Abstract
Purpose
To evaluate the changes in anterior chamber flare after a single intravitreal injection of ocriplasmin (125 μg), in patients with symptomatic vitreomacular traction syndrome (VMT).
Study design
An institutional review board-approved single-center not randomized prospective study.
Methods
Fifteen eyes of fifteen patients (9 women, 6 men) underwent intravitreal injection with ocriplasmin for symptomatic VMT (width of attachment ≤ 1500 μm). Anterior segment flare was measured with a laser flare meter (Kowa) before intravitreal injection and 1 day, 1 week, 1 month after injection. The changes in flare were analyzed; the resolution of VMT was evaluated with spectral-domain OCT.
Results
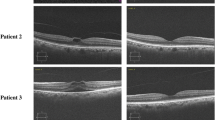
The mean anterior chamber flare was 10.5 ± 1.9 photons per millisecond (photons/ms) before the injection. After 1 day it increased to 13.6 ± 2.7 photons/ms (p = 0.027) and after 1 week to 14.4 ± 2.5 photons/ms (p = 0.005); after 1 month it decreased to 12.3 ± 2.3 photons/ms (p = 0.123). At 1 day and 1 week after injection, mean anterior chamber flare of fellow eyes was significantly lower than study eyes, while at 1 month this difference was not significant (12.3 ± 2.3 vs. 10.5 ± 1.8 photons/ms, p = 0.124, for study and fellow eyes). There was no statistically significant difference in the changes in flare between women and men or between phakic (N = 10) and pseudophakic (N = 5) eyes. No eye demonstrated intraretinal damage at any time-point. Also, 9 eyes showed resolution of VMT while 6 eyes demonstrated persistence of VMT.
Conclusion
Our study shows that intravitreal injection of ocriplasmin can be a safe and effective approach to treat symptomatic VMT syndrome in selected patients.


Similar content being viewed by others
References
Reese AB, Jones IS, Cooper WC. Vitreomacular traction syndrome confirmed histologically. Am J Ophthalmol. 1970;69:975–7.
Jackson TL, Nicod E, Simpson A, Angelis A, Grimaccia F, Kanavos P. Symptomatic vitreomacular adhesion. Retina. 2013;33:1503–11.
Johnson MW. How should we release vitreomacular traction: surgically, pharmacologically, or pneumatically? Am J Ophthalmol. 2013;155:203–205.e1.
Duker JS, Kaiser PK, Binder S, de Smet MD, Gaudric A, Reichel E, et al. The International Vitreomacular Traction Study Group classification of vitreomacular adhesion, traction, and macular hole. Ophthalmology. 2013;120:2611–9.
Hahn P, Chung MM, Flynn HW, Huang SS, Kim JE, Mahmoud TH, et al. Safety profile of ocriplasmin for symptomatic vitreomacular adhesion: a comprehensive analysis of premarketing and postmarketing experiences. Retina. 2015;35:1128–34.
Shah SP, Jeng-Miller KW, Fine HF, Wheatley HM, Roth DB, Prenner JL. Post-marketing survey of adverse events following ocriplasmin. Ophthalmic Surg Lasers Imaging Retina. 2016;47:156–60.
Figueira J, Martins D, Pessoa B, Ferreira N, Meireles A, Sampaio A, et al. The Portuguese experience with ocriplasmin in clinical practice. Ophthalmic Res. 2016;56(4):186–92.
Tyndall J. On the blue of the sky, the polarization of the skylight, and on the polarization of light by cloudy matter generally. Philos Mag J Sci. 1869;37:384–404.
Sawa M, Tsurimaki Y, Tsuru T, Shimizu H. New quantitative method to determine protein concentration and cell number in aqueous in vivo. Jpn J Ophthalmol. 1988;32:132–42.
Shah SM, Spalton DJ, Taylor JC. Correlations between laser flare measurements and anterior chamber protein concentrations. Investig Ophthalmol Vis Sci. 1992;33:2878–84.
el-Harazi SM, Feldman RM, Chuang AZ, Ruiz RS, Villanueva G. Reproducibility of the laser flare meter and laser cell counter in assessing anterior chamber inflammation following cataract surgery. Ophthalmic Surg Lasers. 1998;29:380–4.
Tugal-Tutkun I, Herbort CP. Laser flare photometry: a noninvasive, objective, and quantitative method to measure intraocular inflammation. Int Ophthalmol. 2010;30:453–64.
Blaha G, Brooks N, Mackel C, Pani A, Stewart AP, Price LL, et al. Changes in flare after intravitreal injection of three different anti-vascular endothelial growth factor medications. Retina. 2015;35:577–81.
Uzun A, Yalcindag FN, Demirel S, Batýoðlu F, Ozmert E. Evaluation of aqueous flare levels following intravitreal ranibizumab injection for neovascular age-related macular degeneration. Ocul Immunol Inflamm. 2017;25:229–32.
Morioka M, Takamura Y, Yamada Y, Matsumura T, Gozawa M, Inatani M. Flare levels after intravitreal injection of ranibizumab, aflibercept, or triamcinolone acetonide for diabetic macular edema. Graefes Arch Clin Exp Ophthalmol. 2018;256:2301–7.
Quiram P, Leverenz V, Baker R, Dang L, Giblin F, Trese M. Microplasmin-induced posterior vitreous detachment affects vitreous oxygen levels. Retina. 2007;27:1090–6.
Shaikh M, Miller JB, Papakostas TD, Husain D. The efficacy and safety profile of ocriplasmin in vitreomacular interface disorders. Semin Ophthalmol. 2017;32:52–5.
Itoh Y, Kaiser PK, Singh RP, Srivastava SK, Ehlers JP. Assessment of retinal alterations after intravitreal ocriplasmin with spectral-domain optical coherence tomography. Ophthalmology. 2014;121:2506–7.e2.
Sakuma T, Tanaka M, Mizota A, Inoue J, Pakola S. Safety of in vivo pharmacologic vitreolysis with recombinant microplasmin in rabbit eyes. Investig Ophthalmol Vis Sci. 2015;46:3295–9.
Chatziralli I, Theodossiadis G, Parikakis E, Datseris I, Theodossiadis P. Real-life experience after intravitreal ocriplasmin for vitreomacular traction and macular hole: A spectral-domain optical coherence tomography prospective study. Graefes Arch Clin Exp Ophthalmol. 2016;254:223–33.
Conflicts of interest
V. Pirani, None; P. Pelliccioni, None; C. Cesari, None; G. Carrozzi, None; E. Cavallero, None; C. Mariotti, None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding author: Paolo Pelliccioni
About this article
Cite this article
Pirani, V., Pelliccioni, P., Cesari, C. et al. Flare changes after intravitreal injection of ocriplasmin in symptomatic vitreomacular traction syndrome. Jpn J Ophthalmol 63, 255–261 (2019). https://doi.org/10.1007/s10384-019-00660-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-019-00660-z