Abstract
Background
Texas is the second largest state by area and population in the USA and is reported to have high incidence and mortality rates for hepatocellular carcinoma (HCC). The reasons for the increasingly high burden of HCC in Texas are not clear.
Aims
We explored trends and demographic and regional variations in HCC incidence to better understand reasons for the high burden in Texas.
Methods
We analyzed Texas Cancer Registry incidence data from 2001 to 2015 and compared results to the U.S. National Program of Cancer Registries and SEER for the same period. Rates were stratified by sex, race/ethnicity, and age at diagnosis. Rates were also compared between the US/Mexico border region of Texas and the rest of Texas.
Results
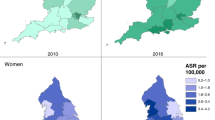
Texas had the highest HCC age-adjusted incidence rate of all states, 13.2/100,000, which was 45% higher than the national average. In Texas and nationally, rates increased by 4% per year between 2001 and 2015. Rates in Texas were 26–37% greater than national rates for Hispanics, African-Americans, and non-Hispanic whites. Among Hispanics in states with the largest percentage of Hispanics, Texas-based Hispanics had the highest HCC incidence rate in 2015 (21.2/100,000) compared with Hispanics in New Mexico, California, Arizona, Nevada, and Florida. Incidence rates were highest in South Texas and US/Mexico border regions.
Conclusions
Increasing rates in the large Hispanic population may explain why Texas now has the highest HCC incidence rate in the USA.

Similar content being viewed by others
Abbreviations
- HCC:
-
Hepatocellular carcinoma
- HCV:
-
Hepatitis C virus
- NAFLD:
-
Nonalcoholic fatty liver disease
- NASH:
-
Nonalcoholic steatohepatitis
References
Kulik L, El-Serag HB. Epidemiology and management of hepatocellular carcinoma. Gastroenterology. 2019;156:477–491.e471.
White DL, Thrift AP, Kanwal F, et al. Incidence of hepatocellular carcinoma in all 50 United States, from 2000 through 2012. Gastroenterology. 2017;152:812–820.e815.
Texas Cancer Registry (www.dshs.state.tx.us/tcr) SEER*Stat Database, 1995–2015 Incidence, Texas statewide, Texas Department of State Health Services, created December 2017, based on NPCR-CSS Submission, cut-off 11/13/17.
National Program of Cancer Registries and Surveillance, Epidemiology, and End Results SEER*Stat Database: NPCR and SEER Incidence—U.S. Cancer Statistics 2001–2015 Public Use Research Database, United States Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute. Released June 2018, based on the November 2017 submission. Accessed at www.cdc.gov/cancer/uscs/public-use.
Xu J. Trends in Liver Cancer Mortality Among Adults Aged 25 and Over in the United States, 2000–2016. NCHS Data Brief 2018:1–8.
Texas Department of State Health Services. Office of Border Public Health 2019. https://www.dshs.texas.gov/borderhealth/. Accessed March 12, 2020.
Kim D, Li AA, Perumpail RB, et al. Disparate trends in mortality of etiology-specific chronic liver diseases among hispanic subpopulations. Clin Gastroenterol Hepatol. 2019;17:1607–1615.e1602.
Rich NE, Oji S, Mufti AR, et al. Racial and ethnic disparities in nonalcoholic fatty liver disease prevalence, severity, and outcomes in the United States: a systematic review and meta-analysis. Clin Gastroenterol Hepatol. 2018;16:198–210.e192.
Kanwal F, Kramer JR, Mapakshi S, et al. Risk of hepatocellular cancer in patients with nonalcoholic fatty liver disease. Gastroenterology. 2018;155:1828–1837.
Kanwal F, Kramer J, Asch SM, et al. Risk of hepatocellular cancer in HCV patients treated with direct-acting antiviral agents. Gastroenterology. 2017;153:996–1005.e1001.
El-Serag HB, Kramer J, Duan Z, et al. Racial differences in the progression to cirrhosis and hepatocellular carcinoma in HCV-infected veterans. Am J Gastroenterol. 2014;109:1427–1435.
Lim U, Monroe KR, Buchthal S, et al. Propensity for intra-abdominal and hepatic adiposity varies among ethnic groups. Gastroenterology. 2019;156:966–975.e910.
Romeo S, Kozlitina J, Xing C, et al. Genetic variation in PNPLA3 confers susceptibility to nonalcoholic fatty liver disease. Nat Genet. 2008;40:1461–1465.
Jiao J, Niu W, Wang Y, et al. Prevalence of aflatoxin-associated TP53R249S mutation in hepatocellular carcinoma in hispanics in south Texas. Cancer Prev Res (Phila). 2018;11:103–112.
Ramirez AG, Munoz E, Parma DL, et al. Lifestyle and clinical correlates of hepatocellular carcinoma in south Texas: a matched case-control study. Clin Gastroenterol Hepatol. 2017;15:1311–1312.
Feng Z, Marrero JA, Khaderi S, et al. Design of the Texas hepatocellular carcinoma consortium cohort study. Am J Gastroenterol. 2019;114:530–532.
Funding
This research was supported by grants from Cancer Prevention Research Institute of Texas (CPRIT) (RP150587) and National Institutes of Health (NIDDK P30DK056338) to HES. The collection of cancer incidence data used in this study was supported by the Texas Department of State Health Services and CPRIT, as part of the statewide cancer reporting program and the Centers for Disease Control and Prevention’s National Program of Cancer Registries Cooperative Agreement # #1NU58DP006308.
Author information
Authors and Affiliations
Contributions
All authors were involved in study design and interpretation of the data and critical revision of manuscript for intellectual content. PM, RS were responsible for the acquisition of the data and statistical analyses. HES, RS, APT, and PM were responsible for drafting the manuscript. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflicts to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
El-Serag, H.B., Sardell, R., Thrift, A.P. et al. Texas Has the Highest Hepatocellular Carcinoma Incidence Rates in the USA. Dig Dis Sci 66, 912–916 (2021). https://doi.org/10.1007/s10620-020-06231-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06231-4