Abstract
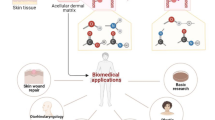
Full-thickness skin wounds occur in many different clinical cases and the use of biological acellular dermal matrices (ADMs) to reconstruct the damaged area is increasing in the field of plastic and reconstructive surgery. In particular, the ability of ADMs to maintain the structural properties of extracellular matrix as well as to provide a suitable environment for cell growth makes their use suitable for the improvement of wound healing and the reduction of side effects deriving from contracture and scar tissue formation. In this study, we describe the clinical use of a recently developed human dermal matrix (HDM) in combination with graft skin as an alternative reconstructive solution for the treatment of full-thickness skin wounds. The HDM was applied in combination with autologous graft skin on three different clinical cases in which full-thickness skin wounds occurred. The clinical outcomes were evaluated in the patients during their follow-up. Histological as well as ultra-structural analysis were also performed on skin biopsy of the clinical case 3 one year after the treatment with HDM. The use of HDM stimulates the wound healing process in all clinical cases of full-thickness skin wounds here described with a functional and aesthetic rescue of the damaged area. Histological and ultra-structural analysis show a regenerative healing of the wound area with well-organized/oriented connective tissue in which cellular infiltration as well as blood vessels are evident. Our results support the clinical use of HDM as a permanent dermal replacement for the treatment of full-thickness skin wounds.



Similar content being viewed by others
References
Askari M, Cohen MJ, Grossman PH, Kulber DA (2011) The use of acellular dermal matrix in release of burn contracture scars in the hand. Plast Reconstr Surg 127:1593–1599. https://doi.org/10.1097/PRS.0b013e31820a6511
Aurora A, McCarron J, Iannotti JP, Derwin K (2007) Commercially available extracellular matrix materials for rotator cuff repairs: state of the art and future trends. J Shoulder Elbow Surg 18:982. https://doi.org/10.1016/j.jse.2007.03.008
Badylak SF (2005) Regenerative medicine and development biology: the role of the extracellular matrix. Anat Rec New Anat 287:36–41. https://doi.org/10.1002/ar.b.20081
Badylak SF, Gilbert TW (2008) Immune response to biologic scaffold materials. Semin Immunol 20:109–116. https://doi.org/10.1016/j.smim.2007.11.003
Bondioli E, Fini M, Veronesi F et al (2014) Development and evaluation of a decellularized membrane from human dermis. J Tissue Eng Regen Med 8:325–336. https://doi.org/10.1002/term.1530
Brennan EP, Reing J, Chew D, Myers-Irvin JM, Young EJ, Badylak SF (2006) Antibacterial activity within degradation products of biological scaffolds composed of extracellular matrix. Tissue Eng 12:2945–2949. https://doi.org/10.1089/ten.2006.12.2949
Brigido SA, Boc SF, Lopez RC (2004) Effective management of major lower extremity wounds using an acellular regenerative tissue matrix: a pilot study. Orthopedics 27(1 Suppl):S145–S149
Brown BN, Badylak SF (2014) Extracellular matrix as an inductive scaffold for functional tissue reconstruction. Transl Res 163:268–285. https://doi.org/10.1016/j.trsl.2013.11.0030
Browne AC, Vearncombe M, Sibbald RG (2001) High bacterial load in asymptomatic diabetic patients with neurotrophic ulcers retards wound healing after application of Dermagraft. Ostomy Wound Manag 47:44–49
Chetty BV, Boissy RE, Warden GD, Nordlund JJ (1992) Basement membrane and fibroblast aberration in blisters at the donor, graft, and spontaneously healed sites in patients with burns. Arch Dermatol 128:181–186
Cohen IK, Diegelmann RF, Lindblad WJ (1992) Wounding healing: biochemical and clinical aspects. WB Saunders Company, Philadelphia
Derwin KA, Baker AR, Spragg RK, Leigh DR, Iannotti JP (2006) Commercial extracellular matrix scaffolds for rotator cuff tendon repair. Biomechanical, biochemical, and cellular properties. J Bone Jt Surg Am 88:2665–2672. https://doi.org/10.2106/JBJS.E.01307
Fini M, Bondioli E, Castagna A et al (2012) Decellularized human dermis to treat massive rotator cuff tears: in vitro evaluations. Connect Tissue Res 53:298–306. https://doi.org/10.3109/03008207.2011.649929
Fosnot J, Kovach SJ 3rd, Serletti JM (2011) Acellular dermal matrix: general principles for the plastic surgeon. Aesthet Surg J 1(7 Suppl):5S–12S. https://doi.org/10.1177/1090820X11417576
Ghetti M, Papa V, Deluca G et al (2017a) Histological and ultrastructural evaluation of human decellularized matrix as a hernia repair device. Ultrastruct Pathol 1:1–7. https://doi.org/10.1080/01913123.2017.1365788
Ghetti M, Bondioli E, Purpura V, Cenacchi G, Ruscelli P, Melandri D (2017b) Decellularized human dermal matrix produced by a skin bank: a new treatment for abdominal wall defects. Ann Ital Chir 5:443–448
Hughes OB, Rakosi A, Macquhae F (2016) A review of cellular and acellular matrix products: indications, techniques and outcomes. Plast Reconstr Surg 138(3 Suppl):138S–147S. https://doi.org/10.1097/PRS.0000000000002643
Ingham E, Matthews J-B, Kearney JN, Gowland G (1993) The effects of variation of cryopreservation protocols on the immunogenicity of allogeneic skin graft. Cryobiology 30:443–458
Jiong C, Jiake C, Chunmao H et al (2010) Clinical application and long-term follow-up study of porcine acellular dermal matrix combined with autoskin grafting. J Burn Care Res 31:280–285. https://doi.org/10.1097/BCR.0b013e3181d0f42d
Livesey S-A, Herndon DN, Hollyoak MA, Atkinson YH, Nag A (1995) Transplanted acellular allograft dermal matrix. Potential as a template for the reconstruction of viable dermis. Transplantation 60:1–9
Mulder G, Wallin K, Tenenhaus M (2012) Regenerative materials that facilitate wound healing. Clin Plast Surg 39:249–267. https://doi.org/10.1016/j.cps.2012.05.006
Perrone AM, Livi A, Fini M et al (2016) A surgical multi-layer technique for pelvic reconstruction after total exenteration using a combination of pedicled omental flap, human acellular dermal matrix and autologous adipose derived cells. Gynecol Oncol Rep 18:36–39. https://doi.org/10.1016/j.gore.2016.10.006
Reing JE, Zhang L, Myers-Irvin J et al (2009) Degradation products of extracellular matrix affect cell migration and proliferation. Tissue Eng Part A 15:605–614. https://doi.org/10.1089/ten.tea.2007.0425
Reyzelman A, Crews RT, Moore JC et al (2009) Clinical effectiveness of an acellular dermal regenerative tissue matrix compared to standard wound management in healing diabetic foot ulcers: a prospective, randomised, multicentre study. Int Wound J 6:196–208. https://doi.org/10.1111/j.1742-481X.2009.00585.x
Rotini R, Marinelli A, Guerra E et al (2011) Human dermal matrix scaffold augmentation for large and massive rotator cuff repairs: preliminary clinical and MRI results at 1-year follow-up. Musculoskelet Surg 95(Suppl 1):S13–S23. https://doi.org/10.1007/s12306-011-0141-8
Shevchenko RV, James SL, James SE (2010) A review of tissue-engineered skin bioconstructs available for skin reconstruction. J R Soc Interface 7:229–258. https://doi.org/10.1098/rsif.2009.0403
Tabata Y (2008) Current status of regenerative medical therapy based on drug delivery technology. Reprod Biomed Online 16:70–80
Valentin JE, Badylak JS, McCabe GP (2006) Extracellular matrix bioscaffolds for orthopaedic applications. A comparative histologic study. J Bone Jt Surg Am. 88:2673–2686. https://doi.org/10.2106/JBJS.E.01008
Vorotnikova E, McIntosh D, Dewilde A et al (2010) Extracellular matrix-derived products modulate endothelial and progenitor cell migration and proliferation in vitro and stimulate regenerative healing in vivo. Matrix Biol 29:690–700. https://doi.org/10.1016/j.matbio.2010.08.007
Wainwright DJ (1995) Use of an acellular allograft dermal matrix (AlloDerm) in the management of full-thickness burns. Burns 21:243–248
Wainwright DJ, Bury SB (2011) Acellular dermal matrix in the management of the burn patient. Aesthet Surg J 31(7 Suppl):13S–23S. https://doi.org/10.1177/1090820X11418202
Wainwright D, Madden M, Luterman A et al (1996) Clinical evaluation of an acellular allograft dermal matrix in full-thickness burns. J Burn Care Rehabil 17:124–136
Walden JL, Garcia H, Hawkins H et al (2000) Both dermal matrix and epidermis contribute to an inhibition of wound contraction. Ann Plast Surg 45:162–166
Yim H, Cho YS, Seo CH et al (2010) The use of AlloDerm on major burn patients: AlloDerm prevents post-burn joint contracture. Burns 36:322–328. https://doi.org/10.1016/j.burns.2009.10.018
Zheng MH, Chen J, Kirilak Y, Willers C, Xu J, Wood D (2005) Porcine small intestine submucosa (SIS) is not an acellular collagenous matrix and contains porcine DNA: possible implications in human implantation. J Biomed Mater Res B Appl Biomater 73:61–67. https://doi.org/10.1002/jbm.b.30170
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interests.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bondioli, E., Purpura, V., Orlandi, C. et al. The use of an acellular matrix derived from human dermis for the treatment of full-thickness skin wounds. Cell Tissue Bank 20, 183–192 (2019). https://doi.org/10.1007/s10561-019-09755-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10561-019-09755-w