Abstract
Background
Chicago classification version 4.0 suggests additional maneuvers, such as upright testing, multiple rapid swallows (MRS), and the rapid drink challenge (RDC), for high-resolution manometry (HRM) to minimize ambiguity in the diagnosis of esophageal motility disorders. The present study investigated normative thresholds for these new metrics using the Starlet system as well as their diagnostic yields for relevant esophagogastric outflow disorders (EGJOD).
Methods
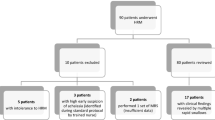
In study 1, 30 asymptomatic volunteers prospectively performed HRM including MRS and RDC in the supine/upright positions. We calculated normative thresholds for the new metrics, such as upright integrated relaxation pressure (IRP), upright intrabolus pressure (IBP), and IRP during RDC (RDC-IRP). In study 2, we retrospectively analyzed the HRM tracings of 82 patients who underwent HRM in both positions at our hospital to assess the diagnostic yields of HRM metrics.
Results
Based on the results of study 1, we adopted the following normative thresholds: upright IRP < 20 mmHg, upright IBP < 21 mmHg, and RDC-IRP < 16 mmHg. In study 2, 45 patients with dysphagia or chest pain were included in the analysis to identify predictive factors for clinically relevant esophagogastric outflow disorders (true EGJOD). Supine/upright IRP, RDC-IRP, and pan-esophageal pressurization > 20 mmHg during RDC (RDC-PEP) predicted true EGJOD with RDC-PEP with the highest sensitivity of 91.7%.
Conclusions
HRM with additional maneuvers may facilitate the diagnosis of clinically relevant EGJOD.



Similar content being viewed by others
Abbreviations
- HRM:
-
High-resolution manometry
- EMD:
-
Esophageal motility disorders
- CCv4.0:
-
Chicago classification version 4.0
- RDC:
-
Rapid drink challenge
- NCCP:
-
Non-cardiac chest pain
- GI:
-
Gastrointestinal
- MRS:
-
Multiple rapid swallows
- FSSG:
-
Frequency scale for the symptoms of GERD
- IRP:
-
Integrated relaxation pressure
- DCI:
-
Distal contractile integral
- DL:
-
Distal latency
- IBP:
-
Intrabolus pressure
- LES:
-
Lower esophageal sphincter
- EGJ-CI:
-
Esophagogastric junction-contractile integral
- PEP:
-
Pan-esophageal pressurization
- EGJOO:
-
Esophagogastric junction outflow obstruction
- IEM:
-
Ineffective esophageal motility
- CCv3.0:
-
Chicago classification version 3.0
- EGJOD:
-
EGJ-outflow disorders
- POEM:
-
Per-oral endoscopic myotomy
- TBE:
-
Timed barium esophagogram
- IQR:
-
Interquartile ranges
- HE:
-
Hypercontractile esophagus
- FLIP:
-
Functional lumen imaging probe
References
Pandolfino JE, Fox MR, Bredenoord AJ, Kahrilas PJ. High-resolution manometry in clinical practice: utilizing pressure topography to classify oesophageal motility abnormalities. Neurogastroenterol Motil. 2009;21:796–806.
Bredenoord AJ, Fox M, Kahrilas PJ, Pandolfino JE, Schwizer W, Smout AJPM. Chicago classification criteria of esophageal motility disorders defined in high resolution esophageal pressure topography. Neurogastroenterol Motil. 2012;24(1):57–65.
Kahrilas PJ, Bredenoord AJ, Fox M, et al. The Chicago classification of esophageal motility disorders, v3.0. Neurogastroenterol Motil. 2015;27:160–74.
Pandolfino JE, Gawron AJ. Achalasia: a systematic review. J Am Med Assoc. 2015;313:1841–52.
Bredenoord AJ, Babaei A, Carlson D, et al. Esophagogastric junction outflow obstruction. Neurogastroenterol Motil. 2021;33: e14193.
Chen JW, Savarino E, Smout A, et al. Chicago classification Update (v4.0): technical review on diagnostic criteria for hypercontractile esophagus. Neurogastroenterol Motility. 2021;33:e14115.
Gyawali CP, Zerbib F, Bhatia S, et al. Chicago classification update (V4.0): technical review on diagnostic criteria for ineffective esophageal motility and absent contractility. Neurogastroenterol Motility. 2021;33:e14134.
Yadlapati R, Kahrilas PJ, Fox MR, et al. Esophageal motility disorders on high-resolution manometry: Chicago classification version 4.0©. Neurogastroenterol Motility. 2020;33:e14058.
Rengarajan A, Rogers BD, Wong Z, et al. High-resolution manometry thresholds and motor patterns among asymptomatic individuals. Clin Gastroenterol Hepatol. 2022;20:e398–406.
Kuribayashi S, Iwakiri K, Shinozaki T, et al. Clinical impact of different cut-off values in high-resolution manometry systems on diagnosing esophageal motility disorders. J Gastroenterol. 2019;54:1078–82.
Kuribayashi S, Iwakiri K, Kawada A, et al. Variant parameter values-as defined by the Chicago Criteria-produced by ManoScan and a new system with Unisensor catheter. Neurogastroenterol Motil. 2015;27:188–94.
Eckardt VF. Clinical presentation and complications of achalasia. Gastrointest Endosc Clin N Am. 2001;11:281–92.
Kusano M, Shimoyama Y, Sugimoto S, et al. Development and evaluation of FSSG: frequency scale for the symptoms of GERD. J Gastroenterol. 2004;39:888–91.
Nicodème F, Pipa-Muniz M, Khanna K, Kahrilas PJ, Pandolfino JE. Quantifying esophagogastric junction contractility with a novel HRM topographic metric, the EGJ-Contractile Integral: normative values and preliminary evaluation in PPI non-responders. Neurogastroenterol Motil. 2014;26:353–60.
Marin I, Cisternas D, Abrao L, et al. Normal values of esophageal pressure responses to a rapid drink challenge test in healthy subjects: results of a multicenter study. Neurogastroenterol Motil. 2017;29:1–8.
Marin I, Caballero N, Guarner-Argente C, Serra J. Rapid drink challenge test for the clinical evaluation of patients with Achalasia. Neurogastroenterol Motil. 2018;30:1–8.
Triggs JR, Carlson DA, Beveridge C, et al. Upright integrated relaxation pressure facilitates characterization of esophagogastric junction outflow obstruction. Clin Gastroenterol Hepatol. 2019;17:2218-2226.e2.
Masuda T, Yano F, Omura N, et al. Optimal cutoff value of integrated relaxation pressure on the esophagogastric junction to detect outflow obstruction using starlet high-resolution manometry system. J Gastroenterol. 2021;56:231–9.
Kanda Y. Statistical analysis using freely-available “EZR (Easy R)” software [Rinshō ketsueki]. Jpn J Clin Hematol. 2015;56:2258–66.
Aziz Q, Fass R, Gyawali CP, et al. Esophageal disorders. Gastroenterology. 2016;150:1368–79.
Fox MR, Sweis R, Yadlapati R, et al. Chicago classification version 4.0© technical review: update on standard high-resolution manometry protocol for the assessment of esophageal motility. Neurogastroenterol Motility. 2021;33:e14120.
Su H, Ge H, Liu H, et al. High-resolution manometry in the upright position could improve the manometric evaluation of morbidly obese patients with esophagogastric junction outflow obstruction. Neurogastroenterol Motil. 2020;32: e13924.
Lis S, Vachhani H, Tanner S, et al. Vascular pressure bands on high-resolution esophageal manometry with impedance studies. Dis Esophagus. 2020;33:1–6.
Su H, Krause AJ, Masihi M, et al. Normal values of high-resolution manometry parameters with provocative maneuvers. J Neurogastroenterol Motility. 2021;27:354–62.
Misselwitz B, Hollenstein M, Bütikofer S, et al. Prospective serial diagnostic study: the effects of position and provocative tests on the diagnosis of oesophageal motility disorders by high-resolution manometry. Aliment Pharmacol Ther. 2020;51:706–18.
Marin I, Serra J. Patterns of esophageal pressure responses to a rapid drink challenge test in patients with esophageal motility disorders. Neurogastroenterol Motil. 2016;28:543–53.
Woodland P, Gabieta-Sonmez S, Arguero J, et al. 200 Ml rapid drink challenge during high resolution manometry best predicts objective esophagogastric junction obstruction and correlates with symptom severity. J Neurogastroenterol Motility. 2018;24(3):410–4. https://doi.org/10.5056/jnm18038.
Vaezi MF, Pandolfino JE, Yadlapati RH, et al. ACG clinical guidelines: diagnosis and management of achalasia. Am J Gastroenterol. 2020;115:1393–411.
Ponds FA, Bredenoord AJ, Kessing BF, et al. Esophagogastric junction distensibility identifies achalasia subgroup with manometrically normal esophagogastric junction relaxation. Neurogastroenterol Motil. 2017;29:1–8.
Iwakiri K, Hoshihara Y, Kawami N, et al. The appearance of rosette-like esophageal folds (' “esophageal rosette”’) in the lower esophagus after a deep inspiration is a characteristic endoscopic finding of primary achalasia. J Gastroenterol. 2010;45:422–5.
Hoshikawa Y, Hoshino S, Kawami N, et al. Possible new endoscopic finding in patients with achalasia: “Gingko leaf sign.” Esophagus. 2020;17:208–13.
Blonski W, Kumar A, Feldman J, et al. Timed barium swallow: diagnostic role and predictive value in untreated Achalasia, esophagogastric junction outflow obstruction, and non-Achalasia dysphagia. Am J Gastroenterol. 2018;113:196–203.
Carlson DA, Prescott JE, Baumann AJ, et al. Validation of clinically relevant thresholds of esophagogastric junction obstruction using FLIP Panometry. Clin Gastroenterol Hepatol. 2022;20:e1250–62.
Xiao Y, Kahrilas PJ, Kwasny MJ, et al. High resolution manometry correlates of ineffective esophageal motility. Am J Gastroenterol. 2012;107:1647–54.
Carlson DA, Roman S. Esophageal provocation tests: are they useful to improve diagnostic yield of high resolution manometry? Neurogastroenterol Motil. 2018;30:1–7.
Acknowledgements
The authors thank Ms. Satoko Nishimura for her administrative assistance.
Funding
The authors received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
YH, SK, and KI contributed to the study conception and design. Material preparation and data collection were performed by YH, EM, NK. Data analyses were performed by YH and MI. The first draft of the manuscript was written by YH, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest associated with this manuscript.
Ethical standard
The study protocol was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board (B-2021-377). Informed consent was obtained from all participants. The present study was registered in the UMIN clinical trial register system [UMIN000046572].
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hoshikawa, Y., Momma, E., Kawami, N. et al. High-resolution manometry with additional maneuvers using the Starlet system: normative thresholds and diagnostic yields for relevant esophagogastric junction outflow disorders. Esophagus 20, 150–157 (2023). https://doi.org/10.1007/s10388-022-00956-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10388-022-00956-z