Abstract
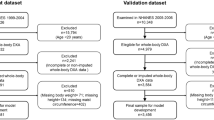
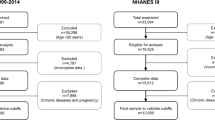
An inverse association between body mass index (BMI) and risk of lung cancer has been reported. However, the association of body composition such as fat mass (FM) and lean body mass (LBM) with risk of lung cancer has not been fully investigated. Using two large prospective cohort studies (Nurses’ Health Study, 1986–2014; Health Professionals Follow-up Study, 1987–2012) in the United States, we included 100,985 participants who were followed for occurrence of lung cancer. Predicted FM and LBM derived from validated anthropometric prediction equations were categorized by sex-specific deciles. During an average 22.3-year follow-up, 2615 incident lung cancer cases were identified. BMI showed an inverse association with lung cancer risk. Participants in the 10th decile of predicted FM and LBM had a lower risk of lung cancer compared with those in the 1st decile, but when mutually adjusted for each other, predicted FM was not associated with lung cancer risk (adjusted hazard ratio [aHR] = 0.98, 95% confidence interval [CI] 0.72–1.35; P(trend) = 0.97) whereas predicted LBM had an inverse association (aHR = 0.73, 95% CI 0.53–1.00; P(trend) = 0.03), especially among participants who were current smokers or had smoked in the previous 10 years (aHR = 0.55, 95% CI 0.36–0.84; P(trend) = 0.008). In conclusion, BMI was inversely associated with lung cancer risk. Based on anthropometric prediction equations, low LBM rather than low FM accounted for the inverse association between BMI and lung cancer risk.
Similar content being viewed by others
References
Renehan AG, Tyson M, Egger M, Heller RF, Zwahlen M. Body-mass index and incidence of cancer: a systematic review and meta-analysis of prospective observational studies. Lancet. 2008;371(9612):569–78. https://doi.org/10.1016/s0140-6736(08)60269-x.
Smith L, Brinton LA, Spitz MR, Lam TK, Park Y, Hollenbeck AR, et al. Body mass index and risk of lung cancer among never, former, and current smokers. J Natl Cancer Inst. 2012;104(10):778–89. https://doi.org/10.1093/jnci/djs179.
Sanikini H, Yuan J-M, Butler LM, Koh W-P, Gao Y-T, Steffen A, et al. Body mass index and lung cancer risk: a pooled analysis based on nested case-control studies from four cohort studies. BMC Cancer. 2018;18(1):220. https://doi.org/10.1186/s12885-018-4124-0.
Kabat GC, Kim M, Hunt JR, Chlebowski RT, Rohan TE. Body mass index and waist circumference in relation to lung cancer risk in the Women’s Health Initiative. Am J Epidemiol. 2008;168(2):158–69. https://doi.org/10.1093/aje/kwn109.
Bethea TN, Rosenberg L, Charlot M, O’Connor GT, Adams-Campbell LL, Palmer JR. Obesity in relation to lung cancer incidence in African American women. Cancer Causes Control. 2013;24(9):1695–703. https://doi.org/10.1007/s10552-013-0245-6.
El-Zein M, Parent ME, Nicolau B, Koushik A, Siemiatycki J, Rousseau MC. Body mass index, lifetime smoking intensity and lung cancer risk. Int J Cancer. 2013;133(7):1721–31. https://doi.org/10.1002/ijc.28185.
Olson JE, Yang P, Schmitz K, Vierkant RA, Cerhan JR, Sellers TA. Differential association of body mass index and fat distribution with three major histologic types of lung cancer: evidence from a cohort of older women. Am J Epidemiol. 2002;156(7):606–15. https://doi.org/10.1093/aje/kwf084.
Chiolero A, Faeh D, Paccaud F, Cornuz J. Consequences of smoking for body weight, body fat distribution, and insulin resistance. Am J Clin Nutr. 2008;87(4):801–9. https://doi.org/10.1093/ajcn/87.4.801.
Malhotra J, Malvezzi M, Negri E, La Vecchia C, Boffetta P. Risk factors for lung cancer worldwide. Eur Respir J. 2016;48(3):889–902. https://doi.org/10.1183/13993003.00359-2016.
Yu D, Zheng W, Johansson M, Lan Q, Park Y, White E, et al. Overall and central obesity and risk of lung cancer: a pooled analysis. J Natl Cancer Inst. 2018;110(8):831–42. https://doi.org/10.1093/jnci/djx286.
Dewi NU, Boshuizen HC, Johansson M, Vineis P, Kampman E, Steffen A, et al. Anthropometry and the Risk of Lung Cancer in EPIC. Am J Epidemiol. 2016;184(2):129–39. https://doi.org/10.1093/aje/kwv298.
Padwal R, Leslie WD, Lix LM, Majumdar SR. Relationship among body fat percentage, body mass index, and all-cause mortality: a cohort study. Ann Intern Med. 2016;164(8):532–41. https://doi.org/10.7326/m15-1181.
Han SS, Kim KW, Kim KI, Na KY, Chae DW, Kim S, et al. Lean mass index: a better predictor of mortality than body mass index in elderly Asians. J Am Geriatr Soc. 2010;58(2):312–7. https://doi.org/10.1111/j.1532-5415.2009.02672.x.
Lee DH, Giovannucci EL. Body composition and mortality in the general population: a review of epidemiologic studies. Exp Biol Med. 2018;243(17–18):1275–85. https://doi.org/10.1177/1535370218818161.
Tsai S. Importance of lean body mass in the oncologic patient. Nutr Clin Pract. 2012;27(5):593–8. https://doi.org/10.1177/0884533612457949.
Schols AM, Broekhuizen R, Weling-Scheepers CA, Wouters EF. Body composition and mortality in chronic obstructive pulmonary disease. Am J Clin Nutr. 2005;82(1):53–9. https://doi.org/10.1093/ajcn.82.1.53.
Lee DH, Keum N, Hu FB, Orav EJ, Rimm EB, Sun Q, et al. Development and validation of anthropometric prediction equations for lean body mass, fat mass and percent fat in adults using the National Health and Nutrition Examination Survey (NHANES) 1999–2006. Br J Nutr. 2017;118(10):858–66. https://doi.org/10.1017/s0007114517002665.
Lee DH, Keum N, Hu FB, Orav EJ, Rimm EB, Willett WC, et al. Comparison of the association of predicted fat mass, body mass index, and other obesity indicators with type 2 diabetes risk: two large prospective studies in US men and women. Eur J Epidemiol. 2018;33(11):1113–23. https://doi.org/10.1007/s10654-018-0433-5.
Lee DH, Keum N, Hu FB, Orav EJ, Rimm EB, Willett WC, et al. Predicted lean body mass, fat mass, and all cause and cause specific mortality in men: prospective US cohort study. BMJ. 2018;362:k2575. https://doi.org/10.1136/bmj.k2575.
Hanyuda A, Lee DH, Ogino S, Wu K, Giovannucci EL. Long-term status of predicted body fat percentage, body mass index, and other anthropometric factors with risk of colorectal carcinoma: Two large prospective cohort studies in the US. Int J Cancer. 2019.
Rich-Edwards JW, Corsano KA, Stampfer MJ. Test of the National death index and Equifax nationwide death search. Am J Epidemiol. 1994;140(11):1016–9. https://doi.org/10.1093/oxfordjournals.aje.a117191.
Duan P, Hu C, Quan C, Yi X, Zhou W, Yuan M, et al. Body mass index and risk of lung cancer: systematic review and dose-response meta-analysis. Sci Rep. 2015;5:16938. https://doi.org/10.1038/srep16938.
Yang Y, Dong J, Sun K, Zhao L, Zhao F, Wang L, et al. Obesity and incidence of lung cancer: a meta-analysis. Int J Cancer. 2013;132(5):1162–9. https://doi.org/10.1002/ijc.27719.
Zhu H, Zhang S. Body mass index and lung cancer risk in never smokers: a meta-analysis. BMC Cancer. 2018;18(1):635. https://doi.org/10.1186/s12885-018-4543-y.
Lam TK, Moore SC, Brinton LA, Smith L, Hollenbeck AR, Gierach GL, et al. Anthropometric measures and physical activity and the risk of lung cancer in never-smokers: a prospective cohort study. PLoS ONE. 2013;8(8):e70672. https://doi.org/10.1371/journal.pone.0070672.
Kark JD, Yaari S, Rasooly I, Goldbourt U. Are lean smokers at increased risk of lung cancer? The Israel Civil Servant Cancer Study. Arch Intern Med. 1995;155(22):2409–16.
Petersen AMW, Magkos F, Atherton P, Selby A, Smith K, Rennie MJ, et al. Smoking impairs muscle protein synthesis and increases the expression of myostatin and MAFbx in muscle. Am J Physiol Endocrinol Metab. 2007;293(3):E843–8. https://doi.org/10.1152/ajpendo.00301.2007.
Rom O, Kaisari S, Aizenbud D, Reznick AZ. Sarcopenia and smoking: a possible cellular model of cigarette smoke effects on muscle protein breakdown. Ann N Y Acad Sci. 2012;1259(1):47–53. https://doi.org/10.1111/j.1749-6632.2012.06532.x.
Mizoue T, Kasai H, Kubo T, Tokunaga S. Leanness, smoking, and enhanced oxidative DNA damage. Cancer Epidemiol Biomark Prev. 2006;15(3):582–5. https://doi.org/10.1158/1055-9965.epi-05-0658.
Flanders WD, Lally CA, Zhu B-P, Henley SJ, Thun MJ. Lung cancer mortality in relation to age, duration of smoking, and daily cigarette consumption. Results from Cancer Prevention Study II. Cancer Res. 2003;63(19):6556–62.
Zhang X, Liu Y, Shao H, Zheng X. Obesity paradox in lung cancer prognosis: evolving biological insights and clinical implications. J Thorac Oncol. 2017;12(10):1478–88. https://doi.org/10.1016/j.jtho.2017.07.022.
Carreras-Torres R, Johansson M, Haycock PC, Wade KH, Relton CL, Martin RM, et al. Obesity, metabolic factors and risk of different histological types of lung cancer: a Mendelian randomization study. PLoS ONE. 2017;12(6):e0177875. https://doi.org/10.1371/journal.pone.0177875.
Karastergiou K, Smith SR, Greenberg AS, Fried SK. Sex differences in human adipose tissues—the biology of pear shape. Biol Sex Differ. 2012;3(1):13. https://doi.org/10.1186/2042-6410-3-13.
Ntikoudi E, Kiagia M, Boura P, Syrigos KN. Hormones of adipose tissue and their biologic role in lung cancer. Cancer Treat Rev. 2014;40(1):22–30. https://doi.org/10.1016/j.ctrv.2013.06.005.
Creutzberg EC, Schols AM, Bothmer-Quaedvlieg FC, Wouters EF. Prevalence of an elevated resting energy expenditure in patients with chronic obstructive pulmonary disease in relation to body composition and lung function. Eur J Clin Nutr. 1998;52(6):396–401.
Goldkorn T, Filosto S. Lung injury and cancer: mechanistic insights into ceramide and EGFR signaling under cigarette smoke. Am J Respir Cell Mol Biol. 2010;43(3):259–68. https://doi.org/10.1165/rcmb.2010-0220RT.
Khuder SA. Effect of cigarette smoking on major histological types of lung cancer: a meta-analysis. Lung Cancer. 2001;31(2–3):139–48.
Rimm EB, Stampfer MJ, Colditz GA, Chute CG, Litin LB, Willett WC. Validity of self-reported waist and hip circumferences in men and women. Epidemiology. 1990;1(6):466–73. https://doi.org/10.1097/00001648-199011000-00009.
Baracos VE, Reiman T, Mourtzakis M, Gioulbasanis I, Antoun S. Body composition in patients with non-small cell lung cancer: a contemporary view of cancer cachexia with the use of computed tomography image analysis. Am J Clin Nutr. 2010;91(4):1133s–7s. https://doi.org/10.3945/ajcn.2010.28608C.
Acknowledgment
We would like to thank the participants and staff of the NHS and HPFS for their valuable contributions as well as the following state cancer registries for their help: AL, AZ, AR, CA, CO, CT, DE, FL, GA, ID, IL, IN, IA, KY, LA, ME, MD, MA, MI, NE, NH, NJ, NY, NC, ND, OH, OK, OR, PA, RI, SC, TN, TX, VA, WA, WY. The authors assume full responsibility for analyses and interpretation of these data.
Funding
This work was supported by the National Institutes of Health (UM1 CA167552, R01 HL35464, UM1 CA186107, P01 CA87969, and R03 CA223619).
Author information
Authors and Affiliations
Contributions
DHL and ELG contributed to the study design and conception. S-MJ, DHL and ELG drafted the manuscript and the tables. DHL and ELG contributed to the data acquisition and analysis. DHL contributed to the statistical analysis. S-MJ, DHL and ELG critically revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jeong, SM., Lee, D.H. & Giovannucci, E.L. Predicted lean body mass, fat mass and risk of lung cancer: prospective US cohort study. Eur J Epidemiol 34, 1151–1160 (2019). https://doi.org/10.1007/s10654-019-00587-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-019-00587-2