Abstract
In this study, we present a method to experimentally quantify and numerically identify the constituent-specific material behavior of soft biological tissues. This allows the clear identification of the individual contributions of major load-bearing constituents and their interactions in the constitutive law. While the overall approach is applicable for many tissues, here it will be presented for the identification of a sophisticated constituent-specific material model of viable lung parenchyma. This material model will help to better model the effects of various lung diseases that feature altered fiber content in the lungs, such as emphysema or fibrosis. To experimentally quantify the mechanical properties of collagen, elastin, collagen–elastin–fiber interactions, and ground substance, we examined 18 collagenase and elastase treated rat lung parenchymal slices. The mechanical contributions of the collagen and elastin fibers in the living tissue were inferred from uniaxial tension tests comparing the behavior before and after the selective digestion of the respective fibers. In order to also obtain the mechanical influence of the ground substance, we consecutively treated the samples with both proteases. Collagen and elastin fibers are morphologically interconnected. Thus, a mechanical interaction between these fibers appears likely, but has not yet been experimentally verified. In this paper, we propose an experimental method to quantitatively assess the mechanical behavior of these collagen–elastin–fiber interactions. Based on our experiments, we have identified individual material models within a nonlinear continuum mechanics framework for each load-bearing component via an inverse analysis. The proposed constituent-specific material law can be incorporated into computational models of the respiratory system to simulate and even predict the behavior and alteration of the individual constituents and their effect on the whole respiratory system during normal and artificial breathing, in particular in the case of diseases that alter the fibers in the tissue.


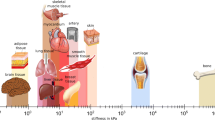
Adapted from Birzle et al. (2019), with permission








Similar content being viewed by others
References
Al Jamal R, Roughley PJ, Ludwig MS (2001) Effect of glycosaminoglycan degradation on lung tissue viscoelasticity. Am J Physiol Lung Cell Mol 280(2):L306–L315. https://doi.org/10.1152/ajplung.2001.280.2.L306
Barbir A, Michalek AJ, Abbott RD, Iatridis JC (2010) Effects of enzymatic digestion on compressive properties of rat intervertebral discs. J Biomech 43(6):1067–1073. https://doi.org/10.1016/j.jbiomech.2009.12.005
Bel-Brunon A, Kehl S, Martin C, Uhlig S, Wall WA (2014) Numerical identification method for the non-linear viscoelastic compressible behavior of soft tissue using uniaxial tensile tests and image registration application to rat lung parenchyma. J Mech Behav Biomed Mater 29:360–374. https://doi.org/10.1016/j.jmbbm.2013.09.018
Berger L, Bordas R, Burrowes K, Grau V, Tavener S, Kay D (2016) A poroelastic model coupled to a fluid network with applications in lung modelling. Int J Numer Method Biomed Eng. https://doi.org/10.1002/cnm.2731
Birzle AM, Wall WA (2019) A viscoelastic, nonlinear, compressible material model of lung parenchyma: experiments and numerical identification. J Mech Behav Biomed Mater (in press). https://doi.org/10.1016/j.jmbbm.2019.02.024
Birzle AM, Martin C, Yoshihara L, Uhlig S, Wall WA (2018) Experimental characterization and model identification of the nonlinear compressible material behavior of lung parenchyma. J Mech Behav Biomed Mater 77(Suppl C):754–763. https://doi.org/10.1016/j.jmbbm.2017.08.001
Birzle AM, Martin C, Uhlig S, Wall WA (2019) A coupled approach for identification of nonlinear and compressible material models for soft tissue based on different experimental setups: exemplified and detailed for lung parenchyma. J Mech Behav Biomed Mater 94:126–143. https://doi.org/10.1016/j.jmbbm.2019.02.019
Brewer KK, Sakai H, Alencar AM, Majumdar A, Arold SP, Lutchen KR, Ingenito EP, Suki B (2003) Lung and alveolar wall elastic and hysteretic behavior in rats: effects of in vivo elastase treatment. J Appl Physiol 95:1926–1936. https://doi.org/10.1152/japplphysiol.00102.2003
Brown RE, Butler JP, Rogers RA, Leith DE (1994) Mechanical connections between elastin and collagen. Connect Tissue Res 30(4):295–308. https://doi.org/10.3109/03008209409015044
Burgstaller G, Oehrle B, Gerckens M, White ES, Schiller HB, Eickelberg O (2017) The instructive extracellular matrix of the lung: basic composition and alterations in chronic lung disease. Eur Respir J 50(1):1601805. https://doi.org/10.1183/13993003.01805-2016
Carton RW, Dainauskas J, Clark JW (1962) Elastic properties of single elastic fibers. J Appl Physiol 17(3):547–551. https://doi.org/10.1152/jappl.1962.17.3.547
Cavalcante FSA, Ito S, Brewer K, Sakai H, Alencar AM, Almeida MP, Andrade JS, Majumdar A, Ingenito EP, Suki B (2005) Mechanical interactions between collagen and proteoglycans: implications for the stability of lung tissue. J Appl Physiol 98(2):672–679. https://doi.org/10.1152/japplphysiol.00619.2004
Ceresa M, Olivares AL, Noailly J, Ballester GAM (2018) Coupled immunological and biomechanical model of emphysema progression. Front Physiol. https://doi.org/10.3389/fphys.2018.00388
Chow MJ, Turcotte R, Lin C, Zhang Y (2014) Arterial extracellular matrix: a mechanobiological study of the contributions and interactions of elastin and collagen. Biophys J 106(12):2684–2692. https://doi.org/10.1016/j.bpj.2014.05.014
Debes JC, Fung YC (1992) Effect of temperature on the biaxial mechanics of excised lung parenchyma of the dog. J Appl Psychol 73(3):1171–1180. https://doi.org/10.1152/jappl.1992.73.3.1171
Dobrin PB, Canfield TR (1984) Elastase, collagenase, and the biaxial elastic properties of dog carotid artery. Am J Physiol Heart Circ Physiol 247(1):H124–H131. https://doi.org/10.1152/ajpheart.1984.247.1.H124
Ethier CR, Simmons CA (2007) Introductory biomechanics: from cells to organisms. Cambridge University Press, Cambridge
Eyre DR, Paz MA, Gallop PM (1984) Cross-linking in collagen and elastin. Annu Rev Biochem 53(1):717–748. https://doi.org/10.1146/annurev.bi.53.070184.003441
Faffe DS, Zin WA (2009) Lung parenchymal mechanics in health and disease. Physiol Rev 89(3):759–775. https://doi.org/10.1152/physrev.00019.2007
Fonck E, Prod’hom G, Roy S, Augsburger L, Rüfenacht DA, Stergiopulos N (2007) Effect of elastin degradation on carotid wall mechanics as assessed by a constituent-based biomechanical model. Am J Physiol Heart Circ Physiol 292(6):H2754–H2763. https://doi.org/10.1152/ajpheart.01108.2006
Fratzl P, Misof K, Zizak I, Rapp G, Amenitsch H, Bernstorff S (1998) Fibrillar structure and mechanical properties of collagen. J Struct Biol 122(1):119–122. https://doi.org/10.1006/jsbi.1998.3966
Fung YC (1993) Biomechanics: mechanical properties of living tissues, 2nd edn. Springer, New York
Fust A, LeBellego F, Iozzo RV, Roughley PJ, Ludwig MS (2005) Alterations in lung mechanics in decorin-deficient mice. Am J Physiol Lung Cell Mol Physiol 288(1):L159–L166. https://doi.org/10.1152/ajplung.00089.2004
Hance AJ, Crystal RG (1975) The connective tissue of lung. Am Rev Respir Dis 112(5):657–711. https://doi.org/10.1164/arrd.1975.112.5.657
Hartley BS, Shotton DM (1971) Pancreatic elastase. In: Boyer PD (ed) The enzymes, hydrolysis: peptide bonds, vol 3. Academic Press, New York, pp 323–373. https://doi.org/10.1016/S1874-6047(08)60401-1
Hoffman AS, Grande LA, Gibson P, Park JB, Daly CH, Bornstein P, Ross R (1973) Preliminary studies on mechanochemical-structure relationships in connective tissues using enzymolysis techniques. In: Perspectives in biomedical engineering, Palgrave Macmillan, London, pp 173–176. https://doi.org/10.1007/978-1-349-01604-4_28
Holzapfel GA, Ogden RW (2009) Constitutive modelling of passive myocardium: a structurally based framework for material characterization. Philos Trans R Soc A Math Phys Eng Sci 367(1902):3445–3475. https://doi.org/10.1098/rsta.2009.0091
Holzapfel GA, Gasser TC, Ogden RW (2000) A new constitutive framework for arterial wall mechanics and a comparative study of material models. J Elast Phys Sci Solids 61(1–3):1–48. https://doi.org/10.1023/A:1010835316564
Humphrey JD, Rajagopal KR (2002) A constrained mixture model for growth and remodeling of soft tissues. Math Models Methods Appl Sci 12(03):407–430. https://doi.org/10.1142/S0218202502001714
Isaacs JL, Vresilovic E, Sarkar S, Marcolongo M (2014) Role of biomolecules on annulus fibrosus micromechanics: effect of enzymatic digestion on elastic and failure properties. J Mech Behav Biomed Mater 40:75–84. https://doi.org/10.1016/j.jmbbm.2014.08.012
Johanson WG, Pierce AK (1972) Effects of elastase, collagenase, and papain on structure and function of rat lungs in vitro. J Clin Investig 51(2):288–293. https://doi.org/10.1172/JCI106813
Karlinsky JB, Snider GL, Franzblau C, Stone PJ, Hoppin FG (1976) In vitro effects of elastase and collagenase on mechanical properties of hamster lungs. Am Rev Respir Dis 113(6):769–777. https://doi.org/10.1164/arrd.1976.113.6.769
Karlinsky JB, Bowers JT, Fredette JV, Evans J (1985) Thermoelastic properties of uniaxially deformed lung strips. J Appl Psychol 58(2):459–467. https://doi.org/10.1152/jappl.1985.58.2.459
Kelley J, Chrin L, Coflesky J, Evans J (1989) Localization of collagen in the rat lung: biochemical quantitation of types I and III collagen in small airways, vessels, and parenchyma. Lung 167(1):313–322. https://doi.org/10.1007/BF02714960
Kelley C, Liao L, Qi L, Chu M, Reese J, Winton C (2008) Projected pseudotransient continuation. SIAM J Numer Anal 46(6):3071–3083. https://doi.org/10.1137/07069866X
Kielty CM, Sherratt MJ, Shuttleworth CA (2002) Elastic fibres. J Cell Sci 115(14):2817–2828
Kitoh T, Kawai Y, Ohhashi T (1993) Effects of collagenase, elastase, and hyaluronidase on mechanical properties of isolated dog jugular veins. Am J Physiol Heart Circ Physiol 265(1):H273–H280. https://doi.org/10.1152/ajpheart.1993.265.1.H273
Kochová P, Kuncová J, Ŝvíglerová J, Cimrman R, Miklíková M, Liŝka V, Tonaz Z (2012) The contribution of vascular smooth muscle, elastin and collagen on the passive mechanics of porcine carotid arteries. Physiol Meas 33(8):1335. https://doi.org/10.1088/0967-3334/33/8/1335
Lanir Y (1979) A structural theory for the homogeneous biaxial stress-strain relationships in flat collagenous tissues. J Biomech 12(6):423–436. https://doi.org/10.1016/0021-9290(79)90027-7
Levenberg K (1944) A method for the solution of certain problems in least squares. Q Appl Math 2:164–168. https://doi.org/10.1090/qam/10666
Mallya SK, Mookhtiar KA, Wart HEV (1992) Kinetics of hydrolysis of type I, II, and III collagens by the class I and II Clostridium histolyticum collagenases. J Prot Chem 11(1):99–107. https://doi.org/10.1007/BF01025096
Marquardt DW (1963) An algorithm for least-squares estimation of nonlinear parameters. SIAM J Appl Math 11(2):431–441. https://doi.org/10.1137/0111030
Martin C, Uhlig S, Ullrich V (1996) Videomicroscopy of methacholine-induced contraction of individual airways in precision-cut lung slices. ERJ Open Res 9(12):2479–2487
Mercer RR, Crapo JD (1990) Spatial distribution of collagen and elastin fibers in the lungs. J Appl Physiol 69(2):756–765. https://doi.org/10.1152/jappl.1990.69.2.756
Mercer RR, Russell ML, Crapo JD (1994) Alveolar septal structure in different species. J Appl Physiol 77(3):1060–1066. https://doi.org/10.1152/jappl.1994.77.3.1060
Moretto A, Dallaire M, Romero P, Ludwig M (1994) Effect of elastase on oscillation mechanics of lung parenchymal strips. J Appl Physiol 77(4):1623–1629. https://doi.org/10.1152/jappl.1994.77.4.1623
Otis DR, Ingenito EP, Kamm RD, Johnson M (1994) Dynamic surface tension of surfactant TA: experiments and theory. J Appl Physiol 77(6):2681–2688. https://doi.org/10.1152/jappl.1994.77.6.2681
Oxlund H, Manschot J, Viidik A (1988) The role of elastin in the mechanical properties of skin. J Biomech 21(3):213–218. https://doi.org/10.1016/0021-9290(88)90172-8
Rausch S, Haberthür D, Stampanoni M, Schittny J, Wall W (2011) Local strain distribution in real three-dimensional alveolar geometries. Ann Biomed Eng 39(11):2835–2843. https://doi.org/10.1007/s10439-011-0328-z
Ressmeyer AR, Larsson AK, Vollmer E, Dahlèn SE, Uhlig S, Martin C (2006) Characterisation of guinea pig precision-cut lung slices: comparison with human tissues. Eur Resp J 28(3):603–611. https://doi.org/10.1183/09031936.06.00004206
Roth CJ, Becher T, Frerichs I, Weiler N, Wall WA (2016) Coupling of EIT with computational lung modeling for predicting patient-specific ventilatory responses. J Appl Physiol. https://doi.org/10.1152/japplphysiol.00236.2016
Roth CJ, Yoshihara L, Ismail M, Wall WA (2017) Computational modelling of the respiratory system: discussion of coupled modelling approaches and two recent extensions. Comput Methods Appl Mech Eng 314:473–493. https://doi.org/10.1016/j.cma.2016.08.010
Sata M, Takahashi K, Sato S, Tomoike H (1995) Structural and functional characteristics of peripheral pulmonary parenchyma in golden hamsters. J Appl Physiol 78(1):239–246. https://doi.org/10.1152/jappl.1995.78.1.239
Selman M, Thannickal VJ, Pardo A, Zisman DA, Martinez FJ, Lynch Iii JP (2004) Idiopathic pulmonary fibrosis: pathogenesis and therapeutic approaches. Drugs 64(4):405–431. https://doi.org/10.2165/00003495-200464040-00005
Senior RM, Bielefeld DR, Abensohn MK (1975) The effects of proteolytic enzymes on the tensile strength of human lung. Am Rev Respir Dis 111(2):184–188. https://doi.org/10.1164/arrd.1975.111.2.184
Shen ZL, Dodge MR, Kahn H, Ballarini R, Eppell SJ (2008) Stress–strain experiments on individual collagen fibrils. Biophys J 95(8):3956–3963. https://doi.org/10.1529/biophysj.107.124602
Snider GL, Sherter CB, Koo KW, Karlinsky JB, Hayes JA, Franzblau C (1977) Respiratory mechanics in hamsters following treatment with endotracrael elastase or collagenase. J Appl Physiol 42(2):206–215. https://doi.org/10.1152/jappl.1977.42.2.206
Snider GL, Kleinerman J, Thurlbeck WM, Bengali ZH (1985) The definition of emphysema. Am Rev Respir Dis 132(1):182–185. https://doi.org/10.1164/arrd.1985.132.1.182
Sobin SS, Fung YC, Tremer HM (1988) Collagen and elastin fibers in human pulmonary alveolar walls. J Appl Psychol 64(4):1659–1675. https://doi.org/10.1152/jappl.1988.64.4.1659
Suki B (2014) Assessing the functional mechanical properties of bioengineered organs with emphasis on the lung. J Cell Physiol 229(9):1134–1140. https://doi.org/10.1002/jcp.24600
Suki B, Bates JHT (2008) Extracellular matrix mechanics in lung parenchymal diseases. Respir Physiol Neurobiol 163(1–3):33–43. https://doi.org/10.1016/j.resp.2008.03.015
Suki B, Ito S, Stamenović D, Lutchen KR, Ingenito EP (2005) Biomechanics of the lung parenchyma: critical roles of collagen and mechanical forces. J Appl Psychol 98(5):1892–1899. https://doi.org/10.1152/japplphysiol.01087.2004
Suki B, Stamenović D, Hubmayr R (2011) Lung parenchymal mechanics. Compr Physiol 1(3):1317–1351. https://doi.org/10.1002/cphy.c100033
Suki B, Sato S, Parameswaran H, Szabari MV, Takahashi A, Bartolák-Suki E (2013) Emphysema and mechanical stress-induced lung remodeling. Physiology 28(6):404–413. https://doi.org/10.1152/physiol.00041.2013
Toshima M, Ohtani Y, Ohtani O (2004) Three-dimensional architecture of elastin and collagen fiber networks in the human and rat lung. Arch Histol Cytol 67(1):31–40. https://doi.org/10.1679/aohc.67.31
Tschanz SA, Makanya AN, Haenni B, Burri PH (2003) Effects of neonatal high-dose short-term glucocorticoid treatment on the lung: a morphologic and morphometric study in the rat. Pediatr Res 53(1):72–80. https://doi.org/10.1203/00006450-200301000-00014
Ujiie Y, Shimada A, Komatsu K, Gomi K, Oida S, Arai T, Fukae M (2008) Degradation of noncollagenous components by neutrophil elastase reduces the mechanical strength of rat periodontal ligament. J Periodontal Res 43(1):22–31. https://doi.org/10.1111/j.1600-0765.2007.00990.x
Wall WA, Wiechert L, Comerford A, Rausch S (2010) Towards a comprehensive computational model for the respiratory system. Int J Numer Method Biomed Eng 26(7):807–827. https://doi.org/10.1002/cnm.1378
Weibel ER (2011) Functional morphology of lung parenchyma. In: Comprehensive physiology, Wiley. https://doi.org/10.1002/cphy.cp030308
Weisbecker H, Viertler C, Pierce DM, Holzapfel GA (2013) The role of elastin and collagen in the softening behavior of the human thoracic aortic media. J Biomech 46(11):1859–1865. https://doi.org/10.1016/j.jbiomech.2013.04.025
Wiechert L, Metzke R, Wall WA (2009) Modeling the mechanical behavior of lung tissue at the microlevel. J Eng Mech ASCE 135(5):434–438
Yi E, Sato S, Takahashi A, Parameswaran H, Blute TA, Bartolák-Suki E, Suki B (2016) Mechanical forces accelerate collagen digestion by bacterial collagenase in lung tissue strips. Front Physiol. https://doi.org/10.3389/fphys.2016.00287
Yuan H, Ingenito EP, Suki B (1997) Dynamic properties of lung parenchyma: mechanical contributions of fiber network and interstitial cells. J Appl Psychol 83(5):1420–1431. https://doi.org/10.1152/jappl.1997.83.5.1420
Yuan H, Kononov S, Cavalcante FS, Lutchen KR, Ingenito EP, Suki B (2000) Effects of collagenase and elastase on the mechanical properties of lung tissue strips. J Appl Psychol 89(1):3–14. https://doi.org/10.1152/jappl.2000.89.1.3
Zulliger MA, Fridez P, Hayashi K, Stergiopulos N (2004) A strain energy function for arteries accounting for wall composition and structure. J Biomech 37(7):989–1000. https://doi.org/10.1016/j.jbiomech.2003.11.026
Acknowledgements
We gratefully acknowledge the technical assistance of Hanna Czajkowska, Igor Heinze, and Sebastian Maltan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Birzle, A.M., Hobrack, S.M.K., Martin, C. et al. Constituent-specific material behavior of soft biological tissue: experimental quantification and numerical identification for lung parenchyma. Biomech Model Mechanobiol 18, 1383–1400 (2019). https://doi.org/10.1007/s10237-019-01151-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10237-019-01151-3