Abstract
Purpose
There is limited information about the dietary habits associated with stomach adenocarcinoma in the Brazilian population, so our purpose is to analyze the consumption of processed and ultra-processed foods by patients with stomach adenocarcinoma in Brazil.
Methods
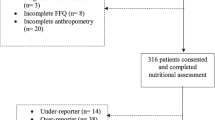
A multicentric hospital-based case–control study was conducted in São Paulo (southeastern region) and Belém (Amazon region) of Brazil with 1,045 individuals, both sexes, between 18 and 75 years old. In São Paulo, there were 214 cases with stomach adenocarcinoma and 150 controls patients submitted to stomach endoscopy named as Group I (without any pre-malignant gastric disease) and the Healthy Controls (Group 2) comprised 401 individuals matched by age and sex from the prevention unit at A.C .Camargo Cancer Center. In Belém, it has two groups one are cases 140 and second 140 hospital controls, recruited in outpatient clinics. Lifestyle and food frequency questionnaires (FFQ) were administered in cases and controls in both places. Univariate and multivariable binomial logistic regression analyses were performed.
Results
In São Paulo, cases reported two times greater consumption of processed meat (adjusted OR 2.56, 95% CI 1.32–4.96) and of sweets (≥ 80 g/day) than Group 1 (endoscopic controls) (adjusted OR 2.25, 95% CI 1.21–4.18). Compared with Group 2, processed food consumption (≥ 44 g/day) as well as ≥ 44 g/day of salted bread increased the odds of having stomach adenocarcinoma (adjusted OR 2.96, 95% CI 1.82–4.81 and adjusted OR 2.03, 95% CI 1.30–3.18), respectively. In Belém, individuals who reported consuming ≥ 166 g/day of fried and roasted meat and fish were more likely to have stomach adenocarcinoma (adjusted OR 2.21, 95% CI 1.13–4.30).
Conclusions
In both cities, consumption of processed and ultra-processed foods, especially salted bread, yellow cheese, fried and roasted meats, fish fried, processed meat, and sweets, was independently associated with the chance of having stomach adenocarcinoma.

Similar content being viewed by others
Data availability
Data will be made available on reasonable request.
Code availability
Not applicable.
References
Ferlay J, Ervik M, Lam F, Colombet M, Mery L, Piñeros M, Znaor A, Soerjomataram I, Bray F (2020). Global Cancer Observatory: Cancer Today. Lyon, France: International Agency for Research on Cancer. Available from: https://gco.iarc.fr/today (accessed 09 April 2021).
Ministry of Health of Brazil (2021) José Alencar Gomes da Silva National Cancer Institute. Estimate 2020–2022: Cancer incidence in Brazil. Rio de Janeiro. INCA
Curado MP, Silva DRME, Oliveira MM, Soares F, Begnami MD, Coimbra FJF, Assumpção PP, de Sant’Ana RO, Demachki S, Dias-Neto E (2019) Disparities in Epidemiological Profile of Gastric Adenocarcinoma in Selected Cities of Brazil. Asian Pac J Cancer Prev 20:2253–2258. https://doi.org/10.31557/APJCP.2019.20.8.2253
Guimarães RM, Muzi CD (2012) Trend of mortality rates for gastric cancer in Brazil and regions in the period of 30 years (1980–2009). Arq Gastroenterol 49:184–188. https://doi.org/10.1590/S0004-28032012000300003
Giusti ACBS, Salvador PTO, Dos Santos J, Meira KC, Camacho AR, Guimarães RM, Souza DL (2016) Trends and predictions for cancer mortality in Brazil. World J Gastroenterol 22:6527–6538. https://doi.org/10.3748/wjg.v22.i28.6527
Guerra MR, Bustamante-Teixeira MT, Corrêa CSL, Abreu DMX, Curado MP, Mooney M, Naghavi M, Teixeira R, França EB, Malta DC (2017) Magnitude and variation of the burden of cancer mortality in Brazil and Federation Units, 1990 and 2015. Rev Bras Epidemiol 20:102–115. https://doi.org/10.1590/1980-5497201700050009
World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Expert Report 2018. Diet, nutrition, physical activity and stomach cancer. Available from: dietandcancerreport.org (accessed 10 Abril 2020).
Ministry of Health of Brazil. Health Care Secretariat. Department of Primary Care. Food guide for the Brazilian population. Brasília: Ministry of Health of Brazil, 2014. Available from: http://www.fao.org/nutrition/education/food-based-dietary guidelines/regions/countries/brazil/en/ (accessed 13 March 2020).
Monteiro C, Levy R, Claro R, De Castro I, Cannon G (2010) Increasing consumption of ultra-processed foods and likely impact on human health: Evidence from Brazil. Public Health Nutr 14:5–13. https://doi.org/10.1017/S1368980010003241
Monteiro CA, Cannon G, Moubarac J-C et al (2018) The UN Decade of Nutrition, the NOVA food classification and the trouble with ultra-processing. Public Health Nutr 21:5–17
[WHO] World Health Organization. Health topics: cancer. 2018 Avaliable from: <URL:http://www.who.int/topics/cancer/en/> (accessed 20 April 2020)
Lameza MMS. Validação de questionário de frequência alimentar para pacientes tratados de câncer colorretal. São Paulo; 2010. [Master's Dissertation-Antônio Prudente Foundation]
Bagley SC, White H, Golomb BA (2001) Logistic regression in the medical literature: standards for use and reporting, with particular attention to one medical domain. J Clin Epidemiol 54(10):979–985. https://doi.org/10.1016/s0895-4356(01)00372-9 (PMID: 11576808)
Kumar R, Chhabra P (2014) Cautions required during planning, analysis and reporting of multivariable logistic regression. Current Medicine Research and Practice 4(1):31–39. https://doi.org/10.1016/j.cmrp.2014.01.004
Luiten CM, Steenhuis IH, Eyles H, Ni Mhurchu C, Waterlander WE (2016) Ultra-processed foods have the worst nutrient profile, yet they are the most available packaged products in a sample of New Zealand supermarkets–CORRIGENDUM. Public Health Nutr 19:539. https://doi.org/10.1017/S1368980015002840pmid:26419699
Adams J, White M (2015) Characterisation of UK diets according to degree of food processing and associations with socio-demographics and obesity: cross-sectional analysis of UK National Diet and Nutrition Survey (2008–12). Int J Behav Nutr Phys Act 12:160. https://doi.org/10.1186/s12966-015-0317-ypmid:26684833
Cediel G, Reyes M, da Costa Louzada ML et al (2018) Ultra-processed foods and added sugars in the Chilean diet (2010). Public Health Nutr 21:125–133. https://doi.org/10.1017/S1368980017001161pmid:28625223
Martínez E, Baraldi LG, Louzada ML, Moubarac JC, Mozaffarian D, Monteiro CA (2016) Ultra-processed foods and added sugars in the US diet evidence from a nationally representative cross-sectional study. BMJ Open. https://doi.org/10.1136/bmjopen-2015-009892pmid:26962035
Moubarac JC, Martins AP, Claro RM, Levy RB, Cannon G, Monteiro CA (2013) Evidence from Canada: consumption of ultra-processed foods and likely impact on human health. Public Health Nutr 16:2240. https://doi.org/10.1017/S1368980012005009pmid:23171687
Moubarac JC, Batal M, Louzada ML, Martinez Steele E (2017) Monteiro CA Consumption of ultra-processed foods predicts diet quality in Canada. Appetite 108:512–520. https://doi.org/10.1016/j.appet.2016.11.006pmid:27825941
Rauber F, Steele EM, Louzada MLC, Millet C, Monteiro CA, Levy RB (2020) Ultra-processed food consumption and indicators of obesity in the United Kingdom population (2008–2016). Plos Ones. 15(5):232676. https://doi.org/10.1371/journal.pone.0232676
Fiolet T, Srour B, Sellem L et al (2018) Consumption of ultra-processed foods and cancer risk: results from NutriNet-Santé prospective cohort. BMJ 360:322. https://doi.org/10.1136/bmj.k322
Monteiro C, Cannon G, Levy R, Moubarac J, Louzada M, Rauber F, Jaime P (2019) Ultra-processed foods: What they are and how to identify them. Public Health Nutr 22:936–941. https://doi.org/10.1017/S1368980018003762
Costa Louzada ML, Martins AP, Canella DS et al (2015) Ultra-processed foods and the nutritional dietary profile in Brazil. Rev Saude Publica 49:38. https://doi.org/10.1590/S0034-8910.2015049006132
Ferguson LR (2010) Meat and cancer. Meat Sci 84:308–313. https://doi.org/10.1016/j.meatsci.2009.06.032
Fisberg M, Kovalskys I, Gómez G, Rigotti A, Sanabria LY, García MC, Torres RG, Herrera-Cuenca M, Zimberg IZ, Koletzko B, Pratt M (2018) Total and added sugar intake: assessment in eight Latin American countries. Nutrients 10:389. https://doi.org/10.3390/nu10040389
Carvalho AM, César CL, Fisberg RM, Marchioni DM (2014) Meat consumption in São Paulo-Brazil: trend in the last decade. PLoS ONE. https://doi.org/10.1371/journal.pone.0096667
Carvalho AM, César CL, Fisberg RM, Marchioni DM (2013) Excessive meat consumption in Brazil: diet quality and environmental impacts. Public Health Nutr 16:1893–1899. https://doi.org/10.1017/S1368980012003916
Bomfim NS, Dias EP, Sbeghen MR, Sbeghen MR (2014) A atuação do nutricionista em pacientes com câncer gástrico. Unoesc & Ciência – ACBS. 5:129–134
Ferrari TK, Cesar CL, Alves MC, Barros MB, Goldbaum M, Fisberg RM (2017) Estilo de vida saudável em São Paulo. Brasil Cadernos de Saúde Pública. https://doi.org/10.1590/0102-311x00188015
Silva AE, G, de Moura L, Curado MP, Gomes Fda S, Otero U, Rezende LF, Daumas RP, Guimarães RM, Meira KC, Leite Ida C, Valente JG, Moreira RI, Koifman R, Malta DC, Mello MS, Guedes TW, Boffetta P, (2016) The fraction of cancer attributable to ways of life, infections, occupation, and environmental agents in Brazil in 2020. PLoS ONE. https://doi.org/10.1371/journal.pone.0148761
Baiao DDS, de Freitas CS, Gomes LP, da Silva D, Correa A, Pereira PR, Aguila EMD, Paschoalin VMF (2017) Polyphenols from root, tubercles and grains cropped in Brazil: Chemical and nutritional characterization and their effects on human health and diseases. Nutrients 9:1044. https://doi.org/10.3390/nu9091044
Campolina AG et al (2012) Multimorbidade e Expressão Gênica Perspectivas Nutrigenômicas e Nutrigenética para Abordagem das Doenças Crônicas. Kur´yt`yba. São Paulo 4:19–42
Resende ALS, Mattos IE, Koifman S (2006) Dieta e câncer gástrico: aspectos históricos associados ao padrão de consumo alimentar no Estado do Pará. Rev Nutr 19:511–519. https://doi.org/10.1590/S1415-52732006000400010
Search for family budgets: 2017–2018: avaliação nutricional da disponibilidade domiciliar de alimentos no Brasil / IBGE, Coordenação de Trabalho e Rendimento. - Local: Rio de JaneiroEditor: IBGE. 56
Selem SS, Carvalho AM, Verly-Junior E, Carlos JV, Teixeira JA, Marchioni DM, Fisberg RM (2014) Validity and reproducibility of a food frequency questionnaire for adults of São Paulo. Brazil Rev Bras Epidemiol 17:852–859. https://doi.org/10.1590/1809-4503201400040005
Kim SR, Kim K, Lee SA, Kwon SO, Lee JK, Keum N, Park SM (2019) Effect of red, processed, and white meat consumption on the risk of stomach cancer: an overall and dose response meta-analysis. Nutrients 11(4):826. https://doi.org/10.3390/nu11040826
Song P, Wu L, Guan W (2015) Dietary nitrates, nitrites, and nitrosamines intake and the risk of stomach cancer: a meta-analysis. Nutrients 7(12):9872–9895
Poorolajal J, Moradi L, Mohammadi Y, Cheraghi Z, Gohari-Ensaf F (2020) Risk factors for stomach cancer: a systematic review and meta-analysis. Epidemiol Health 42:e2020004. https://doi.org/10.4178/epih.e2020004]
Wang Z, Graham DY, Khan A, Balakrishnan M, Abrams HR, El-Serag HB, Thrift AP (2018) Incidence of stomach cancer in the USA during 1999 to 2013: a 50-state analysis. Int J Epidemiol 47(3):966–975. https://doi.org/10.1093/ije/dyy055
Smith AD, Emmett PM, Newby PK, Northstone K (2013) Dietary patterns obtained through principal components analysis: the effect of input variable quantification. Br J Nutr 109(10):1881–1891. https://doi.org/10.1017/S0007114512003868 (Epub 2012 Sep 6 PMID: 22950853)
Acknowledgments
We thank the interviewers from São Paulo (Iara Monique, Camila Gatti, Ana Carolina Cantelli, and Graziela Baladão) and from Belém (Tayana Vago, Ana Carla da Silva, Anna Byatriz Lopes, and Lucas Trindade) who helped with data collection; the study participants, whose generosity made this research possible; and Emmanuel Dias-Neto, the principal investigator of the Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP) project.
Funding
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brazil (CAPES) – Finance Code 001. This research received funding of Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP) Grant 2014/26897–0.
Author information
Authors and Affiliations
Contributions
M.P.C., F.J.F.C., P.P.A., M.S.A., and A.G.P. designed the research; M.A.F. and J.J.N.A. conducted the research; S.V.P. analyzed the data; D.R.M.S., J.J.N.A., S.V.P., M.A.F., and M.P.C. wrote the paper; M.P.C. and S.V.P. had primary responsibility for the final content. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare. All authors have seen and agree with the contents of the manuscript. We certify that the submission is original work and is not under review by any other publication.
Ethical approval
Data described in the manuscript, the codebook, and the analytical codes will be made available upon request and pending approval.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Peres, S.V., Silva, D.R.M., Coimbra, F.J.F. et al. Consumption of processed and ultra-processed foods by patients with stomach adenocarcinoma: a multicentric case–control study in the Amazon and southeast regions of Brazil. Cancer Causes Control 33, 889–898 (2022). https://doi.org/10.1007/s10552-022-01567-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-022-01567-w