Abstract
Background
The presence of Barrett’s mucosa in the esophageal remnant is a result of post-esophagectomy anastomotic site exposure to gastric acid and is regarded as a human model of Barrett’s esophagus onset. Here, we attempted to clarify the relationship between duodenogastric reflux and formation of columnar epithelium by following the changes over time after esophagectomy.
Methods
A total of 96 patients underwent esophagectomy due to superficial cancer from April 2000 to March 2018 were included in this study. Cases were divided into two groups according to the reconstruction technique after esophagectomy as either the gastric pull-up (Ga) group and ileocolonic interposition (Ic) group. Previously obtained endoscopic pictures of the cases were reviewed retrospectively and chronologically.
Results
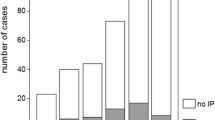
There were 24 cases of columnar epithelium in the Ga group (42%) and 1 in the Ic group (2.6%) (P < 0.01) with 32 reflux cases (56%) in the Ga group and 1 (2.6%) in the Ic group (P < 0.01). Reflux precedes the development of columnar epithelium in both the Ga- and Ic groups. Multivariate analysis revealed surgical technique (odds ratio 10.6, 95% CI 1.2–97.5, P = 0.037) and reflux (odds ratio 4.5, 95% CI 1.3–15.6, P = 0.0017) as risk factors.
Conclusions
The development of columnar epithelium was preceded by reflux comprising principally gastric acid and was strongly associated with a strong inflammatory state.






Similar content being viewed by others
References
Li Y, Martin RC. Reflux injury of esophageal mucosa: experimental studies in animal models of esophagitis, Barrett’s esophagus and esophageal adenocarcinoma. Dis Esophagus. 2007;20:372–8.
Mukaisho K, Miwa K, Hattori T, et al. Gastric carcinogenesis by duodenal reflux through gut regenerative cell lineage. Dig Dis Sci. 2003;48:2153–8.
Dunn LJ, Shenfine J, Griffin SM. Columnar metaplasia in the esophageal remnant after esophagectomy: a systematic review. Dis Esophagus. 2015;28:32–41.
Kimura K, Takemoto T. An endoscopic recognition of the atrophic border and its significance in chronic gastritis. Endoscopy. 1969;3:87–97.
Franchimont D, Covas A, Brasseur C, Van Laethem J-L, El-Nakadi I, Deviere J. Newly developed Barrett’s esophagus after subtotal esophagectomy. Endoscopy. 2003;35:850–3.
O’Riordan J, Tucker O, Byrne P, et al. Factors influencing the development of Barrett’s epithelium in the esophageal remnant postesophagectomy. Am J Gastroenterol. 2004;99:205–11.
da Rocha J, Ribeiro U, Sallum R, Szachnowicz S, Cecconello I. Barrett’s Esophagus (BE) and carcinoma in the esophageal stump (ES) after esophagectomy with gastric pull-up in achalasia patients: a study based on 10 years follow-up. Ann Surg Oncol. 2008;15:2903–9.
D’Journo X, Martin J, Rakovich G, et al. Mucosal damage in the esophageal remnant after esophagectomy and gastric transposition. Ann Surg. 2009;249:262–8.
Nishimura K, Tanaka T, Tanaka K, et al. Refluxesophagitisand columnar-lined esophagus after cervical esophagogastrostomy (following esophagectomy). Dis Esophagus. 2010;23:94–9.
Tsiouris A, Hammond Z, Velanovich V. Barrett’s esophagus after resection of the gastroesophageal junction: effects of concomitant fundoplication. World J Surg. 2011;35:1867–72.
Aly A, Jamieson GG, Watson DI, et al. An antireflux anastomosis following esophagectomy: a randomized controlled trial. J Gastrointest Surg. 2010;14:470–5.
Yuasa N, Sasaki E, Ikeyama T, Miyake H, Nimura Y. Acid and duodenogastroesophageal reflux after esophagectomy with gastric tube reconstruction. Am J Gastroenterol. 2005;100:1021–7.
Gutschow C, Vallböhmer D, Stolte M, et al. Adenocarcinoma developing indenovo Barrett’s mucosa in the remnant esophagus after esophagectomy: clinical and molecular assessment. Dis Esophagus. 2008;21:E6–E8.
Wolfsen H, Hemminger L, DeVault K. Recurrent Barrett’s esophagus and adenocarcinoma after esophagectomy. BMC Gastroenterol. 2004;4:18.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki declaration of 1964 and later versions.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Iizuka, T., Suzuki, Y., Kikuchi, D. et al. Columnar epithelium morphology after esophagectomy: clinical insight into the development of Barrett’s esophagus. Esophagus 17, 392–398 (2020). https://doi.org/10.1007/s10388-020-00742-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10388-020-00742-9