Abstract
Mechanical ventilation in prone position is a strategy that increases oxygenation and reduces mortality in severe ARDS. The hemodynamic and cardiovascular assessment of these patients is essential. Transthoracic echocardiography (TTE) is a widely used tool to assess hemodynamics in critical care, but the prone position is thought to limit adequate TTE views and goal-oriented measurements. The aim of this study is to show the feasibility of the hemodynamic assessment by transthoracic echocardiography during prone position ventilation (PPV). This is a retrospective, observational study, carried out in the intensive care unit (ICU) of a tertiary-care center in Buenos Aires, Argentina. We included all the adult patients admitted to the ICU between March 2020 and August 2021 who had a TTE examination in PPV due to ARDS. During the study period, we evaluated by TTE a total of 35 patients requiring PPV. The vast majority of the patients had COVID-19 pneumonia (91.4%). In 33 out of 35 (94.3%) cases, it was able to achieve an adequate apical four chamber view. We assessed qualitatively the systolic function of left ventricle (LV) and right ventricle (RV) in all of the successfully evaluated patients. We measured the RV basal diameter (94.3%), RV/LV ratio (77.1%), tricuspid annular plane systolic excursion (TAPSE) (91.4%), and septal mitral annular plane systolic excursion (MAPSE) (88.5%) in most of them. Also, we quantified the left ventricle outflow tract velocity time integral (LVOT VTI) in a large part (68.5%) of the examinations. Transthoracic echocardiography is a useful tool for the hemodynamic assessment of patients in prone position under mechanical ventilation.
Similar content being viewed by others
Introduction
Prone position ventilation (PPV) improves oxygenation and reduces mortality in severe or moderate-to-severe acute respiratory distress syndrome (ARDS) [1]. The survival benefit is likely related to a more homogeneous lung ventilation and reduced ventilator-induced lung injury (VILI). Current guidelines recommend prone positioning for a prolonged period of time in adult patients with ARDS and deep hypoxemia [2, 3]. Despite the evidence, the adoption of this maneuver in daily practice used to be low [4, 5], but in recent years it has been widely adopted due to the COVID-19 related ARDS (C-ARDS) [6,7,8].
The hemodynamic assessment of prone patients is crucial for everyday practice but may be challenging. It can be performed with right heart catheterization, transpulmonary thermodilution measurements, or echocardiography. Critical care echocardiography (CCE) is a well-established tool for cardiac function and volume status assessment [9]. Transthoracic echocardiography (TTE) is the most common approach in the critical care setting but, transesophageal echocardiography (TEE) has been advocated during prone position in ARDS patients in terms of image quality and safety [10]. Several limitations arise with the transesophageal route, including the availability of the TEE probe, costs, and specific training [9]. Moreover, early in the COVID-19 pandemic, there were concerns regarding the echocardiographer’s safety during the TEE examination [11].
In the clinical context of C-ARDS, with a large population of mechanically ventilated patients in the prone position, the feasibility of performing TTE as a routine assessment has a crescent interest [12,13,14].
In this study, we reported our experience with TTE as a pragmatic, goal-oriented approach in PPV during the COVID-19 pandemic.
Materials and methods
This is a retrospective, observational study, carried out in the 20 medical-surgical bed ICU of a tertiary-care center in Buenos Aires, Argentina (Sanatorio de los Arcos), between March 2020 and August 2021. The Institutional Review Board (Comité de Ética en Investigación, Clínica y Maternidad Suizo-Argentina) approved the study protocol (approval number 6518) and waived the requirement for informed consent.
Study population
We included all the adult (≥ 18 years old) patients admitted to the ICU between March 2020 and August 2021 who had a TTE examination in PPV due to ARDS.
ARDS was diagnosed according to the Berlin definition [15]. Prone ventilation was strongly recommended in patients who met the PROSEVA criteria [1].
Intervention
As this is a pragmatic study carried out in the COVID-19 pandemic with work overload and staff shortening, the decision to perform a TTE examination in prone position was at physician discretion. We also attempted to reduce the exposition time inside the patient’s room; hence the main objective was to perform a goal-oriented TTE examination.
We used a Philips Envisor HD or Sparq ultrasound machine (Philips Healthcare, Bothell, WA, USA) with a phased array S2-4 probe. All the studies were performed by a board-certified intensivist in critical care ultrasonography and echocardiography (IC).
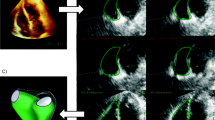
All the patients were in the “swimmer” position. We did not make any specific adjustments to the patient bed or position. The ultrasound machine was located to the left of the prone patient. The probe was placed at the 5th–6th intercostal space, at the apex beat, between the left middle clavicular line and left anterior axillary line. The mark of the probe pointed towards cephalic and dorsal until it was possible to visualize in B mode an apical four chamber view. The five apical chambers view was obtained by slightly tilting the transducer’s tail towards the dorsal region (Figs. 1, 2).
The primary objective was to perform a qualitative assessment of the LV and RV function. In all cases, an attempt was made to measure the LV and RV basal diameters and its ratio, the mitral annular plane systolic excursion (MAPSE), and the tricuspid annular plane systolic excursion (TAPSE). According to individual situations, we additionally measured transmitral E and A wave, lateral and septal mitral annulus e′ wave, E/e′ ratio, and the S′ wave of the lateral tricuspid annulus. On a case-by-case basis, if a tricuspid regurgitation flow could be identified by color Doppler, we used continuous Doppler (CW) to estimate the pulmonary artery systolic pressure (PASP) using Bernoulli’s formula. In the apical five chamber view, we systematically measured the velocity time integral (VTI) of the left ventricle outflow tract (LVOT) if its flow was correctly aligned (Figs. 3, 4).
Left ventricle assesment in prone position. A M mode measurement of lateral MAPSE in an apical four chamber view B PW at the LVOT above the aortic valve in the apical five chamber view with its VTI measurement. C PW at the transmitral flow in the apical four chamber view measuring of E and A waves velocities. D TDI measuring e’ wave velocity at the septal border of the mitral ring in an apical four chamber view
Right ventricle assesment in prone position. A Measurement of the right and left ventricles basal diameter in B mode in an apical four chamber view. B M mode measurement of TAPSE in an apical four chamber view. C S′ wave velocity at the tricuspid ring in an apical four chamber view by TDI D CW at the tricuspid regurgitation flow measuring the peak velocity in an apical four chamber view
Data collection
We collected the following variables from the electronic medical records: age, gender, comorbidities, diagnosis at admission, APACHE II score, respiratory parameters, vasopressor support, and in-hospital mortality.
The LV and RV basal diameter, LV systolic and diastolic function, the LVOT VTI, RV systolic function, and presence of valvular disease were obtained from the recorded images of ultrasonographic studies.
Statistical analysis
The data was analyzed with MedCalc® Statistical Software version 20.011 (MedCalc Software Ltd, Ostend, Belgium; https://www.medcalc.org; 2021). The frequencies and distribution of qualitative variables were expressed in absolute quantity and percentage, while quantitative variables were expressed as median and interquartile range. An exploratory analysis comparing groups of categorical variables was done with Chi-square test. A p-value less than 0.05 was considered statistically significant for all comparisons.
Results
From March 2020 to August 2021, a total of 93 ARDS patients underwent PPV. Of these, 35 patients (38%) were evaluated by TTE (Table 1). The median age was 56 (47–69) years, with a clear predominance of male subjects (80%). The most frequent comorbidities were arterial hypertension, obesity, dyslipidemia, smoking and diabetes. The cause of ARDS was COVID-19 pneumonia (C-ARDS) in the vast majority of cases (91.4%). The in-hospital mortality was 51.4%, with a median APACHE II score of 16 (12–20).
Most of the patients had suitable views for echocardiographic assessment. Overall, in 94.3% of the patients, it was possible to obtain an apical four chambers view and in 68.5% of the examinations, the apical five chambers view was satisfactory enough for LVOT VTI quantification.
The LV and RV systolic function was qualitatively assessed in the vast majority of the patients. Regarding the quantitative assessment, the septal MAPSE was measured more frequently (88.5%) than the lateral MAPSE (57.1%). The TAPSE was obtained in 91.4% of the patients. In most of the patients, we were able to measure the LVOT VTI and the RV/LV diameter. We assessed the diastolic LV function through the E and A wave ratio in more than half of the study population. Only 14.2% of the patients presented mild tricuspid regurgitation flow by color Doppler that allowed PASP estimation. Given the potential impact of obesity in the echocardiographic quality image, we performed an exploratory analysis of the feasibility of obtaining the echocardiographic variables in obese patients compared to non-obese patients with no statistical significance. Table 2 describes the number of measurements of echocardiographic variables and its comparison between obese and non-obese patients.
In our study, 30 of the patients had a preserved LV systolic function, while two had moderate to severe impairment. The median LVOT VTI was 20.6 (18.3–24.2) cm. All evaluated patients (94.3%) had a preserved RV systolic function (“eyeball”). The median value of RV/LV ratio was 0.8 (0.7–0.9). The TAPSE was 2.0 (1.8–2.2) cm and the tricuspid lateral ring S’ wave was 11.6 (10.6–13.6) cm/sec. In none of the cases pericardial effusion or significant valvulopathies were found. The characteristics of echocardiographic variables are described in Table 3.
Discussion
The rate of PPV in ARDS was low for years, in spite of its benefits on gas exchange and mortality. In recent years, it has been steeply offered to mechanically ventilated patients with C-ARDS. Prone ventilation similarly improves oxygenation in C-ARDS and non-C-ARDS patients, but mortality remains high (45%) in both [6, 16]
The critical condition of these patients requires careful hemodynamic monitoring. In an international survey, more than half of the COVID-19 ICU patients (54%) had an echocardiographic examination performed, mostly with a transthoracic approach (97%) [17].
Due to the interposition of the air-filled lungs between the heart and the thoracic wall, mechanical ventilated patients proposed a challenge for TTE assessment, especially obese and prone patients. In those circumstances, a TEE assessment is recommended given the improvement in quality image [10]. Nevertheless, its implementation has inherent difficulties that were accentuated by the COVID-19 pandemic: the probe is not available in many of the ICUs, a TEE trained physician is needed, has higher risk of aerosol generation, and require high workload including proper equipment sterilization and longer exposure to the patient’s infected particles [9, 11, 18].
As we do not have at disposal a TEE probe, we have been performing TTE assessment in PPV patients since 2015. Its practice and implementation increased considerably since 2020 with C-ARDS.
The objective of the study was not to measure the largest number of echocardiographic variables but to adopt a pragmatic and point of care approach in accordance with the catastrophic health situation with scarce resources. We had in consideration to limit the exposure time of the sonographer and to not create excessive burden given the staff shortage, as posed at the beginning of the pandemic [11, 19].
In our study, a transthoracic echocardiographic assessment was feasible in 94.3% of the evaluated patients. In them, we obtained a qualitative LV and RV systolic function assessment and in most of the examinations, we measured the LV/RV ratio. These findings are similar to the ones previously reported [12,13,14].
The LVOT VTI was quantified in 68.5% of the patients, limited due to impediment obtaining an apical five-chamber view. The quantitative LV systolic assessment by MAPSE was slightly lower than previous studies, mainly regarding the lateral MAPSE (57.1%). This may be explained because in some of our examinations we experienced difficulties obtaining a proper view of the LV’s lateral free wall. Unlike some authors, we did not implement any specific maneuver to enhance our echocardiographic views. Giustiniano et al. deflated the lower thoracic sector of the air-mattress to place the probe and Ugalde et al. elevated the left shoulder with a pillow to create a space to fit in the transducer [14,15,16,17,18,19,20].
Considering that the obese population often present a challenge to obtain a good quality echocardiographic image, even as outpatients [21, 22], we performed an exploratory analysis comparing our echocardiographic measurements among obese and non-obese patients. There was no difference of statistical significance in this small series of cases.
The evaluation of the RV focused on the visual estimation of its systolic function, the measurement of the RV/LV basal diameter ratio, TAPSE in most cases, and the S′ wave in some, acknowledging that there is active research on the best assessment of this topic [23,24,25,26,27].
Our study shows that transthoracic echocardiography in prone position ventilation is feasible. It is a non-invasive, reproducible, and readily-available method that could be the preferred first tier assessment of the PPV patients.
We acknowledge several limitations in our research, principally due to its retrospective design. We were not able to control confounders or compare measurements. We performed TTE studies in only 38% of the prone ventilated patients during the study period, so a selection bias cannot be ruled out. We could not applied to the PRICES recommendation for reporting CCE data [28]; rather than having a protocol for exhaustive quantitative assessments, we used a goal-oriented TTE examination. As described in a recent systematic review of the literature, this circumstance was not unusual while depicting echocardiographic findings from COVID-19 patients [29]. Moreover, that study found a heterogeneous approach to data reporting, with the larger study included providing mainly qualitative information [30].
Nevertheless, we think this limited evaluation reflects real life care in several ICUs due to excessive workload and staff shortage.
Conclusion
Transthoracic echocardiography assessment could be used, even in suboptimal conditions, as an initial hemodynamic assessment of mechanical ventilated patients in prone position. In most cases, it allows to evaluate the LV and RV systolic function and the measurement of LVOT VTI as a surrogate of the SV.
References
Guérin C, Reignier J, Richard J-C, Beuret P, Gacouin A, Boulain T et al (2013) Prone positioning in severe acute respiratory distress syndrome. N Engl J Med 368(23):2159–68. https://doi.org/10.1056/NEJMoa1214103
Fan E, Del Sorbo L, Goligher EC, Hodgson CL, Munshi L, Walkey AJ et al (2017) An official American Thoracic Society/European Society of Intensive Care Medicine/society of critical care medicine clinical practice guideline: mechanical ventilation in adult patients with acute respiratory distress syndrome. Am J Respir Crit Care Med 195(9):1253–1263. https://doi.org/10.1164/rccm.201703-0548ST
Papazian L, Aubron C, Brochard L, Chiche J-D, Combes A, Dreyfuss D et al (2019) Formal guidelines: management of acute respiratory distress syndrome. Ann Intensive Care 9(1):69. https://doi.org/10.1186/s13613-019-0540-9
Bellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A et al (2016) Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA 315(8):788. https://doi.org/10.1001/jama.2016.0291
Guérin C, Beuret P, Constantin JM, Bellani G, Garcia-Olivares P, Roca O et al (2018) A prospective international observational prevalence study on prone positioning of ARDS patients: the APRONET (ARDS prone position network) study. Intensive Care Med 44(1):22–37. https://doi.org/10.1007/s00134-017-4996-5
Ferrando C, Mellado-Artigas R, Gea A, Arruti E, Aldecoa C, Bordell A et al (2020) Características, evolución clínica y factores asociados a la mortalidad en UCI de los pacientes críticos infectados por SARS-CoV-2 en España: estudio prospectivo, de cohorte y multicéntrico. Rev Esp Anestesiol Reanim 67(8):425–37
Langer T, Brioni M, Guzzardella A, Carlesso E, Cabrini L, Castelli G et al (2021) Prone position in intubated, mechanically ventilated patients with COVID-19: a multi-centric study of more than 1000 patients. Crit Care 25(1):128. https://doi.org/10.1186/s13054-021-03552-2
Estenssoro E, Loudet CI, Ríos FG, Kanoore Edul VS, Plotnikow G, Andrian M et al (2021) Clinical characteristics and outcomes of invasively ventilated patients with COVID-19 in Argentina (SATICOVID): a prospective, multicentre cohort study. Lancet Respir Med 9(9):989–998
Vieillard-Baron A, Millington SJ, Sanfilippo F, Chew M, Diaz-Gomez J, McLean A et al (2019) A decade of progress in critical care echocardiography: a narrative review. Intensive Care Med 45(6):770–788. https://doi.org/10.1007/s00134-019-05604-2
Mekontso Dessap A, Proost O, Boissier F, Louis B, Roche Campo F, Brochard L (2011) Transesophageal echocardiography in prone position during severe acute respiratory distress syndrome. Intensive Care Med 37(3):430–4. https://doi.org/10.1007/s00134-010-2114-z
Kirkpatrick JN, Mitchell C, Taub C, Kort S, Hung J, Swaminathan M (2020) ASE statement on protection of patients and echocardiography service providers during the 2019 novel coronavirus outbreak: endorsed by the American College of Cardiology. J Am Soc Echocardiogr 33(6):648–53
García-Cruz E, Manzur-Sandoval D, Gopar-Nieto R, Murillo-Ochoa AL, Bejarano-Alva G, Rojas-Velasco G et al (2020) Transthoracic echocardiography during prone position ventilation: lessons from the COVID-19 pandemic. J Am Coll Emerg Physicians Open 1(5):730–736
Gibson LE, Di Fenza R, Berra L, Bittner EA, Chang MG (2020) Transthoracic echocardiography in prone patients with acute respiratory distress syndrome: a feasibility study. Crit Care Explor 2(8):e0179. https://doi.org/10.1097/CCE.0000000000000179
Giustiniano E, Padua E, Negri K, Bragato RM, Cecconi M (2020) Echocardiography during prone-position mechanical ventilation in patients with COVID-19: a proposal for a new approach. J Am Soc Echocardiogr 33(7):905–6
Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, Camporota L, Slutsky ASADTF (2012) Acute respiratory distress syndrome: the Berlin definition. JAMA. https://doi.org/10.1001/jama.2012.5669
Camporota L, Sanderson B, Chiumello D, Terzi N, Argaud L, Rimmelé T et al (2021) Prone position in coronavirus disease 2019 and noncoronavirus disease 2019 acute respiratory distress syndrome. Crit Care Med. https://doi.org/10.1097/CCM.0000000000005354
Michard F, Malbrain ML, Martin GS, Fumeaux T, Lobo S, Gonzalez F et al (2020) Haemodynamic monitoring and management in COVID-19 intensive care patients: an international survey. Anaesth Crit Care Pain Med 39(5):563–9
Taha HS, Mohamed AM, Mahrous HA, Shaker MM, Alsayed OS, Sayed HG et al (2021) Correlation of echocardiographic parameters in prone and supine positions in normal adults using a novel approach. Echocardiography 38(6):892–900. https://doi.org/10.1111/echo.15072
Ward RP, Lee L, Ward TJ, Lang RM (2020) Utilization and appropriateness of transthoracic echocardiography in response to the COVID-19 pandemic. J Am Soc Echocardiogr 33(6):690–1. https://doi.org/10.1016/j.echo.2020.04.006
Ugalde D, Medel JN, Romero C, Cornejo R (2018) Transthoracic cardiac ultrasound in prone position: a technique variation description. Intensive Care Med 44(6):986–7. https://doi.org/10.1007/s00134-018-5049-4
El Hajj MC, Litwin SE (2020) Echocardiography in the era of obesity. J Am Soc Echocardiogr 33(7):779–87. https://doi.org/10.1016/j.echo.2020.03.009
Finkelhor RS, Moallem M, Bahler RC (2006) Characteristics and impact of obesity on the outpatient echocardiography laboratory. Am J Cardiol 97(7):1082–1084
Gonzalez F, Gomes R, Bacariza J, Michard F (2021) Could strain echocardiography help to assess systolic function in critically ill COVID-19 patients? J Clin Monit Comput 35(5):1229–34. https://doi.org/10.1007/s10877-021-00677-1
Vieillard-Baron A, Prigent A, Repessé X, Goudelin M, Prat G, Evrard B et al (2020) Right ventricular failure in septic shock: characterization, incidence and impact on fluid responsiveness. Crit Care 24(1):4–11
Zhang H, Huang W, Zhang Q, Chen X, Wang X, Liu D (2021) Prevalence and prognostic value of various types of right ventricular dysfunction in mechanically ventilated septic patients. Ann Intensive Care 11(1):108. https://doi.org/10.1186/s13613-021-00902-9
Gibson LE, Di FR, Lang M, Capriles MI, Li MD, Kalpathy-Cramer J et al (2021) Right ventricular strain is common in intubated COVID-19 patients and does not reflect severity of respiratory illness. J Intensive Care Med 36(8):900–9. https://doi.org/10.1177/08850666211006335
Chotalia M, Ali M, Alderman JE, Kalla M, Parekh D, Bangash MN et al (2021) Right ventricular dysfunction and its association with mortality in coronavirus disease 2019 acute respiratory distress syndrome. Crit Care Med 49(10):1757–68. https://doi.org/10.1097/CCM.0000000000005167
Sanfilippo F, Huang S, Herpain A, Balik M, Chew MS, Clau-Terré F et al (2021) The PRICES statement: an ESICM expert consensus on methodology for conducting and reporting critical care echocardiography research studies. Intensive Care Med 47(1):1–13. https://doi.org/10.1007/s00134-020-06262-5
Messina A, Sanfilippo F, Milani A, Calabrò L, Negri K, Monge García MI et al (2021) COVID-19-related echocardiographic patterns of cardiovascular dysfunction in critically ill patients: a systematic review of the current literature. J Crit Care 65:26–35
Dweck MR, Bularga A, Hahn RT, Bing R, Lee KK, Chapman AR et al (2020) Global evaluation of echocardiography in patients with COVID-19. Eur Hear J Cardiovasc Imaging 21(9):949–58
Acknowledgements
We thank the critical care team from Sanatorio de los Arcos.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization: IC; Methodology: IC, VOC, RAG; Formal analysis and investigation: IC, VOC, RAG; Writing—original draft preparation: IC; Writing—review and editing: IC, VOC, RAG; Supervision: RAG, PMM, FMT.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cheong, I., Otero Castro, V., Gómez, R.A. et al. Transthoracic echocardiography of patients in prone position ventilation during the COVID-19 pandemic: an observational and retrospective study. Int J Cardiovasc Imaging 38, 2303–2309 (2022). https://doi.org/10.1007/s10554-022-02659-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-022-02659-z