Abstract
Objectives
To evaluate the health economics evidence based on randomized controlled trials of pharmacist-led medication review in pharmacotherapy managed cardiovascular disease risk factors, specifically, hypertension, type-2 diabetes mellitus and dyslipidaemia in ambulatory settings and to provide recommendations for future evaluations.
Methods
A systematic review was carried out according to the Cochrane Handbook for Systematic Reviews. PubMed (Medline), Scopus, Web of Science, National Health System Economic Evaluation Database (NHS EED), Cochrane Library, and Econlit were searched and screened by two independent authors. Incremental cost-effectiveness ratio was the main outcome. Risk of bias was assessed with the Effective Practice and Organisation of Care tool by the Cochrane Collaboration. Economic evaluation quality was assessed with the he Consensus Health Economic Criteria list (CHEC list).
Results
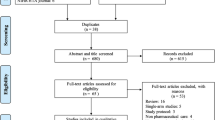
5636 records were found, and 174 were retrieved for full-text review yielding 11 articles. Eight articles deemed the intervention as cost effective and two as dominant. Two cost–utility analyses were performed yielding ICERs of $612.7 and $59.8 per QALY. Four articles were considered to perform a high-quality economic evaluation and four had a low risk of bias. Future economic evaluations should consider cost–utility analysis, to describe usual care thoroughly, and use time horizons that capture the effect of cardiovascular disease prevention, a societal perspective and uncertainty analysis.
Conclusion
Pharmacist-led medication review has proven to be cost effective in various studies in different settings. Policy decision makers are advised to undertake local economic evaluations reflecting the gaps observed in this systematic review and published literature. If this is not possible, a transferability assessment should be conducted.


Similar content being viewed by others
References
Mendis, S., Puska, P., Norving, B.: Global atlas on cardiovascular disease prevention and control. World Heal, Organ (2011)
Benjamin, E.J., Blaha, M.J., Chiuve, S.E., Cushman, M., Das, S.R., Deo, R., De Ferranti, S.D., Floyd, J., Fornage, M., Gillespie, C., Isasi, C.R., Jimnez, M.C., Jordan, L.C., Judd, S.E., Lackland, D., Lichtman, J.H., Lisabeth, L., Liu, S., Longenecker, C.T., MacKey, R.H., Matsushita, K., Mozaffarian, D., Mussolino, M.E., Nasir, K., Neumar, R.W., Palaniappan, L., Pandey, D.K., Thiagarajan, R.R., Reeves, M.J., Ritchey, M., Rodriguez, C.J., Roth, G.A., Rosamond, W.D., Sasson, C., Towfghi, A., Tsao, C.W., Turner, M.B., Virani, S.S., Voeks, J.H., Willey, J.Z., Wilkins, J.T., Wu, J.H.Y., Alger, H.M., Wong, S.S., Muntner, P.: Heart Disease and Stroke Statistics’ 2017 update: a report from the American Heart Association. Circulation 135, e146–e603 (2017). https://doi.org/10.1161/cir.0000000000000485
Wilkins, E., Wilson, L., Wickramasinghe, K., Bhatnagar, P., Leal, J., Luengo-Fernandez, R., Burns, R., Rayner, M., Townsend, N.: European Cardiovascular Disease Statistics 2017. Eur. Hear, Network (2017)
Piepoli, M.F., Hoes, A.W., Agewall, S., Albus, C., Brotons, C., Catapano, A.L., Cooney, M.T., Corrà, U., Cosyns, B., Deaton, C., Graham, I., Hall, M.S., Hobbs, F.D.R., Løchen, M.L., Löllgen, H., Marques-Vidal, P., Perk, J., Prescott, E., Redon, J., Richter, D.J., Sattar, N., Smulders, Y., Tiberi, M., Van Der Worp, H.B., Van Dis, I., Verschuren, W.M.M., Binno, S., De Backer, G., Roffi, M., Aboyans, V., Bachl, N., Carerj, S., Cho, L., Cox, J., De Sutter, J., Egidi, G., Fisher, M., Fitzsimons, D., Franco, O.H., Guenoun, M., Jennings, C., Jug, B., Kirchhof, P., Kotseva, K., Lip, G.Y.H., Mach, F., Mancia, G., Bermudo, F.M., Mezzani, A., Niessner, A., Ponikowski, P., Rauch, B., Stauder, A., Turc, G., Wiklund, O., Windecker, S., Zamorano, J.L., Achenbach, S., Badimon, L., Barón-Esquivias, G., Baumgartner, H., Bax, J.J., Dean, V., Erol, Ç., Gaemperli, O., Kolh, P., Lancellotti, P., Nihoyannopoulos, P., Torbicki, A., Carneiro, A.V., Metzler, B., Najafov, R., Stelmashok, V., De Maeyer, C., Dilić, M., Gruev, I., Miličić, D., Vaverkova, H., Gustafsson, I., Attia, I., Duishvili, D., Ferrières, J., Kostova, N., Klimiashvili, Z., Hambrecht, R., Tsioufis, K., Szabados, E., Andersen, K., Vaughan, C., Zafrir, B., Novo, S., Davletov, K., Jashari, F., Kerimkulova, A., Mintale, I., Saade, G., Petrulioniene, Z., Delagardelle, C., Magri, C.J., Rudi, V., Oukerraj, L., Çölkesen, B.E., Schirmer, H., Dos Reis, R.P., Gherasim, D., Nedogoda, S., Zavatta, M., Giga, V., Filipova, S., Padial, L.R., Kiessling, A., Mahdhaoui, A., Ural, D., Nesukay, E., Gale, C.: 2016 European Guidelines on cardiovascular disease prevention in clinical practice. Eur. Heart J. 37, 2315–2381 (2016). https://doi.org/10.1093/eurheartj/ehw106
Whelton, P., Carey, R., Aronow, W., Casey, D.J., Collins, K., Dennison Himmelfarb, C., DePalma, S., Gidding, S., Jamerson, K., Jones, D., MacLaughlin, E., Muntner, P., Ovbiagele, B., Smith, S.J., Spencer, C., Stafford, R., Taler, S., Thomas, R., Williams, K.S., Williamson, J., Wright, J.J.: 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Pr. Hypertension 71, e13–e115 (2017). https://doi.org/10.1161/HYP.0000000000000065/-/DC1.The
American Diabetes Association: Summary of Revisions: standards of Medical Care in Diabetes—2019. Diabetes Care 42, S4–S6 (2019). https://doi.org/10.2337/dc19-Srev01
Yancy, C.W., Jessup, M., Bozkurt, B., Butler, J., Casey, D.E., Colvin, M.M., Drazner, M.H., Filippatos, G.S., Fonarow, G.C., Givertz, M.M., Hollenberg, S.M., Lindenfeld, J.A., Masoudi, F.A., McBride, P.E., Peterson, P.N., Stevenson, L.W., Westlake, C.: 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of Amer. Circulation 136, e137–e161 (2017). https://doi.org/10.1161/CIR.0000000000000509
Pharmaceutical Care Network Europe Foundation: The PCNE Classification V 8.02. http://www.pcne.org/upload/files/152_PCNE_classification_V7-0.pdf. Accessed 9 May 2019
Westerlund, T., Marklund, B.: Assessment of the clinical and economic outcomes of pharmacy interventions in drug-related problems. J. Clin. Pharm. Ther. 34, 319–327 (2009). https://doi.org/10.1111/j.1365-2710.2008.01017.x
National Coordinating Council for Medication Error Reporting and Prevention. What is a medication error? New York, NY: National Coordinating Council for Medication Error Reporting and Prevention; 2015. https://www.nccmerp.org/about-medication-errors. Accessed 9 May 2019
Walsh, E.K., Hansen, C.R., Sahm, L.J., Kearney, P.M., Doherty, E., Bradley, C.P.: Economic impact of medication error: a systematic review. Pharmacoepidemiol. Drug Saf. 26, 481–497 (2017). https://doi.org/10.1002/pds.4188
Pharmaceutical Care Network Europe: Position Paper on the PCNE definition of Medication Review 2016. https://www.pcne.org/upload/files/149_Position_Paper_on_PCNE_Medication_Review_final.pdf. Accessed 9 May 2019
Pharmaceutical Care Network Europe Foundation: PCNE statement on medication review 2013. https://www.pcne.org/upload/files/150_20160504_PCNE_MedRevtypes.pdf. Accessed 9 May 2019
Jokanovic, N., Tan, E.C., Sudhakaran, S., Kirkpatrick, C.M., Dooley, M.J., Ryan-Atwood, T.E., Bell, J.S.: Pharmacist-led medication review in community settings: an overview of systematic reviews. Res. Soc. Adm. Pharm. 13, 661–685 (2017). https://doi.org/10.1016/j.sapharm.2016.08.005
Tan, E.C.K., Stewart, K., Elliott, R.A., George, J.: Pharmacist services provided in general practice clinics: a systematic review and meta-analysis. Res. Soc. Adm. Pharm. 10, 608–622 (2014). https://doi.org/10.1016/j.sapharm.2013.08.006
Altowaijri, A., Phillips, C.J., Fitzsimmons, D.: A systematic review of the clinical and economic effectiveness of clinical pharmacist intervention in secondary prevention of cardiovascular disease. J Manag Care Pharm 19, 408–416 (2013). https://doi.org/10.18553/jmcp.2013.19.5.408
Wang, Y., Yeo, Q.Q., Ko, Y.: Economic evaluations of pharmacist-managed services in people with diabetes mellitus: a systematic review. Diabet. Med. 33, 421–427 (2016). https://doi.org/10.1111/dme.12976
Jacob, V., Chattopadhyay, S.K., Thota, A.B., Proia, K.K., Njie, G., Hopkins, D.P., Finnie, R.K.C., Pronk, N.P., Kottke, T.E.: Economics of team-based care in controlling blood pressure: a community guide systematic review. Am. J. Prev. Med. 49, 772–783 (2015). https://doi.org/10.1016/j.amepre.2015.04.003
Bodrogi, J., Kaló, Z.: Principles of pharmacoeconomics and their impact on strategic imperatives of pharmaceutical research. Br. J. Pharmacol. 159, 1367–1373 (2010). https://doi.org/10.1111/j.1476-5381.2009.00550.x
Higgins, J., Green, S.: Cochrane handbook for systematic reviews of interventions version 5.1. 0 [updated March 2011]. Cochrane Collab. (2011). https://www.handbook.cochrane.org. Accessed 9 May 2019
Moher, D., Liberati, A., Tetzlaff, J., Altman, D.G.: Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 6, 1–6 (2009). https://doi.org/10.1371/journal.pmed.1000097
Drummond, M., Sculpher, M., Claxton, K., Stoddart, G.L., Torrance, G.: Methods for the economic evaluation of health care programmes. Oxford University Press, Oxford (2015)
Cochrane effective practice and organisation of care (EPOC): Suggested risk of bias criteria for EPOC reviews. https://epoc.cochrane.org/resources/epoc-resources-review-authors. Accessed 9 May 2019
Malet-Larrea, A., García-Cárdenas, V., Sáez-Benito, L., Benrimoj, S.I., Calvo, B., Goyenechea, E.: Cost-effectiveness of professional pharmacy services in community pharmacy: a systematic review. Expert Rev. Pharmacoecon. Outcomes Res. 16, 747–758 (2016). https://doi.org/10.1080/14737167.2016.1259071
Evers, S., Goossens, M., de Vet, H., van Tulder, M., Ament, A.: Criteria list for assessment of methodological quality of economic evaluations: consensus on Health Economic Criteria. Int. J. Technol. Assess. Health Care 21, 240–245 (2005). https://doi.org/10.1017/S0266462305050324
Philips, Z., Bojke, L., Sculpher, M., Claxton, K., Golder, S.: Good practice guidelines for decision-analytic modelling in health technology assessment. Pharmacoeconomics. 24, 355–371 (2006). https://doi.org/10.2165/00019053-200624040-00006
Shemilt, I., Thomas, J., Morciano, M.: A web-based tool for adjusting costs to a specific target currency and price year. Evid. Policy. 6, 51–59 (2010). https://doi.org/10.1332/174426410X482999
Nixon, J., Khan, K.S., Kleijnen, J.: Summarising economic evaluations in systematic reviews: a new approach. BMJ 322, 1596–1598 (2001). https://doi.org/10.1136/bmj.322.7302.1596
Okamoto, M.P., Nakahiro, R.K.: Pharmacoeconomic evaluation of a pharmacist-managed hypertension clinic. Pharmacotherapy. 21, 1337–1344 (2001). https://doi.org/10.1016/j.jval.2011.02.542
Polgreen, L.A., Han, J., Carter, B.L., Ardery, G.P., Coffey, C.S., Chrischilles, E.A., James, P.A.: Cost-effectiveness of a physician-pharmacist collaboration intervention to improve blood pressure control. Hypertension 66, 1145–1151 (2015). https://doi.org/10.1161/HYPERTENSIONAHA.115.06023
Borenstein, J.E., Graber, G., Saltiel, E., Wallace, J., Ryu, S., Jackson, A., Deutsch, S., Weingarten, S.R.: Physician-pharmacist comanagement of hypertension: a randomized, comparative trial. Pharmacotherapy. 23, 209–216 (2003). https://doi.org/10.1592/phco.23.2.209.32096
Shireman, T.I., Svarstad, B.L.: Cost-effectiveness of Wisconsin TEAM model for improving adherence and hypertension control in black patients. J. Am. Pharm. Assoc. 56, 389–396 (2016). https://doi.org/10.1016/j.japh.2016.03.002
Fishman, P.A., Cook, A.J., Anderson, M.L., Ralston, J.D., Catz, S.L., Carrell, D., Carlson, J., Green, B.B.: Improving BP control through electronic communications: an economic evaluation. Am. J. Manag. Care. 19, 709–716 (2013)
Obreli-Neto, P.R., Marusic, S., Guidoni, C.M., Baldoni, A.D., Renovato, R.D., Pilger, D., Cuman, R.K.N., Pereira, L.R.L.: Economic evaluation of a pharmaceutical care program for elderly diabetic and hypertensive patients in primary health care: a 36-month randomized controlled clinical trial. J Manag Care Spec Pharm 21, 66–75 (2015). https://doi.org/10.18553/jmcp.2015.21.1.66
Simpson, S.H., Lier, D.A., Majumdar, S.R., Tsuyuki, R.T., Lewanczuk, R.Z., Spooner, R., Johnson, J.A.: Cost-effectiveness analysis of adding pharmacists to primary care teams to reduce cardiovascular risk in patients with Type 2 diabetes: results from a randomized controlled trial. Diabet. Med. 32, 899–906 (2015). https://doi.org/10.1111/dme.12692
Chan, C.-W., Siu, S.-C., Wong, C.K.W., Lee, V.W.Y.: A Pharmacist Care Program: positive impact on cardiac risk in patients with type 2 diabetes. J. Cardiovasc. Pharmacol. Ther. 17, 57–64 (2012). https://doi.org/10.1177/1074248410396216
Adibe, M.O., Aguwa, C.N., Ukwe, C.V.: Cost-utility analysis of pharmaceutical care intervention versus usual care in management of nigerian patients with type 2 diabetes. Value Heal. Reg. Issues. 2, 189–198 (2013). https://doi.org/10.1016/j.vhri.2013.06.009
Chen, J.-H., Huang-Tz, O., Tzu-Chieh, L., Chia-Cheng Lai, E., Yang Kao, Y.-H.: Pharmaceutical care of elderly patients with poorly controlled type 2 diabetes mellitus: a randomized controlled trial. Int. J. Clin. Pharm. 38, 88–95 (2016). https://doi.org/10.1007/s11096-015-0210-4
The Community Pharmacy Medicines Management Project Evaluation Team: The MEDMAN study: a randomized controlled trial of community pharmacy-led medicines management for patients with coronary heart disease. Fam. Pract. 24, 189–200 (2007). https://doi.org/10.1093/fampra/cml075
Carter, B.L., Coffey, C.S., Ardery, G., Uribe, L., Ecklund, D., James, P., Egan, B., Vander Weg, M., Chrischilles, E., Vaughn, T.: Cluster-randomized trial of a physician/pharmacist collaborative model to improve blood pressure control. Circ Cardiovasc Qual Outcomes 8, 235–243 (2015). https://doi.org/10.1161/circoutcomes.114.001283
Simpson, S.H., Majumdar, S.R., Tsuyuki, R.T., Lewanczuk, R.Z., Spooner, R., Johnson, J.A.: Effect of adding pharmacists to primary care teams on blood pressure control in patients with type 2 diabetes A randomized controlled trial. Diabetes Care 34, 20–26 (2011)
Green, B.B., Cook, A., Ralston, J., Fishman, P., Catz, S., Carlson, J., Carrell, D., Tyll, L., Larson, E., Thompson, R.: Effectiveness of home blood pressure monitoring, web communication, and pharmacist care on hypertension control. J. Am. Med. Assoc. 299, 2857–2867 (2008). https://doi.org/10.1001/jama.299.24.2857
Svarstad, B.L., Kotchen, J.M., Shireman, T.I., Crawford, S.Y., Palmer, P.A., Vivian, E.M., Brown, R.L.: The team education and adherence monitoring (TEAM) trial: pharmacy interventions to improve hypertension control in blacks. Circ. Cardiovasc. Qual. Outcomes. 2, 264–271 (2009). https://doi.org/10.1161/CIRCOUTCOMES.109.849992
Neumann, P.J., Cohen, J.T., Weinstein, M.C.: Updating cost-effectiveness—the curious resilience of the $50,000-per-QALY threshold. N. Engl. J. Med. 371, 796–797 (2014). https://doi.org/10.1056/NEJMp1405158
Woods, B., Revill, P., Sculpher, M., Claxton, K.: Country-level cost-effectiveness thresholds: initial estimates and the need for further research. Value Heal. 19, 929–935 (2016). https://doi.org/10.1016/j.jval.2016.02.017
Huiskes, V.J.B., Burger, D.M., Van Den Ende, C.H.M., Van Den Bemt, B.J.F.: Effectiveness of medication review: a systematic review and meta-analysis of randomized controlled trials. BMC Fam. Pract. 18, 1–15 (2017). https://doi.org/10.1186/s12875-016-0577-x
James, P.A., Oparil, S., Carter, B.L., Cushman, W.C., Dennison-Himmelfarb, C., Handler, J., Lackland, D.T., LeFevre, M.L., MacKenzie, T.D., Ogedegbe, O., Smith, S.C., Svetkey, L.P., Taler, S.J., Townsend, R.R., Wright, J.T., Narva, A.S., Ortiz, E.: 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). J Am Med Assoc 311, 507–520 (2014). https://doi.org/10.1001/jama.2013.284427
Kulchaitanaroaj, P., Brooks, J.M., Chaiyakunapruk, N., Goedken, A.M., Chrischilles, E.A., Carter, B.L.: Cost-utility analysis of physician–pharmacist collaborative intervention for treating hypertension compared with usual care. J. Hypertens. 35, 178–187 (2017). https://doi.org/10.1097/HJH.0000000000001126
Drummond, M., Barbieri, M., Cook, J., Glick, H.A., Lis, J., Malik, F., Reed, S.D., Rutten, F., Sculpher, M., Severens, J.: Transferability of economic evaluations across jurisdictions: ISPOR good research practices task force report. Value Heal. 12, 409–418 (2009). https://doi.org/10.1111/j.1524-4733.2008.00489.x
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they do not have any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ahumada-Canale, A., Quirland, C., Martinez-Mardones, F.J. et al. Economic evaluations of pharmacist-led medication review in outpatients with hypertension, type 2 diabetes mellitus, and dyslipidaemia: a systematic review. Eur J Health Econ 20, 1103–1116 (2019). https://doi.org/10.1007/s10198-019-01080-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10198-019-01080-z
Keywords
- Medication review
- Pharmacist
- Economic evaluation
- Cardiovascular disease
- Hypertension
- Type 2 diabetes mellitus