Abstract
Aims
The mechanisms of monocyte recruitment to arteriogenic collaterals are largely unknown. We investigated the role of chemokine (C-X-C-motif) ligand 1 (CXCL1) and its cognate receptor, chemokine (C-X-C-motif) receptor 2 (CXCR2) in arteriogenesis.
Methods and results
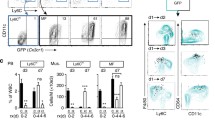
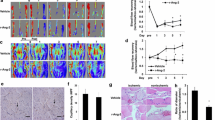
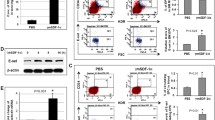
After femoral artery ligation in Sprague–Dawley rats, either native collaterals were harvested or placebo, CXCL1 or CXCR2 blocker was administered via an osmopump. Perfusion recovery was measured with Laser Doppler, leukocyte populations were analyzed by fluorescence-activated cell sorting, and hind limb sections were stained for macrophage marker cluster of differentiation 68 (CD68). In vitro, fluorescent CXCL1 or human acute monocytic leukemia cell line (THP-1) monocytic cells were flown over shear-stressed endothelium. CXCL1 mRNA expression in collaterals was dramatically upregulated already 1 h after ligation (ratio ligated/sham 5.73). CD68 mRNA was upregulated from 12 h until 3 days after ligation (peak ratio ligated/sham 2.65). CXCL1 treatment augmented perfusion recovery at 3 and 7 days (p < 0.05) after ligation, and a significant increase in the number of peri-collateral macrophages was evident concomitantly (p < 0.05). Conversely, CXCR2 antagonist treatment caused a decrease in perfusion recovery both at 7 and 10 days postligation (p = 0.01) and also significantly reduced the number of peri-collateral macrophages (p < 0.05). In vitro, CXCL1 tethered to and was taken up by endothelial cells under shear stress conditions and enhanced THP-1 adherence compared to control (p < 0.05). In contrast, CXCR2 antagonist compromised THP-1 adherence to endothelial cells (p < 0.05).
Conclusion
CXCL1 presented on the luminal endothelial surface leads to an increase in the number of peri-collateral macrophages, thus improving the arteriogenic response after arterial ligation.






Similar content being viewed by others
Abbreviations
- CXCL1:
-
(C-X-C-motif) ligand 1
- CXCR2:
-
(C-X-C-motif) receptor 2
- THP-1:
-
Human acute monocytic leukemia cell line
- CD68:
-
Cluster of differentiation 68
References
Schaper W, Schaper J (2004) Arteriogenesis. Kluwer Academic Publishers Group, Boston
Heil M, Eitenmuller I, Schmitz-Rixen T, Schaper W (2006) Arteriogenesis versus angiogenesis: similarities and differences. J Cell Mol Med 10:45–55
Vogel R, Traupe T, Steiger VS, Seiler C (2010) Physical coronary arteriogenesis: a human “model” of collateral growth promotion. Trends Cardiovasc Med 20:129–133
Jain RK (2003) Molecular regulation of vessel maturation. Nat Med 9:685–693
Schirmer SH, van Nooijen FC, Piek JJ, van Royen N (2009) Stimulation of collateral artery growth: travelling further down the road to clinical application. Heart 95:191–197
Hoefer IE, Grundmann S, van Royen N, Voskuil M, Schirmer SH, Ulusans S, Bode C, Buschmann IR, Piek JJ (2005) Leukocyte subpopulations and arteriogenesis: specific role of monocytes, lymphocytes and granulocytes. Atherosclerosis 181:285–293
Takeda Y, Costa S, Delamarre E, Roncal C, de Oliveira RL, Squadrito ML, Finisguerra V, Deschoemaeker S, Bruyere F, Wenes M, Hamm A, Serneels J, Magat J, Bhattacharyya T, Anisimov A, Jordan BF, Alitalo K, Maxwell P, Gallez B, Zhuang ZW, Saito Y, Simons M, De Palma M, Mazzone M (2011) Macrophage skewing by Phd2 haplodeficiency prevents ischaemia by inducing arteriogenesis. Nature 479:122–126
Addison CL, Daniel TO, Burdick MD, Liu H, Ehlert JE, Xue YY, Buechi L, Walz A, Richmond A, Strieter RM (2000) The CXC chemokine receptor 2, CXCR2, is the putative receptor for ELR+ CXC chemokine-induced angiogenic activity. J Immunol 165:5269–5277
Hagiwara H, Mitsumata M, Yamane T, Jin X, Yoshida Y (1998) Laminar shear stress-induced GRO mRNA and protein expression in endothelial cells. Circulation 98:2584–2590
Bozic CR, Gerard NP, von Uexkull-Guldenband C, Kolakowski LF Jr, Conklyn MJ, Breslow R, Showell HJ, Gerard C (1994) The murine interleukin 8 type B receptor homologue and its ligands. Expression and biological characterization. J Biol Chem 269:29355–29358
White JR, Lee JM, Young PR, Hertzberg RP, Jurewicz AJ, Chaikin MA, Widdowson K, Foley JJ, Martin LD, Griswold DE, Sarau HM (1998) Identification of a potent, selective non-peptide CXCR2 antagonist that inhibits interleukin-8-induced neutrophil migration. J Biol Chem 273:10095–10098
Ito WD, Arras M, Winkler B, Scholz D, Schaper J, Schaper W (1997) Monocyte chemotactic protein-1 increases collateral and peripheral conductance after femoral artery occlusion. Circ Res 80:829–837
Scholz D, Ziegelhoeffer T, Helisch A, Wagner S, Friedrich C, Podzuweit T, Schaper W (2002) Contribution of arteriogenesis and angiogenesis to postocclusive hindlimb perfusion in mice. J Mol Cell Cardiol 34:775–787
Gordon S, Taylor PR (2005) Monocyte and macrophage heterogeneity. Nat Rev Immunol 5:953–964
Wang D, Wang H, Brown J, Daikoku T, Ning W, Shi Q, Richmond A, Strieter R, Dey SK, DuBois RN (2006) CXCL1 induced by prostaglandin E2 promotes angiogenesis in colorectal cancer. J Exp Med 203:941–951
Acharyya S, Oskarsson T, Vanharanta S, Malladi S, Kim J, Morris PG, Manova-Todorova K, Leversha M, Hogg N, Seshan VE, Norton L, Brogi E, Massague J (2012) A CXCL1 paracrine network links cancer chemoresistance and metastasis. Cell 150:165–178
Payne AS, Cornelius LA (2002) The role of chemokines in melanoma tumor growth and metastasis. J Invest Dermatol 118:915–922
Kuo PL, Shen KH, Hung SH, Hsu YL (2012) CXCL1/GROalpha increases cell migration and invasion of prostate cancer by decreasing fibulin-1 expression through NF-kappaB/HDAC1 epigenetic regulation. Carcinogenesis 33:2477–2487
Breland UM, Halvorsen B, Hol J, Oie E, Paulsson-Berne G, Yndestad A, Smith C, Otterdal K, Hedin U, Waehre T, Sandberg WJ, Froland SS, Haraldsen G, Gullestad L, Damas JK, Hansson GK, Aukrust P (2008) A potential role of the CXC chemokine GROalpha in atherosclerosis and plaque destabilization: downregulatory effects of statins. Arterioscler Thromb Vasc Biol 28:1005–1011
Huo Y, Weber C, Forlow SB, Sperandio M, Thatte J, Mack M, Jung S, Littman DR, Ley K (2001) The chemokine KC, but not monocyte chemoattractant protein-1, triggers monocyte arrest on early atherosclerotic endothelium. J Clin Invest 108:1307–1314
Zhou Z, Subramanian P, Sevilmis G, Globke B, Soehnlein O, Karshovska E, Megens R, Heyll K, Chun J, Saulnier-Blache JS, Reinholz M, van Zandvoort M, Weber C, Schober A (2011) Lipoprotein-derived lysophosphatidic acid promotes atherosclerosis by releasing CXCL1 from the endothelium. Cell Metab 13:592–600
Manoharan P, Basford JE, Pilcher-Roberts R, Neumann J, Hui DY, Lingrel JB (2014) Reduced levels of microRNAs miR-124a and miR-150 are associated with increased proinflammatory mediator expression in Krüppel-like factor 2 (KLF2)-deficient macrophages. J Biol Chem 289:31638–31646
Smith DF, Galkina E, Ley K, Huo Y (2005) GRO family chemokines are specialized for monocyte arrest from flow. Am J Physiol Heart Circ Physiol 289:H1976–H1984
Kuo YT, Jan RL, Kuo CH, Kuo PL, Wang WL, Huang MY, Chen HN, Hung CH (2012) Effects of vitamin D3 on the expression of GROalpha in THP-1 cells and human primary monocytes. J Food Sci 77:H47–H52
Arisaka T, Mitsumata M, Kawasumi M, Tohjima T, Hirose S, Yoshida Y (1995) Effects of shear stress on glycosaminoglycan synthesis in vascular endothelial cells. Ann N Y Acad Sci 748:543–554
Gouverneur M, Spaan JA, Pannekoek H, Fontijn RD, Vink H (2006) Fluid shear stress stimulates incorporation of hyaluronan into endothelial cell glycocalyx. Am J Physiol Heart Circ Physiol 290:H458–H462
Grundmann S, Schirmer SH, Hekking LH, Post JA, Ionita MG, de Groot D, van Royen N, van den Berg B, Vink H, Moser M, Bode C, de Kleijn D, Pasterkamp G, Piek JJ, Hoefer IE (2009) Endothelial glycocalyx dimensions are reduced in growing collateral arteries and modulate leucocyte adhesion in arteriogenesis. J Cell Mol Med 13:3463–3474
Mantovani A, Bonecchi R, Locati M (2006) Tuning inflammation and immunity by chemokine sequestration: decoys and more. Nat Rev Immunol 6:907–918
Poluri KM, Joseph PR, Sawant KV, Rajarathnam K (2013) Molecular basis of glycosaminoglycan heparin binding to chemokine CXCL1 dimer. J Biol Chem 288:25143–25153
Meen AJ, Oynebraten I, Reine TM, Duelli A, Svennevig K, Pejler G, Jenssen T, Kolset SO (2010) Serglycin is a major proteoglycan in polarized human endothelial cells and is implicated in the secretion of the chemokine GROalpha/CXCL1. J Biol Chem 286:2636–2647
Whittall C, Kehoe O, King S, Rot A, Patterson A, Middleton J (2013) A chemokine self-presentation mechanism involving formation of endothelial surface microstructures. J Immunol 190:1725–1736
Schaper J, Konig R, Franz D, Schaper W (1976) The endothelial surface of growing coronary collateral arteries. Intimal margination and diapedesis of monocytes. A combined SEM and TEM study. Virchows Arch A Pathol Anat Histol 370:193–205
Serbina NV, Pamer EG (2006) Monocyte emigration from bone marrow during bacterial infection requires signals mediated by chemokine receptor CCR2. Nat Immunol 7:311–317
Jetten N, Donners MM, Wagenaar A, Cleutjens JP, van Rooijen N, de Winther MP, Post MJ (2013) Local delivery of polarized macrophages improves reperfusion recovery in a mouse hind limb ischemia model. PLoS ONE 8:e68811
Braber S, Overbeek SA, Koelink PJ, Henricks PA, Zaman GJ, Garssen J, Kraneveld AD, Folkerts G (2011) CXCR2 antagonists block the N-Ac-PGP-induced neutrophil influx in the airways of mice, but not the production of the chemokine CXCL1. Eur J Pharmacol 668:443–449
Shireman PK (2007) The chemokine system in arteriogenesis and hind limb ischemia. J Vasc Surg 45(Suppl A):A48–A56
Martin D, Galisteo R, Gutkind JS (2009) CXCL8/IL8 stimulates vascular endothelial growth factor (VEGF) expression and the autocrine activation of VEGFR2 in endothelial cells by activating NFkappaB through the CBM (Carma3/Bcl10/Malt1) complex. J Biol Chem 284:6038–6042
Acknowledgments
This work was supported by CTMM, the Center for Translational Molecular Medicine (www.ctmm.nl) project EMINENCE [Grant No. 01C-204].
Conflict of interest
The authors declare that they have no conflict of interest.
Compliance with Ethical Standards
Experiments were conducted according to the Guide for the Care and Use of Laboratory Animals published by the USA National Institutes of Health and were approved by the institutional Ethics Committee on Experimental Animal Welfare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vries, M.H.M., Wagenaar, A., Verbruggen, S.E.L. et al. CXCL1 promotes arteriogenesis through enhanced monocyte recruitment into the peri-collateral space. Angiogenesis 18, 163–171 (2015). https://doi.org/10.1007/s10456-014-9454-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-014-9454-1