Abstract
Background
Vulnerable populations, such as hemodialysis (HD) patients and kidney transplant (RTx) recipients, have priority for anti-COVID-19 vaccination, because of their impaired immune status. Here, we investigated the immune response after vaccination with BNT162b2 (two doses plus booster) in HD and RTx patients.
Methods
A prospective, observational study was started in two homogeneous groups of 55 HD and 51 RTx patients previously matched from a cohort of 336 patients. Anti-RBD IgG levels, assayed after the second dose with BNT162b2 mRNA, were used to stratify subjects into quintiles. After the second dose and after booster, anti-RBD and IGRA test were evaluated in RTx and HD, belonging to the first and fifth quintiles.
Results
After the second dose of vaccine, the median circulating levels of anti-RBD IgG were significantly higher in HD (1456 AU/mL) compared to RTx (27.30 AU/mL). IGRA test showed significantly higher values in the HD (382 mIU/mL) compared with the RTx (73 mIU/mL). After the booster, humoral response increased significantly in both HD (p = 0.0002) and RTx groups (p = 0.009), whereas the T-cellular immunity remained essentially stable in most patients. In RTx patients with a low humoral response after the second dose, the third dose did not significantly strengthen either humoral or cellular immunity.
Conclusions
For HD and RTx, there is great variability in the humoral response to anti-COVID-19 vaccination, with a stronger response in the HD group. The booster dose was ineffective at reinforcing the humoral and cellular immune response in most RTx patients hyporesponsive to the second dose.
Similar content being viewed by others
Introduction
The disease caused by SARS-CoV-2 infection (COVID-19) has a strong impact on vulnerable populations, such as hemodialysis (HD) and kidney transplant (RTx) patients.
Uremia interferes with innate and adaptive immunity, leading to insufficient neutrophil and monocyte function, decreased antigen processing, reduced cell- and antibody-mediated responsiveness to vaccinations. Anti-rejection regimens further suppress immunity. Other risk factors are elderly, dialysis vintage, malnutrition, inflammation and comorbidities, including hypertension, diabetes, obesity, and cardiovascular disease [1, 2].
The impaired immune status of HD and RTx patients has been described as a major risk factor for COVID-19 and for complicated disease course, with higher mortality rates than in general population [3]. Therefore, vaccination is a priority for these patients, although SARS-CoV-2 vaccines have only been clinically tested in general population, whose protection rates reach up to 95% after two administrations. At present, there is scarce and incomplete knowledge about the immune response and protection from SARS-CoV-2 in HD and RTx patients after standard doses of mRNA vaccines [4, 5].
This study is aimed at evaluating and comparing the efficacy of COVID-19 vaccination in two populations of HD and RTx patients from two Nephrology Units, by measuring the levels of antibodies and the T cells response after administration of a mRNA vaccine (two doses plus booster).
Materials and methods
A cohort of 336 patients, 185 on HD and 151 RTx, from the Nephrology Units of Taranto and Martina Franca (Southern Italy), was recruited from April 2021 to May 2021. HD cases included adults (> 18 years) with end-stage renal disease (ESRD), treated with thrice-weekly hemodialysis for at least 3 months. RTx cases included adult patients with a kidney transplant from a deceased donor for more than 2 years. We excluded patients transplanted since less than 2 years because of exposure to high-dose immunosuppressive regimens and patients, both HD and RTx, who had a previous SARS-CoV-2 infection documented by PCR testing on nasopharyngeal swab. During the recruitment period, enrolled patients received two doses, 28 days apart, of the mRNA vaccine BNT162b2 (BioNTech Manufacturing GmbH, Germany/Pfizer Manufacturing Belgium NV, Belgium).
Two members of our team independently matched HD and RTx patients for gender, age, dialysis vintage, BMI, comorbidities and obtained two homogeneous groups of 55 HD and 51 RTx patients, whose main demographic and clinical characteristics are shown in Table 1.
A prospective, observational study was started in the 106 patients, after approval by the local Ethical Committee and written informed consent of participants.
Blood samples were collected 7 weeks after the second vaccination dose. IgG antibodies against the receptor binding domain region of SARS-CoV-2 Spike glycoprotein (anti-RBD) were assayed and, based on the antibodies levels, subjects were divided into quintiles. Three months after the second vaccination dose, the cellular immune response was evaluated by an interferon-γ (IFN-γ) releasing assay (IGRA test) in patients belonging to the lowest (Q1) and highest (Q5) anti-RBD quintiles.
A booster dose of BNT162b2 was administered 5 months after the second. Anti-RBD and IGRA test were performed again 3 months after the booster dose in the same selected patients.
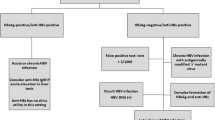
Figure 1 shows a flow chart that supports understanding of the steps which led from the initial cohort of HD and RTx patients to the cases included in the final statistical data analysis.
Anti-RBD were detected by a chemiluminescent microparticle immunoassay, using SARS-CoV-2 IgG II Quant (Abbott Laboratories, Ireland) on Architect i4000SR analyzer and measured as antibody units (AU) per milliliter. The conversion factor in binding AU (BAU) following the WHO International Standard (NIBCS 20/136) is 0.142.
The IGRA test for the evaluation of T cell response consisted in an IFN-γ releasing assay using a stimulation kit (Quan-T-Cell SARS-CoV-2, Euroimmun, Germany) and an enzyme-linked immunosorbent assay for the quantification of the IFN-γ released (Quan-T-Cell ELISA, Euroimmun, Germany). IFN-γ concentrations were expressed as milli-international units per milliliter (mIU/mL).
For the statistical analysis, the normality of quantitative variables was checked with the Shapiro–Wilk test. Continuous variables were reported as mean ± standard deviation when normally distributed, or as median plus 25th and 75th percentiles when non-normally distributed. Categorical variables were presented as relative frequencies and compared by the Pearson/Fisher two-tailed Chi-square test. The Mann–Whitney U or Wilcoxon matched-pairs signed-rank test was used in the bivariate analysis to compare quantitative non-normally distributed variables between unpaired and paired groups. The Spearman’s rho correlation coefficient was used to evaluate relationships between skewed continuous variables. Statistical significance was accepted at two-sided p < 0.05. All statistical analyses were performed using R (version 3.6.3; The R Foundation for Statistical Computing, Vienna, Austria) in a bundle with the R Commander Plug-in for the EZR (Easy R) Package (version 1.36).
Results
Table 1 shows the demographic and clinical characteristics of the two matched groups (55 HD and 51 RTx patients). The higher numbers of diabetics in the HD group and of patients without comorbidities in the RTx group were not statistically significant.
The anti-RBD levels measured 7 weeks after two doses of vaccine demonstrated non-normally distributed antibody levels, with a wide range of variability in both groups, but much more pronounced in the RTx group, where values were concentrated mainly on the lowest range (Fig. 2 panel A). Furthermore, the median circulating levels of anti-RBD was significantly higher (p < 0.001) in HD patients (1456 AU/mL, IQR 555–3947) compared to RTx patients (27.30 AU/mL, IQR 4–247) (Fig. 2 panel B).
Anti-RBD serum levels by patient status (HD, N = 55; RTx, N = 51) at 7 weeks after completion of the anti-COVID vaccination cycle with two doses of mRNA vaccine. Panel A: density plot for the representation of data distribution. Panel B: Box and Whisker plot. Each Box and Whisker expresses the median, IQR, minimum and maximum values, while dots identify outliers
All but two RTx patients assumed calcineurin inhibitors and there was no statistically significant anti-RBD difference (p = 0.47) between patients taking cyclosporine or tacrolimus. In addition, the 80 percent of RTx patients taking azathioprine or mycophenolate did not have significantly different anti-RBD levels compared to the remaining 20 percent (p = 0.48). The limited number of RTx patients on sirolimus, everolimus and steroid-free immunosuppression did not allow us to reveal any differences in anti-RBD levels.
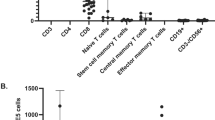
The IGRA test performed 3 months after the second dose of vaccine in 20 HD and 19 RTx patients, belonging to Q1 and Q5 quintiles of anti-RBD after the second shot, showed significantly higher values in the HD than in RTx patients (382 mIU/mL, IQR 84–1657, vs 73, IQR 28–181, p = 0.022).
Anti-RBD and IGRA test were repeated 3 months after the third dose of BNT162b2 on the same patients previously evaluated for the IGRA test, but we excluded one HD and one RTx patients for their refusal of the third dose, and another one who received a renal transplant days before the booster dose. Figure 3 shows the significant correlation between anti-RBD levels and IGRA test values in 18 HD patients (p = 0.02) and 18 RTx patients (p = 0.001) 3 months after the third dose.
Relationship between anti-RBD and IGRA test in HD and RTx patients at 3 months after the third dose of mRNA vaccine. Patients (total N = 36) were selected as belonging to the lowest (Q1) and highest (Q5) quintiles for anti-RBD 7 weeks after the second dose. The correlation coefficient is shown as Spearman’s rho coefficient
Figure 4 displays that, after the second and third vaccine doses in the same patients, anti-RBD levels (panels 4A and 4B) increased significantly in the HD and RTx groups,(p = 0.0002 and 0.009, respectively), whereas the IGRA test values (panels 4C and 4D) remained stable in most patients (in HD and RTx groups, p = 0.09 and 0.17, respectively).
Parallel coordinate plot for humoral and cellular immune response after the second and third homologous doses of anti-SARS-CoV-2 mRNA vaccine in 36 patients (18 HD and 18 RTx) who belonged to the lowest (Q1) and highest (Q5) quintiles of anti-RBD antibodies after the second dose. Timing for evaluation after the second dose was 7 weeks for anti-RBD and 3 months for IGRA testing. Timing for evaluation after the third dose was 3 months for both anti-RBD and IGRA testing. Each Box and Whisker expresses the median, IQR, minimum and maximum values
In the patients (Fig. 5) with lower anti-RDB levels after the second vaccine dose (Q1), the third dose determined an increase of antibodies levels in HD patients (panel 5A) (p = 0.004), but not in RTx patients (panel 5B). The IGRA test values not increased in both groups (panels 5C and 5D).
Parallel coordinate plot for anti-RBD levels and IGRA test after the second and third homologous doses of anti-SARS-CoV-2 mRNA vaccine in 20 patients (11 HD and 9 RTx) who had a low immune response after the second dose (anti-RBD in the lowest Q1 quintile). Timing for evaluation after the second dose was 7 weeks for anti-RBD and 3 months for IGRA testing. Timing for evaluation after the third dose was 3 months for both anti-RBD and IGRA testing. Each Box and Whisker expresses the median, IQR, minimum and maximum values
Two RTx patients acquired COVID-19 in a pauci-symptomatic form between the first and second doses of vaccine and other five patients, 4 HD and 1 RTx, after the third dose, during the massive epidemic surge occurred in Italy between December 2021 and February 2022, mainly attributed to the omicron variant. Four of the five patients experienced no or mild symptoms, while one 75-year-old HD woman with multiple comorbidities experienced a severe course and died.
Discussion
In this study, we describe the humoral and cellular responses after the second and third dose of BNT162b2 in HD patients and long-term RTx, without previous COVID-19.
Uremic toxins, inflammation, anemia, vitamin D and erythropoietin deficiencies, comorbidities, elderly, hypoalbuminemia, high BMI, and impaired immunity (or immunosuppressive drugs) influence T cells activity, antigen presenting ability, and B cells production of neutralizing antibodies [6, 7].
ESRD patients should be prioritized for vaccination, because the risk of severe SARS-CoV-2 infection is increased by several factors, such as comorbidities, immunodeficiency, older age, residence in nursing homes, travels to the dialysis facility, contacts with staff and other patients within the dialysis facility and, for transplanted patients, immunosuppression.
In ESRD, a poor response was reported to hepatitis, influenza and pneumococcal vaccines, whereas improvement of dialysis efficiency determined better responses [8,9,10]. A diminished response has been reported in ESRD also after SARS-CoV-2 vaccination. In several studies, up to 97.7% HD patients developed a response (humoral, cellular or both) after 2 vaccine doses, but often HD patients presented lower antibodies levels and/or a slower rate of seroconversion compared to controls and general population [11,12,13,14,15,16,17,18,19,20]. In RTx patients, a suboptimal response after two doses of vaccine has been observed, with seroconversion rates between 2.6 and 66% [19,20,21,22]. Seroconversion failures were mainly attributed to immunosuppressive therapy, with belatacept, mycophenolate and calcineurin inhibitors associated to higher failure rates than mTOR-inhibitors and glucocorticoids [22,23,24].
Cellular immunity may offset the absence of post-vaccination antibodies, and patients without detectable anti-RBD still can have a robust T cell response. Considering that it might be unsuitable to label patients as “non-responders” in the absence of T cells data [11, 25], an assessment of the cellular response should be added to the antibody determinations.
We measured the humoral and cellular responses to the second and third doses of anti-SARS-CoV-2 vaccine in HD and RTx patients not previously affected by COVID-19. RTx patients had not previously experienced cellular or humoral rejection nor they had received rituximab therapy. It is noteworthy that we always used the same mRNA vaccine (BNT162b2) and that the two groups were well matched for demographic and clinical characteristics, with the obvious exception of immunosuppressive therapy. Patients in the early transplant period were excluded because of the higher immunosuppression therapy usually administered at this time.
There were no statistically significant differences in anti-RBD levels in 106 patients (55 HD and 51 RTx) 7 weeks after the second dose based on the presence of comorbidities such as diabetes, overweight or obesity status, hypertension, or a cancer history (data not shown).
We found relevant differences between HD and RTx patients. HD patients showed a significantly stronger humoral response to vaccine. The effect of immunosuppressive therapy in RTx patients is the most likely explanation for this difference. Unlike other studies, the type of immunosuppressant determined no difference in RTx patients’ response, probably because of the low number of cases.
In both groups of patients, antibodies levels had a wide variability, more pronounced in RTx patients, with a much bigger density in the lower range of values. Previous data report that, even among responders, a large number of ESRD patients show low-intermediate antibodies levels after two doses, although no threshold is clearly established for protective immunity. Consequently, it is not excluded that low responders might actually remain unprotected against severe SARS-COV-2 infection [23]. For this reason, many countries have adopted the policy of three SARS-CoV-2 vaccinations to improve immune responses in patients with possible incomplete protection after two doses or to enhance waning immunity [26].
In our HD and RTx patients, the third vaccination significantly boosted anti-RBD levels, although less pronounced in RTx. However, the increase of cellular response was not significant in both groups, although anti-RBD and IGRA test values were significantly correlated. Anyway, the cellular immunologic response to the third dose appears uneven for both groups, with higher median values in HD patients. For many patients in this group, we can hypothesize maintenance of a state of cellular immunity already stimulated by the primary vaccine cycle and confirmed by the third dose. Of note, most of the low responders to two vaccine doses, i.e., patients belonging to anti-RBD Q1, improved their immunological status very poorly after a booster dose with increased anti-RBD levels only in HD patients. In any case, even for anti-RBD, patients who did not respond well to the second dose of vaccine maintained mainly low antibody levels even after the third dose.
However, according to our findings, the immunological booster of the third dose was detected more effectively by anti-RBD than by the IGRA test, and it was observed more frequently in HD than in RTx patients. This undoubtedly made the IGRA test more difficult to interpret, possibly due to its own underlying methodological aspects.
Our data are in accordance with recent reports, demonstrating that non-responders after two vaccine doses responded to a third dose only in 35–55% of HD and in 30–50% of RTx patients [27,28,29,30,31]. In another report, the chance of non-response for RTx patients was, on average, four times higher than for HD patients [22]. Other works show conflicting results, with good immune responses in HD and RTx patients who failed the primary vaccination [13, 22, 32], and even a sixfold increase in the number of RTx patients developing a protective antibodies levels after the booster dose [33].
There are some limitations in our study. First, the statistical analyses were limited by the small-sized groups. Moreover, we tested twenty healthy immunocompetent subjects for anti-RBD and IGRA test, but only after the second vaccine dose. Three months after the booster, the circulating anti-RBD median value in this group was 3570 AU/mL (IQR 1157–8716), while the IGRA test median value was 757 mIU/mL (IQR 447–1535).
Second, for the limited observation time, our data reflect only the early vaccination response, and the persistence of vaccine-induced immunity has not been assessed.
Third, we did not determine neutralizing antibodies’ levels. However, there is increasing evidence that anti-RBD correlate with neutralizing capacity and with recruitment of innate immunity and T cell-specific SARS-CoV-2 responses [31, 34, 35]. Until neutralizing antibody levels are not broadly established in routine diagnostic laboratories, the determination of anti-RBD should be used to guide clinical decision.
Finally, the clinical efficacy of a third vaccine dose was not fully assessed in our study. Out of our 106 patients, 2 were diagnosed COVID-19 after two doses and 6 after three doses. However, the cases after the third dose were observed during a massive epidemic of COVID-19 attributed to the omicron variant.
In conclusion, there is a great variability in antibody response to SARS-COV-2 vaccination in HD and RTx patients, with stronger responses in the former group. A third dose of BNT162b2 substantially increased the antibody response, which showed a good correlation with the cellular response. However, there was little evidence of an improved in immune response after the third dose in patients with initial low antibodies levels. Therefore, a large proportion of ESRD patients remained at risk for COVID-19. Barrier measures should be maintained and vaccination of the patients’ relatives and health care workers should be encouraged. A special attention is needed for diabetic, older or immunosuppressed patients. Alternative policies of vaccination and SARS-COV-2 infection management should be found for weak vaccine responders.
References
Vaziri ND, Pahl MV, Crum A, Norris K. Effect of uremia on structure and function of immune system. J Ren Nutr. 2012;22:149–56. https://doi.org/10.1053/j.jrn.2011.10.020.
Kato S, Chmielewski M, Honda H, et al. Aspects of immune dysfunction in end-stage renal disease. Clin J Am Soc Nephrol. 2008;3:1526–33. https://doi.org/10.2215/CJN.00950208.
Shrotri M, van Schalkwyk MCI, Post N, et al. T cell response to SARS-CoV-2 infection in humans: a systematic review. PLoS ONE. 2021;16:e0245532. https://doi.org/10.1371/journal.pone.0245532.
Windpessl M, Bruchfeld A, Anders H-J, et al. COVID-19 vaccines and kidney disease. Nat Rev Nephrol. 2021;17:291–3. https://doi.org/10.1038/s41581-021-00406-6.
Malipiero G, Moratto A, Infantino M, et al. Assessment of humoral and cellular immunity induced by the BNT162b2 SARS-CoV-2 vaccine in healthcare workers, elderly people, and immunosuppressed patients with autoimmune disease. Immunol Res. 2021;69:576–83. https://doi.org/10.1007/s12026-021-09226-z.
Hou Y-C, Lu K-C, Kuo K-L. The efficacy of COVID-19 vaccines in chronic kidney disease and kidney transplantation patients: a narrative review. Vaccines (Basel). 2021;9:885. https://doi.org/10.3390/vaccines9080885.
Vaiciuniene R, Sitkauskiene B, Bumblyte IA, et al. Immune response after SARS-CoV-2 vaccination in kidney transplant patients. Medicina (Kaunas). 2021;57:1327. https://doi.org/10.3390/medicina57121327.
Kong NCT, Beran J, Kee SA, et al. A new adjuvant improves the immune response to hepatitis B vaccine in hemodialysis patients. Kidney Int. 2008;73:856–62. https://doi.org/10.1038/sj.ki.5002725.
European Consensus Group on Hepatitis B Immunity. Are booster immunisations needed for lifelong hepatitis B immunity? European Consensus Group on Hepatitis B Immunity. Lancet. 2000;355(9203):561–5. https://doi.org/10.1016/S0140-6736(99)07239-6.
Krueger KM, Ison MG, Ghossein C. Practical guide to vaccination in all stages of CKD, including patients treated by dialysis or kidney transplantation. Am J Kidney Dis. 2020;75:417–25. https://doi.org/10.1053/j.ajkd.2019.06.014.
Broseta JJ, Rodríguez-Espinosa D, Rodríguez N, et al. Humoral and cellular responses to mRNA-1273 and BNT162b2 SARS-CoV-2 vaccines administered to hemodialysis patients. Am J Kidney Dis. 2021;78:571–81. https://doi.org/10.1053/j.ajkd.2021.06.002.
Bensouna I, Caudwell V, Kubab S, et al. SARS-CoV-2 antibody response after a third dose of the BNT162b2 vaccine in patients receiving maintenance hemodialysis or peritoneal dialysis. Am J Kidney Dis. 2022;79:185-192.e1. https://doi.org/10.1053/j.ajkd.2021.08.005.
Frantzen L, Thibeaut S, Moussi-Frances J, et al. COVID-19 vaccination in haemodialysis patients: good things come in threes. Nephrol Dial Transpl. 2021;36:1947–9. https://doi.org/10.1093/ndt/gfab224.
Attias P, Sakhi H, Rieu P, et al. Antibody response to the BNT162b2 vaccine in maintenance hemodialysis patients. Kidney Int. 2021;99:1490–2. https://doi.org/10.1016/j.kint.2021.04.009.
Yanay NB, Freiman S, Shapira M, et al. Experience with SARS-CoV-2 BNT162b2 mRNA vaccine in dialysis patients. Kidney Int. 2021;99:1496–8. https://doi.org/10.1016/j.kint.2021.04.006.
Simon B, Rubey H, Treipl A, et al. Haemodialysis patients show a highly diminished antibody response after COVID-19 mRNA vaccination compared to healthy controls. Nephrol Dial Transpl. 2021. https://doi.org/10.1093/ndt/gfab179.
Agur T, Ben-Dor N, Goldman S, et al. Antibody response to mRNA SARS-CoV-2 vaccine among dialysis patients—a prospective cohort study. Nephrol Dial Transpl. 2021. https://doi.org/10.1093/ndt/gfab155.
Grupper A, Katchman H. SARS-CoV-2 vaccines: safety and immunogenicity in solid organ transplant recipients and strategies for improving vaccine responses. Curr Transpl Rep. 2022. https://doi.org/10.1007/s40472-022-00359-0.
Sattler A, Schrezenmeier E, Weber UA, et al. (2021) Impaired humoral and cellular immunity after SARS-CoV-2 BNT162b2 (tozinameran) prime-boost vaccination in kidney transplant recipients. J Clin Invest. 2021;131(14):e150175. https://doi.org/10.1172/JCI150175.
Boedecker-Lips SC, Lautem A, Runkel S, et al. (2022) Six-month follow-up after vaccination with BNT162b2: SARS-CoV-2 antigen-specific cellular and humoral immune responses in hemodialysis patients and kidney transplant recipients. Pathogens. 2022;11:67. https://doi.org/10.3390/pathogens11010067.
Grupper A, Sharon N, Finn T, et al. Humoral response to the Pfizer BNT162b2 vaccine in patients undergoing maintenance hemodialysis. CJASN. 2021;16:1037–42. https://doi.org/10.2215/CJN.03500321.
Stumpf J, Siepmann T, Lindner T, et al. Humoral and cellular immunity to SARS-CoV-2 vaccination in renal transplant versus dialysis patients: A prospective, multicenter observational study using mRNA-1273 or BNT162b2 mRNA vaccine. Lancet Reg Health Eur. 2021;9:100178. https://doi.org/10.1016/j.lanepe.2021.100178.
Georgery H, Devresse A, Yombi J-C, et al. Disappointing immunization rate after 2 doses of the BNT162b2 vaccine in a belgian cohort of kidney transplant recipients. Transplantation. 2021;105:e283–4. https://doi.org/10.1097/TP.0000000000003861.
Hod T, Ben-David A, Olmer L, et al. Humoral Response of Renal Transplant Recipients to the BNT162b2 SARS-CoV-2 mRNA Vaccine Using Both RBD IgG and Neutralizing Antibodies. Transplantation. 2021;105:e234. https://doi.org/10.1097/TP.0000000000003889.
Hall VG, Ferreira VH, Ierullo M, et al. Humoral and cellular immune response and safety of two-dose SARS-CoV-2 mRNA-1273 vaccine in solid organ transplant recipients. Am J Transpl. 2021. https://doi.org/10.1111/ajt.16766.10.1111/ajt.16766.
Dulovic A, Strengert M, Ramos GM, et al. Diminishing immune responses against variants of concern in dialysis patients four months after SARS-CoV-2 mRNA vaccination. Nephrology. 2021;15:11180.
Krueger KM, Halasa N, Ison MG. SARS-CoV-2 vaccine in dialysis patients: time for a boost? Am J Kidney Dis. 2022;79:162–3. https://doi.org/10.1053/j.ajkd.2021.10.003.
Kamar N, Abravanel F, Marion O, et al. Three doses of an mRNA Covid-19 vaccine in solid-organ transplant recipients. N Engl J Med. 2021;385:661–2. https://doi.org/10.1056/NEJMc2108861.
Dekervel M, Henry N, Torreggiani M, et al. Humoral response to a third injection of BNT162b2 vaccine in patients on maintenance haemodialysis. Clin Kidney J. 2021;14:2349–55. https://doi.org/10.1093/ckj/sfab152.
Reindl-Schwaighofer R, Heinzel A, Mayrdorfer M, et al. Comparison of SARS-CoV-2 antibody response 4 weeks after homologous vs heterologous third vaccine dose in kidney transplant recipients. JAMA Intern Med. 2021;182:165. https://doi.org/10.1001/jamainternmed.2021.7372.
Schrezenmeier E, Rincon-Arevalo H, Stefanski AL, et al. B and T Cell responses after a third dose of SARS-CoV-2 vaccine in kidney transplant recipients. J Am Soc Nephrol ASN. 2021;32(12):3027–33. https://doi.org/10.1681/ASN.2021070966.
Massa F, Cremoni M, Gérard A, et al. Safety and cross-variant immunogenicity of a three-dose COVID-19 mRNA vaccine regimen in kidney transplant recipients. EBioMedicine. 2021;73:103679. https://doi.org/10.1016/j.ebiom.2021.103679.
Ben-Dov IZ, Tzukert K, Aharon M, et al. Response to tozinameran (BNT162b2) booster in twice-vaccinated kidney transplant and maintenance dialysis patients. J Nephrol. 2022. https://doi.org/10.1007/s40620-021-01235-3.
Sadarangani M, Marchant A, Kollmann TR. Immunological mechanisms of vaccine-induced protection against COVID-19 in humans. Nat Rev Immunol. 2021. https://doi.org/10.1038/s41577-021-00578-z.
Miskulin DC, Combe C. mRNA COVID-19 vaccine for people with kidney failure: hope but prudence warranted. CJASN. 2021;16:996–8. https://doi.org/10.2215/CJN.04500421.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no conflict of interest exists.
Ethical approval
All procedures performed in these studies involving human participants were in accordance with the ethical standards of the ASL BR Ethical Committee (approval number 147/21), which evaluated and approved the study protocol.
Research involving human and animal participants
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
De Cagna, M.R., Colucci, V., Di Maggio, A. et al. Humoral and cellular response after BNT162b2 vaccine booster in hemodialysis patients and kidney transplant recipients. Clin Exp Nephrol 27, 445–453 (2023). https://doi.org/10.1007/s10157-023-02317-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-023-02317-1