Abstract
Purpose
High output is a common complication after stoma formation. Although the management of high output is described in the literature, there is a lack of consensus on definitions and treatment. Our aim was to review and summarise the current best evidence.
Methods
MEDLINE, Cochrane Library, BNI, CINAHL, EMBASE, EMCARE, and ClinicalTrials.gov were searched from 1 Jan 2000 to 31 Dec 2021 for relevant articles on adult patients with a high-output stoma. Patients with enteroatmospheric fistulas and case series/reports were excluded. Risk of bias was assessed using RoB2 and MINORS. The review was registered in PROSPERO (CRD42021226621).
Results
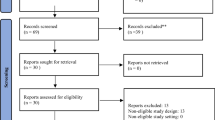
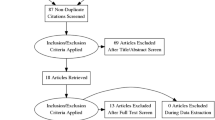
The search strategy identified 1095 articles, of which 32 studies with 768 patients met the inclusion criteria. These studies comprised 15 randomised controlled trials, 13 non-randomised prospective trials, and 4 retrospective cohort studies. Eighteen different interventions were assessed. In the meta-analysis, there was no difference in stoma output between controls and somatostatin analogues (g − 1.72, 95% CI − 4.09 to 0.65, p = 0.11, I2 = 88%, t2 = 3.09), loperamide (g − 0.34, 95% CI − 0.69 to 0.01, p = 0.05, I2 = 0%, t2 = 0) and omeprazole (g − 0.31, 95% CI − 2.46 to 1.84, p = 0.32, I2 = 0%, t2 = 0). Thirteen randomised trials showed high concern of bias, one some concern, and one low concern. The non-randomised/retrospective trials had a median MINORS score of 12 out of 24 (range 7–17).
Conclusion
There is limited high-quality evidence favouring any specific widely used drug over the others in the management of high-output stoma. Evidence, however, is weak due to inconsistent definitions, risk of bias and poor methodology in the existing studies. We recommend the development of validated core descriptor and outcomes sets, as well as patient-reported outcome measures.




Similar content being viewed by others
Data availability
The authors declare that all relevant data used to conduct this review are included in the manuscript and the accompanying supplements.
References
Harris DA, Egbeare D, Jones S, Benjamin H, Woodward A, Foster ME (2005) Complications and mortality following stoma formation. Ann R Coll Surg Engl 87(6):427–431
Nightingale J (2001) Intestinal failure. London: Greenwich Medical Media
Phillips SF, Giller J (1973) The contribution of the colon to electrolyte and water conservation in man. J Lab Clin Med 81(5):733–746
Debongnie JC, Phillips SF (1978) Capacity of the human colon to absorb fluid. Gastroenterology 74(4):698–703
Nightingale J, Woodward JM, Small Bowel and Nutrition Committee of the British Society of Gastroenterology (2006) Guidelines for management of patients with a short bowel. Gut 55(Suppl 4):iv1–iv12
Williams RN, Hemingway D, Miller AS (2009) Enteral Clostridium difficile, an emerging cause for high-output ileostomy. J Clin Pathol 62(10):951–953
Hanna S, Mac II (1960) The influence of aldosterone on magnesium metabolism. Lancet 2(7146):348–350
Hessov I, Andersson H, Isaksson B (1983) Effects of a low-fat diet on mineral absorption in small-bowel disease. Scand J Gastroenterol 18(4):551–554
Kennedy HJ, Al-Dujaili EA, Edwards CR, Truelove SC (1983) Water and electrolyte balance in subjects with a permanent ileostomy. Gut 24(8):702–705
Ovesen L, Chu R, Howard L (1983) The influence of dietary fat on jejunostomy output in patients with severe short bowel syndrome. Am J Clin Nutr 38(2):270–277
Nightingale JM, Lennard-Jones JE, Gertner DJ, Wood SR, Bartram CI (1992) Colonic preservation reduces need for parenteral therapy, increases incidence of renal stones, but does not change high prevalence of gall stones in patients with a short bowel. Gut 33(11):1493–1497
Nightingale JMD (2022) How to manage a high-output stoma. Frontline Gastroenterol 13(2):140–151
Higgins JPT, Thomas J, Chandler J et al (2022) Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane Collaboration
Page MJ, McKenzie JE, Bossuyt PM, et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Int J Surg 88:105906
Page MJ, Moher D, Bossuyt PM, et al (2021) PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ 372:n160
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan-a web and mobile app for systematic reviews. Syst Rev 5(1):210
Sterne JAC, Savovic J, Page MJ et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Sterne JA, Hernan MA, Reeves BC et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
R Core Team (2022) R: A language and environment for statistical computing. R Foundation for Statistical Computing
RStudio Team (2022) RStudio: integrated development environment for R. RStudio, PBC
Balduzzi S, Rücker G, Schwarzer G (2019) How to perform a meta-analysis with R: a practical tutorial. Evid Based Ment Health 22:153–160
Viechtbauer W (2010) Conducting meta-analyses in R with the metafor package. J Stat Softw 36(3):1–48
Harrer M, Cuijpers P, Furukawa T, Ebert DD (2019) Dmetar: companion R package for the guide 'Doing Meta-Analysis in R'
McGuinness LA (2019) robvis: An R package and web application for visualising risk-of-bias assessments
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135
Paule RC, Mandel J (1982) Consensus values and weighting factors. J Res Natl Bur Stand (1977) 87(5):377–385
Sidik K, Jonkman JN (2002) A simple confidence interval for meta-analysis. Stat Med 21(21):3153–3159
Knapp G, Hartung J (2003) Improved tests for a random effects meta-regression with a single covariate. Stat Med 22(17):2693–2710
Hedges L (1981) Distribution theory for glass’s estimator of effect size and related estimators. J Educ Stat 6(2):107–128
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Peters JL, Sutton AJ, Jones DR, Abrams KR, Rushton L (2008) Contour-enhanced meta-analysis funnel plots help distinguish publication bias from other causes of asymmetry. J Clin Epidemiol 61(10):991–996
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56(2):455–463
Rucker G, Schwarzer G, Carpenter JR, Schumacher M (2008) Undue reliance on I(2) in assessing heterogeneity may mislead. BMC Med Res Methodol 8:79
Sterne JA, Sutton AJ, Ioannidis JP et al (2011) Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ 343:d4002
Tytgat G, Huibregtse K (1975) Loperamide and ileostomy output–placebo-controled double-blind crossover study. BMJ 2(5972):667
Tytgat G, Huibregtse K, Dagevos J, van den Ende A (1977) Effect of loperamide on fecal output and composition in well-established ileostomy and ileorectal anastomosis. Am J Digestive Dis 22(8):669–676
Aly A, Barany F, Kollberg B, Monsen U, Wisen O, Johansson C (1980) Effect of an H2-receptor blocking agent on diarrhoeas after extensive small bowel resection in Crohn’s disease. Acta Med Scand 207(1–2):119–122
King R, Norton T, Hill G (1982) A double-blind crossover study of the effect of loperamide hydrochloride and codeine phosphate on ileostomy output. Aust N Z J Surg 52(2):121–124
Rodrigues CA, Lennard-Jones JE, Thompson DG, Farthing MJ (1989) The effects of octreotide, soy polysaccharide, codeine and loperamide on nutrient, fluid and electrolyte absorption in the short-bowel syndrome. Aliment Pharmacol Ther 3(2):159–169
Beaugerie L, Cosnes J, Verwaerde F et al (1991) Isotonic high-sodium oral rehydration solution for increasing sodium absorption in patients with short-bowel syndrome. Am J Clin Nutr 53(3):769–772
Kusuhara K, Kusunoki M, Okamoto T, Sakanoue Y, Utsunomiya J (1992) Reduction of the effluent volume in high-output ileostomy patients by a somatostatin analogue, SMS 201–995. Int J Colorectal Dis 7(4):202–205
Jeppesen P, Staun M, Tjellesen L, Mortensen P (1998) Effect of intravenous ranitidine and omeprazole on intestinal absorption of water, sodium, and macronutrients in patients with intestinal resection. Gut 43(6):763–769
Heydorn S, Jeppesen PB, Mortensen PB (1999) Bile acid replacement therapy with cholylsarcosine for short-bowel syndrome. Scand J Gastroenterol 34(8):818–823
Ecker K-W, Stallmach A, Seitz G, Gierend M, Greinwald R, Achenbach U (2003) Oral budesonide significantly improves water absorption in patients with ileostomy for crohn disease. Scand J Gastroenterol 38(3):288–293
Clarebrough E, Guest G, Stupart D (2015) Eating marshmallows reduces ileostomy output: a randomized crossover trial. Colorectal Dis 17(12):1100–1103
Kristensen K, Qvist N (2017) The acute effect of loperamide on ileostomy output: a randomized, double-blinded, placebo-controlled, crossover study. Basic Clin Pharmacol Toxicol 121(6):493–498
Naimi RM, Hvistendahl M, Enevoldsen LH et al (2019) Glepaglutide, a novel long-acting glucagon-like peptide-2 analogue, for patients with short bowel syndrome: a randomised phase 2 trial. Lancet Gastroenterol Hepatol 4(5):354–363
Mesli Y, Holterbach L, Delhorme J-B et al (2021) Is lanreotide really useful in high output stoma? Comparison between lanreotide to conventional antidiarrheal treatment alone. J Invest Surg 34(12):1312–1316
Culkin A, Gabe SM, Nightingale JMD (2022) A new palatable oral rehydration solution: a randomised controlled cross-over study in patients with a high output stoma. J Hum Nutr Diet 35(1):94–101
Lévy E, Palmer D, Frileux P, Parc R, Huguet C, Loygue J (1983) Inhibition of upper gastrointestinal secretions by reinfusion of succus entericus into the distal small bowel. A clinical study of 30 patients with peritonitis and temporary enterostomy. Ann Surg 198(5):596–600
Cooper JC, Williams NS, King RF, Barker MC (1986) Effects of a long-acting somatostatin analogue in patients with severe ileostomy diarrhoea. Br J Surg 73(2):128–131
Jacobsen O, Ladefoged K, Stage JG, Jarnum S (1986) Effects of cimetidine on jejunostomy effluents in patients with severe short-bowel syndrome. Scand J Gastroenterol 21(7):824–828
Nightingale JM, Walker ER, Burnham WR, Farthing MJ, Lennard-Jones JE (1989) Octreotide (a somatostatin analogue) improves the quality of life in some patients with a short intestine. Aliment Pharmacol Ther 3(4):367–373
Nightingale J, Walker E, Farthing M, Lennard-Jones J (1991) Effect of omeprazole on intestinal output in the short bowel syndrome. Aliment Pharmacol Ther 5(4):405–412
O’Keefe SJ, Peterson ME, Fleming CR (1994) Octreotide as an adjunct to home parenteral nutrition in the management of permanent end-jejunostomy syndrome. JPEN J Parenter Enteral Nutr 18(1):26–34
Nehra V, Camilleri M, Burton D, Oenning L, Kelly DG (2001) An open trial of octreotide long-acting release in the management of short bowel syndrome. Am J Gastroenterol 96(5):1494–1498
Ecker KW, Stallmach A, Löffler J, Greinwald R, Achenbach U (2005) Long-term treatment of high intestinal output syndrome with budesonide in patients with Crohn’s disease and ileostomy. Dis Colon Rectum 48(2):237–242
Jeppesen PB (2005) Teduglutide (ALX-0600), a dipeptidyl peptidase IV resistant glucagon-like peptide 2 analogue, improves intestinal function in short bowel syndrome patients. Gut 54(9):1224–1231
Buchman A, Fryer J, Wallin A, Ahn C, Polensky S, Zaremba K (2006) Clonidine reduces diarrhea and sodium loss in patients with proximal jejunostomy: a controlled study. J Parenter Enter Nutr 30(6):487–491
Scribano M, Monterubbianesi R, Kohn A (eds) (2015) Efficacy of antisecretory factor in reducing high intestinal output in patients with ileostomy for Crohn's disease. J Crohns Colitis 9(Suppl_1):S338. https://doi.org/10.1093/ecco-jcc/jju027.635
Hvistendahl M, Brandt CF, Tribler S et al (2016) Effect of liraglutide treatment on jejunostomy output in patients with short bowel syndrome. J Parenter Enteral Nutr 42(1):112–121
Liu C, Ludlow E, Davidson RB et al (2021) Stoma-output reinfusion device for ileostomy patients. Dis Colon Rectum 64(11):e662–e668
Chia CLK, Tai YS, Tan K-Y (2017) A preliminary study of the use of oral rehydration salts in decreasing ileostomy output. Tech Coloproctol 21(7):587–588
Picot D, Layec S, Seynhaeve E, Dussaulx L, Trivin F, Carsin-Mahe M (2020) Chyme reinfusion in intestinal failure related to temporary double enterostomies and enteroatmospheric fistulas. Nutrients 12(5):1376
Sobocki J, Zaczek Z, Jurczak P et al (2021) Restricted vs. unrestricted oral intake in high output end-jejunostomy patients referred to reconstructive surgery. Br J Nutr 125(10):1125–1131
Zaczek Z, Dabrowska K, Omidi M, Panczyk M, Sobocki J (2022) Effect of thickening powder on gastrointestinal losses in patients with high-output end jejunostomy syndrome—preliminary results. In Vivo 36(2):884–889
Nightingale JM, Lennard-Jones JE, Walker ER, Farthing MJ (1990) Jejunal efflux in short bowel syndrome. Lancet 336(8718):765–768
Hara Y, Miura T, Sakamoto Y, Morohashi H, Nagase H, Hakamada K (2020) Organ/space infection is a common cause of high output stoma and outlet obstruction in diverting ileostomy. BMC Surg 20(1):83
Teitelbaum EN, Vaziri K, Zettervall S, Amdur RL, Orkin BA (2013) Intraoperative small bowel length measurements and analysis of demographic predictors of increased length. Clin Anat 26(7):827–832
Tacchino RM (2015) Bowel length: measurement, predictors, and impact on bariatric and metabolic surgery. Surg Obes Relat Dis 11(2):328–334
Funding
No financial or non-financial support or incentives were received for this review.
Author information
Authors and Affiliations
Contributions
NJS and IRD had the initial idea for the review. All authors contributed to the study’s conception and design. HL, VEK and MRSS performed the literature search. HL, VEK and AES performed study selection and data extraction. HL, LHM and FMD performed the risk of bias assessment. The first draft of the manuscript was written by HL and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
IRD is the Honorary President of the UK registered charity Colostomy UK and on the editorial board of Techniques in Coloproctology. All other authors declare no conflict of interest.
Ethical approval
Not applicable.
Informed Consent
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary Fig. 1
. Contour-enhanced funnel plots, trim & fill analysis and limit meta-analysis. a Contour-enhanced funnel plot for loperamide vs. control; b trim & fill funnel plot for loperamide vs. control; c contour-enhanced funnel plot for somatostatin analogues vs. control; d trim & fill funnel plot for somatostatin analogues vs. control; e contour-enhanced funnel plot for omeprazole vs. control; f trim & fill adjusted results; g limit meta-analysis adjusted results. K number of trials including additionally imputed trials in the trim & fill analysis, SMD standardised mean difference, 95% CI 95% confidence interval, PI prediction interval (PDF 888 KB)
Supplementary Fig. 2
. Leave-one-out meta-analysis of somatostatin analogues vs. control. Recalculation of the meta-analysis K times, each time leaving out one study. K number of trials included in the meta-analysis. θ(hat) = estimated effect size. The dotted line and shaded area represent the original meta-analysis’s pooled effect size and 95% confidence interval (PDF 476 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lederhuber, H., Massey, L.H., Kantola, V.E. et al. Clinical management of high-output stoma: a systematic literature review and meta-analysis. Tech Coloproctol 27, 1139–1154 (2023). https://doi.org/10.1007/s10151-023-02830-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-023-02830-1