Abstract
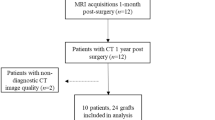
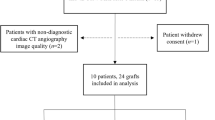
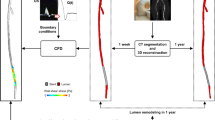
We predicted human lower extremity vein bypass graft remodeling by hemodynamics. Computed tomography and duplex ultrasound scans of 55 patients were performed at 1 week and 1, 6, and 12 months post-implantation to obtain wall shear stress (WSS) and oscillatory shear index (OSI) at 1-mm intervals via computational fluid dynamics simulations. Graft remodeling was quantified by computed tomography-measured lumen diameter changes in the early (1 week-1 month), intermediate (1–6 months), and late (6–12 months) periods. Linear mixed-effect models were constructed to examine the overall relationship between remodeling and initial hemodynamics using the average data of all cross sections within the same graft. A significant association of graft remodeling with WSS (p < 0.001) and time (p = 0.001) was found; however, the effect size decreased with time (every 2.7 dyne/cm2 increase of WSS was associated with a 0.39, 0.35, 0.002 mm diameter increase in the three periods, respectively). The association of remodeling with OSI was significant only in the intermediate period (every 0.1 increase of OSI was associated with a 0.25 mm lumen diameter decrease, p = 0.004). Therefore, the association of graft lumen remodeling with local hemodynamics has a distinct temporal pattern; WSS and OSI are predictive of remodeling only in certain postoperative periods.







Similar content being viewed by others
References
Colombo, M., Y. He, A. Corti, D. Gallo, F. Ninno, S. Casarin, J. M. Rozowsky, F. Migliavacca, S. Berceli, and C. Chiastra. In-stent restenosis progression in human superficial femoral arteries: dynamics of lumen remodeling and impact of local hemodynamics. Ann. Biomed. Eng. 49:2349–2364, 2021.
Dobrin, P. B. Mechanical factors associated with the development of intimal and medial thickening in vein grafts subjected to arterial pressure. A model of arteries exposed to hypertension. Hypertension. 26:38–43, 1995.
Donadoni, F., C. Pichardo-Almarza, S. Homer-Vanniasinkam, A. Dardik, and V. Diaz-Zuccarini. Multiscale, patient-specific computational fluid dynamics models predict formation of neointimal hyperplasia in saphenous vein grafts. J. Vasc. Surg. Cases. Innov. Tech. 6:292–306, 2020.
Fillinger, M. F., J. L. Cronenwett, S. Besso, D. B. Walsh, and R. M. Zwolak. Vein adaptation to the hemodynamic environment of infrainguinal grafts. J. Vasc. Surg. 19:970–978, 1994.
Fledderus, J. O., R. A. Boon, O. L. Volger, H. Hurttila, S. Yla-Herttuala, H. Pannekoek, A.-L. Levonen, and A. J. G. Horrevoets. KLF2 Primes the antioxidant transcription factor Nrf2 for activation in endothelial cells. Arterioscler. Thromb. Vasc. Biol. 28:1339–1346, 2008.
Fledderus, J. O., J. V. van Thienen, R. A. Boon, R. J. Dekker, J. Rohlena, O. L. Volger, A.-P.J.J. Bijnens, M. J. A. P. Daemen, J. Kuiper, T. J. C. van Berkel, H. Pannekoek, and A. J. G. Horrevoets. Prolonged shear stress and KLF2 suppress constitutive proinflammatory transcription through inhibition of ATF2. Blood. 109:4249–4257, 2007.
Garbey, M., and S. A. Berceli. A dynamical system that describes vein graft adaptation and failure. J. Theor. Biol. 336:209–220, 2013.
Glagov, S. Intimal hyperplasia, vascular modeling, and the restenosis problem. Circulation. 89:2888–2891, 1994.
Gusic, R. J., R. Myung, M. Petko, J. W. Gaynor, and K. J. Gooch. Shear stress and pressure modulate saphenous vein remodeling ex vivo. J. Biomech. 38:1760–1769, 2005.
He, X., and D. N. Ku. Pulsatile flow in the human left coronary artery bifurcation: average conditions. J. Biomech. Eng. 118:74–82, 1996.
He, Y., K. DeSart, P. S. Kubilis, A. Irwin, R. Tran-Son-Tay, P. R. Nelson, and S. A. Berceli. Heterogeneous and dynamic lumen remodeling of the entire infrainguinal vein bypass grafts in patients. J. Vasc. Surg. 71:1620, 2020.
He, Y., C. M. Fernandez, Z. Jiang, M. Tao, K. A. O’Malley, and S. A. Berceli. Flow reversal promotes intimal thickening in vein grafts. J. Vasc. Surg. 60:471–478, 2014.
He, Y., H. Northrup, H. Le, A. K. Cheung, S. A. Berceli, and Y. T. Shiu. Medical image-based computational fluid dynamics and fluid-structure interaction analysis in vascular diseases. Front. Bioeng. Biotechnol.10:855791, 2022.
He, Y., C. M. Terry, C. Nguyen, S. A. Berceli, Y. T. Shiu, and A. K. Cheung. Serial analysis of lumen geometry and hemodynamics in human arteriovenous fistula for hemodialysis using magnetic resonance imaging and computational fluid dynamics. J. Biomech. 46:165–169, 2013.
Jackson, M., N. B. Wood, S. Zhao, A. Augst, J. H. Wolfe, W. M. W. Gedroyc, A. D. Hughes, S. A. M. Thom, and X. Y. Xu. Low wall shear stress predicts subsequent development of wall hypertrophy in lower limb bypass grafts. Artery. Res. 3:32–38, 2009.
Jacot, J. G., I. Abdullah, M. Belkin, M. Gerhard-Herman, P. Gaccione, J. F. Polak, M. C. Donaldson, A. D. Whittemore, and M. S. Conte. Early adaptation of human lower extremity vein grafts: wall stiffness changes accompany geometric remodeling. J. Vasc. Surg. 39:547–555, 2004.
Jiang, Z., L. Wu, B. L. Miller, D. R. Goldman, C. M. Fernandez, Z. S. Abouhamze, C. K. Ozaki, and S. A. Berceli. A novel vein graft model: adaptation to differential flow environments. Am. J. Physiol. Heart Circ. Physiol. 286:H240–H245, 2004.
Klein, B., A. Destephens, L. Dumeny, Q. Hu, Y. He, K. O’Malley, Z. Jiang, R. Tran-Son-Tay, and S. Berceli. Hemodynamic influence on smooth muscle cell kinetics and phenotype during early vein graft adaptation. Ann. Biomed. Eng. 45:644–655, 2017.
Ku, D. N., D. P. Giddens, C. K. Zarins, and S. Glagov. Pulsatile flow and atherosclerosis in the human carotid bifurcation. Positive correlation between plaque location and low oscillating shear stress. Arteriosclerosis. 5:293–302, 1985.
Longchamp, A., F. Alonso, C. Dubuis, F. Allagnat, X. Berard, P. Meda, F. Saucy, J.-M. Corpataux, D. Sébastien, and J.-A. Haefliger. The use of external mesh reinforcement to reduce intimal hyperplasia and preserve the structure of human saphenous veins. Biomaterials. 35:2588–2599, 2014.
Meyerson, S. L., C. L. Skelly, M. A. Curi, U. M. Shakur, J. E. Vosicky, S. Glagov, L. B. Schwartz, T. Christen, and G. Gabbiani. The effects of extremely low shear stress on cellular proliferation and neointimal thickening in the failing bypass graft. J. Vasc. Surg. 34:90–97, 2001.
Morinaga, K., H. Eguchi, T. Miyazaki, K. Okadome, and K. Sugimachi. Development and regression of intimal thickening of arterially transplanted autologous vein grafts in dogs. J. Vasc. Surg. 5:719–730, 1987.
Osterberg, K., and E. Mattsson. Intimal hyperplasia in mouse vein grafts is regulated by flow. J. Vasc. Res. 42:13–20, 2005.
Owens, C. D., W. J. Gasper, A. S. Rahman, and M. S. Conte. Vein graft failure. J. Vasc. Surg. 61:203–216, 2015.
Owens, C. D., F. J. Rybicki, N. Wake, A. Schanzer, D. Mitsouras, M. D. Gerhard-Herman, and M. S. Conte. Early remodeling of lower extremity vein grafts: inflammation influences biomechanical adaptation. J. Vasc. Surg. 47:1235–1242, 2008.
Owens, C. D., N. Wake, M. S. Conte, M. Gerhard-Herman, and J. A. Beckman. In vivo human lower extremity saphenous vein bypass grafts manifest flow mediated vasodilation. J. Vasc. Surg. 50:1063–1070, 2009.
Owens, C. D., N. Wake, J. G. Jacot, M. Gerhard-Herman, P. Gaccione, M. Belkin, M. A. Creager, and M. S. Conte. Early biomechanical changes in lower extremity vein grafts–distinct temporal phases of remodeling and wall stiffness. J. Vasc. Surg. 44:740–746, 2006.
Papaharilaou, Y., D. J. Doorly, and S. J. Sherwin. The influence of out-of-plane geometry on pulsatile flow within a distal end-to-side anastomosis. J. Biomech. 35:1225–1239, 2002.
Peiffer, V., A. A. Bharath, S. J. Sherwin, and P. D. Weinberg. A novel method for quantifying spatial correlations between patterns of atherosclerosis and hemodynamic factors. J. Biomech. Eng.135:021023, 2013.
Peiffer, V., S. J. Sherwin, and P. D. Weinberg. Does low and oscillatory wall shear stress correlate spatially with early atherosclerosis? A systematic review. Cardiovasc. Res. 99:242–250, 2013.
Ponzini, R., C. Vergara, A. Redaelli, and A. Veneziani. Reliable CFD-based estimation of flow rate in haemodynamics measures. Ultrasound. Med. Biol. 32:1545–1555, 2006.
Rehfuss, J., S. Scali, Y. He, B. Schmit, K. Desart, P. Nelson, and S. Berceli. The correlation between computed tomography and duplex evaluation of autogenous vein bypass grafts and their relationship to failure. J. Vasc. Surg. 62:1546–1554, 2015.
Rowland, E. M., Y. Mohamied, K. Yean Chooi, E. L. Bailey, and P. D. Weinberg. Comparison of statistical methods for assessing spatial correlations between maps of different arterial properties. J. Biomech. Eng. 137:101003, 2015.
Schwartz, L. B., M. K. O’Donohoe, C. M. Purut, E. M. Mikat, P. O. Hagen, and R. L. McCann. Myointimal thickening in experimental vein grafts is dependent on wall tension. J. Vasc. Surg. 15:176–186, 1992.
Sobel, M., M. Yagi, K. Moreno, T. R. Kohler, G. L. Tang, E. S. Wijelath, J. Marshall, and R. D. Kenagy. Anti-phosphorylcholine IgM, an Anti-inflammatory mediator, predicts peripheral vein graft failure: a prospective observational study. Eur. J Vasc. Endovasc. Surg. 57:259–266, 2019.
Stooker, W., M. Gök, P. Sipkema, H. W. M. Niessen, A. Baidoshvili, N. Westerhof, E. K. Jansen, C. R. H. Wildevuur, and L. Eijsman. Pressure-diameter relationship in the human greater saphenous vein. Ann. Thorac. Surg. 76:1533–1538, 2003.
Tran-Son-Tay, R., M. Hwang, M. Garbey, Z. Jiang, C. K. Ozaki, and S. A. Berceli. An experiment-based model of vein graft remodeling induced by shear stress. Ann. Biomed. Eng. 36:1083–1091, 2008.
Tricarico, R., Y. He, L. Laquian, S. T. Scali, R. Tran-Son-Tay, A. W. Beck, and S. A. Berceli. Hemodynamic and anatomic predictors of renovisceral stent-graft occlusion following chimney endovascular repair of juxtarenal aortic aneurysms. J. Endovasc. Ther. 24:880–888, 2017.
Ward, A. O., G. D. Angelini, M. Caputo, P. C. Evans, J. L. Johnson, M. S. Suleiman, R. M. Tulloh, S. J. George, and M. Zakkar. NF-kappaB inhibition prevents acute shear stress-induced inflammation in the saphenous vein graft endothelium. Sci. Rep. 10:15133, 2020.
Zwolak, R. M., M. C. Adams, and A. W. Clowes. Kinetics of vein graft hyperplasia: association with tangential stress. J. Vasc. Surg. 5:126–136, 1987.
Acknowledgements
This study was funded by the U.S. Veterans Affairs Clinical Science Research and Development Merit Review Grant (S.A.B.) and the National Institutes of Health Grant 1K23HL084090 (Peter R Nelson).
Conflict of interest
The authors have no professional or financial conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Jane Grande-Allen oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
He, Y., Tran-Son-Tay, R. & Berceli, S.A. Distinct Temporal Pattern of the Prediction of Lumen Remodeling of Lower Extremity Vein Bypass Grafts by Initial Local Hemodynamics. Ann Biomed Eng 51, 296–307 (2023). https://doi.org/10.1007/s10439-022-03019-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-022-03019-7