Abstract
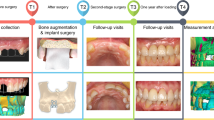
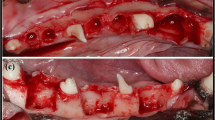
The guided bone regeneration (GBR) technique is often applied to provide sufficient bone for ideal implant placement. The objective of this study was to evaluate whether GC membrane®, which has already been used for guided tissue regeneration (GTR), can also be available for GBR. Twenty-three implants in 18 patients were evaluated in the study. All patients underwent implant placement with GBR using GC membrane®. Cone-beam computed tomography was performed at 13–30 weeks after surgery and the amount of augmented bone was assessed. The implant stability quotient (ISQ) was measured at the second operation to evaluate implant stability. Although wound dehiscence was observed at 4 of 23 regions (17.4%), all wounds closed quickly without any events by additional antibiotic administration. GBR-induced bone augmentation of 0.70–2.56 mm horizontally and 0–6.82 mm vertically. Only 0.18 mm of bone recession was observed at 16–24 months after implant placement. GBR with GC membrane® induced sufficient bone augmentation, leading to successful implant treatment. The present results suggest that GC membrane® is available not only for GTR, but also for GBR.





Similar content being viewed by others
References
Tanaka K. A comparison between the upper and lower jaws of the alveolar bone changes due to the extraction of frontal teeth. Shika Kiso Igakkai Zasshi. 1989;31:148–83 (in Japanese).
Hermann JS, Buser D. Guided bone regeneration for dental implants. Curr Opin Periodontol. 1996;3:168–77.
Rakhmatia YD, Ayukawa Y, Furuhashi A, Koyano K. Current barrier membranes: titanium mesh and other membranes for guided bone regeneration in dental applications. J Prosthod Res. 2013;57:3–14.
Konstantinidis I, Kumar T, Kher U, Stanitsas PD, Hinriches JE, Kotsakis GA. Clinical results of implant placement in resorbed ridges using simultaneous guided bone regeneration: a multicenter case series. Clin Oral Invest. 2015;19:553–9.
Shneider D, Weber FE, Grunder U, Andreoni C, Burkhardt R, Jung RE. A randomized controlled clinical multicenter trial comparing the clinical and histological performance of a new, modified polyactide-co-glycolide acid membrane to an expanded polytetrafluorethylene membrane in guided bone regeneration procedures. Clin Oral Impl Res. 2014;25:150–8.
Bunyaratavej P, Wang HL. Collagen membranes: a review. J Periodontol. 2001;72:215–29.
Rodella LF, Favero G, Labanca M. Biomaterials in maxillofacial surgery: membranes and grafts. Int J Biomed Sci. 2011;7:81–8.
Geurs NC, Korostoff JM, Vassilopoulos PJ, Kang TH, Jeffcoat M, Kellar R, Reddy MS. Clinical and histologic assessment of lateral alveolar ridge augmentation using a synthetic long-term bioabsorbable membrane and an allograft. J Periodontol. 2008;79:1133–40.
Yamada S, Matsumoto Y, Takahashi Y, Yamanouchi K, Aoki H, Sato T, Ishikawa T, Hyon SH, Ikada Y. Histopathological study of poly (lactic acid-co-glycolic acid) membranes to guided tissue regeneration in dogs. Jpn Clin Periodontol. 1991;33:396–405 in Japanese.
Yamanouchi K, Nakagawa T, Seida K, Saito A, Yamada S, Hiwatashi K, Setoguchi T, Chuman M, Sueda T. Clinical study on the effect of absorbable membrane applied to guided tissue regeneration technique. Jpn Clin Periodontol. 1994;36:884–94 in Japanese.
Buser D, Brägger U, Lang NP, Nyman S. Regeneration and enlargement of jaw bone using guided tissue regeneration. Clin Oral Impl Res. 1990;1:22–32.
Chiapasco M, Romeo E, Casentini P, Rimondini L. Alveolar distraction osteogenesis vs. vertical guided bone regeneration for the correction of vertically deficient edentulous ridges; a 1-3-year prospective study on humans. Clin Oral Impl Res. 2004;15:82–95.
Duyck J, Vandamme K. The effect of loading on peri-implant bone: a critical review of the literature. J Oral Rehab. 2014;41:783–94.
Mario MS, Sacha A J, Istvan U, Luigi C, Milena P, Marco T. Horizontal ridge augmentation using GBR with a native collagen membrane and 1:1 ratio of particulated xenograft and autologous bone: A 1-year prospective clinical study. Clin Impl Dent Relat Res. In press.
Le B, Borzabadi-Farahani A, Nielsen B. Treatment of labial soft tissue recession around dental implants in the esthetic zone using guided bone regeneration with mineralized allograft: a retrospective clinical case series. J Oral Maxillofac Surg. 2016;74:1552–61.
Lόpez AB, Martínez JB, Pelayo JL, Carcía CC, Diago MP. Resonance frequency analysis of dental implant stability during the healing period. Med Oral Pathol Oral Cir Bucal. 2008;13:e244–7.
Aimetti M, Romano F, Pigella E, Pranzini F, Debernardi C. Treatment of wide, shallow, and predominantly 1-wall intrabony defects with a bioabsorbable membrane: a randomized controlled clinical trial. J Periodontol. 2005;76:1354–61.
McGinnis M, Larsen P, Miloro M, Beck M. Comparison of resorbable and nonresorbable guided bone regeneration materials: a preliminary study. Int J Oral Maxillofac Implants. 1998;13:30–5.
Jung RE, Benic GI, Scherrer D, Hämmerle CHF. Cone beam computed tomography evaluation of regenerated buccal bone 5 years after simultaneous implant placement and guided bone regeneration procedures—a randomized, controlled clinical trial. Clin Oral Impl Res. 2015;26:28–34.
Ramel CF, Wismeijer DA, Hammerle CH, Jung RE. A randomized, controlled clinical evaluation of a synthetic gel membrane for guided bone regeneration around dental implants: clinical and radiologic 1- and 3-year results. Int J Oral Maxillofac Impl. 2012;27:435–41.
Becker W, Urist M, Becker BE, Jackson W, Parry DA, Bartold M, Vincenzzi G, Georges DD, Niederwanger M. Clinical and histologic observations of sites implanted with intraoral autologous bone grafts or allografts. 15 human case reports. J Periodontol. 1996;67:1025–33.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kawasaki, T., Ohba, S., Nakatani, Y. et al. Clinical study of guided bone regeneration with resorbable polylactide-co-glycolide acid membrane. Odontology 106, 334–339 (2018). https://doi.org/10.1007/s10266-018-0349-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-018-0349-2