Abstract
Aim
The aim of this study was to determine the validity and reliability of a sleep hygiene index for the elderly.
Subjects and methods
A total of 598 elderly people (mean age 68.34 years) were selected through cluster sampling, and the validity and reliability of the sleep hygiene index were measured. Confirmatory factor analysis was used to determine the structure validity, internal consistency and reliability of the questionnaire. To this end, Cronbach’s alpha coefficient was used. In addition, concurrent validities with indicators such as sleep quality, Epworth sleepiness, insomnia severity, overall sleepiness measurement and the Berlin Questionnaire were studied.
Results
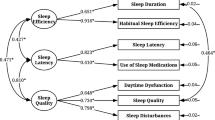
The confirmatory factor analysis indexes of the structural equation model showed that the model fitted well with the data. The χ2/df ratio for the three-factor structure of sleep hygiene was 4.65, and the goodness of fit indices for this structural model (RMSEA = 0.064, CFI =0.9, TLI = 0.9, NFI = 0.9, GFI = 0.9) were good. The Cronbach’s alpha coefficient of the whole scale was 0.78, and the re-test coefficient was 0.87.
Conclusion
The Persian version of the Sleep Hygiene Index can be used as a reliable and valid tool for assessing sleep hygiene in the population of non-clinical elderly.

Similar content being viewed by others
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- SHI:
-
Sleep Health Index
- ISI:
-
Insomnia Severity Index
- ESS:
-
Epworth Sleepiness Scale
- TLI:
-
Tucker-Lewis Index
- NFI:
-
Normed Fit Index
- CFS:
-
Chronic fatigue syndrome
- GFI:
-
Goodness of fit index
- RMSEA:
-
Root mean square error of approximation
- CFI:
-
Confirmatory fit index
- GSAQ:
-
Global Sleep Assessment Questionnaire
- KUMS:
-
Kermanshah University of Medical Sciences
References
Ağargün MY, Kara H, Anlar Ö (1996) The validity and reliability of the Pittsburgh sleep quality index. Turk Psikiyatri Derg 7:107–115
Amorim L et al (2018) Poor sleep quality associates with decreased functional and structural brain connectivity in normative aging: a MRI multimodal approach. Front Aging Neurosci 10:375. https://doi.org/10.3389/fnagi.2018.00375
Amra B, Nouranian E, Golshan M, Fietze I, Penzel T (2013) Validation of the persian version of berlin sleep questionnaire for diagnosing obstructive sleep apnea. Int J Prev Med 4:334–339
Bastien CH, Vallières A, Morin CM (2001) Validation of the insomnia severity index as an outcome measure for insomnia research. Sleep Med 2:297–307
Chehri A, Kiamanesh A, Ahadi H, Khazaie H (2016) Psychometric properties of the Persian version of sleep hygiene index in women. J Kerman Univ Med Sci 19:311–318
Chehri A, Khazaie H, Eskandari S, Khazaie S, Holsboer-Trachsler E, Brand S, Gerber MJB (2017) Validation of the Farsi version of the revised adolescent sleep hygiene scale (ASHSr): a cross-sectional study. BMC Psychiatry 17:408
Cho S, Kim G-S, Lee J-H (2013) Psychometric evaluation of the sleep hygiene index: a sample of patients with chronic pain. Health Qual Life Outcomes 11:213–213. https://doi.org/10.1186/1477-7525-11-213
Farrahi Moghaddam J, Nakhaee N, Sheibani V, Garrusi B, Amirkafi A (2012) Reliability and validity of the Persian version of the Pittsburgh sleep quality index (PSQI-P). Sleep & Breathing = Schlaf & Atmung 16:79–82. https://doi.org/10.1007/s11325-010-0478-5
Irwin MR (2014) Sleep and inflammation in resilient aging. Interface focus 4:20140009–20140009. https://doi.org/10.1098/rsfs.2014.0009
Jefferson CD, Drake CL, Scofield HM, Myers E, McClure T, Roehrs T, Roth T (2005) Sleep hygiene practices in a population-based sample of insomniacs. Sleep 28:611–615
Kang I, Kim S, Kim BS, Yoo J, Kim M, Won CW (2019) Sleep latency in men and sleep duration in women can be frailty markers in community-dwelling older adults: the Korean frailty and aging cohort study (KFACS). J Nutr Health Aging 23:63–67. https://doi.org/10.1007/s12603-018-1109-2
Khazaie H, Chehri A, Sadeghi K, Heydarpour F, Soleimani A, Rezaei Z (2016) Sleep hygiene pattern and behaviors and related factors among general population in west of Iran. Global J Health Sci 8:114
Kline CE, Irish LA, Buysse DJ, Kravitz HM, Okun ML, Owens JF, Hall MH (2014) Sleep hygiene behaviors among midlife women with insomnia or sleep-disordered breathing: the SWAN sleep study. J Women's Health 23:894–903. https://doi.org/10.1089/jwh.2014.4730
Lin C-Y, Strong C, Siu AM, Jalilolghadr S, Nilsen P, Broström A, Pakpour, AHJSM (2018) Validating the Persian adolescent sleep hygiene scale-revised (ASHSr) using comprehensive psychometric testing methods. Sleep Medicine 50:63-71.
Mastin DF, Bryson J, Corwyn R (2006) Assessment of sleep hygiene using the sleep hygiene index. J Behav Med 29:223–227
Mollayeva T, Thurairajah P, Burton K, Mollayeva S, Shapiro CM, Colantonio A (2016) The Pittsburgh sleep quality index as a screening tool for sleep dysfunction in clinical and non-clinical samples: a systematic review and meta-analysis. Sleep Med Rev 25:52–73. https://doi.org/10.1016/j.smrv.2015.01.009
Okun ML, Kravitz HM, Sowers MF, Moul DE, Buysse DJ, Hall M (2009) Psychometric evaluation of the insomnia symptom questionnaire: a self-report measure to identify chronic insomnia. J Clin Sleep Med 5:41–51
Ozdemir PG, Boysan M, Selvi Y, Yildirim A, Yilmaz E (2015) Psychometric properties of the Turkish version of the sleep hygiene index in clinical and non-clinical samples. Compr Psychiatry 59:135–140. https://doi.org/10.1016/j.comppsych.2015.02.001
Popević MB, Milovanović APS, Milovanović S, Nagorni-Obradović L, Nešić D, Velaga M (2018) Reliability and validity of the Pittsburgh sleep quality index-Serbian translation. Eval Health Prof 41:67–81. https://doi.org/10.1177/0163278716678906
Sadeghniiat Haghighi K, Montazeri A, Khajeh Mehrizi A, Aminian O, Rahimi Golkhandan A, Saraei M, Sedaghat M (2013) The Epworth sleepiness scale: translation and validation study of the Iranian version. Sleep & breathing = Schlaf & Atmung 17:419–426. https://doi.org/10.1007/s11325-012-0646-x
Senaratna CV et al (2017) Validity of the Berlin questionnaire in detecting obstructive sleep apnea: a systematic review and meta-analysis. Sleep Med Rev 36:116–124. https://doi.org/10.1016/j.smrv.2017.04.001
Seun-Fadipe CT, Aloba OO, Oginni OA, Mosaku KSJJCSM (2018) Sleep hygiene index: psychometric characteristics and usefulness as a screening tool in a sample of Nigerian undergraduate students. J Clin Sleep Med 14:1285–1292
Sheikhy L, Karami-mattin B, Chupani J, Hookari S, Fallah B (2015) Evaluation the status of sleep quality in elderly people in Kermanshah city. J Rehabil Med 3:81–88. (Inpersian). https://doi.org/10.22037/r.m.v3i4.7850
Simonelli G, Marshall NS, Grillakis A, Miller CB, Hoyos CM, Glozier N (2018) Sleep health epidemiology in low and middle-income countries: a systematic review and meta-analysis of the prevalence of poor sleep quality and sleep duration. Sleep health 4:239–250. https://doi.org/10.1016/j.sleh.2018.03.001
Smith S, Trinder J (2001) Detecting insomnia: comparison of four self-report measures of sleep in a young adult population. J Sleep Res 10:229–235
Storfer-Isser A, Lebourgeois MK, Harsh J, Tompsett CJ, Redline S (2013) Psychometric properties of the adolescent sleep hygiene scale. J Sleep Res 22:707–716. https://doi.org/10.1111/jsr.12059
Suzuki K, Miyamoto M, Hirata K (2017) Sleep disorders in the elderly: diagnosis and management. Journal of general and family medicine 18:61–71. https://doi.org/10.1002/jgf2.27
Tanaka H (2015) Sleep disorder and sleep health promotion for the elderly. Nihon rinsho Japanese journal of clinical medicine 73:909–915
Voinescu BI, Szentagotai-Tatar A (2015) Sleep hygiene awareness: its relation to sleep quality and diurnal preference. Journal of molecular psychiatry 3:1–1. https://doi.org/10.1186/s40303-015-0008-2
Yazdi Z, Sadeghniiat-Haghighi K, Zohal MA, Elmizadeh K (2012) Validity and reliability of the Iranian version of the insomnia severity index. The Malaysian journal of medical sciences : MJMS 19:31–36
Zamanian Z, Nikeghbal K, Khajehnasiri F (2016) Influence of sleep on quality of life among hospital nurses electronic. Physician 8:1811–1816. https://doi.org/10.19082/1811
Acknowledgements
We are grateful to the Deputy for Research and Technology (grant no. 95668), Kermanshah University of Medical Sciences, for cooperating in this research. We thank all the participants in the study.
Author information
Authors and Affiliations
Contributions
Azita Chehri contributed to the study concept, study design, data collection and manuscript preparation.
Layla Parsa contributed to the study concept, study design, data collection and manuscript preparation.
Sepideh Khazaie contributed to the study concept, study design and manuscript preparation.
Habibolah Khazaie contributed to the study concept, study design, data collection and manuscript preparation.
Amir Jalali contributed to the study concept, study design, data analysis, manuscript preparation and submitting the manuscript.
Corresponding author
Ethics declarations
Consent to publication
Not applicable.
Ethics approval and consent to participate
In this research, the ethical considerations including the principles of confidentiality of information, obtaining written informed consent for participating in study, publication and having the right to withdraw from the research at any time were observed. This study was approved by the research committee (grant no. 95668) and ethics committee of Kermanshah University of Medical Sciences (KUMS.REC 1397.678).
Consent for publication
All the authors and the Kermanshah University of Medical Sciences consented to publish the study in this journal.
Conflict of interest
The authors declare that they have no conflict of interest related to this work.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chehri, A., Parsa, L., Khazaie, S. et al. Validation of the sleep hygiene index for the elderly. J Public Health (Berl.) 29, 787–793 (2021). https://doi.org/10.1007/s10389-019-01180-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-019-01180-3