Abstract
Cryptococcal species often cause lung infections and are the main cause of fungal meningitis. Claudin-4 appears to be a major structural component that maintains a tight alveolar barrier and prevents fluid and electrolyte leakage into the alveolar space. We aimed to determine whether S7-tetrahydrocurcumin (THC) could clearance of C. deneoformans and regulate claudin-4 expression during C. deneoformans infection. We investigated the effect of THC on C. deneoformans infection and its possible mechanism in vivo. Transmission electron microscopy was used to observe the ultrastructure of the lung tissue and the invasion of Cryptococcus. To clarify the effect of THC, we examined claudin-4, c-Jun, and Smad2 expression. We also measured claudin-4 expression in pulmonary specimens from clinical patients. THC reduced cryptococcal cell invasion in the lungs, improved alveolar exudation, and reduced inflammation. Pretreatment with THC suppressed c-Jun and Smad2 expression, resulting in significantly increased claudin-4 levels. In contrast, the expression of claudin-4 in clinical specimens from patients with cryptococcal infection was higher than that in normal specimens. THC enhanced the clearance of C. deneoformans during infection in vivo. We investigated the expression of claudin-4 and the possible mechanism of THC against C. deneoformans infection.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cryptococcus deneoformans is the leading cause of fungal meningitis in populations with impaired immunity (Kwon-Chung 2014). Cryptococcus often causes lung and brain infections in individuals who are immunocompromised (Taylor-Smith 2017). The global burden of this disease is estimated to be close to 1 million cases, with 700,000 deaths annually (Park 2007).
The rising prevalence of various diseases is believed to be closely linked to, or even dependent upon, modifications occurring within the tight junctions (Cereijido 2007). Claudins, which are major transmembrane proteins that localize at tight junctions, were first discovered by Furuse et al. in the chicken liver in 1998 (Furuse 9). Previous studies suggest that claudins 1, 3, 4, 5, 7, 10, and 18 (splice variant 1) are expressed in bronchi and bronchioles, and some have also been detected in the distal lung (Coyne 2003). Claudins 3, 4, and 7 are predominantly expressed in alveolar type II cells. Claudin-4 appears to be a major structural component that maintains a tight alveolar barrier and prevents the leakage of fluid and electrolytes into the alveolar space. Wray C and colleagues demonstrated that claudin-4 suppressed air space fluid clearance and exacerbated ventilator-induced pulmonary oedema in vitro (Wray 2009). Consistent with this finding, the expression of claudin-4 is associated with alveolar fluid clearance (Rokkam 2011). Amasheh et al. showed that the downregulation of claudin-1 and upregulation of claudin-2 was mediated by the TNF-/NF-κB pathway in the intestinal HT-29/B6 cell line. These effects could be suppressed by the herbal compound berberine (Amasheh 2010).
Smad proteins, distinguished as members of the TGF-β family due to their structural and functional characteristics in signaling, have been implicated in hepatic metastasis in colorectal cancer (Halder 2008). C-Jun, a key component of the protein activator protein-1 (AP-1) complex, plays a significant role in numerous cellular processes, including proliferation, apoptosis, survival, tumorigenesis, and histomorphogenesis. Despite years of rigorous research, the intricate functional properties of c-Jun, positioned at the core of the molecular network, remain to be fully unravelled (Meng 2011). Christina Van Itallie and colleagues observed that claudin-4 overexpression led to a reduction in paracellular electrical conductance and impacted paracellular ion selectivity (Itallie 2001). In another study, Patrick Michl and his team demonstrated that claudin-4 could suppress invasiveness and the metastatic phenotype of pancreatic cancer cells through the TGF-β and Ras signaling pathways (Michl 2003). Furthermore, Michl's team revealed claudin-4 overexpression in pancreatic cancer and illustrated that targeting claudin-4-expressing tumors with CPE resulted in extensive tumor cell necrosis and a substantial decrease in tumor growth (Michl 2001). Notably, claudin-4 is also found at elevated levels in prostate tissue (Long 2001). The overexpression of both claudin-3 and claudin-4 has been linked to malignancy in ovarian cystadenoma (Rangel 2003).
Curcumin improves intestinal barrier function through the modulation of intracellular signalling and the organization of tight junctions (Wang 2017). Erin E. Olson et al showed that S7-tetrahydrocurcumin (THC), which is derived from extracts rich in curcuminoids and catechins could reduce immune cell inflammation and preserve tight junction integrity in an in vitro coculture model of intestinal inflammation (Olson 2020). Interestingly, THC could alter these functional and molecular changes (Mondal 2019).
Based on these findings, the present study was conducted to examine the effect of THC, a major secondary metabolite of curcumin, and the possible mechanism against C. deneoformans infection.
Materials and methods
Materials
THC was obtained from China Haoxin Biotechnology Co., Ltd. and subsequently dissolved in dimethyl sulfoxide (DMSO) before being stored as a frozen 200 µM stock solution. The following primary antibodies were used: claudin-4 (Abcam, ab15104), c-Jun (Abcam, ab40766), Smad2 (Abcam, ab63576), and β-actin (1:1000 Cell Signaling Technology, CST). The secondary antibody was goat anti-mouse/rabbit IgG (1:5000 Cell Signaling Technology, CST).
C. deneoformans
The C. deneoformans strain 52D (ATCC 24067) was obtained from the American Type Culture Collection (Manassas, VA). For infection, yeast were grown to stationary phase after an incubation period of 48 to 72 h at 37 °C in Sabouraud dextrose broth (1% neopeptone and 2% dextrose; Difco, Detroit, MI) on a shaker. Cells were washed twice with saline, counted on a haemocytometer, and diluted to 3.3 * 105 CFU/ml in nonpyrogenic saline.
Mouse controls
Male KM mice (5–6 weeks of age) were obtained from Shanghai SLAC Laboratory Animal Co., Ltd. The mice were randomly assigned to five groups: (1) the normal group (n = 6); (2) the control group: C. deneoformans plus DMSO (n = 8); (3) the low-dose THC group: C. deneoformans plus 50 mg/kg/d THC (n = 8); (4) the middle-dose THC group: C. deneoformans plus 100 mg/kg/d THC (n = 8); and (5) the high-dose THC group: C. deneoformans plus 200 mg/kg/d THC (n = 8). THC was administered to mice by gavage for one week. Mice were infected with C. deneoformans on day 8. All experiments were approved by the Ethics Committee of Changxing People’s Hospital.
Intratracheal inoculation of C. deneoformans
Mice were anesthetized using intraperitoneal injections of pentobarbital sodium. Fifty microlitres of C. deneoformans (105 CFU) was dripped into the trachea through a syringe. Body weight was measured every 4 days for 5 weeks, and then the mice were sacrificed by intraperitoneal injections of pentobarbital sodium.
Histological analysis
Three specimens were randomly selected from each group. Lung tissues were fixed in 4% formaldehyde for 3–5 days. After paraffin embedding, 4 µm sections were cut and stained with haematoxylin and eosin. Sections were analysed using light microscopy.
Immunohistochemical staining
The lung tissues were fixed in 4% formaldehyde, embedded in paraffin, and cut into 4-µm-thick sections. Before being boiled in citrate buffer, the slides were immersed in 3% hydrogen peroxide for 15 min to block endogenous peroxidase activity. The slides were incubated with claudin-4, c-Jun, and Smad2 antibodies and then incubated with HRP-conjugated antibodies. The slides were visualized with a DAB Horseradish Peroxidase Colour Development Kit (Beyotime) and counterstained with haematoxylin. The images were analysed by Image-Pro Plus 6.0 software.
Visualization of the interaction of C. deneoformans with the lung by TEM
Lung tissues were fixed with 2.5% glutaraldehyde phosphate buffer. Then, the samples were postfixed in osmium acid for 1 h, stained with 2% uranyl acetate in an aqueous solution for 30 min, dehydrated through a graded alcohol series, and embedded in Spurr resin. The tissues were cut into 120 nm sections, poststained in uranyl acetate and lead citrate, and viewed with a Philips TECNA-10 transmission electron microscope.
Quantitative real-time PCR
Total RNA was extracted using a high-purity total RNA rapid extraction kit, and cDNA was synthesized using a PrimeScript™ RT reagent kit and HiScript-IIQ RT SuperMix (Vazyme, Piscataway, USA). The reaction was mixed in an ice bath and then reacted at 50 °C for 15 min and then at 85 °C for 2 min. The reaction was then stopped and stored at − 20 °C until use. Each sample was run in a final volume of 20.0 µl containing 10 µl of 2X ChamQ SYBR Colour qPCR Master Mix, 0.6 µl of forward primer (10 µM), 0.6 µl of reverse primer (10 µM), and 8.8 µl of template cDNA(claudin-4 forward, CCGCACTGTCTTGCTAATG and reverse, CAGAGGGGCCAACTCAA; c-Jun forward, GAACTCGGACCTTCTCACG and reverse, TGGGGCACAAGAACTGG; Smad2 forward, CCTTCCATGCGTCACAG and reverse, CGCACTCCCCTTCCTAT). β-actin served as the reference gene, and the 2-ΔΔCq technique was employed to ascertain the relative expression levels of each gene. Three samples were randomly chosen from each group to ensure a representative analysis.
Western blot analysis
Three samples were randomly selected from each group for analysis. Lung tissues were lysed using RIPA buffer, and protein concentrations were determined employing a BCA kit from Beyotime. Subsequently, 30 μg of protein was isolated for further examination. Equal quantities of proteins were separated using either 4% or 12% SDS-polyacrylamide gels and then transferred onto nitrocellulose membranes provided by Millipore. The membranes were blocked using 5% nonfat milk in TBST (Tris-buffered saline, pH 7.4, with 0.05% Tween 20) and incubated with Claudin-4 antibody (1:100), c-Jun antibody (1:100), and Smad2 antibody (1:100)—all sourced from Abcam—overnight at 4 °C. Following this, the membranes were incubated with alkaline phosphatase-conjugated goat anti-mouse IgG or goat anti-rabbit IgG (1:5000) for 1 hour at room temperature. Finally, the signals were detected using an enhanced chemiluminescence detection kit to reveal the desired outcomes.
Statistical analysis
The data were meticulously analyzed using GraphPad Prism version 9.0 (Graph Pad Software, San Diego, CA, USA) and are presented as the mean ± standard deviation (SD). To assess differences between groups, ANOVA was employed, followed by a Bonferroni multiple comparisons posttest. A P value of < 0.05 was deemed indicative of statistical significance. Each experiment was performed in triplicate to ensure consistency and reliability in the findings.
Results
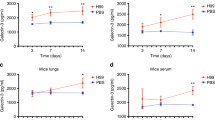
In order to investigate the impact of THC on Cryptococcus infection in mice, several treatment groups were established. The lung tissues from mice in each group were subsequently analyzed for further experimentation. Following cryptococcal infection, the other groups did not exhibit weight loss in comparison to the uninfected control group of mice (Figure 1a). Histological analysis showed that compared with those in the normal group, multiple granulomatous nodules appeared in the control group, and Cryptococcus was surrounded by large numbers of macrophages, lymphocytes, and a small number of neutrophils. Additionally, mild bronchial pneumonia, intra-alveolar haemorrhage, alveolar fusion, and interstitial widening were observed (Figure 1b). Cryptococcus was observed in one specimen in the THC low-dose group. No Cryptococcus was found in the other two specimens. We also observed mild bronchopneumonia, a small amount of haemorrhage in the alveoli, mild fusion of the alveoli, and widening of the interstitium. Additionally, these groups showed less severe inflammation than the control group. We observed a small amount of Cryptococcus in the middle-dose THC group. However, there was no obvious inflammation in the lungs, and the alveoli were normal. The results from the high-dose group were in between. In this experiment, THC reduced the invasion of cryptococcal cells in the lungs, improved alveolar exudation, and reduced inflammation.
a Measurement of mouse weight every four days. b Histopathology of lung for Male KM mice infected with C. deneoformans. Three specimens were randomly selected from each group. Black arrowheads indicates C.neoformans cells stained hematoxylin and eosin. Many yeast cells appear as degenerated cells within macrophages
We performed immunohistochemistry and found that THC promoted claudin-4 expression and suppressed c-Jun and Smad2 compared to those in the control group (Figure 2). Compared with the normal group, the expression of Claudin-4 in the control group was significantly reduced. Compared with claudin-4 expression in the control group, the expression of Claudin-4 in the presence of THC increased to varying degrees in each other group (Figure 3a). As shown in Figure 3b, the expression of Smad2 in the control group was significantly increased. Compared with the control group, the expression of Smad2 in each group in the presence of THC was reduced. The same effect on the expression of c-Jun was also observed (Figure 3c).
Type I and type II alveolar epithelial cells had a complete structure, and the organelles were not damaged, but the lamellar bodies of type II alveolar epithelial cells were reduced or even vacuolated, and some capillaries were congested and blocked in the normal group (Figure 4a). In the control group, we observed a large number of lamellar bodies and capillary congestion and blockage. In the low-dose THC group, the number of lamellar bodies was in between. Capillary congestion was improved, but some red blood cells were exuded. Compared with the corresponding data in the THC low-dose group, the number of lamellar bodies was greater in the middle-dose THC group, and capillary congestion was improved, but some red blood cells were still exuded. The ultrastructure of the high-dose THC group was similar to that of the control group (Figure 4b).
Electron microscopy of lung tissue from mice inoculated with C. deneoformans. a The ultrastructure of lung tissue and the invasion of Cryptococcus after treatment with THC.One sample were randomly selected from each group. The overview in a shows a well-preserved type II cell from a rat lung. Lamellar bodies (LB), nucleus (Nu) and mitochondria (Mt) are well preserved.Bars = 2 μm. b Analysis of LBs number within the alveolar epithelial type II cells( ATII).Values are expressed as mean ± SEM. (*p < 0.05, **p < 0.01, ***p < 0.001,****p < 0.0001), n = 5/group
Quantitative real-time PCR indicated that THC decreased the expression of c-Jun and Smad2 (Figure 5b and Figure 5c). However, THC upregulated the expression of claudin-4 compared with that in the control group (Figure 5a). Additionally, the middle-dose THC group showed the greatest effect.
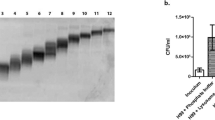
Western blotting indicated that claudin-4 was upregulated in the presence of THC in the lung tissues of mice (Figure 6a). In contrast, the expression of c-Jun and Smad2 was suppressed by THC (Figure 6b, c). We also found that the effect was more notable in the group treated with 100 mg/kg THC (Figure 6d).
We also measured the expression of claudin-4 in pulmonary specimens from clinical patients (Table1). The expression of claudin-4 in lung tissues from clinical patients who were infected with C. deneoformans was significantly increased compared with that in normal lung tissues. (Figure 7). This finding was the opposite of what was observed in mice.
Discussion
Claudin-3, claudin-4, and claudin-18 are the predominant claudins expressed by the alveolar epithelium (Koval 2013). Many studies suggest that several human lung disorders are linked to claudin dysregulation. Charlie Wray et al demonstrated that increased claudin-4 expression early in acute lung injury represents a mechanism to limit pulmonary oedema that is dependent on PKC activation and the JNK MAPK pathway. Low expression of claudin-4 results in leakier tight junctions, decreased alveolar fluid clearance, and increased pulmonary oedema with mechanical ventilation (Wray 2009). However, the expression of alveolar epithelial claudin-4 is downregulated in sepsis, which increases the severity of lung injury (Cohen 2010). LSH Chuang et al observed that TGF-β signalling resulted in the dissolution of tight junctions (Chuang 2010). Chang et al also found that the cooperation of Runx3 and the TGF-β effector Smad directly upregulates claudin-1 transcription (Chang 2010).
Cryptococcus heteromorphous, an opportunistic fungal pathogen, infects the lungs via airborne transmission and frequently results in fatal meningoencephalitis. It has been reported that Cldn-4 functions as a paracellular sodium barrier and plays a somewhat ambiguous role in safeguarding the lung from acute injury, even though its contribution to normal lung physiology is minimal (Kage 2014). Ko Sato and colleagues discovered that there was no significant difference in pulmonary fungal load between Cldn-4+/+ and Cldn-4−/− mice at day 14 post-infection. Fungal clearance appeared normal in Cldn-4-deficient mice (Sato 2021).
In this study, we investigated the effect of THC and its possible mechanism against C. deneoformans infection in vivo. THC reduced the invasion of cryptococcal cells in the lungs, improved alveolar exudation, and reduced inflammation. Pretreatment with THC suppressed the expression of c-Jun and Smad2, resulting in a significant increase in claudin-4. In contrast, we found that the expression of claudin-4 was higher in clinical specimens from patients with cryptococcal infection than in normal specimens. This difference may be because the inflammatory response in the human body is more complicated than that in mice.
The study of Girish Rachakonda et al provided convincing evidence that TGF-β induced Claudin-4 expression through c-Jun signalling in non-small-cell lung cancer. Treatment with curcumin, a c-Jun inhibitor, abrogated TGF-β-induced claudin-4 expression, suggesting the involvement of the c-Jun pathway (Rachakonda 2016). Similarly, we have provided evidence that THC altered the expression of claudin-4 possibly via the c-Jun signalling pathway. In addition, we observed that THC pretreatment regulated the expression of Smad2 in response to C. deneoformans infection. Consistent with these results, Chuang LSH et al observed that TGF-β signalling resulted in the dissolution of tight junctions (Chuang 2010). Chang et al also found that cooperation between Runx3 and the TGF-β effector Smad directly upregulated claudin-1 transcription (Chang 2010).
THC possesses antioxidant, antifungal, and antimycotoxic properties; however, its typically low water solubility considerably restricts its potential application in water-based formulations (Coma 2011). Anne Loron et al.’s study revealed that, in preliminary tests, 10 µM THC did not inhibit the growth of F. graminearum. THC-loaded particles have demonstrated promising antifungal properties. Since the product does not interfere with fungal growth at this concentration, THC’s impact on toxin production can be assessed accordingly (Coma 2021). Shan Chen discovered that neither free nor encapsulated THC affected non-cancerous mouse embryonic cells, suggesting that THC is biocompatible with healthy non-melanoma cells and exhibits no biotoxicity (Shan 2021). THC's influence on host response has not been thoroughly validated. Perhaps from a more critical standpoint, the untreated THC treatment group’s effect should be examined. Evaluating THC’s impact on Cryptococcus activity in vitro is also essential. If THC has antifungal activity, it could potentially result from a weakened host response by reducing the fungal population. However, this hypothesis was not fully considered and verified in our experiments. In BALB/c mice infected with Cryptococcal strain 52D, Aditya V. Jain observed that strain 52D proliferated rapidly (1000-fold increase compared to the original inoculum) at week 1, but its subsequent growth was inhibited (weeks 2 and 3), and significant clearance was observed at week 4 compared to the peak level at week (Jain 2009). It is also necessary to expand the assay's time points in the experiment to thoroughly comprehend Cryptococcus clearance and the changes in the indicators over time. In clinical practice, patients are often infected with cryptococci first and then follow up with treatment. Therefore, a mouse model of cryptococcal infection can be considered in the laboratory before subsequent THC treatment.
This study is the first to demonstrate that THC can be used to address Cryptococcus pneumoniae. These findings suggest specific roles for claudin-4, c-Jun, and Smad2 during C. deneoformans infection, but the exact mechanism remains to be elucidated. Therefore, this report demonstrates for the first time that THC may be a potent therapeutic agent for cryptococcal pneumonia, but this finding must be tested further.
References
Amasheh M, Fromm A, Krug SM et al (2010) TNFα-induced and berberine-antagonized tight junction barrier impairment via tyrosine kinase, Akt and NFκB signaling. J Cell Sci 123(23):4145–4155
Cereijido M, Contreras RG, Flores-Benitez D et al (2007) New diseases derived or associated with the tight junction. Arch Med Res. https://doi.org/10.1016/j.arcmed.2007.02.003
Chang TL, Ito K, Ko TK et al (2010) Claudin-1 has tumor suppressive activity and is a direct target of RUNX3 in gastric epithelial cells. Gastroenterology 138(1):255-265. e3
Chuang LSH, Ito Y (2010) RUNX3 is multifunctional in carcinogenesis of multiple solid tumors. Oncogene 29(18):2605–2615
Cohen TS, Gray Lawrence G, Margulies SS (2010) Cultured alveolar epithelial cells from septic rats mimic in vivo septic lung. PLoS ONE 5(6):e11322
Coma V (2021) Polysaccharide matrices for the encapsulation of tetrahydrocurcumin—potential application as biopesticide against Fusarium graminearum. Molecules. https://doi.org/10.3390/molecules26133873
Coma V, Portes E, Gardrat C et al (2011) Invitro inhibitory effect of tetrahydrocurcuminoids on growth and fumonisin Bbiosynthesis. Food Addit Contam Part A Chem Anal Control Exposure Risk Assess 28(2):218–225
Coyne CB, Gambling TM, Boucher RC et al (2003) Role of claudin interactions in airway tight junctional permeability. Am J Physiol Lung Cell Mol Physiol 285(5):L1166–L1178
Furuse M, Fujita K, Hiiragi T et al (1998) Claudin-1 and-2: novel integral membrane proteins localizing at tight junctions with no sequence similarity to occludin. J Cell Biol 141(7):1539–1550
Halder SK, Rachakonda G, Deane NG et al (2008) Smad7 induces hepatic metastasis in colorectal cancer. Br J Cancer 99(6):957–965
Itallie CV, Rahner C, Anderson JM (2001) Regulated expression of claudin-4 decreases paracellular conductance through a selective decrease in sodium permeability. J Clin Investig 107(10):1319
Jain AV, Zhang Y, Fields WB et al (2009) Th2 but not Th1 immune bias results in altered lung functions in a murine model of pulmonary Cryptococcus neoformans infection. Infect Immun 77(12):5389–5399
Kage H, Flodby P, Gao D et al (2014) Claudin 4 knockout mice: normal physiological phenotype with increased susceptibility to lung injury. Am J Physiol Lung Cell Mol Physiol 307(7):524–536
Koval M (2013) Claudin heterogeneity and control of lung tight junctions. Annu Rev Physiol 75:551–567
Kwon-Chung KJ, Fraser JA, Doering TL et al (2014) Cryptococcus neoformans and Cryptococcus gattii, the etiologic agents of cryptococcosis. Cold Spring Harb Perspect Med 4(7):a019760
Long H, Crean CD, Lee WH et al (2001) Expression of Clostridium perfringens enterotoxin receptors claudin-3 and claudin-4 in prostate cancer epithelium. Can Res 61(21):7878–7881
Meng Q, Ying X (2011) c-Jun, at the crossroad of the signaling network. Protein Cell 2(11):10
Michl P, Buchholz M, Rolke M et al (2001) Claudin-4: a new target for pancreatic cancer treatment using Clostridium perfringens enterotoxin. Gastroenterology 121(3):678–684
Michl P, Barth C, Buchholz M et al (2003) Claudin-4 expression decreases invasiveness and metastatic potential of pancreatic cancer. Can Res 63(19):6265
Mondal NK, Behera J, Kelly KE et al (2019) Tetrahydrocurcumin epigenetically mitigates mitochondrial dysfunction in brain vasculature during ischemic stroke. Neurochem Int 122:120–138
Olson EE, Zastrow AL, Sharda DR (2020) Protective effects of the novel phytonutrient Spectra7 against intestinal tight junction disruption: composition matters. FASEB J 34(S1):1–1
Park BJ, Wannemuehler KA, Marston BJ et al (2009) Estimation of the current global burden of cryptococcal meningitis among persons living with HIV/AIDS. AIDS 23(4):525–530
Rachakonda G, Vu T, Jin L et al (2016) Role of TGF-β-induced Claudin-4 expression through c-Jun signaling in non-small cell lung cancer. Cell Signal. https://doi.org/10.1016/j.cellsig.2016.07.006
Rangel L, Agarwal R, D’Souza T et al (2003) Tight Junction proteins claudin-3 and claudin-4 are frequently overexpressed in ovarian cancer but not in ovarian cystadenomas. Clin Cancer Res 9(7):2567–2575
Rokkam D, LaFemina MJ, Lee JW et al (2011) Claudin-4 levels are associated with intact alveolar fluid clearance in human lungs. Am J Pathol 179(3):1081–1087
Sato Ko et al (2021) Deficiency of lung-specific claudin-18 leads to aggravated infection with Cryptococcus deneoformans through dysregulation of the microenvironment in lungs. Sci Rep 11(1):1–13
Shan CA, Qiao WA, Mm A et al (2021) Designing biocompatible protein nanoparticles for improving the cellular uptake and antioxidation activity of tetrahydrocurcumin. J Drug Deliv Sci Technol. https://doi.org/10.1016/j.jddst.2021.102404
Taylor-Smith LM (2017) Cryptococcus–epithelial interactions. J Fungi 3(4):53
Wang J, Ghosh SS, Ghosh S (2017) Curcumin improves intestinal barrier function: modulation of intracellular signaling, and organization of tight junctions. Am J Physiol Cell Physiol 312(4):C438–C445
Wray C, Mao Y, Pan J et al (2009) Claudin-4 augments alveolar epithelial barrier function and is induced in acute lung injury. Am J Physiol Lung Cell Mol Physiol 297(2):L219–L227
Acknowledgements
Our study was supported by the Medical Health Science and Technology Project of Zhejiang Provincial Health Commission (2018270021).
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Contributions
TH was responsible for organization and coordination of the study. GS was the chief investigator and was responsible for data analysis. ZJ, WH, XX, DL, WY, GL, and XZ developed the study design. All authors contributed to the writing of the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
He, T., Jin, Z., Hu, W. et al. Tetrahydrocurcumin (THC) enhanced the clearance of Cryptococcus deneoformans during infection in vivo. Antonie van Leeuwenhoek 116, 565–576 (2023). https://doi.org/10.1007/s10482-023-01830-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10482-023-01830-3