Abstract
Background
Bismuth-containing quadruple therapy is the first-line treatment for eradicating Helicobacter pylori (H. pylori). The optimal duration for H. pylori eradication using bismuth-containing quadruple therapy remains controversial. Therefore, we aimed to compare the clinical effects of the 10- and 14-day bismuth-containing quadruple treatment regimen to eradicate H. pylori.
Methods
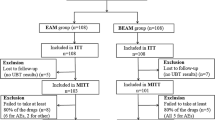
Treatment-naïve patients with H. pylori infection (n = 1300) were enrolled in this multicenter randomized controlled study across five hospitals in China. They were randomized into 10- or 14-day treatment groups to receive bismuth-containing quadruple therapy as follows: vonoprazan 20 mg twice daily; bismuth 220 mg twice daily; amoxicillin 1000 mg twice daily; and either clarithromycin 500 mg twice daily or tetracycline 500 mg four times daily. At least 6 weeks after treatment, we performed a 13C-urea breath test to evaluate H. pylori eradication.
Results
The per-protocol eradication rates were 93.22% (564/605) and 93.74% (569/607) (p < 0.001) and the intention-to-treat eradication rates were 88.62% (576/650) and 89.38% (581/650) (p = 0.007) for the 10- and 14-day regimens, respectively. Incidence of adverse effects was lower in patients who received 10- vs. 14 days of treatment (22.59% vs. 28.50%, p = 0.016). We observed no significant differences in the compliance to treatment or the discontinuation of therapy because of severe adverse effects between the groups.
Conclusion
Compared with the 14-day bismuth-containing quadruple regimens, the 10-day regimen demonstrated a non-inferior efficacy and lower incidence of adverse effects. Therefore, the 10-day regimen is safe and tolerated and could be recommended for H. pylori eradication (NCT05049902).

Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Ren S, Cai P, Liu Y et al. Prevalence of Helicobacter pylori infection in China: A systematic review and meta-analysis. J Gastroenterol Hepatol. 2022;37:464–470. https://doi.org/10.1111/jgh.15751.
Xia C, Dong X, Li H et al. Cancer statistics in China and United States, 2022: profiles, trends, and determinants. Chin Med J (Engl). 2022;135:584–590. https://doi.org/10.1097/cm9.0000000000002108.
Liu WZ, Xie Y, Lu H et al. Fifth Chinese National Consensus Report on the management of Helicobacter pylori infection. Helicobacter. 2018;23:e12475. https://doi.org/10.1111/hel.12475.
Malfertheiner P, Megraud F, O’Morain CA et al. Management of Helicobacter pylori infection-the Maastricht V/Florence Consensus Report. Gut. 2017;66:6–30. https://doi.org/10.1136/gutjnl-2016-312288.
Liou JM, Malfertheiner P, Lee YC et al. Screening and eradication of Helicobacter pylori for gastric cancer prevention: the Taipei global consensus. Gut. 2020;69:2093–2112. https://doi.org/10.1136/gutjnl-2020-322368.
Zhou L, Lu H, Song Z et al. 2022 Chinese national clinical practice guideline on Helicobacter pylori eradication treatment. Chin Med J (Engl). 2022;135:2899–2910. https://doi.org/10.1097/CM9.0000000000002546.
Kato MA-O, Ota H, Okuda MA-O, et al. Guidelines for the management of Helicobacter pylori infection in Japan: 2016 Revised Edition. Helicobacter. 2019.
Jung HK, Kang SJ, Lee YC et al. Evidence-Based Guidelines for the Treatment of Helicobacter pylori Infection in Korea 2020. Gut Liver. 2021;15:168–195. https://doi.org/10.5009/gnl20288.
Ding YM, Li YY, Liu J et al. The cure rate of 10-day bismuth-containing quadruple therapy for Helicobacter pylori eradication is equivalent to 14-day: a systematic review and meta-analysis. Clin Exp Med. 2022. https://doi.org/10.1007/s10238-022-00953-7.
Qiao C, Li Y, Liu J et al. Clarithromycin versus furazolidone for naïve Helicobacter pylori infected patients in a high clarithromycin resistance area. J Gastroenterol Hepatol. 2021;36:2383–2388. https://doi.org/10.1111/jgh.15468.
D’Agostino RB Sr, Massaro JM, Sullivan LM. Non-inferiority trials: design concepts and issues - the encounters of academic consultants in statistics. Stat Med. 2003;22:169–186. https://doi.org/10.1002/sim.1425.
Liu DS, Wang YH, Zeng ZR et al. Primary antibiotic resistance of Helicobacter pylori in Chinese patients: a multiregion prospective 7-year study. Clin Microbiol Infect. 2018;24:e5–e8. https://doi.org/10.1016/j.cmi.2017.11.010.
Han Z, Li Y, Kong Q et al. Efficacy of bismuth for antibiotic-resistant Helicobacter pylori strains eradication: A systematic review and meta-analysis. Helicobacter. 2022;27:e12930. https://doi.org/10.1111/hel.12930.
Qian HS, Li WJ, Dang YN, et al. Ten-Day Vonoprazan-Amoxicillin Dual Therapy as a First-Line Treatment of Helicobacter pylori Infection Compared With Bismuth-Containing Quadruple Therapy. Am J Gastroenterol. 2023;118:627–34. https://doi.org/10.14309/ajg.0000000000002086.
Graham DY. It Is Time for a Paradigm Shift in Design, Execution, and Publishing of Comparative Helicobacter pylori Treatment Trials. Am J Gastroenterol. 2023;118:1154–6. https://doi.org/10.14309/ajg.0000000000002298.
Xu H, Yun J, Li R et al. Antibiotics Resistance Prevalence of Helicobacter pylori Strains in Northwest China. Infect Drug Resist. 2022;15:5519–5528. https://doi.org/10.2147/IDR.S383444.
Shu X, Ye D, Hu C et al. Alarming antibiotics resistance of Helicobacter pylori from children in Southeast China over 6 years. Sci Rep. 2022;12:17754. https://doi.org/10.1038/s41598-022-21661-y.
Kong Q, Li Y, Li R et al. Low compliance to post-screening recommendations in a family-based Helicobacter pylori screening and treatment program: A prospective cohort study. Helicobacter. 2022;27:e12912. https://doi.org/10.1111/hel.12912.
Tsuda M, Asaka M, Kato M, et al. Effect on Helicobacter pylori eradication therapy against gastric cancer in Japan. Helicobacter. 2017;22. https://doi.org/10.1111/hel.12415.
Deguchi H, Uda A, Murakami K. Current Status of Helicobacter pylori Diagnosis and Eradication Therapy in Japan Using a Nationwide Database. Digestion. 2020;101:441–449. https://doi.org/10.1159/000500819.
Gao K, Wu J. National trend of gastric cancer mortality in China (2003–2015): a population-based study. Cancer Commun (Lond). 2019;39:24. https://doi.org/10.1186/s40880-019-0372-x.
Han Y, Yan T, Ma H et al. Cost-Effectiveness Analysis of Helicobacter pylori Eradication Therapy for Prevention of Gastric Cancer: A Markov Model. Dig Dis Sci. 2020;65:1679–1688. https://doi.org/10.1007/s10620-019-05910-1.
Mason J, Axon AT, Forman D et al. The cost-effectiveness of population Helicobacter pylori screening and treatment: a Markov model using economic data from a randomized controlled trial. Aliment Pharmacol Ther. 2002;16:559–568. https://doi.org/10.1046/j.1365-2036.2002.01204.x.
Chiang TH, Chang WJ, Chen SL et al. Mass eradication of Helicobacter pylori to reduce gastric cancer incidence and mortality: a long-term cohort study on Matsu Islands. Gut. 2021;70:243–250. https://doi.org/10.1136/gutjnl-2020-322200.
Graham DY, Shiotani A. New concepts of resistance in the treatment of Helicobacter pylori infections. Nat Clin Pract Gastroenterol Hepatol. 2008;5:321–331. https://doi.org/10.1038/ncpgasthep1138.
Hori Y, Imanishi A, Matsukawa J et al. 1-[5-(2-Fluorophenyl)-1-(pyridin-3-ylsulfonyl)-1H-pyrrol-3-yl]-N-methylmethanamine monofumarate (TAK-438), a novel and potent potassium-competitive acid blocker for the treatment of acid-related diseases. J Pharmacol Exp Ther. 2010;335:231–238. https://doi.org/10.1124/jpet.110.170274.
Jenkins H, Sakurai Y, Nishimura A et al. Randomised clinical trial: safety, tolerability, pharmacokinetics and pharmacodynamics of repeated doses of TAK-438 (vonoprazan), a novel potassium-competitive acid blocker, in healthy male subjects. Aliment Pharmacol Ther. 2015;41:636–648. https://doi.org/10.1111/apt.13121.
Sakurai Y, Nishimura A, Kennedy G et al. Safety, Tolerability, Pharmacokinetics, and Pharmacodynamics of Single Rising TAK-438 (Vonoprazan) Doses in Healthy Male Japanese/non-Japanese Subjects. Clin Transl Gastroenterol. 2015;6:e94. https://doi.org/10.1038/ctg.2015.18.
Chey WD, Mégraud F, Laine L, López LJ, Hunt BJ, Howden CW. Vonoprazan Triple and Dual Therapy for Helicobacter pylori Infection in the United States and Europe: Randomized Clinical Trial. Gastroenterology. 2022;163:608–619. https://doi.org/10.1053/j.gastro.2022.05.055.
Rokkas T, Gisbert JP, Malfertheiner P et al. Comparative Effectiveness of Multiple Different First-Line Treatment Regimens for Helicobacter pylori Infection: A Network Meta-analysis. Gastroenterology. 2021;161:495-507.e4. https://doi.org/10.1053/j.gastro.2021.04.012.
Graham DY, Lu H, Shiotani A. Vonoprazan-containing Helicobacter pylori triple therapies contribution to global antimicrobial resistance. J Gastroenterol Hepatol. 2021;36:1159–1163. https://doi.org/10.1111/jgh.15252.
Gisbert JP. Empirical or susceptibility-guided treatment for Helicobacter pylori infection? A comprehensive review. Therap Adv Gastroenterol. 2020;13:1756284820968736. https://doi.org/10.1177/1756284820968736.
Li P, Jin J, Chen Y, Ma J, Du Q, Han Y. Susceptibility-guided vs. empirical 10-day quadruple treatment for Helicobacter pylori-infected patients: A prospective clinical trial of first-line therapy. Front Microbiol. 2022;13:973975. https://doi.org/10.3389/fmicb.2022.973975.
Hsu PI, Tsai FW, Kao SS et al. Ten-Day Quadruple Therapy Comprising Proton Pump Inhibitor, Bismuth, Tetracycline, and Levofloxacin is More Effective than Standard Levofloxacin Triple Therapy in the Second-Line Treatment of Helicobacter pylori Infection: A Randomized Controlled Trial. Am J Gastroenterol. 2017;11:1374–1381. https://doi.org/10.1038/ajg.2017.195.
Funding
This study was supported by the National Natural Science Foundation of China (82070551 and 81770538), the Taishan Scholars Program of Shandong Province, and the National Clinical Research Center for Digestive Diseases supporting technology project (2015BAI13B07).
Author information
Authors and Affiliations
Contributions
Yu-Ming Ding and Yue-Yue Li designed and planned the study. Miao Duan, Zhong-Xue Han, Xiao-Hui Song, Feng-Lan Zhang, Zhi Wang, Zhang Ning, Shu-yan Zeng, Qing-Zhou Kong, Wen-Lin Zhang, Min-Juan Lin, Bo-Shen Lin, Xue-ping Nan, and Hui Wang collected the data. Jing Liu and Meng Wan performed statistical analysis. Yu-Ming Ding prepared the original draft. Yue-Yue Li, Xiu-Li Zuo, and Yan-Qing Li supported editing of the original draft and critically revised the manuscript. All authors approved the final draft.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial conflict of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the Helsinki Declaration and its later amendments. The study was approved by the Medical Ethics Committee of Qilu Hospital of Shandong University (No. 2021028).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ding, YM., Duan, M., Han, ZX. et al. Bismuth-Containing Quadruple Therapy for Helicobacter pylori Eradication: A Randomized Clinical Trial of 10 and 14 Days. Dig Dis Sci (2024). https://doi.org/10.1007/s10620-024-08460-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10620-024-08460-3