial perturbation contributing to cognitive decline in streptozotocin-induced type 1 diabetic rats. Cell Physiol Biochem 46(4):1668–1682. https://doi.org/10.1159/000489243
Acknowledgements
We sincerely appreciate the help provided by the ICMR-SRF and RA grants (No. 45/35/2018-PHA/BMS and 3/1/3/5/M/2022-NCD-II) from the Indian Council of Medical Research (ICMR), New Delhi, India.
Author information
Authors and Affiliations
Contributions
MK: design and creation of the research; planning, and executing behavioral investigations; carrying out the surgery; assessing the outcomes; performing outcomes analysis; and writing the manuscript. NS: executing experiments (ROS and protein carbonyls estimation), evaluating the results, statistical analysis. AK: carrying out experiments (ROS, protein carbonyls and TNF-alpha estimation), evaluating the results. AK: design and creation of the research; creating and directing all of the experiments; evaluating and analysing the results; writing, reviewing, and editing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors further state that there are no conflicts of interest between them that need to be disclosed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kadian, M., Saini, N., Khera, A. et al. Neuroprotective mechanism of trans,trans-Farnesol in an ICV-STZ-induced rat model of Alzheimer’s pathology. Inflammopharmacol 32, 1545–1573 (2024). https://doi.org/10.1007/s10787-023-01413-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-023-01413-8