Abstract—
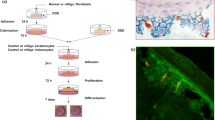
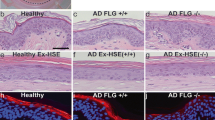
Hidradenitis suppurativa (HS) is a complex and debilitating inflammatory skin disease for which no effective treatment is available currently. This is partly because of the lack of adequate human or animal models for defining the pathobiology of the disease. Here, we describe the development of air–liquid (A-L) interface, liquid-submersion (L-S), and bioreactor (Bio) ex vivo skin culture models. All three ex vivo platforms were effective for culturing skin samples for up to 14 days. Tissue architecture and integrity remained intact for at least 3 days for healthy skin and 14 days for HS skin. Up to day 3, no significant differences were observed in % early apoptotic cells among all three platforms. However, late apoptotic/necrotic cell death was increased in HS skin at day 3 in A-L and Bio culture. These cultures efficiently support the growth of various cells populations, including keratinocytes and immune cells. Profiling inflammatory gene signatures in HS skin from these ex vivo cultures showed dynamic changes in expression at day 3 and day 14. All three culture platforms were necessary to represent the inflammatory gene status of HS skin at day 0, suggesting that not all gene clusters were identically altered in each culture method. Similarly, cytokine/chemokine profiling of the supernatants from vehicle- and drug-treated ex vivo HS cultures again showed a better prediction of drug efficacy against HS. Overall, development of these three culture systems collectively provides a powerful tool to uncover the pathobiology of HS progression and screen various drugs against HS.
Graphical abstract








Similar content being viewed by others
Availability of Data and Materials
Data generated/analyzed during this study are included in this published article (and its supplementary information files).
References
Garg, A., J.S. Kirby, J. Lavian, G. Lin, and A. Strunk. 2017. Sex- and age-adjusted population analysis of prevalence estimates for hidradenitis suppurativa in the United States. JAMA dermatology 153: 760–764.
Phan, K., O. Charlton, and S.D. Smith. 2020. Global prevalence of hidradenitis suppurativa and geographical variation—Systematic review and meta-analysis. Biomedical Dermatology 4: 2.
Frew, J.W., K. Navrazhina, M. Marohn, P.C. Lu, and J.G. Krueger. 2019. Contribution of fibroblasts to tunnel formation and inflammation in hidradenitis suppurativa/acne inversa. Experimental dermatology 28: 886–891.
Guenin-Mace, L., J.D. Morel, J.M. Doisne, A. Schiavo, L. Boulet, V. Mayau, P. Goncalves, S. Duchatelet, A. Hovnanian, V. Bondet, et al. 2020. Dysregulation of tryptophan catabolism at the host-skin microbiota interface in hidradenitis suppurativa. JCI Insight 5: e140598.
Byrd, A.S., C. Carmona-Rivera, L.J. O’Neil, P.M. Carlucci, C. Cisar, A.Z. Rosenberg, M.L. Kerns, J.A. Caffrey, S.M. Milner, J.M. Sacks, et al. 2019. Neutrophil extracellular traps B cells, and type I interferons contribute to immune dysregulation in hidradenitis suppurativa. Science translational medicine 11: 508.
van der Zee, H.H., L. de Ruiter, J. Boer, D.G. van den Broecke, J.C. den Hollander, J.D. Laman, and E.P. Prens. 2012. Alterations in leucocyte subsets and histomorphology in normal-appearing perilesional skin and early and chronic hidradenitis suppurativa lesions. British Journal of Dermatology 166: 98–106.
Shah, N. 2005. Hidradenitis suppurativa: A treatment challenge. American family physician 72: 1547–1552.
Hotz, C., M. Boniotto, A. Guguin, M. Surenaud, F. Jean-Louis, P. Tisserand, N. Ortonne, B. Hersant, R. Bosc, F. Poli, et al. 2016. Intrinsic defect in keratinocyte function leads to inflammation in hidradenitis suppurativa. Journal of Investigative Dermatology 136: 1768–1780.
Navrazhina, K., J.W. Frew, P. Gilleaudeau, M. Sullivan-Whalen, S. Garcet, and J.G. Krueger. 2021. Epithelialized tunnels are a source of inflammation in hidradenitis suppurativa. Journal of Allergy and Clinical Immunology 147: 2213–2224.
Sbidian, E., C. Hotz, J. Seneschal, A. Maruani, F. Amelot, F. Aubin, C. Paul, M. Beylot-Barry, P. Humbert, A. Dupuy, et al. 2016. Antitumour necrosis factor-alpha therapy for hidradenitis suppurativa: Results from a national cohort study between 2000 and 2013. British Journal of Dermatology 174: 667–670.
Theut-Riis, P., L.R. Thorlacius, and G.B. Jemec. 2018. Investigational drugs in clinical trials for hidradenitis suppurativa. Expert opinion on investigational drugs 27: 43–53.
van der Zee, H.H., L. de Ruiter, D.G. van den Broecke, W.A. Dik, J.D. Laman, and E.P. Prens. 2011. Elevated levels of tumour necrosis factor (TNF)-alpha, interleukin (IL)-1beta and IL-10 in hidradenitis suppurativa skin: A rationale for targeting TNF-alpha and IL-1beta. British Journal of Dermatology 164: 1292–1298.
Lowe, M.M., H.B. Naik, S. Clancy, M. Pauli, K.M. Smith, Y. Bi, R., Dunstan, J.E. Gudjonsson, M. Paul, H. Harris, et al. 2020. Immunopathogenesis of hidradenitis suppurativa and response to anti-TNF-alpha therapy. JCI Insight 5: e139932.
Folkes, A.S., F.Z. Hawatmeh, A. Wong, and F.A. Kerdel. 2020. Emerging drugs for the treatment of hidradenitis suppurativa. Expert Opinion on Emerging Drugs 25: 201–211.
Marzano, A.V., G. Genovese, G. Casazza, C. Moltrasio, P. Dapavo, G. Micali, R. Sirna, P. Gisondi, A. Patrizi, V. Dini, et al. 2021. Evidence for a “window of opportunity” in hidradenitis suppurativa treated with adalimumab: A retrospective real-life multicentre cohort study. British Journal of Dermatology 184: 133–140.
Frew, J.W., J.E. Hawkes, and J.G. Krueger. 2018. A systematic review and critical evaluation of inflammatory cytokine associations in hidradenitis suppurativa. F1000Research 7: 1930.
Goliwas, K.F., J.R. Richter, H.C. Pruitt, L.M. Araysi, N.R. Anderson, R.S. Samant, S.M. Lobo-Ruppert, J.L. Berry, and A.R. Frost. 2017. Methods to evaluate cell growth, viability, and response to treatment in a tissue engineered breast cancer model. Scientific reports 7: 14167.
Kashyap, M., N. Kawamorita, V. Tyagi, Y. Sugino, M. Chancellor, N. Yoshimura, and P. Tyagi. 2013. Down-regulation of nerve growth factor expression in the bladder by antisense oligonucleotides as new treatment for overactive bladder. The Journal of urology 190: 757–764.
Goliwas, K.F., C.S. Simmons, S.A. Khan, A.M. Wood, Y. Wang, J.L. Berry, M. Athar, J.A. Mobley, Y.I. Kim, V.J. Thannickal, et al. 2021. Local SARS-CoV-2 peptide-specific immune responses in convalescent and uninfected human lung tissue models. medRxiv.
Bao, Y., X. Wu, J. Chen, X. Hu, F. Zeng, J. Cheng, H. Jin, and X., Lin, and L.F. Chen. 2017. Brd4 modulates the innate immune response through Mnk2-eIF4E pathway-dependent translational control of IkappaBalpha. Proceedings of the National Academy of Sciences 114: E3993–E4001.
Fink, E.C., and B.L. Ebert. 2015. The novel mechanism of lenalidomide activity. Blood 126: 2366–2369.
Banerjee, A., S. McNish, and V.K. Shanmugam. 2017. Interferon-gamma (IFN-gamma) is elevated in wound exudate from hidradenitis suppurativa. Immunological investigations 46: 149–158.
Hessam, S., M. Sand, T. Gambichler, M. Skrygan, I. Ruddel, and F.G. Bechara. 2018. Interleukin-36 in hidradenitis suppurativa: Evidence for a distinctive proinflammatory role and a key factor in the development of an inflammatory loop. British Journal of Dermatology 178: 761–767.
Jimenez-Gallo, D., R. de la Varga-Martinez, L. Ossorio-Garcia, C. Albarran-Planelles, C. Rodriguez, and M. Linares-Barrios. 2017. The clinical significance of increased serum proinflammatory cytokines C-reactive protein and erythrocyte sedimentation rate in patients with hidradenitis suppurativa. Mediators of inflammation 2017: 2450401.
Kanni, T., V. Tzanetakou, A. Savva, B. Kersten, A. Pistiki, F.L. van de Veerdonk, M.G. Netea, J.W. van der Meer, and E.J. Giamarellos-Bourboulis. 2015. Compartmentalized cytokine responses in hidradenitis suppurativa. PLoS One 10: e0130522.
Vossen, A., C.B. Ardon, H.H. van der Zee, E. Lubberts, and E.P. Prens. 2019. The anti-inflammatory potency of biologics targeting tumour necrosis factor-alpha, interleukin (IL)-17A, IL-12/23 and CD20 in hidradenitis suppurativa: An ex vivo study. British Journal of Dermatology 181: 314–323.
Brandao, L., R. Moura, P.M. Tricarico, R. Gratton, G. Genovese, C. Moltrasio, S. Garcovich, M. Boniotto, S. Crovella, and A.V. Marzano. 2020. Altered keratinization and vitamin D metabolism may be key pathogenetic pathways in syndromic hidradenitis suppurativa: A novel whole exome sequencing approach. Journal of Dermatological Science 99: 17–22.
Filippou, P.S., G.S. Karagiannis, and A. Constantinidou. 2020. Midkine (MDK) growth factor: A key player in cancer progression and a promising therapeutic target. Oncogene 39: 2040–2054.
Hoffman, L.K., L.E. Tomalin, G. Schultz, M.D. Howell, N. Anandasabapathy, A. Alavi, M. Suarez-Farinas, and M.A. Lowes. 2018. Integrating the skin and blood transcriptomes and serum proteome in hidradenitis suppurativa reveals complement dysregulation and a plasma cell signature. PLoS One 13: e0203672.
Jones, S.E., and C. Jomary. 2002. Clusterin. The international journal of biochemistry & cell biology 34: 427–431.
Sabat, R., A. Chanwangpong, S. Schneider-Burrus, D. Metternich, G. Kokolakis, A. Kurek, S. Philipp, D. Uribe, K. Wolk, and W. Sterry. 2012. Increased prevalence of metabolic syndrome in patients with acne inversa. PLoS One 7: e31810.
Funding
NIH grant RO1 ES026219 and NCI grant 5P01CA210946 and by intramural UAB funds to M.A.
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: J.S.D., C.R., M.S.M., M.A. Performed the experiments: K.F.G., M.P.K., J.K., R.S., Z.W., A.O., L.J., V.A., M.B.L. Analyzed the data: K.F.G., M.P.K., J.K., R.S., Z.W., A.O., L.J., V.A., M.B.L., C.A.E., M.S.M., C.R., J.S.D., M.A. Contributed reagents/materials/analysis tools: C.A.E., M.S.M., C.R., J.S.D., M.A. Wrote the paper: K.F.G., M.P.K., J.S.D., and M.A.
Corresponding authors
Ethics declarations
Ethical Approval and Consent to Participate
The institutional Review Board of the University of Alabama at Birmingham approved the protocol (IRB-300005214) for obtaining surgically removed discarded skin tissues from breast/tummy reduction from otherwise healthy individuals and HS patients.
Consent of Publication
All authors agree to submit this manuscript.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Goliwas, K., Kashyap, M.P., Khan, J. et al. Ex Vivo Culture Models of Hidradenitis Suppurativa for Defining Molecular Pathogenesis and Treatment Efficacy of Novel Drugs. Inflammation 45, 1388–1401 (2022). https://doi.org/10.1007/s10753-022-01629-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-022-01629-w