Abstract
Background
Metastatic bone cancer pain is one of the most common clinical cancer pains and is caused by many factors. This study was conducted to explore the clinical efficacy of using two non-steroidal anti-inflammatory drugs (NSAIDs) along with an opioid in treating metastatic bone cancer pain.
Material and Method
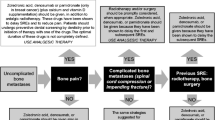
A total of 342 patients with a pain score of 7–10 on the visual analog scale (VAS) were recruited for 4 weeks of treatment and randomly assigned to three different groups—one group received two NSAIDs (diclofenac and celecoxib), one group received diclofenac, and one group received celecoxib. All patients received morphine sulfate 10 mg/12 h with a reduction of 50% or addition of 25% each time until the VAS score was <5. The VAS score, remission rate (RR), breakthrough pain (BTP), morphine sulfate dose and side-effects among the three groups were compared.
Results
After 4 weeks of treatment, we found that using two NSAIDs along with an opioid could yield a significantly lower VAS score (p = 0.006), higher RR (p = 0.0002) and fewer incidences of BTP (p = 0.011), compared to the use of only one NSAID. Furthermore, using two NSAIDS could significantly decrease the consumption of morphine sulfate compared to using each NSAID in isolation (p = 0.0031 in week 1; p = 0.020 in week 2; p = 0.0012 in week 4). Additionally, using two NSAIDs could produce fewer incidences of dizziness (p = 0.002), constipation (p < 0.0001) and drowsiness (p < 0.0001).
Conclusion
Although limited by the relatively small samples, these results indicate that using two NSAIDs along with an opioid in treating metastatic bone cancer pain was more effective and acceptable, which is worthy of further clinical application.



Similar content being viewed by others
References
Casimiro S, Luis I, Fernandes A et al (2012) Analysis of a bone metastasis gene expression signature in patients with bone metastasis from solid tumors. Clin Exp Metastasis 29(2):155–164
Egeblad M, Werb Z (2002) New functions for the matrix metalloproteinases in cancer progression. Nat Rev Cancer 2(3):161–174
Lu X, Wang Q, Hu G et al (2009) ADAMTS1 and MMP1 proteolytically engage EGF-like ligands in an osteolytic signaling cascade for bone metastasis. Genes Dev 23(16):1882–1894
Jimenez-Andrade JM, Mantyh WG, Bloom AP et al (2010) Bone cancer pain. Ann N Y Acad Sci 1198(1):173–181
Clohisy DR, Mantyh PW (2003) Bone cancer pain. Cancer 97(3 Suppl):866–873
Goblirsch MJ, Zwolak P, Clohisy DR (2005) Advances in understanding bone cancer pain. J Cell Biochem 96(4):682–688
Langer C, Hirsh V (2010) Skeletal morbidity in lung cancer patients with bone metastases: demonstrating the need for early diagnosis and treatment with bisphosphonates. Lung Cancer 67(1):4–11
Mantyh P (2013) Bone cancer pain: causes, consequences, and therapeutic opportunities. Pain 154(Suppl 1):S54–S62
Ross JR, Saunders Y, Edmonds PM et al (2003) Systematic review of role of bisphosphonates on skeletal morbidity in metastatic cancer. Br Med J 327(7413):469
McNicol E, Strassels S, Goudas L et al (2004) Nonsteroidal anti-inflammatory drugs, alone or combined with opioids, for cancer pain: a systematic review. J Clin Oncol 22(10):1975–1992
Mercadante S, Fulfaro F (2005) World Health Organization guidelines for cancer pain: a reappraisal. Ann Oncol. 16(Suppl 4):iv132–iv135
Liu J, Liu FY, Tong ZQ et al (2013) Lysine-specific demethylase 1 in breast cancer cells contributes to the production of endogenous formaldehyde in the metastatic bone cancer pain model of rats. PLoS One 8(3):e58957
Coleman RE (2006) Clinical features of metastatic bone disease and risk of skeletal morbidity. Clin Cancer Res 12:6243s–6249s
Sevcik MA, Ghilardi JR, Peters CM et al (2005) Anti-NGF therapy profoundly reduces bone cancer pain and the accompanying increase in markers of peripheral and central sensitization. Pain 115:128–141
Peters CM, Lindsay TH, Pomonis JD et al (2004) Endothelin and the tumorigenic component of bone cancer pain. Neuroscience 126:1043–1052
Mercadante S (1997) Malignant bone pain: pathophysiology and treatment. Pain 69:1–18
Wolff RF, Aune D, Truyers C et al (2012) Systematic review of efficacy and safety of buprenorphine versus fentanyl or morphine in patients with chronic moderate to severe pain. Curr Med Res Opin 28(5):833–845
Fan Z, Lin H, He Q (2011) Celecoxib combined preoperative concurrent chemotherapy for rectal cancer short-term efficacy. Pract J Cancer 26(1):49–55
Setoguchi N, Takamura N, Fujita K et al (2013) A diclofenac suppository-nabumetone combination therapy for arthritic pain relief and a monitoring method for the diclofenac binding capacity of HSA site II in rheumatoid arthritis. Biopharm Drug Dispos 34(2):125–136
Dahl JB, Kehlet H (1991) Non-steroidal anti-inflammatory drugs: ratio-nale for use in severe postoperative pain. Br J Anaesth 66:703–712
Chan A, Dore CJ, Ramachandra V (1996) Analgesia for day surgery. Evaluation of the effect of diclofenac given before or after surgery with or without bupivacaine infiltration. Anaesthesia 51:592–595
White P, Sacan O, Tufanogullari B et al (2007) Effect of short-term postoperative celecoxib administration on patient outcome after outpatient laparoscopic surgery. Can J Anaesth 54(5):342–348
Yeganeh Mogadam A, Fazel MR, Parviz S (2012) Comparison of analgesic effect between gabapentin and diclofenac on post-operative pain in patients undergoing tonsillectomy. Arch Trauma Res 1(3):108–111
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
About this article
Cite this article
Liu, Z., Xu, Y., Liu, Zl. et al. Combined application of diclofenac and celecoxib with an opioid yields superior efficacy in metastatic bone cancer pain: a randomized controlled trial. Int J Clin Oncol 22, 980–985 (2017). https://doi.org/10.1007/s10147-017-1133-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-017-1133-y