Abstract
Introduction
The development of non-anastomotic biliary strictures (NAS) following orthotopic adult liver transplantation (OLT) is associated with significant morbidity. We performed a systematic review and meta-analysis to identify all prognostic factors for the development of NAS.
Methods
A systematic review was conducted following preferred reporting items for systematic reviews and meta-analyses (PRISMA) and the meta-analysis of observational studies in epidemiology (MOOSE) guidelines. We used the Newcastle–Ottawa scale to assess the quality of the included studies. Using the random-effects model, we calculated the weighted pooled odds ratios (OR), mean differences (MD), hazard ratios (HR), and 95% confidence intervals (CI) of the risk factors.
Results
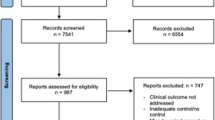
Based on 19 international studies that included a total of 8269 adult LT patients, we calculated an 8% overall incidence of NAS. In this study, 7 potential prognostic factors were associated with a statistically significant hazard ratio for NAS in pooled analyses including (1) DCD donors compared to DBD donors (2) PSC as an indication for a liver transplant (3) Roux-en-Y bile duct reconstruction compared to duct-to-duct reconstruction (4) hepatic artery thrombosis (5) longer cold ischemia time (6) longer warm ischemia time (7) and total operative times.
Conclusion
In this systematic review and meta-analysis, we identified 7 prognostic factors for the development of NAS following OLT. These findings might lay the groundwork for development of diagnostic algorithms to better risk stratify patients at risk for development of NAS.



Similar content being viewed by others
References
Hampe T, Dogan A, Encke J, Mehrabi A, Schemmer P, Schmidt J et al. Biliary complications after liver transplantation. Clin Transplant. 2006;20:93–96.
Buis CI, Verdonk RC, Van der Jagt EJ, van der Hilst CS, Slooff MJH, Haagsma EB et al. Nonanastomotic biliary strictures after liver transplantation, part 1: Radiological features and risk factors for early vs. Late presentation. Liver Transpl. 2007;13:708–718.
Verdonk RC, Buis CI, van der Jagt EJ, Gouw ASH, Limburg AJ, Slooff MJH et al. Nonanastomotic biliary strictures after liver transplantation, part 2: Management, outcome, and risk factors for disease progression. Liver Transplant Off Publ Am Assoc Study Liver Dis Int Liver Transplant Soc. 2007;13:725–732.
Guichelaar MMJ, Benson JT, Malinchoc M, Krom RAF, Wiesner RH, Charlton MR. Risk factors for and clinical course of non-anastomotic biliary strictures after liver transplantation. Am J Transplant Off J Am Soc Transplant Am Soc Transpl Surg. 2003;3:885–890.
Zajko AB, Campbell WL, Logsdon GA, Bron KM, Tzakis A, Esquivel CO et al. Cholangiographic findings in hepatic artery occlusion after liver transplantation. AJR Am J Roentgenol. 1987;149:485–489.
Sankary HN, McChesney L, Hart M, Foster P, Williams J. Identification of donor and recipient risk factors associated with nonanastomotic biliary strictures in human hepatic allografts. Transplant Proc. 1993;25:1964–1967.
Krom RA, Sanchez-Urdazpal L. The biliary tree–the Achilles tendon of liver preservation? Transplantation. 1992;53:1167.
Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement | The BMJ [Internet]. [cited 2022 May 16]. Available from: https://www.bmj.com/content/339/bmj.b2535
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283:2008–12.
Deeks JJ, Dinnes J, D’Amico R, Sowden AJ, Sakarovitch C, Song F, et al. Evaluating non-randomised intervention studies. Health Technol Assess Winch Engl. 2003;7:iii–x, 1–173.
Higgins JPT, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–560.
Dacha S, Barad A, Martin J et al. Association of hepatic artery stenosis and biliary strictures in liver transplant recipients. Liver Transpl. 2011;17:849–854. https://doi.org/10.1002/lt.22298. (PMID: 21455929).
den Dulk AC, Shi X, Verhoeven CJ, et al. (2018) Donor-specific anti-HLA antibodies are not associated with nonanastomotic biliary strictures but both are independent risk factors for graft loss after liver transplantation. Clin Transplant. 32(2). doi: https://doi.org/10.1111/ctr.13163. Epub 12/23/2017. PMID: 29193362.
DeOliveira ML, Jassem W, Valente R, et al. Biliary complications after liver transplantation using grafts from donors after cardiac death: results from a matched control study in a single large volume center. Ann Surg. 2011;254(5):716–22; discussion 722–3. doi: https://doi.org/10.1097/SLA.0b013e318235c572. PMID: 22042467.
Dulaney DT, Dokus KM, McIntosh S et al. Tobacco use is a modifiable risk factor for post-transplant biliary complications. J Gastrointest Surg. 2017;21:1643–1649. https://doi.org/10.1007/s11605-017-3519-6.
Gámán G, Gelley F, Doros A et al. Biliary complications after orthotopic liver transplantation: the Hungarian experience. Transplant Proc. 2013;45:3695–3697. https://doi.org/10.1016/j.transproceed.2013.10.009. (PMID: 24315000).
Gilbo N, Fieuws S, Meurisse N et al. Donor hepatectomy and implantation time are associated with early complications after liver transplantation: a single-center retrospective study. Transplantation. 2021;105:1030–1038. https://doi.org/10.1097/TP.0000000000003335. (PMID: 33052640).
Hoekstra H, Buis CI, Verdonk RC et al. Is Roux-en-Y choledochojejunostomy an independent risk factor for nonanastomotic biliary strictures after liver transplantation? Liver Transpl. 2009;15:924–930. https://doi.org/10.1002/lt.21764. (PMID: 19642122).
Howell JA, Gow PJ, Angus PW et al. Early-onset versus late-onset nonanastomotic biliary strictures post liver transplantation: risk factors reflect different pathogenesis. Transpl Int. 2012;25:765–775. https://doi.org/10.1111/j.1432-2277.2012.01501.x.
Ito T, Botros M, Aziz A et al. Nonanastomotic Biliary Strictures After Liver Transplantation. Am Surg. 2020;86:1363–1367. https://doi.org/10.1177/0003134820964461.
Liu Y, Wang J, Yang P, et al. Delayed rearterialization unlikely leads to nonanastomotic stricture but causes temporary injury on bile duct after liver transplantation. Transpl Int. 2015;28(3):341–51. https://doi.org/10.1111/tri.12490. Epub 12/1/2014. PMID: 25406364; PMCID: PMC4383644.
Mathur AK, Ranney DN, Patel SP et al. The effect of smoking on biliary complications following liver transplantation. Transpl Int. 2011;24:58–66. https://doi.org/10.1111/j.1432-2277.2010.01146.x.
Mocchegiani F, Vincenzi P, Lanari J et al. Immunological risk factors in biliary strictures after liver transplantation. Ann Transplant. 2015;20:218–224. https://doi.org/10.12659/AOT.892393.
Rostved AA, Ostrowski SR, Peters L et al. Hyaluronic acid is a biomarker for allograft dysfunction and predicts 1-year graft loss after liver transplantation. Transplant Proc. 2018;50:3635–3643. https://doi.org/10.1016/j.transproceed.2018.09.018.
Scotté M, Dousset B, Calmus Y et al. The influence of cold ischemia time on biliary complications following liver transplantation. J Hepatol. 1994;21:340–346. https://doi.org/10.1016/s0168-8278(05)80311-3.
Sundaram V, Jones DT, Shah NH et al. Posttransplant biliary complications in the pre- and post-model for end-stage liver disease era. Liver Transpl. 2011;17:428–435. https://doi.org/10.1002/lt.22251.
van Leeuwen OB, van Reeven M, van der Helm D et al. Donor hepatectomy time influences ischemia-reperfusion injury of the biliary tree in donation after circulatory death liver transplantation. Surgery. 2020;168:160–166. https://doi.org/10.1016/j.surg.2020.02.
Zheng BW, Yi SH, Wu T, et al. CEUS detection of biliary ischaemia during the first 4 weeks after liver transplantation predicts non-anastomotic biliary stricture. Clin Hemorheol Microcirc. 2021. https://doi.org/10.3233/CH-211097. Epub ahead of print.
Kohli DR, Harrison ME, Adike AO et al. Predictors of biliary strictures after liver transplantation among recipients of DCD (Donation After Cardiac Death) grafts. Dig Dis Sci. 2019;64:2024–2030. https://doi.org/10.1007/s10620-018-5438-0.
Graziadei IW, Wiesner RH, Batts KP et al. Recurrence of primary sclerosing cholangitis following liver transplantation. Hepatology. 1999;29:1050–1056. https://doi.org/10.1002/hep.510290427.
Fickert P, Pollheimer MJ, Beuers U et al. International PSC Study Group (IPSCSG). Characterization of animal models for primary sclerosing cholangitis (PSC). J Hepatol. 2014;60:1290–303. https://doi.org/10.1016/j.jhep.2014.02.006.
Welling TH, Heidt DG, Englesbe MJ, Magee JC, Sung RS, Campbell DA et al. Biliary complications following liver transplantation in the model for end-stage liver disease era: Effect of donor, recipient, and technical factors. Liver Transpl. 2008;14:73–80.
Akamatsu N, Sugawara Y, Hashimoto D. Biliary reconstruction, its complications and management of biliary complications after adult liver transplantation: a systematic review of the incidence, risk factors and outcome. Transpl Int Off J Eur Soc Organ Transplant. 2011;24:379–392.
Fasullo M, Patel M, Khanna L, Shah T. Post-transplant biliary complications: advances in pathophysiology, diagnosis, and treatment. BMJ Open Gastroenterol. 2022;9:e000778.
Sutton ME, Bense RD, Lisman T et al. Duct-to-duct reconstruction in liver transplantation for primary sclerosing cholangitis is associated with fewer biliary complications in comparison with hepaticojejunostomy. Liver Transpl. 2014;20:457–463. https://doi.org/10.1002/lt.23827.
Fasullo M, Shah T, Zhou H, Siddiqui MS. Post-Transplant Biliary Strictures: An Updated Review. Semin Liver Dis. 2022 Mar 9
Gámán G, Gelley F, Doros A, Zádori G, Görög D, Fehérvári I et al. Biliary complications after orthotopic liver transplantation: the Hungarian experience. Transplant Proc. 2013;45:3695–3697.
Abt P, Crawford M, Desai N, Markmann J, Olthoff K, Shaked A. Liver transplantation from controlled non–heart-beating donors: an increased incidence of biliary complications. Transplantation. 2003;75:1659–1663.
Kalisvaart M, Croome KP, Hernandez-Alejandro R, Pirenne J, Cortés-Cerisuelo M, Miñambres E et al. Donor warm ischemia time in DCD liver transplantation—working group report from the ILTS DCD, liver preservation, and machine perfusion consensus conference. Transplantation. 2021;105:1156–1164.
Lee DD, Li J, Wang G, Croome KP, Burns JM, Perry DK et al. Looking inward: The impact of operative time on graft survival after liver transplantation. Surgery. 2017;162:937–949.
Author information
Authors and Affiliations
Contributions
MF: conception and design; analysis and interpretation of the data; drafting of the article; critical revision of the article for important intellectual content; final approval of the article. SG: conception and design; critical revision of the article for important intellectual content; final approval of the article. WS: conception and design; analysis and interpretation of the data; drafting of the article; critical revision of the article for important intellectual content; final approval of the article. RV: analysis and interpretation of the data; critical revision of the article for important intellectual content; final approval of the article. TC: analysis and interpretation of the data; critical revision of the article for important intellectual content; final approval of the article. TG: analysis and interpretation of the data; critical revision of the article for important intellectual content; final approval of the article. EJ: conception and design; critical revision of the article for important intellectual content; final approval of the article. LK: critical revision of the article for important intellectual content; final approval of the article. Gregory Haber: critical revision of the article for important intellectual content; final approval of the article. TS: conception and design; critical revision of the article for important intellectual content; final approval of the article.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fasullo, M., Ghazaleh, S., Sayeh, W. et al. Prognostic Factors for Non-anastomotic Biliary Strictures Following Adult Liver Transplantation: A Systematic Review and Meta-Analysis. Dig Dis Sci 68, 2683–2694 (2023). https://doi.org/10.1007/s10620-023-07861-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-023-07861-0