Abstract
Purpose
Fetal intra-abdominal umbilical vein varix (FIUVV) can cause thrombosis, fetal growth restriction (FGR), and intrauterine fetal death (IUFD). However, its management and evaluation to avoid fetal risks have not been elucidated. The aim of this study was to develop a novel method to evaluate fetal risks, including FGR and fetal dysfunction via frequent ultrasound examinations.
Methods
A 28-year-old pregnant woman was diagnosed with FIUVV via ultrasound at 26 weeks of gestation and admitted to our hospital. Ultrasound examinations were performed two to three times weekly to evaluate size and shape of the FIUVV and umbilical vein blood flow at the inflow and outflow sites of the FIUVV.
Results
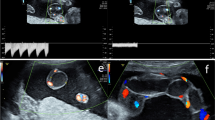
The outflow site of the FIUVV was constricted and collapsed, and the blood flow velocity at the inflow site of the FIUVV was decreased. At 32 weeks of gestation, spontaneous echo contrast (SEC), which indicates increased echogenicity, appeared. At 35 weeks of gestation, the patient noticed decreased fetal movement, and CTG showed non-reassuring fetal status. SEC in the FIUVV was remarkable. Fetal movement could not be confirmed at ultrasound. Cesarean section was performed and a 1,854-g healthy infant was delivered with an umbilical cord arterial pH of 7.266.
Conclusion
The echographic changes, such as decreased umbilical vein blood flow and SEC, in FIUVV observed in this case could indicate thrombus formation, which can lead to fetal dysfunction. Frequent ultrasound examinations can help determine the timing of delivery and improve the neonatal prognosis.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author.
References
Lee SW, Kim MY, Kim JE, et al. Clinical characteristics and outcomes of antenatal fetal intra-abdominal umbilical vein varix detection. Obstet Gynecol Sci. 2014;57:181–6.
Bas-Lando M, Rabinowitz R, Samueloff A, et al. The prenatal diagnosis of isolated fetal varix of the intra-abdominal umbilical vein is associated with favorable neonatal outcome at term: a case series. Arch Gynecol Obstet. 2013;288:33–9.
Weissmann-Brenner A, Simchen MJ, Moran O, et al. Isolated fetal umbilical vein varix–prenatal sonographic diagnosis and suggested management. Prenat Diagn. 2009;29:229–33.
Fung TY, Leung TN, Leung TY, et al. Fetal intra-abdominal umbilical vein varix: what is the clinical significance? Ultrasound Obstet Gynecol. 2005;25:149–54.
Valsky DV, Rosenak D, Hochner-Celnikier D, et al. Adverse outcome of isolated fetal intra-abdominal umbilical vein varix despite close monitoring. Prenat Diagn. 2004;24:451–4.
di Pasquo E, Kuleva M, O’Gorman N, et al. Fetal intra-abdominal umbilical vein varix: retrospective cohort study and systematic review and meta-analysis. Ultrasound Obstet Gynecol. 2018;51:580–5.
Fuster JS, Benasco C, Saad I. Giant dilatation of the umbilical vein. J Clin Ultrasound. 1985;13:363–5.
Gowda S, Chakkalakkoombil SV, Bharathi S, et al. Large fetal intra-abdominal umbilical vein varix: antenatal sonographic diagnosis and follow-up. J Obstet Gynaecol Res. 2019;45:1936–40.
Beraud E, Rozel C, Milon J, et al. Umbilical vein varix: Importance of ante- and post-natal monitoring by ultrasound. Diagn Interv Imaging. 2015;96:21–6.
Merino A, Hauptman P, Badimon L, et al. Echocardiographic “smoke” is produced by an interaction of erythrocytes and plasma proteins modulated by shear forces. J Am Coll Cardiol. 1992;20:1661–8.
Leung DY, Black IW, Cranney GB, et al. Prognostic implications of left atrial spontaneous echo contrast in nonvalvular atrial fibrillation. J Am Coll Cardiol. 1994;24:755–62.
Fatkin D, Kelly RP, Feneley MP. Relations between left atrial appendage blood flow velocity, spontaneous echocardiographic contrast and thromboembolic risk in vivo. J Am Coll Cardiol. 1994;23:961–9.
Mügge A, Kühn H, Nikutta P, et al. Assessment of left atrial appendage function by biplane transesophageal echocardiography in patients with nonrheumatic atrial fibrillation: identification of a subgroup of patients at increased embolic risk. J Am Coll Cardiol. 1994;23:599–607.
Io S, Kondoh E, Iemura Y, et al. Severe fetal anemia as a consequence of extra-abdominal umbilical vein varix: a case report and review of the literature. Congenit Anom (Kyoto). 2021;61:4–8.
Song QY, Tang Y. Foetal death due to extensive extra-abdominal umbilical vein Varix with umbilical vein thrombosis: a case report. BMC Pregnancy Childbirth. 2023;23:155.
Acknowledgements
We thank the woman who participated in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflicts of interest.
Ethical Statements
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions. Informed consent was obtained from the patient for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Takaishi, Y., Kawasaki, K., Uematsu, K. et al. Spontaneous echo contrast and decreased umbilical vein blood flow may predict thrombus formation in fetal intra-abdominal umbilical vein varix. J Med Ultrasonics (2024). https://doi.org/10.1007/s10396-024-01428-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10396-024-01428-w